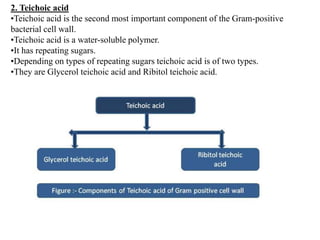
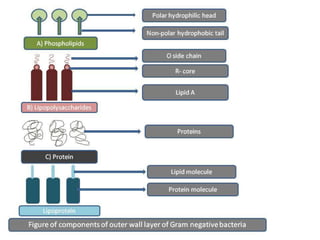
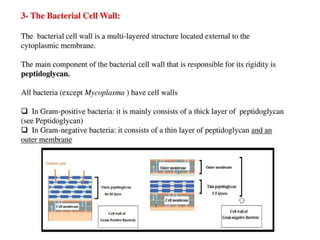
This document defines and describes several important bacteria. It discusses their classification (e.g. Gram-positive/negative), morphology, role in disease, and treatment approaches. Key bacteria mentioned include Clostridium difficile, Staphylococcus aureus (including MRSA), Streptococcus pneumoniae, Escherichia coli, Helicobacter pylori, Mycobacterium tuberculosis, and Neisseria gonorrhoeae. The document provides details on their pathogenic mechanisms, antibiotic resistance patterns, and recommended treatment regimens.