Truamatic dental injuries / prosthodontic courses
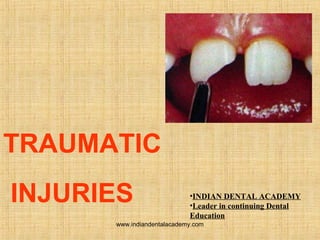
- 1. TRAUMATIC INJURIES •INDIAN DENTAL ACADEMY •Leader in continuing Dental Education www.indiandentalacademy.com
- 3. Trauma refers to injury; damage; impairment; or degeneration to body tissue. www.indiandentalacademy.com
- 4. Fracture is a sudden, violent breach of continuity of bone, which may be complete or incomplete in character. www.indiandentalacademy.com
- 5. Avulsion is loss of tissue due to trauma. www.indiandentalacademy.com
- 7. Traumatic injuries can be classified according to, * Etiology * Anatomy * Pathology * Therapeutic consideration * Prognosis www.indiandentalacademy.com
- 8. Classification based on tissue and site All injuries to the face may be divided into two basic groups, • Injuries to soft tissues • Injuries to bone www.indiandentalacademy.com
- 9. Rabinowitch Classification (1956) • Fractures of the enamel • Fractures into the dentin • Fractures into the pulp • Fractures of the root • Comminuted fractures • Displaced teeth www.indiandentalacademy.com
- 10. Ellis and Davey Classification (1960) • Class 1 - Simple fracture of the crown involving little or no dentin. • Class 2 - Extensive fracture of the crown involving considerable dentin, but not the dental pulp. www.indiandentalacademy.com
- 11. • Class 3 - Extensive fracture of the crown involving considerable dentin and exposing the dental pulp. • Class 4 - The traumatized teeth that become non-vital with or without a loss of crown structure. • Class 5 - Teeth lost as a result of trauma.www.indiandentalacademy.com
- 12. • Class 6 - Fracture of the root with or without a loss of the crown structure. • Class 7 - Displacement of a tooth without fracture of the crown or root. • Class 8 - Fracture of crown en masse and its replacement. • Class 9 - Traumatic injuries to primary teeth. www.indiandentalacademy.com
- 13. Modification of Ellis classification by McDonald, Avery and Lynch (1983) • Class 1 - Simple fracture of the crown involving little or no dentin. • Class 2 - Extensive fracture of the crown involving considerable dentin, but not the dental pulp. www.indiandentalacademy.com
- 14. • Class 3 - Extensive fracture of the crown with an exposure of the dental pulp. • Class 4 - Loss of the entire crown. www.indiandentalacademy.com
- 15. BASRANI CLASSIFICATION • Crown fractures. – Fracture of enamel. – Fracture of enamel and dentin. • Without pulp exposure. • With pulp exposure. • Root fractures. • Crown root fractures. www.indiandentalacademy.com
- 16. WHO Classification (1992) • Adapted from WHO Geneva 1992. • Based on anatomy, therapeutic and prognostic consideration. • It is applied to both primary and permanent teeth. • Code numbers used according to the International classification of diseases 1992.www.indiandentalacademy.com
- 17. Injuries to the hard dental tissues and pulp Enamel infraction N 502.50: An incomplete fracture (crack) of the enamel without loss of tooth substance. www.indiandentalacademy.com
- 18. Enamel fracture (Uncomplicated crown fracture) N 502.50: A fracture with loss of tooth substance confined to enamel. www.indiandentalacademy.com
- 19. Enamel - dentin fracture (Uncomplicated crown fracture) N 502.51: A fracture with loss of tooth substance confined to enamel and dentin but not involving pulp. www.indiandentalacademy.com
- 20. Complicated crown fracture N 502.52 A fracture involving enamel and dentin and exposing the pulp. www.indiandentalacademy.com
- 21. Uncomplicated crown root fracture N 502.54 A fracture involving enamel, dentin and cementum but not involving the pulp. www.indiandentalacademy.com
- 22. Complicated crown root fracture N 502.54 A fracture involving enamel, dentin and cementum and exposing pulp. www.indiandentalacademy.com
- 23. Root fracture N 502.53: A fracture involving dentin, cementum and the pulp. www.indiandentalacademy.com
- 24. Injuries to the periodontal tissues Concussion N 503.20: An injury to the tooth supporting structures without abnormal loosening or displacement of the tooth. www.indiandentalacademy.com
- 25. Subluxation N 503.20 An injury to the tooth supporting structures with abnormal loosening but without displacement of the tooth. www.indiandentalacademy.com
- 26. Extrusive luxation (peripheral dislocation, partial avulsion) N 503.20 Partial displacement of the tooth out of its socket. www.indiandentalacademy.com
- 27. Lateral luxation N 503.20 Displacement of the tooth in a direction other than axially. This is accompanied by fracture of the alveolar socket. www.indiandentalacademy.com
- 28. Intrusive luxation (central dislocation) N 503.21: Displacement of the tooth into the alveolar bone. This injury is accompanied by fracture of the alveolar socket. www.indiandentalacademy.com
- 29. Exarticulation (complete avulsion) N 503.22 Complete displacement of the tooth out of its socket. www.indiandentalacademy.com
- 30. Injuries of the supporting bone Comminution of alveolar socket (mandible N 502.60, maxilla N 502.40): Crushing and compression of the alveolar socket. intrusion and lateral luxation. www.indiandentalacademy.com
- 31. Fracture of the alveolar socket wall (mandible N 502.60, Maxilla N 502.40) A fracture contained to the facial or lingual socket wall. www.indiandentalacademy.com
- 32. Fracture of the alveolar process (Mandible N 502.60, Maxilla N 502.40) A fracture of the alveolar process which may or may not involve the alveolar socket. www.indiandentalacademy.com
- 33. Fracture of mandible and maxilla (Mandible N 502.61, Maxilla N 502.42) A fracture involving the base of the mandible or maxilla and often the alveolar process (jaw fracture). The fracture may or may not involve the alveolar socket. www.indiandentalacademy.com
- 34. Injuries to gingival or oral mucosa Laceration of gingival or oral mucosa N S01.50: A shallow or deep wound in the mucosa resulting from a tear and usually produced by a sharp object. www.indiandentalacademy.com
- 35. Contusion of gingival or oral mucosa N S00.50 A bruise usually produced by an impact from a blunt object and not accompanied by a break of the continuity in the mucosa, causing sub-mucosal hemorrhage. www.indiandentalacademy.com
- 36. Abrasion of gingiva or oral mucosa N S00.50 A superficial wound produced by rubbing or scraping of the mucosa leaving a raw bleeding surface. www.indiandentalacademy.com
- 38. Iatrogenic injuries in new born • Prematurely born infants kept under prolonged intubations in ICU . • Intubations rests along maxillary alveolar process. • Cause developmental enamel defect in primary dentition. www.indiandentalacademy.com
- 39. Fall in infancy • Dental and maxillo-facial injuries are common during later half of first year of life. • Because of child's lack of experience and motor coordination and learning motor activity like crawl, stand, or walk . • Occasionally due to fall from a baby carriage. www.indiandentalacademy.com
- 40. Fall in child hood • Another peak incidence period for dental injuries is just before school age and is mainly the result of falls and collision. • In school age play ground injuries are most case of traumatic injuries. • High frequency of crown fracture is reported. www.indiandentalacademy.com
- 41. Child physical abuse • Battered child syndrome • 0.6 %of children suffer traumatic injuries due to Child physical abuse. • In USA 3000 children per year die due to sever traumatic injuries caused by child physical abuse. www.indiandentalacademy.com
- 42. • Fatal out come mainly due to intra-cranial hemorrhage. 50% of abuse injury are found on face around mouth. • Facial trauma is the principle reason for admission to hospital. www.indiandentalacademy.com
- 43. Automobile / bicycle Accidents • In young children more common. • High velocity impact. • Multiple crown fracture with lip and chin injuries are most common results. www.indiandentalacademy.com
- 44. • In recent years, injuries secondary to automobile accidents has been observed to be on the rise. • Front seat passenger are more prone to trauma. • Facial trauma due to collision of face to dash board or steering . www.indiandentalacademy.com
- 45. • Child standing or sitting on front seat thrown against dash board during sudden stop. www.indiandentalacademy.com
- 46. Assault / torture • Commonly seen in adults alcoholic abuse. • Battered wife syndrome leads to battered child syndrome --vicious cycle. • Substantial delay in injury and treatment period. • Repeated injury to head and neck. • Previous history of abuse. www.indiandentalacademy.com
- 47. Sports • Teenagers are commonly injured. • These injuries are often related to contact sports (1.5%- 3.5% ) like football, baseball, basketball, ice hockey, soccer and wrestling. • Soccer > Hand ball > Horse back riding www.indiandentalacademy.com
- 48. Drug related / GA recovery • Drug abusers • 3-4 hrs after drug in take violent tooth clenching • Fracture in premolar and molar region Epilepsy • Special risk category • 52% of all patient suffer from facial injuries • 1/3rd of such injuries reported due to fall during attack. www.indiandentalacademy.com
- 49. Dentinogenesis imperfecta • Spontaneous root # is common • Due to low micro hardness of dentin abnormally tapered root Mental retardation • Lack of motor coordination www.indiandentalacademy.com
- 51. Mechanism of dental injury Direct trauma • Tooth strike directly Indirect trauma • Lower jaw force fully closed with upper • Associated with Jaw # • Cerebral involvement seen • Posterior teeth involved in #www.indiandentalacademy.com
- 52. Type of dental injury • Primary dentition due to resilient supporting tissue ex-articulation luxation common • Permanent dentition crown # is more common Place of injury • In Iraq, Australia and in India injury in play ground is more than other places. www.indiandentalacademy.com
- 53. Complication of dental injury to primary teeth • Failure to continue eruption • Color change • Infection and abscess • Early exfoliation space loss • Ankylosis • Injury to developing bud • Financial cost www.indiandentalacademy.com
- 54. Complication of dental injury to permanent teeth • Color change • Infection and abscess • Early exfoliation space loss • Ankylosis • Loss of alveolar bone support • Financial cost • Root resorption www.indiandentalacademy.com
- 56. Examination and diagnosis Consider traumatic injuries as emergency, • To relieve pain. • Reduce psychological stress. • Facilitate reduction of # or avulsion. • For good prognosis. Complete examination correct diagnosis success full treatmentwww.indiandentalacademy.com
- 57. Record all information's in standardized charts, • Save time. • Not miss any information in hurry. • Insurance claiming. • Medico-legal considerations. Only acute bleeding, respiratory problem, severe cerebral trauma and avulsion of teeth will alter above procedure. www.indiandentalacademy.com
- 58. History Ask for personal data: Patient’s name, age, sex, address and telephone number ? • Obvious necessary for record maintenance. • Provide clue for possible cerebral involvement. • Provide clue for general mental states. www.indiandentalacademy.com
- 59. When did injury occurred ? • Time interval between injury and treatment started. • Alter possible prognosis and line of treatment specially in cases of re-implantation, pulp exposure, bone# and severe soft tissue injuries. Where did injury occurred ? • For tetanus prophylaxis.www.indiandentalacademy.com
- 60. How did injury occurred ? • Direction of blow which tells possible structure affected. • Object in mouth like pacifier labial displacement of teeth. • Young child and women with multiple soft tissue injury at deferent stage of healing improper history child abuse. www.indiandentalacademy.com
- 61. Treatment else where ? • Storage of avulsed teeth. • Medication taken. • Re-implantation and immobilization considered. History of previous injury ? • Sustained repeated injury influence pulp vitality test. • Affects healing capacity of pulp and PDL.www.indiandentalacademy.com
- 62. General health and medical history ? • Allergic reaction • Epilepsy • Bleeding disorder • Differs emergency and later treatment www.indiandentalacademy.com
- 63. Spontaneous pain from teeth ? • Hyperemia • PDL damage • Pulp damage • Crown root # Teeth reacts to thermal changes ? • Dentin or pulp exposure www.indiandentalacademy.com
- 64. Did trauma caused amnesia, unconsciousness ? • Drowsiness, vomiting, headache unable to recall past memory possible cerebral involvement. • Emergency medical consultation Teeth tender to touch eating ? Any disturbance in bite ? • Extrusion, lateral luxation, alveolar jaw #, crown root # www.indiandentalacademy.com
- 65. Clinical examination • Record extra oral wound. • Wound penetrating entire thickness of lip. • Demarcated by two parallel wounds, inner and outer which indicate possible tooth # and fragment burreid in soft tissue.www.indiandentalacademy.com
- 66. • Irrespective of size these fragments are not palpable. • So care full x ray examination of soft tissue is required. • see for possible foreign body. • If not treated cause chronic infection and disfiguring fibrosis. www.indiandentalacademy.com
- 67. • Record injury of oral mucosa, gingiva. • Bleeding from non lacerated marginal gingiva indicate damage to PDL ligament. • Sublingual sub-mucosal heamatoma indicate jaw #. www.indiandentalacademy.com
- 68. • Gingival laceration usually associated with displaced teeth. • Check for muco-periosteal displacement by properly cleaning alveolar process. • Palpate facial skeleton for bone #. www.indiandentalacademy.com
- 69. • Examine crown of teeth for #, pulp exposure, color change after proper cleaning. • Infarction lines on enamel seen by directing light beam II to long axis of tooth by shadowing light beam with finger. • Examine for extent of crown fracture, pulp involvement, if pinkish hue visible, Not perforate.www.indiandentalacademy.com
- 70. • In case of indirect trauma suspect, posterior teeth fracture and examine. • Crown root # in posterior teeth one quadrant is often accompanied by similar # on same side of opposing jaw, so suspect and examine. www.indiandentalacademy.com
- 71. • Color change of traumatized tooth noted occurs in post injury period. • Prominent on oral aspect of crown in cervical third. • Examine with trans-illumination reveal change in translucency. www.indiandentalacademy.com
- 72. Grey discoloration of 11 after 3 months of lateral luxation Initial grayish discoloration becoming normal in later visit www.indiandentalacademy.com
- 73. Red discoloration of11 revert back after 5years follow up Yellow discoloration of 21 after 10 yrs pulp canal obliteration www.indiandentalacademy.com
- 74. Follow up of subluxated primary incisor 1st day of injury 3week reddish brown discolor 1year follow up Yellowish discoloration Pulp canal obliteration www.indiandentalacademy.com
- 76. • Record displacement of teeth. • Visual, occlusal x-ray examination done • In case of luxation note direction and extent in mm. • Laterally luxated or intruded teeth some times firmly locked in bone with no tender so only x ray, percussion tone and deranged occlusion can give clue. www.indiandentalacademy.com
- 77. • Due to loss of protective reflexes in unconscious patient. • Avulsion, possibility of inhalation swallowing of teeth or prosthesis are always considered. • Chest abdomen x ray taken. www.indiandentalacademy.com
- 78. • In case of primary dentition diagnose dislocation of apex of teeth as it can impinge on permanent successors www.indiandentalacademy.com
- 79. • Deranged occlusion indicate jaw #, alveolar process #, displacement injury • Abnormal mobility of jaw fragment seen in case of # • Typical sign of alveolar # is movement of adjacent teeth when mobility of one tooth is checked. www.indiandentalacademy.com
- 80. • Palpation of alveolar process un even counter indicate bony # • Mobility of teeth and alveolar fragment check for direction Horizontal , axial • Axial mobility disruption of vascular supply • D/d erupting teeth resorbing primary teeth excluded www.indiandentalacademy.com
- 81. • Depending on location root # exhibit mobility confirmed by X ray • TOP and percussion note • TOP +ve indicate damage to PDL • Vertical and Horizontal • Checked with handle of mouth mirror www.indiandentalacademy.com
- 82. • Begin with non injured tooth to assure reliability of patients response • Smaller children finger tip used • Percussion calibrated instrument introduced periotest • But force produced by this this instrument might contribute to new trauma in root # www.indiandentalacademy.com
- 83. • Hard metallic sound Horizontal teeth locked in bone • Dull sound sub luxation extrusive luxation • D/D apical lesion which also will produce dull sound www.indiandentalacademy.com
- 84. Reaction of pulp to vitality test • Controversial issue • Cooperative and relaxed pt required • Accuracy not possible in first visit • But still noted at time of injury to establish a a point of reference for following test www.indiandentalacademy.com
- 85. • Principle - transmission of stimuli to sensory receptor of the dental pulp and registering the reaction. Mechanical stimulation • Dentin or pulpal stimuli tested by scraping with probe or drilling the test cavity www.indiandentalacademy.com
- 86. • In replanted teeth this is not possible as pain sensation is not noted till dentin pulp junction reached. • In case of clinically visible pulp exposure stimulus is tested by cotton socked in saline. www.indiandentalacademy.com
- 87. Thermal tests • Not reliable completely and not reproducible • Normal pulp may yield negative response • Non vital teeth may yield +ve response in case of gangrene thermal expansion of fluid exerts pressure on inflamed PDL www.indiandentalacademy.com
- 88. Heated GP • Memford 5mm GP stick 2 sec flamed applied to tooth on middle third of the facial surface Ethyl chloride • socked cotton place on facial surface of teeth more consistent than above two • Highly inflammable www.indiandentalacademy.com
- 89. Ice • Cone of ice to facial surface of tooth 5-8 sec normal tooth may not respond. Carbon dioxide snow -ve78 -- -108 C • Consistent reliable results seen even in immature teeth. Allow pulp testing in completely covered tooth with crown splint • But it results in new infarction lines on enamelwww.indiandentalacademy.com
- 90. Dichloro difluoromethane • Frigen, Provotest • Aerosole –28 -- -18 c • Consistent reliable results seen in immature teeth • But it results in new infarction lines on enamel www.indiandentalacademy.com
- 91. Electrometric test Ideal requirements • It should allow control of the mode, duration, frequency of the stimulus. • Voltage measurement type is not satisfactory. • Given voltage produces varying current depending on varying resistance of tissue which is altered from fissure caries and restorations www.indiandentalacademy.com
- 92. • Stimulus should be clearly defined • Electrode area should be as large as tooth shape will permit to allow maximum stimulation. • Stimulus duration of 10 millisecond or more has been advocated. • Digital pulp tester is more reliable than other. www.indiandentalacademy.com
- 93. • Patient is informed and instructed to indicate when sensation is first experienced. • Isolate from saliva to prevent diversion of current to PDL or gingiva. • Do not desiccate tooth which increases resistance. • Medium such as saline and tooth paste can be used between electrode and tooth.www.indiandentalacademy.com
- 94. • Loose teeth immobilized before pulp testing • Pulp testing should be done before administration of LA • Electrode is placed as far from gingiva preferably on fracture area or the incisal edge. www.indiandentalacademy.com
- 95. • Circuit can be completed by • neutral electrode held by patient by grasping the end of pulp tester. • Examiner touching patient mouth with finger or mouth mirror. • Clip to the lip www.indiandentalacademy.com
- 96. • Rheostat of the tester is advanced continuously till the patient reacts to give threshold value. • Threshold value should be determined by a quick increase in current rather than slow which causes adaptation. • Then this value is compared with abnormal tooth. www.indiandentalacademy.com
- 97. • Low reading indicate hyperemia, acute pulpitis • High reading indicate chronic pulpitis degeneration www.indiandentalacademy.com
- 98. • Splints or temporary crown used alter response by increasing threshold value so cold test is the best alternative. • Teeth with luxated injuries may not respond to the stimulus temporarily. • They start reacting after few weeks or months www.indiandentalacademy.com
- 99. • In case of immature root and adult obliterated canals electric pulp testing will gives false – ve results • Teeth under going orthodontic treatment shows high excitation threshold. www.indiandentalacademy.com
- 100. Laser Doppler Flowmetry • Laser beam directed at coronal aspect of pulp the reflected light scattered by moving blood cell under goes a Doppler frequency shift • The fraction of light scattered back from pulp is detected and formed in signal www.indiandentalacademy.com
- 101. • Non vital teeth reliability 97% • Vital teeth reliability 100% • Draw backs • Blood pigment in discolored teeth inter fear with laser light transmission • Price of instrument www.indiandentalacademy.com
- 102. Radiographic examination • Reveal stage of root formation. • Show root # or PDL damage. • Most root # are disclosed by X ray examination as fracture line usually run parallel to central beam. • Luxation injury PDL wide • Intrusion causes PDL narrow www.indiandentalacademy.com
- 103. • Dislocation injury take 3 angulations Central beam directed between two CI, Central beam directed between CI and LI and occlusal. • Steep occlusal exposure used for diagnosis of root # and Lateral luxation with oral displacement of tooth www.indiandentalacademy.com
- 104. • Below two years patient x ray taken with parents and special holder • In uncooperative patients reduce exposure time by 30% for each 10 kvp increase. • Lip exposure ¼ - ½ normal time with decreased kvp • Infarction lines decease kvp. www.indiandentalacademy.com
- 105. Extra oral x ray for jaw # • Waters view or occipito-mental view (OMV) 30/400 for midface, including the zygoma, maxilla, maxillary sinus orbital floors and nasal pyramid. • Extraoral – orthopantomogram (OPG) condyles, alveolar segments..www.indiandentalacademy.com
- 106. • Caldwell view – frontal sinuses, frontal bone, anterior ethmoidal cells and zygomatic frontal suture. • Towns view Lateral oblique mandible body angle www.indiandentalacademy.com
- 108. Management of patient • Emergency management A- Airway with cervical spine control B- Breathing and ventilation C- Circulation and hemorrhage control D- Disability neurological states www.indiandentalacademy.com
- 109. • H/O loss of consciousness • Altered mental status • Dilated and unreactive pupil • Blurring of vision • Severe headache, Dizziness, Drowsiness www.indiandentalacademy.com
- 110. • Seizures • Vomiting • Loss of smell, taste, hearing and/or sight • Discharge from the nose and ears. www.indiandentalacademy.com
- 111. Luxation Injuries • Concussion, subluxation, extrusion, lateral luxation, intrusion. • Prevalence Pry_ -15-61%, Perm_-62-73%. • Primary intrusion and extrusion most common • In permanent dentition other type more. www.indiandentalacademy.com
- 112. Concussion • Miner injury to PDL • No tooth loosening present • Tooth tender on touch • TOP +ve in both vertical and horizontal direction www.indiandentalacademy.com
- 113. Subluxation • Teeth retained in normal position in arch but tooth is mobile in horizontal direction • Sensitive to percussion and occlusal force • Hemorrhage from the gingival crevices indicate trauma to PDL. www.indiandentalacademy.com
- 114. Extrusion • Teeth appear elongated most often with lingual deviation of crown • PDL bleeding seen • Percussion test show dull sound www.indiandentalacademy.com
- 115. Lateral luxation • Crown show lingual displacement • Associated with # of vestibular part of the socket wall • Displacement is usually visible • Check occlusion www.indiandentalacademy.com
- 116. • percussion test show high pitched metallic sound • Teeth are not sensitive to percussion and completely firm www.indiandentalacademy.com
- 117. Intrusion • Show marked displacement in primary teeth • percussion test show high pitched metallic sound • Teeth are not sensitive to percussion and completely firm • Examine floor of nose for bleeding and protruding apex. www.indiandentalacademy.com
- 118. • Palpation of alveolar socket reveals position of displaced tooth. • Note amount of displacement of teeth in mm. And direction of displacement. • In case of lingual displacement permanent successor is directly involved. www.indiandentalacademy.com
- 119. Radiographic examination • Disclose minor dislocations • Bisecting angle technique is used to minimize the error. • Width of PDL space increased in case of extrusive luxation decreased or obliterated in case of intrusion • In primary dentition it reveals relation between permanent to deciduouswww.indiandentalacademy.com
- 120. Pathology Concussion subluxation after 1 hrs • Edema, bleeding, PDL lacerations • Pulp neuro-vascular supply may or not intact. • After 1 day cell free zone seen in PDL bordered by a zone of inflammation. In bony socket osteoclasic activity may seen. After 1 week this reach to root surface. • www.indiandentalacademy.com
- 121. • After 10 days resorption subsides leaving surface resorption cavities along root surface Lateral luxation • Complex injury involving rupture and compression of PDL fibers and nero- vascular supply • With # of alveolar socket wall www.indiandentalacademy.com
- 122. Extrusive luxation • Complete rupture of PDL and neuro-vascular supply to pulp • After 3 days PDL healing starts with fibroblast formation • After 2 weeks newly formed collagen fibers seen • After 3 weeks PDL becomes normal. www.indiandentalacademy.com
- 123. Intrusive luxation • Extensive crushing injury to PDL and alveolar socket and rupture of nero- vascular supply to pulp. • After 3 months some teeth may show ankylosis • Or surface resorption normal PDL www.indiandentalacademy.com
- 124. • Treatment of luxation injuries • Concussion and sub-luxation • Relief occlusion of injured teeth in case of non mobile or grade 1 mobile soft diet is advised for 14 days in case of marked loosening immobilization is indicated • Follow up tooth for 1 year with Xray and pulp vitality test. www.indiandentalacademy.com
- 125. • Extrusive and lateral luxation • Administer LA if forceful repositioning is anticipated • Reposition tooth in its proper position. In case of delayed treatment teeth some time realign spontaneously or moved orthodontically • After replacement tooth is splinted with acid etch resin splint. www.indiandentalacademy.com
- 126. • Splinting period • Extrusion 2-3 weeks • Lateral luxation 3weeks • In case of marginal bone break down 6-8 weeks • Follow up tooth for 1 year with Xray and pulp vitality test. www.indiandentalacademy.com
- 127. • Intrusion • Repositioning is anticipated in incomplete root formation • In case of completely formed root orthodontocally tooth is pulled out to normal position over a period of 3-4 weeks • Follow up tooth for 5 year with X ray and pulp vitality test. www.indiandentalacademy.com
- 131. Avulsed Tooth Immature Pulp Open apex – 2 mm No Dry Storage Time Dry Storage Time Category 1 Replant immediately at site of the incident Category 2 15 min-6hrs extraoral time stored in physiologic media (HBSS or Milk) Category 3 15-120 minutes with wet, but non-physiologic media (water or saliva) Category 4 0-60 min extra oral time with dry storage Category 5 Greater than 60 min extraoral time with dry storage Treatment guideline for avulsed tooth with open apex Soak in 1% Doxycycline solution for five minutes 1mg/20 ml Doxycycline solution or 50 mg capsule/1000 ml saline Change transport media to HBSS if available Soak in citric acid for three minutes and rinse well or debride and remove PDL gently with scaler 1) Replant and reposition 2) Obtain PA radiographs to verify position 3) Place flexible splint 4) Place on systemic antibiotics 5) Assess tetanus vaccination 6) Provide post op instructions 7) Follow-up in 7-10 days Place in NaF for 20 minutes Assess need for apexification, apexogenesis or root canal therapy www.indiandentalacademy.com
- 132. Treatment guideline for avulsed tooth with closed apex Avulsed Tooth Mature Pulp Closed apex Category 1 Replant immediately at site of the incident OR extraoral storage time in physiologic media (HBSS or milk) for 15 min-6 hours Category 3 15-120 minutes with wet, but non-physiologic media (water or saliva), 0-60 minutes extraoral time and dry storage Category 5 Greater than 60 minutes extraoral time with dry storage Change transport media to HBSS if available Soak in citric acid for three minutes and rinse well or debride and remove PDL gently with scaler1) Replant and reposition 2) Obtain PA radiographs to verify position 3) Place flexible splint 4) Place on systemic antibiotics 5) Assess tetanus vaccination 6) Provide post op instructions 7) Follow-up in 7-10 days Place in NaF for 20 minutes With the possible exception of category 1, all these teeth will need root canal therapy www.indiandentalacademy.com
- 133. Consider contraindication • Advanced PDL disease • Intactness of alveolar socket • Dry extra-oral period more than 1hrs ( chemical protectants) www.indiandentalacademy.com
- 134. Repositioning of avulsed tooth with complete root formation Tooth and socket are cleaned with saline Prepare socket Reposition tooth Splinting is done www.indiandentalacademy.com
