Nontransecting modified
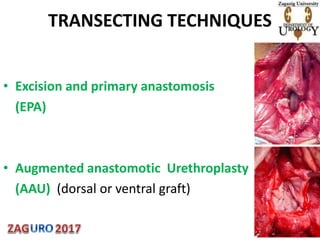
- 1. TRANSECTING TECHNIQUES • Excision and primary anastomosis (EPA) • Augmented anastomotic Urethroplasty (AAU) (dorsal or ventral graft)
- 2. Excision and primary anastomosis (EPA) • The simplest and most effective and durable surgical treatment for anterior strictures. • Ideally suited for bulbar strictures 1- to 3-cm long and in some selected cases up to 5 cm in length. (Gomez. 2014)
- 3. EPA Outcome (The gold standard) • A collection of 12 series from the literature • More than 1,000 patients • Long follow up; • Cure rates ranged from 86 to 98.8 %, with an average of 92 %.
- 4. EPA –Durable outcome • EPA offers the best chance for long-term cure of anterior urethral strictures. • Andrich et al 2003 reported a 4-fold increase in stricture recurrence between non-transecting substitution urethroplasty and EPA.
- 5. • Yuri and colleagues 2016 in their meta analysis after an average follow up of 34 months showed stricture recurrence rates following EPA and BMG were 8.4% (8/107) and 30% (14/46), respectively. EPA –Durable outcome
- 6. Meta analysis EPA • Morey et al in 2014 SIU/ICUD Consultation on Urethral Strictures: Anterior Urethra- Primary Anastomosis • 35-year literature search was conducted (1975-2010) for peer-reviewed articles on EPA for bulbar strictures. • 17 articles fulfilled the criteria with a total of 1234 patients. • Overall success was 93.8%. • Reported complications were < 5%, • No evidence of persistent loss of sexual function. (Morey et al 2014).
- 7. • Intended for bulbar strictures deemed too long for straight-forward primary anastomosis. • This technique saves 1 cm of urethral shortening Augmented Anastomotic Urethroplasty (AAU)
- 8. • Guralnick and Webster 2007 over a mean follow- up of 28 months, reported 93 % stricture-free rate. • Similar results (~90 % success at medium term, 3- year followup) have been reported by Abouassaly & Angermeier 2007 and El-Kassaby et al 2008. Augmented Anastomotic Urethroplasty (AAU)- OUTCOME
- 9. • EPA showed Superior results to any other method of bulbar urethroplasty (Barbagli et al 2014), (Chapple et al 2014). Transection Vs non-transection
- 10. • While attempts to demonstrate equivalency between non- transecting substitution urethroplasty & transection have been reported, these studies showed low urethral patency rates compared to EPA. (Chen, Odom, and Santucci. 2014). Transection Vs non-transection
- 11. • Controversial issue with many divergent opinions. Current data, however, fail to provide clear evidence of the impact of transection on sexual function (Barbagli et al 2012) • Multiple risk factors appear to be involved, such as patient age, stricture length and location, and type of reconstruction. Transection and ED
- 12. • Overall, urethroplasty transient post-operative ED in up to 40% of patients. • While ED in Transection has been shown to be significantly higher at 3 months, there is no demonstrable difference at 6 months and beyond (Erickson et al2007, Coursey et al 2001, Ekerhult et al 2013, El-Assmy et al 2015, Erickson et al 2010, Anger et al 2008 and Blaschko et al 2013) Transection and ED
- 13. Transection and ED retrospective studies
- 14. Transection and ED prospective studies
- 15. Transection and ED more prospective studies
- 16. Transection and ED Meta analysis
- 17. Why not non-transecting • Didn’t remove the fibrotic tissue and recurrence is inevitable. • Not suitable for oblitrative and traumatic stricture. • Despite initially acceptable urethroplasty outcome however it is not durable.
- 18. • Excision of the diseased mucosa only cannot be compared to full excision of the fibrotic segment when stricture recurrence rate is concerned. Why not non-transecting
- 19. • Despite theoretical advantage of non transection over transection regarding erectile function this was not translated clinically after 6 month so it is better to get a long term cure of stricture disease instead of being happy with some earlier return of erection after surgery. Why not non-transecting
