Arthritis Document Sharing
•Download as PPTX, PDF•
0 likes•202 views
The Singapore Resource For Arthritis Treatment including osteoarthritis, rheumatoid arthritis and related conditions. We aim to be a comprehensive resource on the best available options to help patients with arthritis in Singapore.
Report
Share
Report
Share
Recommended
Arthritis and homeopathy Treatment

Arthritis is a form of joint disorder that involves inflammation in one or more joints. There are over 100 different forms of arthritis.
Purvi shah tendonitis ppt

Tendonitis details and it's physiotherapy management.
It is define as inflammation of the tendon, tendonitis occur due to overuse and trauma. Depending upon involvement of tendon special test are used. it is treated with PRICE protocol.
Fe guide

This document provides an outline of topics to be covered in a Health Science final exam, including: 1) presentations on healthy foundations, environmental science, and infectious diseases; 2) the skeletal system including bone structure and types of joints; 3) the muscular system covering muscle types and location; 4) the circulatory system such as blood vessels and heart function; 5) the respiratory system and breathing process; and 6) the nervous system detailing neurons, the central and peripheral nervous systems, and the autonomic and somatic systems.
Radial Tunnel Syndrome Can Further Cause Of Elbow Arthritis & Stiffness

The wrist and hand suffers many symptoms associated with the several tunnels that tendons, nerves, and blood vessels pass through. One of the many symptoms is Radial tunnel syndrome that one suffers due to an increased pressure on the radial nerve running by the bones and muscles of the forearm and elbow.
Elbow wristhand and wrist2010

The document summarizes anatomy and common injuries of the elbow, wrist, and hand. It describes the bones, joints, muscles, ligaments, and tendons involved in movement of the elbow, wrist, and fingers. It then lists and explains common injuries in these areas such as fractures, dislocations, sprains, tendonitis, and other repetitive stress injuries affecting bones, joints, muscles, and tendons. Movement of the elbow, wrist, and fingers is also outlined.
Biology Lesson 7.2

The document summarizes the bones of the appendicular skeleton, including:
- The pectoral and pelvic girdles connect the upper and lower limbs to the axial skeleton.
- The bones of the upper limbs are the humerus, radius, ulna, carpals, metacarpals, and phalanges.
- The bones of the lower limbs are the femur, tibia, fibula, tarsals, metatarsals, and phalanges.
- Each region contains bones that allow for movement and connection between limbs and body.
Credi Bone & Joints Clinic

Do you find any or such kind of problems in your bones or joints, then just book an appointment with a well qualified and experienced doctor in Delhi NCR at http://www.credihealth.com
Stem cell therapy for knee pain

Treatment for knee injuries & joint pain might involve surgery & lengthy recovery times. For more info visit
http://healthfirstmagazine.blogspot.com/2016/09/stem-cell-therapy-for-knee-pain.html
Recommended
Arthritis and homeopathy Treatment

Arthritis is a form of joint disorder that involves inflammation in one or more joints. There are over 100 different forms of arthritis.
Purvi shah tendonitis ppt

Tendonitis details and it's physiotherapy management.
It is define as inflammation of the tendon, tendonitis occur due to overuse and trauma. Depending upon involvement of tendon special test are used. it is treated with PRICE protocol.
Fe guide

This document provides an outline of topics to be covered in a Health Science final exam, including: 1) presentations on healthy foundations, environmental science, and infectious diseases; 2) the skeletal system including bone structure and types of joints; 3) the muscular system covering muscle types and location; 4) the circulatory system such as blood vessels and heart function; 5) the respiratory system and breathing process; and 6) the nervous system detailing neurons, the central and peripheral nervous systems, and the autonomic and somatic systems.
Radial Tunnel Syndrome Can Further Cause Of Elbow Arthritis & Stiffness

The wrist and hand suffers many symptoms associated with the several tunnels that tendons, nerves, and blood vessels pass through. One of the many symptoms is Radial tunnel syndrome that one suffers due to an increased pressure on the radial nerve running by the bones and muscles of the forearm and elbow.
Elbow wristhand and wrist2010

The document summarizes anatomy and common injuries of the elbow, wrist, and hand. It describes the bones, joints, muscles, ligaments, and tendons involved in movement of the elbow, wrist, and fingers. It then lists and explains common injuries in these areas such as fractures, dislocations, sprains, tendonitis, and other repetitive stress injuries affecting bones, joints, muscles, and tendons. Movement of the elbow, wrist, and fingers is also outlined.
Biology Lesson 7.2

The document summarizes the bones of the appendicular skeleton, including:
- The pectoral and pelvic girdles connect the upper and lower limbs to the axial skeleton.
- The bones of the upper limbs are the humerus, radius, ulna, carpals, metacarpals, and phalanges.
- The bones of the lower limbs are the femur, tibia, fibula, tarsals, metatarsals, and phalanges.
- Each region contains bones that allow for movement and connection between limbs and body.
Credi Bone & Joints Clinic

Do you find any or such kind of problems in your bones or joints, then just book an appointment with a well qualified and experienced doctor in Delhi NCR at http://www.credihealth.com
Stem cell therapy for knee pain

Treatment for knee injuries & joint pain might involve surgery & lengthy recovery times. For more info visit
http://healthfirstmagazine.blogspot.com/2016/09/stem-cell-therapy-for-knee-pain.html
Knee joint

The knee joint is the largest synovial joint in the body. It is composed of three bones: the femur, tibia, and patella. The knee joint has two articulations: the tibiofemoral joint between the femur and tibia, and the patellofemoral joint between the patella and femur. The knee joint is a compound synovial joint, with the tibiofemoral joint being a hinge type and the patellofemoral joint being a plane type. The knee joint is surrounded by ligaments such as the ACL and PCL, and contains a synovial fluid within its capsule. It also contains menisci that act as cushions and increase stability.
Kneejoint2

The knee joint is a synovial joint that allows for flexion and extension. It involves the lower end of the femur articulating with the upper end of the tibia and the posterior surface of the patella. The joint is surrounded by a fibrous capsule with thickened medial and lateral collateral ligaments. Within the joint cavity are two cruciate ligaments and two menisci that help stabilize the joint. The knee joint receives nerve supply from four sources and has an interconnecting network of blood vessels around it to provide circulation.
Presentation on Joints (Medical)

Osteoarthritis is a common joint disease that affects many sites in the body including the hands, knees, and hips. The incidence of osteoarthritis is increasing due to an aging population and rising obesity rates. There are many risk factors for osteoarthritis including age, female sex, genetics, obesity, joint injury, and abnormalities in joint shape. Local factors in the joint environment like muscle weakness, malalignment, and excessive or injurious joint loading can also increase the risk or progression of osteoarthritis. Accurately diagnosing and grading osteoarthritis involves both clinical assessment and radiographic evaluation using scales like the Kellgren-Lawrence grading system.
Osteoarthritis

This document provides an overview of osteoarthritis of the knee, including definition, risk factors, clinical features, diagnosis, treatment options, and surgical considerations. It defines osteoarthritis as cartilage failure induced by genetic and biomechanical factors. Risk factors include age, obesity, injury history. Clinical diagnosis is based on symptoms of pain and stiffness, physical exam findings of crepitus and limited range of motion. Treatment includes weight loss, exercise, braces, medications like acetaminophen, NSAIDs, and injections. Surgery such as arthroscopic debridement or joint replacement may be considered for advanced cases.
Surgical anatomy of knee joint

The knee joint is the largest and most complicated joint in the body. It allows for both flexion and extension as well as some rotational movement. The knee joint is formed by the articulation of the femoral condyles and tibial plateaus. It contains two menisci that act as shock absorbers and help with joint lubrication. Stability is provided by ligaments like the ACL, PCL, MCL and LCL as well as dynamic stabilizers like the quadriceps muscles. Proper functioning of the knee relies on the intricate interplay of its bony architecture and soft tissue structures.
Osteoarthritis and total joint replacement.ppt (1)

Osteoarthritis and Total Joint Replacement: Risk Factors, Prevention, and Treatment, and the Effects on Sensory Mechanisms Encountered by Osteoarthritic Total Joint Replacement Patients. This document discusses osteoarthritis, including risk factors like age and obesity, common symptoms like joint pain and stiffness, diagnostic methods like x-rays, and treatment options like physical therapy, medications, joint replacements and resurfacing. It also covers changes to sensory systems like vision and balance that can increase fall risks for osteoarthritic patients and accelerate the need for joint replacement surgery.
The pathophysiology of osteoarthritis

Osteoarthritis is characterized by cartilage loss, synovial thickening, and bone changes. It commonly affects the knees, hands, and hips. While age is a risk factor, osteoarthritis has both inflammatory and mechanical components and is influenced by hereditary, constitutional, and environmental factors like obesity and joint injury. Excess weight places mechanical stress on cartilage and adipose tissue may contribute through inflammatory cytokines. Osteoarthritis is now considered a distinct disease entity rather than simply wear and tear of aging.
Knee joint

The knee joint is a complex synovial joint formed by the fusion of the femur, tibia, and patella. It allows for flexion, extension, and rotation. The knee joint is supported by numerous ligaments including the anterior and posterior cruciate ligaments. It contains menisci to deepen the tibial surfaces and distribute weight. The knee joint has a synovial membrane and 13 bursae to reduce friction.
Osteoarthritis

This document provides an overview of osteoarthritis (OA), including its etiology, diagnosis, and treatment options. It discusses how OA is the breakdown of articular cartilage in a joint. Risk factors include mechanical damage from injury or excess weight, genetics, and residual effects from other arthritic conditions. Diagnosis involves assessing symptoms, physical exam findings, and imaging like x-rays. Conservative treatment includes weight loss, physical therapy, bracing, topical NSAIDs, nutraceuticals like glucosamine and chondroitin, and injections. Surgery is not usually recommended when OA is the sole diagnosis.
Osteo-arthritis Knee, strategies for management

Strategies for management of Osteo-arthritis of knee. A talk given by Dr.A.K.Venkatachalam at the Joint Replacement conclave in Mumbai.
Patellofemoral Pain Syndrome

This document discusses patellofemoral pain syndrome (PFPS). PFPS is characterized by anterior knee pain that is most common in young, active populations. It is typically caused by an imbalance of forces across the patellofemoral joint from issues like increased Q-angle, foot overpronation, and weakness of the vastus medialis obliquus muscle. Symptoms include pain around or behind the kneecap that is aggravated by activities involving knee bending like squatting or going up and down stairs. Treatment focuses on reducing pain/inflammation, addressing contributing biomechanical factors, and strengthening exercises for the quadriceps muscles.
Patello femoral joint - MRI

1) The patellofemoral joint is complex with requirements for normal function dependent on the congruent relationship between the patella and trochlear groove. Developmental or acquired alterations to the joint surface geometry are associated with patellar instability, chondromalacia patella, and anterior knee pain.
2) Trochlear dysplasia, patella alta (high riding patella), and excessive lateralization of the tibial tuberosity are the most important factors predisposing to patellar instability. Trochlear dysplasia can be classified into types A through D based on the shape of the trochlear groove.
3) Measurements of the patella, tro
chondromalacia patellae 

Chondromalacia patellae, also known as runner's knee, is a softening and roughening of the cartilage under the kneecap caused by mechanical overload of the patellofemoral joint. Symptoms include pain in front of or beneath the kneecap that is aggravated by activity like climbing stairs. Examination may reveal tenderness under the kneecap edge or crepitus with knee movement. Conservative treatments include rest, ice, strengthening exercises, and anti-inflammatory medication. Surgery to realign or elevate the patella may be considered if conservative treatments fail after 6 months.
Patellofemoral pain syndrome (pfps)

This document summarizes the pathomechanics of patellofemoral pain syndrome (PFPS). It describes the anatomy and biomechanics of the patellofemoral joint. Abnormal tracking of the patella, such as lateral displacement or tilt, can increase stress on the joint and cause pain. Contributing factors include remote factors like weakness of the vastus medialis obliquus muscle, tightness of the lateral retinaculum, and pronated or supinated feet. Addressing these intrinsic and extrinsic factors can help reduce patellofemoral joint loads and pain.
Patellofemoral disorders

This document discusses patellofemoral disorders, including their anatomy, biomechanics, pathology, and treatment. It describes the anatomy of the patella and trochlea, as well as medial and lateral stabilizers. Biomechanics discussed include joint reaction forces, contact areas and pressures. Pathologies include traumatic injuries, atraumatic causes like chondromalacia and malalignment syndromes. Treatment depends on factors like age, cartilage damage, and underlying causes; it ranges from conservative options to various surgical procedures. The take home message is that patellofemoral disorders require careful evaluation of the whole limb and conservative treatment first before considering surgery.
1. biomechanics of the knee joint basics

This document provides an overview of the biomechanics of the knee complex. It describes the knee as the largest and most complex joint, consisting of the tibiofemoral and patellofemoral joints. The knee functions to flex and extend the leg, support body weight, and facilitate locomotion. Key components include the articular surfaces, menisci, capsule, collateral and cruciate ligaments, muscles, bursae, and plicae. The document outlines the roles and mechanics of each of these structures, as well as common injuries associated with the knee.
Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...

Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...National University of Health Sciences
Current Concepts
in
Patellofemoral Pain Syndrome:
Treatment and Rehabilitation by Dale J. Buchberger, MS, PT, DC, CSCS, DACBSP.Biomechanics of knee complex 8 patellofemoral joint

This document discusses the biomechanics of the patellofemoral joint. It describes the anatomy of the patella and its articulation with the femur. As the knee flexes and extends, the patella translates and rotates in complex motions to maintain contact within the femoral groove. The patellofemoral joint experiences high stresses from quadriceps forces, especially between 30-90 degrees of flexion when contact area is increasing. Several mechanisms help minimize stresses on the joint.
3. biomechanics of Patellofemoral joint

The patellofemoral joint is one of the most incongruent joints in the body. It depends on static structures like the lateral lip of the femoral condyle and the length of the patellar tendon for stability. Forces through the joint increase significantly during activities like squatting or ascending stairs. Pathologies of the patellofemoral joint can include osteoarthritis, ligament injuries, meniscal tears, and patellofemoral pain syndrome resulting from an imbalance of forces through the joint.
Knee Joint Anatomy

The knee joint is the largest and most complex joint in the body. It consists of three joints: the medial and lateral condylar joints between the femur and tibia, and the patellofemoral joint between the femur and patella. Key structures include the cruciate ligaments which provide stability, menisci which absorb shock and distribute force, and synovial membrane which lines the joint space. The document provides detailed descriptions of the articular surfaces, ligaments, bursae, and other anatomical structures that make up the knee joint.
Arthritis details

Arthritis is a term used to describe over 100 medical conditions that affect the joints and cause pain and stiffness. The most common types are osteoarthritis and rheumatoid arthritis. Osteoarthritis generally affects elderly patients and occurs when cartilage breaks down over time. Rheumatoid arthritis is an inflammatory condition where the immune system attacks the joints. Some forms can affect younger people. The symptoms depend on the type of arthritis but may include pain, stiffness, swelling and fatigue. While there is no cure for most types of arthritis, treatments can help reduce symptoms and improve quality of life. These include medications, physical therapy, exercise and maintaining a healthy diet and weight.
Arthritis details

Arthritis is a term used to describe over 100 medical conditions that cause pain and inflammation in the joints. The most common forms are osteoarthritis and rheumatoid arthritis. Osteoarthritis generally affects elderly patients and causes cartilage in the joints to wear down over time, while rheumatoid arthritis is an autoimmune disorder that causes swelling and damage to joint lining. Some other types of arthritis include infectious arthritis caused by bacteria/viruses, and juvenile rheumatoid arthritis which affects children. Symptoms vary depending on the type but can include joint pain, stiffness, swelling and reduced mobility. Treatment involves medications like NSAIDs to reduce inflammation, physical/occupational therapy, weight loss if overweight, and home remedies such as supplements and herbal remedies
More Related Content
Viewers also liked
Knee joint

The knee joint is the largest synovial joint in the body. It is composed of three bones: the femur, tibia, and patella. The knee joint has two articulations: the tibiofemoral joint between the femur and tibia, and the patellofemoral joint between the patella and femur. The knee joint is a compound synovial joint, with the tibiofemoral joint being a hinge type and the patellofemoral joint being a plane type. The knee joint is surrounded by ligaments such as the ACL and PCL, and contains a synovial fluid within its capsule. It also contains menisci that act as cushions and increase stability.
Kneejoint2

The knee joint is a synovial joint that allows for flexion and extension. It involves the lower end of the femur articulating with the upper end of the tibia and the posterior surface of the patella. The joint is surrounded by a fibrous capsule with thickened medial and lateral collateral ligaments. Within the joint cavity are two cruciate ligaments and two menisci that help stabilize the joint. The knee joint receives nerve supply from four sources and has an interconnecting network of blood vessels around it to provide circulation.
Presentation on Joints (Medical)

Osteoarthritis is a common joint disease that affects many sites in the body including the hands, knees, and hips. The incidence of osteoarthritis is increasing due to an aging population and rising obesity rates. There are many risk factors for osteoarthritis including age, female sex, genetics, obesity, joint injury, and abnormalities in joint shape. Local factors in the joint environment like muscle weakness, malalignment, and excessive or injurious joint loading can also increase the risk or progression of osteoarthritis. Accurately diagnosing and grading osteoarthritis involves both clinical assessment and radiographic evaluation using scales like the Kellgren-Lawrence grading system.
Osteoarthritis

This document provides an overview of osteoarthritis of the knee, including definition, risk factors, clinical features, diagnosis, treatment options, and surgical considerations. It defines osteoarthritis as cartilage failure induced by genetic and biomechanical factors. Risk factors include age, obesity, injury history. Clinical diagnosis is based on symptoms of pain and stiffness, physical exam findings of crepitus and limited range of motion. Treatment includes weight loss, exercise, braces, medications like acetaminophen, NSAIDs, and injections. Surgery such as arthroscopic debridement or joint replacement may be considered for advanced cases.
Surgical anatomy of knee joint

The knee joint is the largest and most complicated joint in the body. It allows for both flexion and extension as well as some rotational movement. The knee joint is formed by the articulation of the femoral condyles and tibial plateaus. It contains two menisci that act as shock absorbers and help with joint lubrication. Stability is provided by ligaments like the ACL, PCL, MCL and LCL as well as dynamic stabilizers like the quadriceps muscles. Proper functioning of the knee relies on the intricate interplay of its bony architecture and soft tissue structures.
Osteoarthritis and total joint replacement.ppt (1)

Osteoarthritis and Total Joint Replacement: Risk Factors, Prevention, and Treatment, and the Effects on Sensory Mechanisms Encountered by Osteoarthritic Total Joint Replacement Patients. This document discusses osteoarthritis, including risk factors like age and obesity, common symptoms like joint pain and stiffness, diagnostic methods like x-rays, and treatment options like physical therapy, medications, joint replacements and resurfacing. It also covers changes to sensory systems like vision and balance that can increase fall risks for osteoarthritic patients and accelerate the need for joint replacement surgery.
The pathophysiology of osteoarthritis

Osteoarthritis is characterized by cartilage loss, synovial thickening, and bone changes. It commonly affects the knees, hands, and hips. While age is a risk factor, osteoarthritis has both inflammatory and mechanical components and is influenced by hereditary, constitutional, and environmental factors like obesity and joint injury. Excess weight places mechanical stress on cartilage and adipose tissue may contribute through inflammatory cytokines. Osteoarthritis is now considered a distinct disease entity rather than simply wear and tear of aging.
Knee joint

The knee joint is a complex synovial joint formed by the fusion of the femur, tibia, and patella. It allows for flexion, extension, and rotation. The knee joint is supported by numerous ligaments including the anterior and posterior cruciate ligaments. It contains menisci to deepen the tibial surfaces and distribute weight. The knee joint has a synovial membrane and 13 bursae to reduce friction.
Osteoarthritis

This document provides an overview of osteoarthritis (OA), including its etiology, diagnosis, and treatment options. It discusses how OA is the breakdown of articular cartilage in a joint. Risk factors include mechanical damage from injury or excess weight, genetics, and residual effects from other arthritic conditions. Diagnosis involves assessing symptoms, physical exam findings, and imaging like x-rays. Conservative treatment includes weight loss, physical therapy, bracing, topical NSAIDs, nutraceuticals like glucosamine and chondroitin, and injections. Surgery is not usually recommended when OA is the sole diagnosis.
Osteo-arthritis Knee, strategies for management

Strategies for management of Osteo-arthritis of knee. A talk given by Dr.A.K.Venkatachalam at the Joint Replacement conclave in Mumbai.
Patellofemoral Pain Syndrome

This document discusses patellofemoral pain syndrome (PFPS). PFPS is characterized by anterior knee pain that is most common in young, active populations. It is typically caused by an imbalance of forces across the patellofemoral joint from issues like increased Q-angle, foot overpronation, and weakness of the vastus medialis obliquus muscle. Symptoms include pain around or behind the kneecap that is aggravated by activities involving knee bending like squatting or going up and down stairs. Treatment focuses on reducing pain/inflammation, addressing contributing biomechanical factors, and strengthening exercises for the quadriceps muscles.
Patello femoral joint - MRI

1) The patellofemoral joint is complex with requirements for normal function dependent on the congruent relationship between the patella and trochlear groove. Developmental or acquired alterations to the joint surface geometry are associated with patellar instability, chondromalacia patella, and anterior knee pain.
2) Trochlear dysplasia, patella alta (high riding patella), and excessive lateralization of the tibial tuberosity are the most important factors predisposing to patellar instability. Trochlear dysplasia can be classified into types A through D based on the shape of the trochlear groove.
3) Measurements of the patella, tro
chondromalacia patellae 

Chondromalacia patellae, also known as runner's knee, is a softening and roughening of the cartilage under the kneecap caused by mechanical overload of the patellofemoral joint. Symptoms include pain in front of or beneath the kneecap that is aggravated by activity like climbing stairs. Examination may reveal tenderness under the kneecap edge or crepitus with knee movement. Conservative treatments include rest, ice, strengthening exercises, and anti-inflammatory medication. Surgery to realign or elevate the patella may be considered if conservative treatments fail after 6 months.
Patellofemoral pain syndrome (pfps)

This document summarizes the pathomechanics of patellofemoral pain syndrome (PFPS). It describes the anatomy and biomechanics of the patellofemoral joint. Abnormal tracking of the patella, such as lateral displacement or tilt, can increase stress on the joint and cause pain. Contributing factors include remote factors like weakness of the vastus medialis obliquus muscle, tightness of the lateral retinaculum, and pronated or supinated feet. Addressing these intrinsic and extrinsic factors can help reduce patellofemoral joint loads and pain.
Patellofemoral disorders

This document discusses patellofemoral disorders, including their anatomy, biomechanics, pathology, and treatment. It describes the anatomy of the patella and trochlea, as well as medial and lateral stabilizers. Biomechanics discussed include joint reaction forces, contact areas and pressures. Pathologies include traumatic injuries, atraumatic causes like chondromalacia and malalignment syndromes. Treatment depends on factors like age, cartilage damage, and underlying causes; it ranges from conservative options to various surgical procedures. The take home message is that patellofemoral disorders require careful evaluation of the whole limb and conservative treatment first before considering surgery.
1. biomechanics of the knee joint basics

This document provides an overview of the biomechanics of the knee complex. It describes the knee as the largest and most complex joint, consisting of the tibiofemoral and patellofemoral joints. The knee functions to flex and extend the leg, support body weight, and facilitate locomotion. Key components include the articular surfaces, menisci, capsule, collateral and cruciate ligaments, muscles, bursae, and plicae. The document outlines the roles and mechanics of each of these structures, as well as common injuries associated with the knee.
Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...

Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...National University of Health Sciences
Current Concepts
in
Patellofemoral Pain Syndrome:
Treatment and Rehabilitation by Dale J. Buchberger, MS, PT, DC, CSCS, DACBSP.Biomechanics of knee complex 8 patellofemoral joint

This document discusses the biomechanics of the patellofemoral joint. It describes the anatomy of the patella and its articulation with the femur. As the knee flexes and extends, the patella translates and rotates in complex motions to maintain contact within the femoral groove. The patellofemoral joint experiences high stresses from quadriceps forces, especially between 30-90 degrees of flexion when contact area is increasing. Several mechanisms help minimize stresses on the joint.
3. biomechanics of Patellofemoral joint

The patellofemoral joint is one of the most incongruent joints in the body. It depends on static structures like the lateral lip of the femoral condyle and the length of the patellar tendon for stability. Forces through the joint increase significantly during activities like squatting or ascending stairs. Pathologies of the patellofemoral joint can include osteoarthritis, ligament injuries, meniscal tears, and patellofemoral pain syndrome resulting from an imbalance of forces through the joint.
Knee Joint Anatomy

The knee joint is the largest and most complex joint in the body. It consists of three joints: the medial and lateral condylar joints between the femur and tibia, and the patellofemoral joint between the femur and patella. Key structures include the cruciate ligaments which provide stability, menisci which absorb shock and distribute force, and synovial membrane which lines the joint space. The document provides detailed descriptions of the articular surfaces, ligaments, bursae, and other anatomical structures that make up the knee joint.
Viewers also liked (20)
Osteoarthritis and total joint replacement.ppt (1)

Osteoarthritis and total joint replacement.ppt (1)
Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...

Current Concepts in Patellofemoral Pain Syndrome: Treatment and Rehabilitatio...
Biomechanics of knee complex 8 patellofemoral joint

Biomechanics of knee complex 8 patellofemoral joint
Similar to Arthritis Document Sharing
Arthritis details

Arthritis is a term used to describe over 100 medical conditions that affect the joints and cause pain and stiffness. The most common types are osteoarthritis and rheumatoid arthritis. Osteoarthritis generally affects elderly patients and occurs when cartilage breaks down over time. Rheumatoid arthritis is an inflammatory condition where the immune system attacks the joints. Some forms can affect younger people. The symptoms depend on the type of arthritis but may include pain, stiffness, swelling and fatigue. While there is no cure for most types of arthritis, treatments can help reduce symptoms and improve quality of life. These include medications, physical therapy, exercise and maintaining a healthy diet and weight.
Arthritis details

Arthritis is a term used to describe over 100 medical conditions that cause pain and inflammation in the joints. The most common forms are osteoarthritis and rheumatoid arthritis. Osteoarthritis generally affects elderly patients and causes cartilage in the joints to wear down over time, while rheumatoid arthritis is an autoimmune disorder that causes swelling and damage to joint lining. Some other types of arthritis include infectious arthritis caused by bacteria/viruses, and juvenile rheumatoid arthritis which affects children. Symptoms vary depending on the type but can include joint pain, stiffness, swelling and reduced mobility. Treatment involves medications like NSAIDs to reduce inflammation, physical/occupational therapy, weight loss if overweight, and home remedies such as supplements and herbal remedies
Stem Cell Therapy for Osteoarthritis | Dr. David Greene Arizona

The most prevalent kind of arthritis is osteoarthritis, also known as a degenerative joint disease (DJD). As people get older, they are more prone to acquire osteoarthritis. Changes in osteoarthritis often develop gradually over several years, with few exceptions. Dr. David Greene Arizona discusses osteoarthritis in this presentation.
Rheumatoid Arthritis

Rheumatoid arthritis is an autoimmune disorder that causes chronic inflammation of the joints. It most commonly affects small joints in the hands and feet. While the cause is unknown, it occurs when the immune system mistakenly attacks the synovium lining of joints. Women are more likely to develop it than men, and it often begins between ages 40-60. Complications can include osteoporosis, carpal tunnel syndrome, heart and lung problems. Treatment focuses on reducing inflammation and preventing joint damage through medications, physical therapy, exercise and surgery if needed. Managing stress and lifestyle factors may also help relieve symptoms.
What are the four stages of osteoarthritis.pptx

Do you have osteoarthritis? Learn about what to expect throughout the 4 different stages of knee osteoarthritis and the proper treatment for each stage.
Osteoarthritis

There are more than 100 kinds of arthritis, which literally means joint inflammation. According to the Centers for Disease Control and Prevention (CDC), about 50 million Americans are afflicted, and 27 million have osteoarthritis, by far the most common form, especially among older people.
Arthritis Reference.pdf

This document provides an overview of arthritis, including:
- Arthritis is a group of over 100 diseases that cause joint inflammation and pain. The two most common types are osteoarthritis and rheumatoid arthritis.
- Symptoms include joint pain, swelling, stiffness, and reduced mobility. Arthritis is diagnosed through physical exams, imaging tests, and blood tests.
- Treatment options include medications to reduce pain and inflammation, physical therapy, weight loss, exercise, joint braces, and sometimes surgery. Managing arthritis involves finding the right treatment combination to minimize symptoms and joint damage.
Osteoarthritis ayurveda treatment_india

Osteoarthritis is the most common form of arthritis. It is caused by the breakdown of cartilage, Ayurveda has the best treatment for all type of arthritis.
Ayurvedic treatment for arthritis & osteoarthritis ppt

Arthritis is a disease that causes inflammation in the joints and can affect any joint in the body. It is a degenerative condition which means it will get worse over time. There are many different treatment options available, including traditional Western medicine and alternative treatments like Ayurvedic treatments.
Ayurveda is an ancient Indian holistic system of natural healing that has been used for thousands of years to treat various diseases such as arthritis. The treatment mainly consists of massages, dietary changes, and lifestyle changes.
Arthritis

Arthritis is not a normal part of the aging process. Teach people how it happens and how to prevent it.
Four stages of osteoarthritis.pptx

Do you have osteoarthritis? Learn about what to expect throughout the 4 different stages of knee osteoarthritis and the proper treatment for each stage
Osteoarthritis Presentation

Osteoarthritis is a common form of arthritis where cartilage in joints breaks down over time. It causes pain, stiffness, and loss of mobility in joints like the hands, hips, and knees. While there is no cure, treatments can help manage symptoms and maintain activity. For mild cases, initial treatments include exercise, weight loss, heat/cold therapy, and over-the-counter pain relievers. For moderate to severe cases, stronger medications, cortisone shots, and surgery may be needed to relieve pain and disability. Joint replacement surgery can help severely affected patients resume an active lifestyle.
List of 6 best homeopathic medicines for osteoarthritis

Effective homeopathic medicines for arthritis which gives a long term cure to rheumatoid arthritis, osteoarthritis, gout, joints pain, neck pain, back pain, shoulder pain
List of 6 best homeopathic medicines for osteoarthritis

Homeopathic medicines are very highly effective in management of piles and the symptoms associated with it such as pain, bleeding, itching, etc. The point to be emphasized is that the relief of symptoms is obtained with absolute gentleness and without invasion or surgery of any kind. Besides, the condition has high backslide rate taking after surgical treatment, since surgery does not focus on the main drivers such as hereditary inclinations, periodic clogging, and so forth. Homeopathic drugs work at the root level and can change these hereditary inclinations accordingly decreasing odds of backslide and repeat of the condition essentially. Homeopathy treatment reduces the intra abdominal pressure. There are good medicines that relieve constipation which plays major role in developing piles.
6 most common important homeopathy medicines for piles:
Aesculus :
Nux Vomica:
Graphites
Hamamelis
collinsonia,
aesculus
presentation on arthritis

The document provides information about arthritis, including definitions, common types, signs and symptoms, causes, medical and nursing management. It defines arthritis as inflammation of one or more joints and discusses common types like osteoarthritis, rheumatoid arthritis, psoriatic arthritis, and gout. It outlines signs, causes, who is affected, and treatments for these types. The document also discusses analgesics, corticosteroids, opioids and their use in managing arthritis pain and inflammation. Finally, it lists some common nursing diagnoses for arthritis patients and examples of nursing interventions.
Osteoarosteoarthritis nursing managementthritis nursing management

Osteoarthritis is a common joint disease that affects older individuals. It involves the breakdown of cartilage in the joints. Symptoms include joint stiffness, swelling, and pain that worsens with use. X-rays can show cartilage loss and bone changes in the joints. Treatment focuses on education, activity modification, weight loss, medications like acetaminophen and NSAIDs, steroid injections, and sometimes surgery for severe cases. Lifestyle changes and less impactful exercises can help manage symptoms.
Yoga for orthopedic arthritis and osteoporosis

These slides are for Yoga Teachers or students of Yoga for understanding the disease and what Yoga program we can offer to our client when they reach you for help. Although every individual is unique and Yoga Therapy should also be made considering what level of disease they are going through.
Disclaimer: We dont take any responsibility if someone starts to follow the program as mentioned in the PPT for any harm or injury.
Osteoarthritis.ppt

This document provides a comprehensive overview of osteoarthritis, including its definition, causes, risk factors, signs and symptoms, diagnosis, treatment options, self-care strategies, and the role of yoga and complementary therapies. It describes how osteoarthritis results from the breakdown of cartilage in joints, most often affecting the hands, spine, knees and hips. Risk factors include age, genetics, injury and obesity. Treatments include medications, exercise, weight control, and in some cases surgery.
Similar to Arthritis Document Sharing (20)
Stem Cell Therapy for Osteoarthritis | Dr. David Greene Arizona

Stem Cell Therapy for Osteoarthritis | Dr. David Greene Arizona
Ayurvedic treatment for arthritis & osteoarthritis ppt

Ayurvedic treatment for arthritis & osteoarthritis ppt
List of 6 best homeopathic medicines for osteoarthritis

List of 6 best homeopathic medicines for osteoarthritis
List of 6 best homeopathic medicines for osteoarthritis

List of 6 best homeopathic medicines for osteoarthritis
Osteoarosteoarthritis nursing managementthritis nursing management

Osteoarosteoarthritis nursing managementthritis nursing management
Recently uploaded
Hypotension and role of physiotherapy in it

This particular slides consist of- what is hypotension,what are it's causes and it's effect on body, risk factors, symptoms,complications, diagnosis and role of physiotherapy in it.
This slide is very helpful for physiotherapy students and also for other medical and healthcare students.
Here is the summary of hypotension:
Hypotension, or low blood pressure, is when the pressure of blood circulating in the body is lower than normal or expected. It's only a problem if it negatively impacts the body and causes symptoms. Normal blood pressure is usually between 90/60 mmHg and 120/80 mmHg, but pressures below 90/60 are generally considered hypotensive.
TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardso...

TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardso...rightmanforbloodline
TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardson, Verified Chapters 1 - 18, Complete Newest Version
TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardson, Verified Chapters 1 - 18, Complete Newest Version
TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardson, Verified Chapters 1 - 18, Complete Newest VersionGemma Wean- Nutritional solution for Artemia

GEMMA Wean is a high end larval co-feeding and weaning diet aimed at Artemia optimisation and is fortified with a high level of proteins and phospholipids. GEMMA Wean provides the early weaned juveniles with dedicated fish nutrition and is an ideal follow on from GEMMA Micro or Artemia.
GEMMA Wean has an optimised nutritional balance and physical quality so that it flows more freely and spreads readily on the water surface. The balance of phospholipid classes to- gether with the production technology based on a low temperature extrusion process improve the physical aspect of the pellets while still retaining the high phospholipid content.
GEMMA Wean is available in 0.1mm, 0.2mm and 0.3mm. There is also a 0.5mm micro-pellet, GEMMA Wean Diamond, which covers the early nursery stage from post-weaning to pre-growing.
Can coffee help me lose weight? Yes, 25,422 users in the USA use it for that ...

The South Beach Coffee Java Diet is a variation of the popular South Beach Diet, which was developed by cardiologist Dr. Arthur Agatston. The original South Beach Diet focuses on consuming lean proteins, healthy fats, and low-glycemic index carbohydrates. The South Beach Coffee Java Diet adds the element of coffee, specifically caffeine, to enhance weight loss and improve energy levels.
2024 HIPAA Compliance Training Guide to the Compliance Officers

Join us for a comprehensive 90-minute lesson designed specifically for Compliance Officers and Practice/Business Managers. This 2024 HIPAA Training session will guide you through the critical steps needed to ensure your practice is fully prepared for upcoming audits. Key updates and significant changes under the Omnibus Rule will be covered, along with the latest applicable updates for 2024.
Key Areas Covered:
Texting and Email Communication: Understand the compliance requirements for electronic communication.
Encryption Standards: Learn what is necessary and what is overhyped.
Medical Messaging and Voice Data: Ensure secure handling of sensitive information.
IT Risk Factors: Identify and mitigate risks related to your IT infrastructure.
Why Attend:
Expert Instructor: Brian Tuttle, with over 20 years in Health IT and Compliance Consulting, brings invaluable experience and knowledge, including insights from over 1000 risk assessments and direct dealings with Office of Civil Rights HIPAA auditors.
Actionable Insights: Receive practical advice on preparing for audits and avoiding common mistakes.
Clarity on Compliance: Clear up misconceptions and understand the reality of HIPAA regulations.
Ensure your compliance strategy is up-to-date and effective. Enroll now and be prepared for the 2024 HIPAA audits.
Enroll Now to secure your spot in this crucial training session and ensure your HIPAA compliance is robust and audit-ready.
https://conferencepanel.com/conference/hipaa-training-for-the-compliance-officer-2024-updates
Pediatric Emergency Care for Children | Apollo Hospital

Pediatric Emergency Care for Children | Apollo HospitalApollo 24/7 Adult & Paediatric Emergency Services
At Apollo Hospital, Lucknow, U.P., we provide specialized care for children experiencing dehydration and other symptoms. We also offer NICU & PICU Ambulance Facility Services. Consult our expert today for the best pediatric emergency care.
For More Details:
Map: https://cutt.ly/BwCeflYo
Name: Apollo Hospital
Address: Singar Nagar, LDA Colony, Lucknow, Uttar Pradesh 226012
Phone: 08429021957
Opening Hours: 24X7DR SHAMIN EABENSON - JOURNAL CLUB - NEEDLE STICK INJURY

JOURNAL CLUB - NEEDLE STICK INJURY - TOPIC PRESENTED BY DR SHAMIN
CANSA support - Caring for Cancer Patients' Caregivers

International Cancer Survivors Day is celebrated during June, placing the spotlight not only on cancer survivors, but also their caregivers.
CANSA has compiled a list of tips and guidelines of support:
https://cansa.org.za/who-cares-for-cancer-patients-caregivers/
Let's Talk About It: Breast Cancer (What is Mindset and Does it Really Matter?)

Your mindset is the way you make sense of the world around you. This lens influences the way you think, the way you feel, and how you might behave in certain situations. Let's talk about mindset myths that can get us into trouble and ways to cultivate a mindset to support your cancer survivorship in authentic ways. Let’s Talk About It!
Innovative Minds France's Most Impactful Healthcare Leaders.pdf

This edition features a handful of Innovative Minds: France's Most Impactful Healthcare Leaders that are leading us into a better future.
FACIAL NERVE

The facial nerve, also known as cranial nerve VII, is one of the 12 cranial nerves originating from the brain. It's a mixed nerve, meaning it contains both sensory and motor fibres, and it plays a crucial role in controlling various facial muscles, as well as conveying sensory information from the taste buds on the anterior two-thirds of the tongue.
The Power of Superfoods and Exercise.pdf

Healthy Eating Habits:
Understanding Nutrition Labels: Teaches how to read and interpret food labels, focusing on serving sizes, calorie intake, and nutrients to limit or include.
Tips for Healthy Eating: Offers practical advice such as incorporating a variety of foods, practicing moderation, staying hydrated, and eating mindfully.
Benefits of Regular Exercise:
Physical Benefits: Discusses how exercise aids in weight management, muscle and bone health, cardiovascular health, and flexibility.
Mental Benefits: Explains the psychological advantages, including stress reduction, improved mood, and better sleep.
Tips for Staying Active:
Encourages consistency, variety in exercises, setting realistic goals, and finding enjoyable activities to maintain motivation.
Maintaining a Balanced Lifestyle:
Integrating Nutrition and Exercise: Suggests meal planning and incorporating physical activity into daily routines.
Monitoring Progress: Recommends tracking food intake and exercise, regular health check-ups, and provides tips for achieving balance, such as getting sufficient sleep, managing stress, and staying socially active.
Pneumothorax and role of Physiotherapy in it.

This particular slides consist of- what is Pneumothorax,what are it's causes and it's effect on body, risk factors, symptoms,complications, diagnosis and role of physiotherapy in it.
This slide is very helpful for physiotherapy students and also for other medical and healthcare students.
Here is a summary of Pneumothorax:
Pneumothorax, also known as a collapsed lung, is a condition that occurs when air leaks into the space between the lung and chest wall. This air buildup puts pressure on the lung, preventing it from expanding fully when you breathe. A pneumothorax can cause a complete or partial collapse of the lung.
Professional Secrecy: Forensic Medicine Lecture

Professional Secrecy: Forensic Medicine Lecture , Medical jurisprudence
LEAD Innovation Launch_WHO Innovation Initiative.pptx

WHO Innovation Initiative. WHO Innovation Initiative. WHO Innovation Initiative. WHO Innovation Initiative.
Letter to MREC - application to conduct study

Application to conduct study on research title 'Awareness and knowledge of oral cancer and precancer among dental outpatient in Klinik Pergigian Merlimau, Melaka'
Recently uploaded (20)
TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardso...

TEST BANK For Accounting Information Systems, 3rd Edition by Vernon Richardso...
Can coffee help me lose weight? Yes, 25,422 users in the USA use it for that ...

Can coffee help me lose weight? Yes, 25,422 users in the USA use it for that ...
Bringing AI into a Mid-Sized Company: A structured Approach

Bringing AI into a Mid-Sized Company: A structured Approach
2024 HIPAA Compliance Training Guide to the Compliance Officers

2024 HIPAA Compliance Training Guide to the Compliance Officers
Pediatric Emergency Care for Children | Apollo Hospital

Pediatric Emergency Care for Children | Apollo Hospital
chatgptfornlp-230314021506-2f03f614.pdf. 21506-2f03f614.pdf

chatgptfornlp-230314021506-2f03f614.pdf. 21506-2f03f614.pdf
DR SHAMIN EABENSON - JOURNAL CLUB - NEEDLE STICK INJURY

DR SHAMIN EABENSON - JOURNAL CLUB - NEEDLE STICK INJURY
CANSA support - Caring for Cancer Patients' Caregivers

CANSA support - Caring for Cancer Patients' Caregivers
Let's Talk About It: Breast Cancer (What is Mindset and Does it Really Matter?)

Let's Talk About It: Breast Cancer (What is Mindset and Does it Really Matter?)
Innovative Minds France's Most Impactful Healthcare Leaders.pdf

Innovative Minds France's Most Impactful Healthcare Leaders.pdf
LEAD Innovation Launch_WHO Innovation Initiative.pptx

LEAD Innovation Launch_WHO Innovation Initiative.pptx
Arthritis Document Sharing
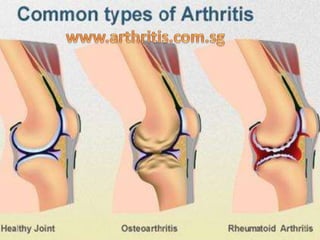
- 2. Osteoarthritis and rheumatoid arthritis have different causes, risk factors, and effects on the body: • Osteoarthritis pain, stiffness, or inflammation most frequently appears in the hips, knees, and hands. • Rheumatoid arthritis commonly affects the hands and wrists but can also affect areas of the body other than the joints.
- 4. Osteoarthritis And Rheumatoid Arthritis Often Share Common Symptoms: Joint pain Stiffness Inflammation or swelling
- 5. Characteristics Of Rheumatoid Arthritis And Osteoarthritis Characteristic Rheumatoid arthritis Osteoarthritis Age at which the condition starts It may begin any time in life. It usually begins later in life. Speed of onset Relatively rapid, over weeks to months Slow, over years Joint symptoms Joints are painful, swollen, and stiff. Joints ache and may be tender but have little or no swelling. Pattern of joints that are affected It often affects small and large joints on both sides of the body (symmetrical), such as both hands, both wrists or elbows, or the balls of both feet. Symptoms often begin on one side of the body and may spread to the other side. Symptoms begin gradually and are often limited to one set of joints, usually the finger joints closest to the fingernails or the thumbs, large weight-bearing joints (hips, knees), or the spine. Duration of morning stiffness Morning stiffness lasts longer than 1 hour. Morning stiffness lasts less than 1 hour. Stiffness returns at the end of the day or after periods of activity. Presence of symptoms affecting the whole body (systemic) Frequent fatigue and a general feeling of being ill are present. Whole-body symptoms are not present.
- 6. Arthritis.com.sg was founded on the principle that arthritis is a major and difficult problem facing many people today. We understand that successful treatment is difficult and may require a correct complement of doctors, medications, supplements, and complementary healthcare providers. We aim to be a comprehensive resource on the best available options available to help patients with arthritis in Singapore.
- 7. 360 Orchard Road, #09-10, International Building Singapore 238869 Ph: 67355368