ECZEMA AND DERMATITIS for dematology.pptx
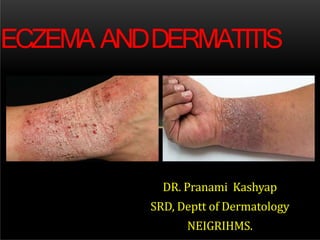
- 1. DR. Pranami Kashyap SRD, Deptt of Dermatology NEIGRIHMS. ECZEMA ANDDERMATITIS
- 2. ECZEMA ⚫'Ekze', in Greek means “toboil over” but it seems that theskin is “Boiling out” or “Oozing out” in eczema. Erythema, papulo-vesicles, oozing &crusting, lichenification ⚫All eczemas are dermatitis, but not all dermatitis are eczemas.
- 3. THE“ITCH/ SCRATCH” CYCLE The sensation of itch and subsequent scratching is hallmark of most eczemas itch scratch itch scratch
- 4. CLASSIFICATION Etiology Pattern/morphology Chronicity Endogenous Discoid Acute Exogenous Hyperkeratotic Chronic Combined Lichenified Seborrheic
- 5. ETIOLOGICAL CLASSIFICATION Eczema Exogenous Endogenous •Irritant Contact Derma. •Allergic Contact Derma. •Photo dermatitis •Infective dermatitis •Atopic dermatitis •Seborrheic dermatitis •Nummular eczema •Stasis Dermatitis •Asteatotic eczema •Pompholyx
- 6. CLASSIFICATIONONTHEBASISOFCHRONICITY Acute eczematous Sub acute eczematous Chronic eczematous ⚫Intense itching ⚫Intense erythema ⚫Oedema ⚫Papulovesicles ⚫Oozing ⚫Erythema (lesser than in acute stage) ⚫Crusting and scaling ⚫Fissuring ⚫Slight to moderate itching ⚫Stinging and burning sensation ⚫Dryness of skin ⚫Excoriation ⚫Fissuring ⚫Lichenification
- 7. CLINICALFEATURES AcuteEczema: • Erythematous&edematousplaque,whichisill-defined &surmountedby papules, vesicles, pustules &exudates that dries to form crusts • scales Chronic Eczema : • Lichenification – Triad of hyperpigmentation, thickening &increased markings of skin • Less vesicular &exudative • Morescaly • Flexural lesions may develop fissures
- 8. COMPLICATIONS: 1. Dermatological : Infection Ide eruption Contact dermatitis Erythroderma 2. Psychosocial : Anxiety Depression Social complications Wage loss Debility Social ostracism
- 9. TREATMENT General measures: • Removetriggers • Hydration&useof Emollients ACUTEPHASE: 1. Topical treatment AcuteEczemaofhands&feet: Soaksofpotassiumpermanganate0.01%,followedby applicationof steroidlotionor creamis best Larger areas : compresses followed by soothing agents like calaminelotion 2. Systemic treatment Systemic steroids : used in extensivelesions &whenIde eruption develop Immunosuppressive: Azathioprine Antibiotics : usedfor infectedlesions Antihistamines: for itching
- 10. CHRONICPHASE 1. Steroids : Topicalsteroids: forlocalizedlesions– t/t ofchoice,for lichenified lesions, topical steroids may be combined with keratolytic agents like salicyclic acid &urea Systemic steroids : for extensive lesions like in airborne contact dermatitis 2. Antibiotics : for bacterial infection – topical or systemic 3. Topical immunomodulators : for their steroid sparing action
- 11. ATOPICDERMATITIS It is a chronic or relapsing dermatitis usually beginning in childhood characterized by marked pruritus and rash ⚫Seen in 3% of all infant ⚫Increased between 3-6 months of age ⚫Increased worldwide incidence because of Pollutants Indoor allergen (house dust mite ) Decline in breast feeding
- 12. ETIOPATHOGENESIS: • Exact cause of atopic dermatitis is unknown • It is genetic predisposition ( due to excessive I.e. hypersensitivity) • Increased histamine release from basophils maylead to persistent pruritus • Produce IL-4and IL-13, which promote IgEproduction by Bcells
- 13. Triggeringfactors ⚫Anxiety; emotional stress ⚫Temperaturechange and sweating ⚫Decreased humidity ⚫Excessive washing ⚫Contact with irritants ⚫Allergens ⚫Foods ⚫Microbial agents
- 14. CLINICALFEATURES 1. Itching : Due to - contact - trauma - Temperaturechanges - Psychic stress 2. Chronic thickening of skin 3. Dry skin 4. Hyperlinear palm
- 15. Oozing, crusted, erythematous, scaly plaques on the scalp and face, sparing the diaper area. When baby begins to crawl, the extensor extremities become more involved. INFANTILE ATOPIC DERMATITIS (2m—2y)
- 16. CHILDHOOD ATOPIC DERMATITIS: (2-12 yrs.) Lesions become prominent on the hands, posterior neck, antecubital and popliteal fossae
- 17. ADULT PHASE (12 YEARS ONWARDS) Commonly involves flexural areas. ⚫The disease may be diffuse or patchy. ⚫Dermatitis of theupper eyelids and blepharitis
- 18. CRITERIAFORDIAGNOSIS(HANIFINANDRAJKA) 1. Major criteria : Pruritus Typical morphology and distribution Facial and ext. involvement in infant. Flexural lichenification in adults and children. Chronic and chronically relapsing dermatitis Personal or family H/o atopy
- 19. 2. Minor criteria : Cataract Cheilitis Ichthyosis Xerosis Orbital darkening Wool intolerance P . alba Dennie- Morgan fold Palmer hyperlinearity Itching when sweating
- 20. MANAGEMENTOFATOPICDERMATITIS INVESTIGATIONS 1. Patch test : ( TypeIV hypersensitivity) 2. Prick test : ( TypeI hypersensitivity ) 3. Bacteria &viral swabs for microscopy &culture.
- 21. TREATMENT 1. First-linetreatment General measures - ⚫Avoidscratching ⚫Avoidfrequent useof soap, contact woollen clothes ⚫Measuretoavoidhousedust mite T opical treatments- ◦ Moisturizer ; Emollients; Humectants ◦ Corticosteroids ◦ Calcineurin inhibitors: Pimecrolimus; tacrolimus
- 22. Oral treatment - ◦ Antihistamines 🞄 Sedative antihistamines preferred 🞄 Promethazine; trimeprazine; hydroxyzine ◦ Antibiotics ◦ Systemic steroids (in severe cases)
- 23. 2. Second-line treatment ⚫Intensive topical therapy ⚫Wet wraptechnique 3. Third-line treatment ⚫Phototherapy ⚫Oral immunosuppresants ◦ Cyclosporine ◦ Azathrioprine ◦ Thymopentin ◦ α- Interferon
- 24. CONTACT DERMATITIS –Acuteorchronicinflammatoryreactions to substancesthatcomeincontactwithth e skin. –TwoformsofCDexist • IritantContactDermatitis(ICD) • AlergicContactDermatitis(ACD)
- 25. • Common allergen-containing products include • cosmetics • Soaps • dyes and • jewellery. • The most frequent sensitizers are • fragrance • nickel, neomycin • formaldehyde, lanolin, and • a host of other common environmental chemicals.
- 27. 27
- 28. 28
- 29. 29
- 30. TREATMENT OF CONTACT DERMATITIS ▪ Avoid the agent. ▪ Topical steroids and if severe systemic steroids can be considered for a short time. ▪ Antipruritics ▪ Treat the complications.
- 31. DISCOID ECZEMA ▪ Nummular or Microbial eczema ▪ A chronic,pruritic,inflammatory dermatitis occuring in the form of coin- shaped plaques. ▪ Unknown cause. ▪ Unrelated to atopic diathesis ▪ IgE levels are normal ▪ Commonly seen in the lower limbs
- 32. 32
- 33. 33
- 35. TREATMENT OF DISCOID ECZEMA ▪ S kin hydration and application of potent steroids with o r with o u t antihistamines. ▪ Usualy recurs.
- 36. SEBORRHOEIC DERMATITIS ▪ V ery common chronic dermatosis characterized by redness and scaling. ▪ O c c u r s i n r e g i o n s w h e r e t h e sebaceous glands are most active. ▪ Affects 4 – 5 % of the population M i l d e r f o r m s i n t h e s c a l p r e f e r r e d t o a s d a n d r u f f o r p i t y r i a s i s s i c c a . 71
- 37. SEBORRHOEIC DERMATITIS ▪ Cause not understood ▪ Associatedfactors: ▪ Genetics ▪ Immunosupresion ▪ Pityrosporum ovale( Malassezia furfur)
- 38. 38
- 39. 39
- 40. TREATMENT OF SEBORRHOEIC DERMATITIS ▪ S e l e n i u m sulfide shampoo ▪ Ketoconazole shampoo ▪ Topical steroids ▪ Systemic azoles ▪ UV radiation ▪ Recurrences and remissions are common