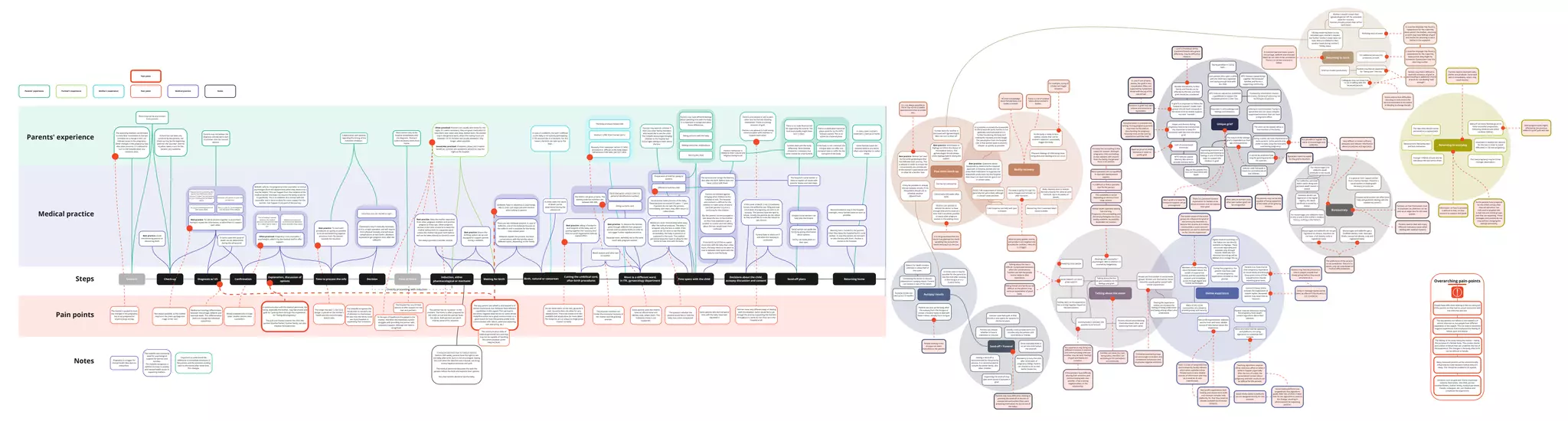
This document outlines the process and experiences of parents going through a stillbirth in Estonia. It discusses the various steps from diagnosis to induction and birth, the options for viewing or spending time with the baby, creating memories, the recovery process for both mother and partner, and support services available. It also notes pain points such as lack of support for partners, difficulties communicating with grieving parents, and barriers due to limited resources or standard practices not accommodating individual needs.