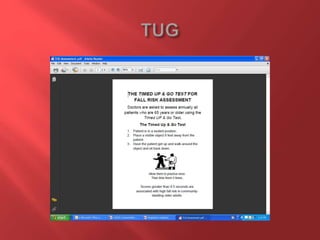
This document discusses strategies for home health care agencies to minimize risks from audits. It outlines the various entities that conduct audits, including RACs, MACs, and ZPICs. Key areas that auditors focus on include medical necessity, coding accuracy, documentation quality, and compliance with Medicare policies. The document provides guidance on ensuring documentation clearly supports the patient's homebound status, medical necessity of skilled services, and demonstrates progress towards goals. It emphasizes having objective data to justify findings and treatment plans.