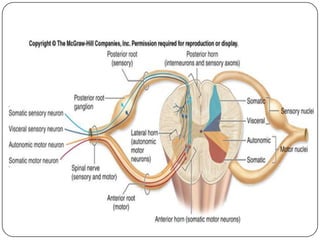
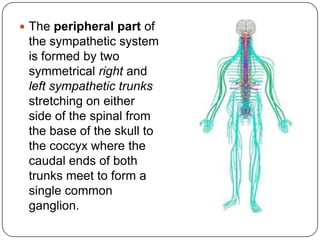
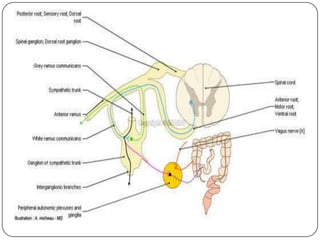
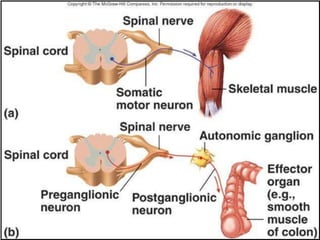
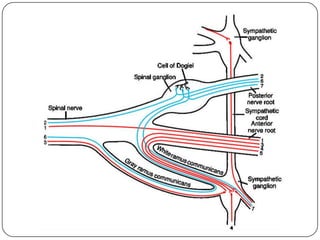
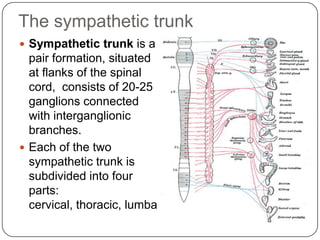
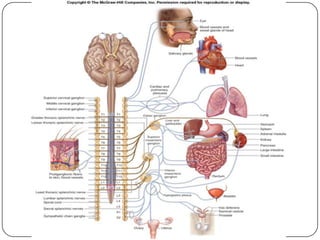
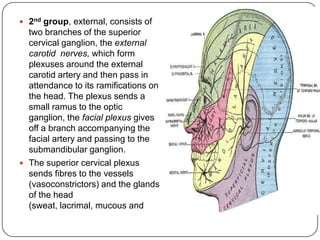
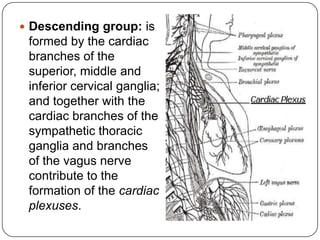
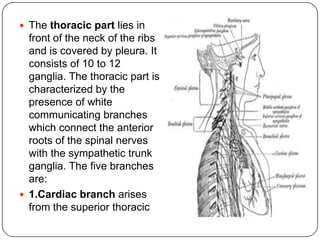
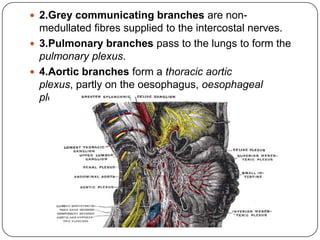
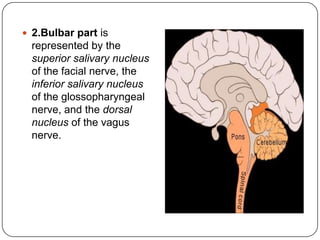
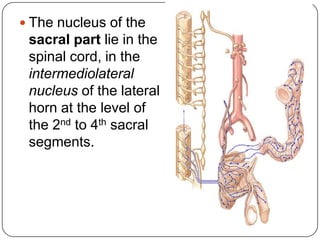
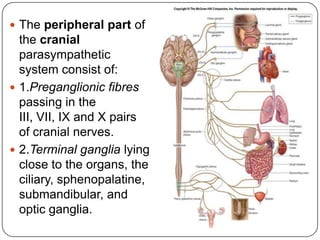
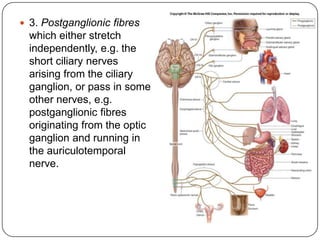
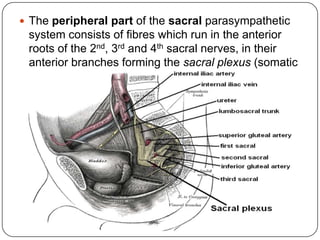
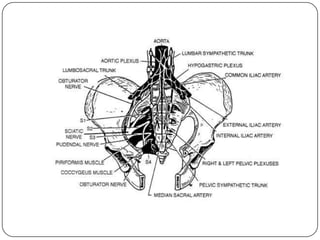
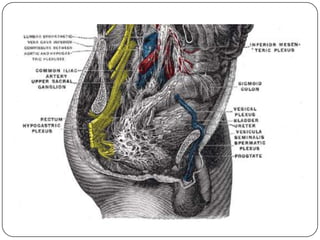
The document summarizes the vegetative (autonomic) nervous system. It describes that the system controls organs like respiration, circulation, reproduction and excretion. It is separated into the sympathetic and parasympathetic systems. The sympathetic system is mainly concerned with trophic functions and increases processes like respiration and cardiac activity. The parasympathetic system has a protective role like pupil constriction and inhibiting cardiac activity. The systems have antagonistic interactions in organs with double innervation.