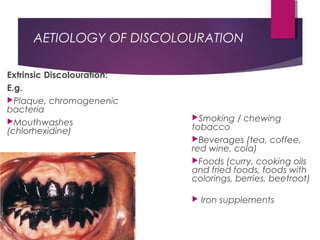
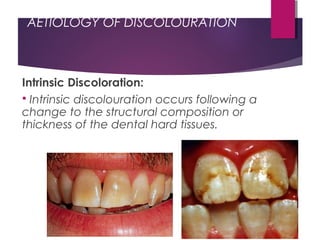
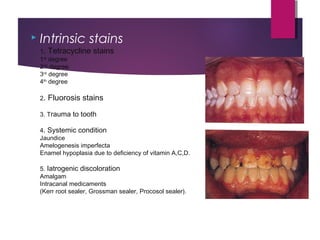
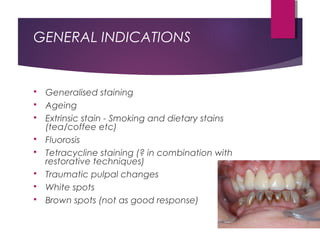
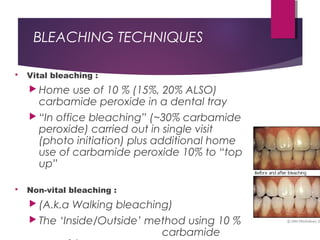
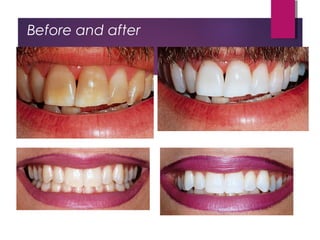
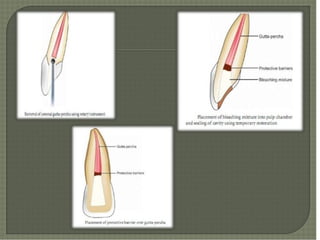
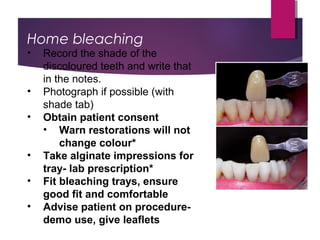
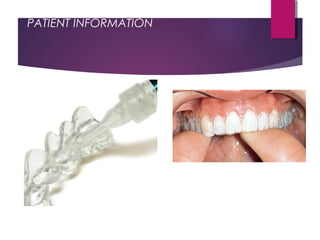
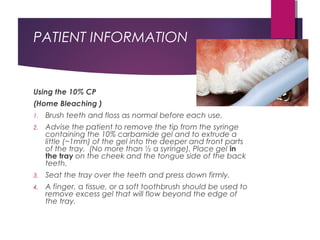
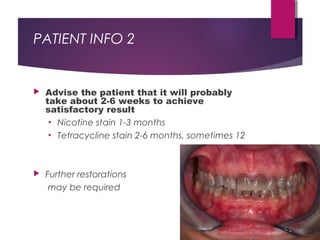
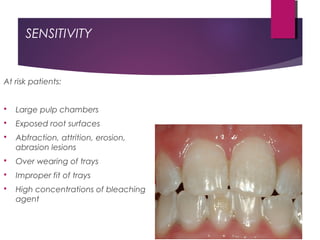
This document discusses tooth colour and bleaching techniques. It begins by describing the natural colours of teeth and factors that affect tooth colour. It then discusses intrinsic and extrinsic tooth discolouration, their causes, and management options. Bleaching techniques are summarized, including home bleaching using trays, in-office bleaching, and non-vital bleaching. Risks and management of sensitivity are also covered. Lasers can be used to enhance bleaching but have higher costs and potential sensitivity risks.