Avascular Necrosis Of Femoral Head.pptx
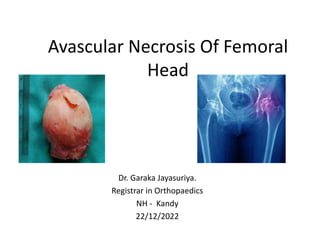
- 1. Avascular Necrosis Of Femoral Head Dr. Garaka Jayasuriya. Registrar in Orthopaedics NH - Kandy 22/12/2022
- 2. Outline • Introduction. • Classification • Etiology • Pathogenesis • Clinical presentation • Investigations • Management • Prognosis
- 4. • Also known as Hip Osteonecrosis. • It represents a condition caused by reduced blood flow to the femoral head secondary to a variety of risk factors such as a • Traumatic event, • Sickle cell disease, • Steroid use • Alcoholism, • Autoimmune disorders, • Hypercoagulable states
- 5. • Accounts for 10% of total hip arthroplaty. • Male > females. • Bilateral hips involved 80% of cases.
- 6. Pathogenesis 1. Traumatic AVN of Hip 2. Idiopathic AVN of Hip
- 7. Traumatic AVN • Due to injury of femoral head blood supply. (medial femoral circumflex) • AVN rates of specific traumatic injuries Femoral head fracture: 75-100% Basicervical fracture: 50% Cervicotrochanteric fracture: 25% Hip dislocation: 2-40% (2-10% if reduced within 6 hrs) Intertrochanteric fracture: rare
- 8. • Higher risk of AVN with greater initial displacement and poor reduction. • Decompression of intracapsular hematoma may reduce risk. • Quicker time to reduction may reduce risk.
- 9. Idiopathic AVN • Coagulation of the intraosseous microcirculation • Venous thrombosis • Retrograde arterial occlusion • Intraosseous hypertension • Decreased blood flow to femoral head • AVN of femoral head • Chondral fracture and collapse
- 10. Risk factors Direct causes indirect causes Irradiation Trauma Hematologic diseases (leukemia, lymphoma) Dysbaric disorders (decompression sickness, "the bends") - caisson disease Marrow-replacing diseases (e.G. Gaucher's disease) Sickle cell diseas alcoholism hypercoagulable states steroids (either endogenous or exogenous) systemic lupus erythematosus (SLE) transplant patient virus (CMV, hepatitis, HIV, rubella, rubeola, varicella) protease inhibitors (type of HIV medication) idiopathic
- 11. Clinical Presentation Symptoms • Insidious onset of pain • Pain with stairs, inclines, and impact • Pain common in anterior hip O/E • Mostly normal initially • Advanced stages similar to hip oa (limited motion, particularly internal rotation
- 12. Investigations • Diagnosis can be made with radiological imaging. • X rays - Moderate/late disease. – Ap hip – frog-lateral of hip – AP and lateral of contralateral hip • MRI - To detect early or subclinical osteonecrosis. – Highest sensitivity (99%) and specificity (99%) • Bone scan
- 13. Ficat classification Stage Clinical features Plain radiograph X ray MRI Bone scan 0 nil normal normal I pain typically in the groin normal or minor osteopenia edema increased uptake II pain and stiffness mixed osteopenia and/or sclerosis and/or subchondral cysts, without any subchondral lucency geographic defect III pain and stiffness +/- radiation to knee and limp crescent sign and eventual cortical collapse same as plain radiograph IV pain and limp end-stage with evidence of secondary degenerative change same as plain radiograph
- 15. Management Goals of Treatment- 1. observation with management of the underlying systemic conditions. 2. Operative management is indicated for advanced disease with presence of…… - Subchondral collapse - Femoral head flattening - Degenerative joint disease
- 16. Non operative Management Bisphosphonates • Indicated for pre collapse AVN (ficat stages 0-II). • Lack of evidence. • Alendronate, Zolindranate etc..
- 18. Operative managements 1. Core decompression with or without bone grafting. 2. Rotational osteotomy. 3. Curettage and bone grafting through mont trapdoor technique or merle d'aubigne lightbulb technique. 4. Vascularized free-fibula transfer. 5. Total hip replacement. 6. Total hip resurfacing. 7. Hip arthrodesis.
- 19. Core decompression with or without bone grafting.
- 25. Hip arthrodesis
- 26. Post op plan…
- 27. Prognosis • Risk of femoral head collapse with osteonecrosis is based on the modified Kerboul combined necrotic angle. • calculated by adding the arc of the femoral head necrosis on a mid-sagittal and mid-coronal MR images.
- 28. • Low-risk group = combined necrotic angle less than 190° • Moderate-risk group = combined necrotic angle between 190° and 240° • High-risk group = combined necrotic angle of more than 240°
- 29. Case - 1 • 47 years old female • C/o L/ Hip Pain for 6/52 Hx of fall 3/12 No constitutional symptoms No PMH • O/E Antalgic limping gait No LLD Painful passive movements
- 30. • Blood Ix Esr 37 RF 18
- 31. • X rays
- 32. • MRI
- 35. Case - 2 15 y old boy. C/o L/ Hip pain and difficulty in walking -3 /12 Hx of slipped and fall 3/12 No constitutional symptoms PMH - none
- 36. O/E Limping gait. LLD- 4cm R>L. painful passive joint movements. Ix FBC, CRP, ESR – normal
- 37. X Ray
- 38. • Diagnosis. Perthes disease. Management shelf osteotomy
- 39. Summary • AVN is diagnosed always retrospectively. • Therefore no primary preventive measures. • Early diagnosis may reduce collapse of articular surface. • Management will be depended on… • Severity of AVN • Age of the Patient • Demand of the Patient • Comorbidities