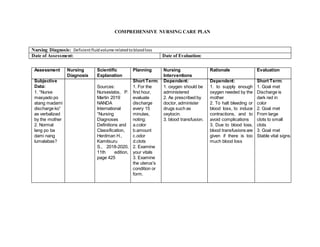
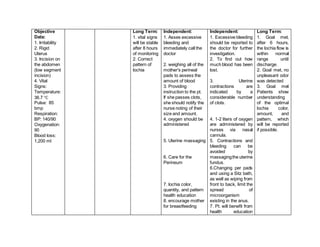
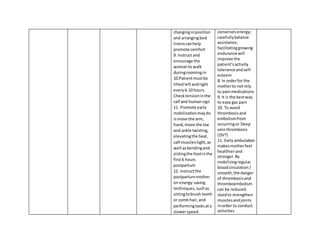
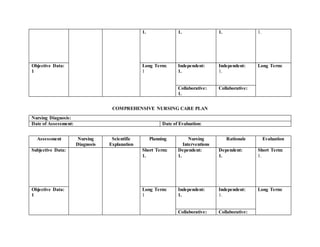
The nursing care plan addresses two nursing diagnoses: deficient fluid volume related to blood loss and activity intolerance related to cesarean section. Short term and long term goals are outlined to monitor bleeding, vital signs, pain levels, and increase mobility. Dependent, independent, and collaborative interventions include medication administration, education, exercise, and physical therapy referral to manage symptoms and improve the patient's condition over time.