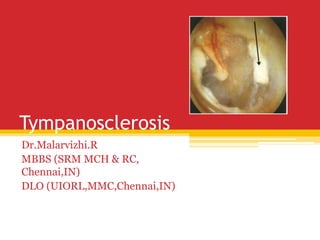
Tympanosclerosis
- 1. Tympanosclerosis Dr.Malarvizhi.R MBBS (SRM MCH & RC, Chennai,IN) DLO (UIORL,MMC,Chennai,IN)
- 2. Tympanosclerosis • Definition ▫ Tympanosclerosis is characterized by hyaline degeneration of the fibrous layer of the tympanic membrane and the middle ear mucosa. (Shambough) ▫ Refers to hyaline deposits of acellular material visible as white plaques in the tympanic membrane and as white nodular deposits in the submucosal layers of the middle ear on otoscopy.(Scott brown)
- 3. • Isolated involvement of the tympanic membrane is more common and termed as Myringosclerosis. • Tympanosclerotic plaques may also be present within the middle ear cleft and mastoid • Is irreversible • Results from infection or inflammation of middle ear space.
- 5. Pathology • Is the end result of a healing process in which collagen in fibrous tissue hyalinizes, loses its structure and becomes fused into a homogenous mass. • Thereafter , calcification and ossification may occur to a variable extent.
- 6. Connective tissue degeneration fibrolysis Hyalinization (hypovascularization) Change in pH Ca phosphate precipitates Dystrophic calcification Fibrocyte degeneration Extracellular matrix vesicles With ca & po4 ions supersaturation Ca phosphates precipitates Matrix vesicle calcification (calcospherules) Calcified tympanosclerotic plaques (Tympanosclerosis)
- 7. Theories of pathogenesis • Local immunologic hypersensitivity • Increased oxygen concentration in the middle ear with exposure to oxygen radicals • Local inflammatory activity • Though pathogenesis is not clear, Chronic Otitis Media is a prerequisite • Tympanosclerotic ears are free of active suppuration
- 8. Types • Depending on integrity of TM ▫ Closed & Open • Examination of plaque under microscope ▫ Soft creamy type with cartilaginous texture, which on removal tends to peel off in onion layers ▫ Pure white, hard and dense plaque • Histologically ▫ Noninvasive superficial called as sclerosing mucositis. Adjacent mucosa and peristeum intact ▫ Deeper invasive called as osteoclastic mucoperiostitis. Destruction of underlying bone .
- 11. • Plaques occur in areas where ▫ Gland population is lowest ▫ Cilia are scanty Deposits tend to form where inflammatory exudates are liable to be trapped during the course of infection; the absence of effective ciliary function together with reduction in glandular secretion and subsequently they get organized in these narrow spaces and possibly convert into tympanosclerotic plaques.
- 12. • Most common sites ▫ Stapes oval window area ▫ Sub fallopian groove ▫ Upper promontory ▫ Epitympanum
- 13. • Symptoms ▫ Asymptomatic ▫ Deafness ▫ Tinnnitus occasionally • Signs ▫ May have normal tympanic membrane with chalky white areas ▫ May have features of glue ear /csom ▫ Rinnne- negative ▫ Weber – lateralized to same ear ▫ ABC normal
- 14. Investigations • PTA- mild to moderate conductive hearing loss • Impedance audiogram- A ‘s’ curve • X Ray of mastoids- poor pneumatization • CT temporal bones – USUALLY NOT INDICATED, reveals unifocal or multifocal masses or linear calcific densities in middle ear , epitympanum or in the tympanic membrane.
- 18. Treatment • Small plaques not intefering with mobility of TM are normally left alone • Removal of plaques before grafting- controversial ▫ Advised if small area involved ▫ Plaques contiguous with perforation and not interfering with TM mobility may be retained ▫ As plaque removal in these cases may risk increase in size of perforation ( result of epithelial reaction or from tearing of TM remnant if it is attenuated)
- 19. • If footplate fixed mobilization may be tried; unsuccessful- second stage stapedectomy may be tried • General dictum that stapedectomy should not be done in concurrence with tympanoplasty or myringoplasty
- 20. • Large area and complaint of deafness ▫ Hearing aid
