Reproductive System Embryology.pptx
- 1. Dr. NDAYISABA CORNEILLE CEO of CHG MBChB,DCM,BCSIT,CCNA Supported BY
- 2. Objectives • Describe the development of gonads (indifferent stage) and sex determination. • Describe the development of testis and ovaries and the related structures. • Describe the development of the genital ducts. • Describe the development of male and female glands. • Describe the development of the male and female external genitalia. • Discuss the related developmental anomalies. Dr Ndayisaba Corneille 2
- 3. Development of Urogenital System • Both the urinary &reproductive systems are closely related (structurally & developmentally) • Urogenital system develop from the intermediate mesoderm • Urogenital ridge is a longitudinal elevation of the mesoderm lateral to the dorsal aorta • Nephrogenic cord (ridge) develop in the urogenital ridge • Gives rise to part of the urinary system • Genital (gonadal) ridge develop close to the nephrogenic cord • Gives rise to part of the genital system Dr Ndayisaba Corneille 3
- 5. Development of Gonads • Early development of male & female gonads are similar (indifferent stage – indifferent gonads) • Development of gonads begin in the 5thweek • Source of gonadal development • Mesothelium of posterior abdominalwall • lateral somatic mesoderm – cortex • Proliferate and form gonadalridge • Primary sexcords • In female formovary • Underlying mesenchyme – intermediate mesoderm –medulla • In male formtestis • Primordial germ cells – from the yolksac • Migrate via mesentery & mesenchyme to the primary sex cords (6thweek) Dr Ndayisaba Corneille 5
- 6. Sex Determination • Y chromosome has SRY gene in the sex determining region for testis determining factor(TDF) • Presence of TDF determines the differentiation of testis • Primary sex cords (in medulla) → seminiferous tubules • Absence of Y chromosome &TDF results in ovary formation • Testosterone from fetal testis determines male characteristics • Female characteristics determined without hormonal effect Dr Ndayisaba Corneille 6
- 7. Development of Testes • Primary sex cords extend into medulla and form seminiferous cords (obliterated tubules) - the primitive sex cords continue to proliferate and penetrate deep into the medulla to form the testis or medullary cords • The cords break up into a network of tiny cell strands that later give rise to tubules of the rete testis • Rete testis connect with 15‐20 mesonephric tubules (Wolfian ducts) → efferent ductules • Mesonephric duct becomes ductus epididymis Dr Ndayisaba Corneille 7
- 8. Development of Testes • The fibrous tunica albuginea form - separates the testis cords from the surface epithelium • In the fourth month, the testis cords become horseshoe-shaped, and their extremities are continuous with those of the rete testis. Testis cords are now composed of primitive germ cells and sustentacular cells of Sertoli derived from the surface epithelium of the gland. • Testis enlarge & separate from the abdominal wall leaving a mesentery (mesorchium) Dr Ndayisaba Corneille 8
- 10. Development of Testes • Interstitial (leydig) cells form from the mesenchyme between seminiferous cords • By 8th week secrete testosterone under influence of hCG • Induce differentiation of mesonephric ducts & externalgenitalia • Sertoli cells derived from surface epithelium of testis • Secrete antimullerian hormone (AMH) at 6‐7week • Suppresses development of paramesonephric (mullerian)ducts • Spermatogonia develop from primordial germcells Dr Ndayisaba Corneille 10
- 11. Development of Ovaries • In female embryos with an XX sex chromosome complement and no Y chromosome, primitive sex cords dissociate into irregular cell clusters. • These clusters, containing groups of primitive germ cells, occupy the medullary part of the ovary. • Later, they disappear and are replaced by a vascular stroma that forms the ovarian medulla. • In the seventh week, it gives rise to a second generation of cords, cortical cords, which penetrate the underlying mesenchyme but remain close to the surface. • In the third month, these cords split into isolated cell clusters. Cells in these clusters continue to proliferate and begin to surround each oogonium with a layer of epithelial cells called follicular cells. • Together, the oogonia and follicular cells constitute a primordial follicle • Extend to underlying mesenchyme at early fetal life Dr Ndayisaba Corneille 11
- 13. Development of Ovaries •In embryos with an XX sex chromosome configuration, medullary cords of the gonad regress, and a secondary generation of cortical cords develops. In embryos with an XY sex chromosome complex, medullary cords develop into testis cords, and secondary cortical cords fail to develop. • Ovary separate from the abdominal wall leaving a mesentery(mesovarium) Dr Ndayisaba Corneille 13
- 14. INFLUENCE OF PRIMORDIAL GERM CELLS ON DIFFERENT GONARDS Dr Ndayisaba Corneille 14
- 15. Development of Genital Ducts • In the indifferent stage two ducts develop (5th‐6thweek) • Mesonephric (wolffian) ducts from mesonephrone • Important in male genital structures • Disappear in female • Paramesonephric (mullarian) ducts – develop lateral to the gonads & mesonephricducts • Form from longitudinal invagination of the mesothelium • Important in female genital structures • Disappear in male Dr Ndayisaba Corneille 15
- 16. Development of Genital Ducts Dr Ndayisaba Corneille 16
- 17. Development of Genital Ducts Dr Ndayisaba Corneille 17
- 18. Development of Genital Ducts Mesonephric ducts • Proximally – form epididymis • Distally – form ductus deferens & ejaculatory duct • Lateral outgrowth give rise to seminal vesicle Paramesonephric ducts • Rostrally (with funnel shape opening into the abdomen) • Caudally they cross anterior to mesonephric ducts & fuse together forming uterovaginal primordium • Ends at the posterior wall of the urogenital sinus • Results in an elevation called sinus tubercle Dr Ndayisaba Corneille 18
- 19. Influence of the sex glands on further sex differentiation. Dr Ndayisaba Corneille 19
- 20. Influence of the sex glands on further sex differentiation. Dr Ndayisaba Corneille 20
- 21. Formation of the Peritoneal Structures • The fusion of the distal parts of the paramesonephric ducts extend parts of the peritoneum towards the midline • The extended peritoneum forms the broad ligament • Anterior to it forms the vesicouterine pouch • Posterior to it forms the rectouterine pouch Dr Ndayisaba Corneille 21
- 23. Development of Female Genital Organs • Uterine tubes develop from proximal part of paramesonephric ducts • Uterus develops from the uterovaginal primordium • Vagina develops from the urogenital sinus • Sinus tubercle induces the outgrowth of sinovaginal bulbs → vaginal plate →vagina • Separation between urogenital sinus & vagina →hymen Dr Ndayisaba Corneille 23
- 24. Development of Female Glands • Urethral & paraurethral glands develop as buds from urethra • Greater vestibular glands develop from outgrowth of urogenital sinus Dr Ndayisaba Corneille 24
- 25. Formation of uterus and Vagina Dr Ndayisaba Corneille 25
- 26. Formation of uterus and Vagina Dr Ndayisaba Corneille 26
- 27. Development of Male Glands • Seminal vesicle develop from a Lateral outgrowth of the distal part of the mesonephric duct • Prostate gland develop from endodermal outgrowth of the prostatic urethra into the surrounding mesenchyme • Bulbourethral glands develop from outgrowths of the penile urethra Dr Ndayisaba Corneille 27
- 28. Development of External Genitalia Indifferent Stage (4th‐7thweeks) • Genital tubercle formed from mesenchymal proliferation at the cranial end of the cloacal membrane • Phallus is an elongated genital tubercle • Urogenital (urethral) & labioscrotal folds develop on sides of the cloacal membrane Dr Ndayisaba Corneille 28
- 29. Development of External Genitalia Indifferent Stage • Cloacal membrane separated into urogenital membrane (anteriorly) and anal membrane (posteriorly) by the urorectal septum • The end of the urorectal septum form the perineal body • After a week the membranes rupture and form anus & urogenital orifice Dr Ndayisaba Corneille 29
- 30. Indifferent stages of the external genitalia. Dr Ndayisaba Corneille 30
- 31. Development of Male External Genitalia • This is under the influence of androgens secreted by the Testis • Phallus (genital tubercle) enlarges and elongates to form penis • Penile corpora formed by phallus mesenchyme • Urogenital folds fuse & close the urethral groove forming spongy urethra. (Site of fusion – penile raphe) • Prepuce formed by circular ectodermal ingrowth around the glans • Scrotum formed by the fusion of the labioscrotal folds. (Site of fusion is the scrotal raphe) Dr Ndayisaba Corneille 31
- 32. Development of male external genitalia Dr Ndayisaba Corneille 32
- 33. Development of Female External Genitalia • The process is stimulated by Estrogen • Phallus elongates slightly to become the clitoris • Urogenital folds form the labia minora • Fuse posteriorly to form frenulum of the labia minora • Labioscrotal folds form the labia majora • Fuse posteriorly & anteriorly to form posterior & anterior labial commissures Dr Ndayisaba Corneille 33
- 34. Development of Female External Genitalia Dr Ndayisaba Corneille 34
- 35. Development of Inguinal Canal • While mesonephric duct degenerates, a ligament (gubernaculum) appears • Gubernaculum connects the gonads with the labioscrotal swellings through the abdominal wall • Peritoneal evagination (processus vaginalis) follow the gubernaculum taking the layers of the abdominal wall in front of it forming the inguinal canal • Processus vaginalis guide the descent of testis through inguinalcanal • Gubernaculum in females form ( Cranially – ovarian ligament, Caudally – round ligament) Dr Ndayisaba Corneille 35
- 36. Female Genital Malformation • Double uterus • Failure of fusion of inferior part of paramesonephric ducts • Bicornuate uterus • Failure of fusion in the superior part • Unicornuate uterus • Failure of development of one paramesonephric duct Dr Ndayisaba Corneille 36
- 37. Uterine and Vaginal abnormalities Dr Ndayisaba Corneille 37
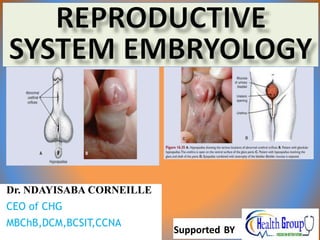
- 38. Male Genital Malformation • Hypospadias (1/300) - External urethral orifice in the ventral side of Glans (glandular hypospadias) • Failure of canalization of glandular plate • Body of penis (penile hypospadias) • Failure of fusion of urogenital folds (Epispadias) - Orifice opens dorsally at the root of the penis • Dorsal development of genital tubercle Dr Ndayisaba Corneille 38
- 39. Male Genital Malformation Dr Ndayisaba Corneille 39
- 40. Male Genital Malformation Testicular anomalies • Cryptorchidism (undescended testes) : 3‐4% of full term men - Found in its path • Ectopic testes - Deviate from its path Dr Ndayisaba Corneille 40
- 41. END Dr Ndayisaba Corneille THANKS FOR LISTENING By DR NDAYISABA CORNEILLE MBChB,DCM,BCSIT,CCNA Contact us: amentalhealths@gmail.com/ ndayicoll@gmail.com whatsaps :+256772497591 /+250788958241 41
