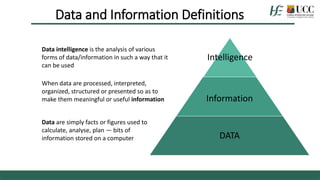
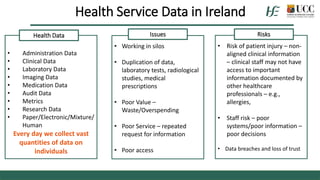
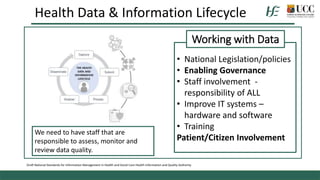
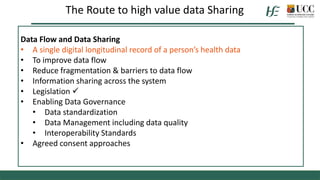
The document discusses the importance of health data sharing in Ireland to improve healthcare services, service planning, and research outcomes. It addresses the existing challenges such as data incompatibility, public perceptions regarding data sharing, and the need for a cohesive health information strategy. Recommendations include fostering trust through clear consent processes and establishing a national framework for data governance and management.