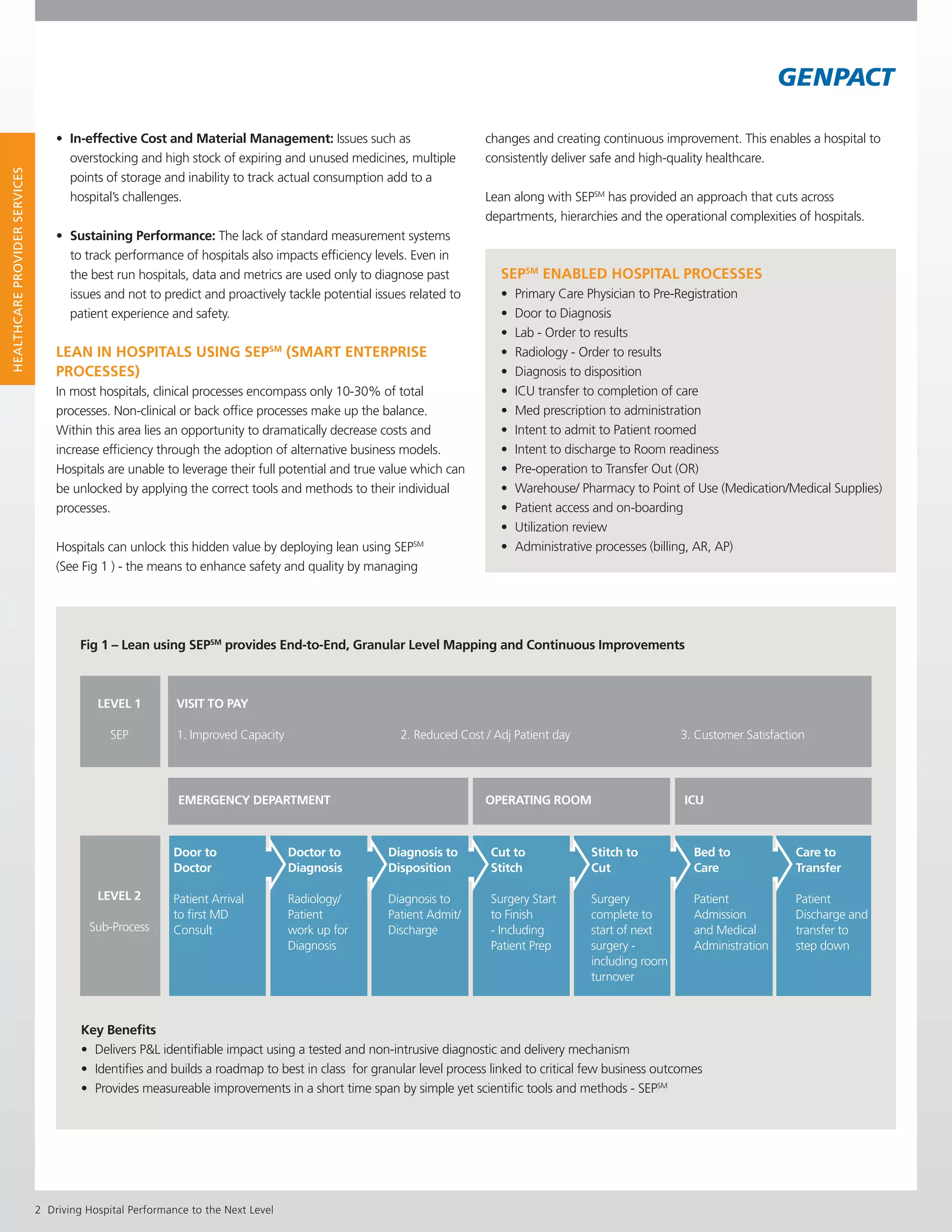
1) The document discusses how hospitals can improve performance by applying Lean methodology and Genpact's proprietary Smart Enterprise Processes (SEPSM) framework to clinical and non-clinical processes.
2) SEPSM enables continuous process improvement through tools like Lean and prior knowledge from benchmarks. It provides end-to-end mapping and granular process improvements.
3) Applying SEPSM has led to reductions in patient wait times, medical stock levels, billing errors and other improvements across the "Visit to Cash" cycle.