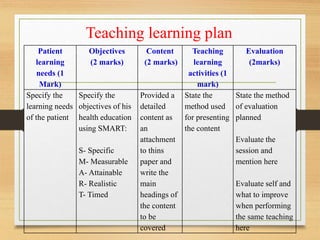
This document provides an orientation for nursing students beginning their Adult Health Nursing I Practicum. It outlines the details of the practicum including the clinical credits, schedule, attendance policy, clinical objectives and locations. It also reviews teaching strategies, safety tips, unsafe practices, student learning activities, grading system, clinical rotation sites, rules, focus areas and assignment requirements like weekly objectives, logs, care plans, case studies and teaching plans. Students will complete their practicum at Nizwa Hospital and Nizwa Poly Clinic over 12 weeks.