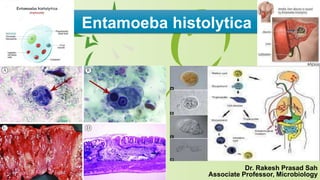
Entamoeba histolytica: symptoms, life cycle, and pathogenesis
- 1. Entamoeba histolytica Dr. Rakesh Prasad Sah Associate Professor, Microbiology
- 2. Introduction to Parasitology › Terms used in Parasitology: Parasite: A living organism which receives nourishment & shelter from another organism where it lives. Host: An organism which harbours the parasite. › Classes of Parasites: › 1.Ectoparasite-lives on the surface of the body of host. – Ex- lice, mites, ticks(arthropods) › 2.Endoparasite-lives inside the body of host ie- in blood, tissues, digestive tract ect. – Ex-All protozoan & helminthic parasites of man. › 3.Temporary parasite-visits its host for a short period.
- 3. › 4.Permanent parasite-leads a parasitic life throughout the whole period of its life. › 5.Facultative parasite-lives a parasitic life when opportunity arises. › 6.Obligatory parasite-cannot exist without a parasitic life. › 7.Accidental parasite-attacks an unusual host. › 8. Wandering parasite-happens to reach a place where it cannot live.
- 4. Classes of Hosts: › Definitive host: which harbours the adult stage of the parasite or host in which sexual multiplication takes place. ex. In malaria mosquito is def…host. In hydatid disease dog. › Intermediate host: which harbours larval stage of parasite or host in which asexual multiplication of parasite occurs.ex.in malaria and Hydatid disease man is Int…host. › Zoonotic diseases: (zoonosis)-Diseases that are transmitted from animals to humans – Ex-hydatid disease
- 5. Classification › Medically Imp. Parasites: 2 kingdoms › 1)Protista 2)Animalia Phyllum-Protozoa Helminths Protozoa- unicellular, Microscopic. Helmints- Multicelular, Macro. * single cell performs all functions. Each special cell performs particular function
- 6. › Medical protozoalogy 4 classes 1.Rhizopoda ex. Entamoeba 2.Flagellates ex. Haemoflagellates & Intestinal Flagellates 3.Sporozoa ex. Plasmodium & Toxoplasma 4.Ciliates ex. Balantidium coli Helminths : 2 phylum- 1. Platyhelminthes (Flat worms) 2. Nemathelminthes (Round worms) i. Platyhelminthes- 2 classes- 1. cestodes(Tape worms) Tape like segments 2. Trematodes (Flukes) Leaf like, unsegmented ii. Nemathelminths- (Round worms)-Cylindrical, Elongated, Unsegmented
- 7. › In General all parasites are classified in to Kingdom – protista Phylum – protozoa/ sarcomestigophora Subphylum – plasmodroma/ Sarcodina Class – rhizopoda(Amoebae) Order – Amoebida Genus – Entamoeba Species – histolytica
- 8. › The systematic study of parasite involves the knowledge of : › 1. Geographical Distribution-Area where it is found › 2. Habitat- Place where the parasite resides in the host › 3. Morphology- Various developmental stages of parasites through which it passes in its life cycle are studied › Ex. Trophozoites, cysts, Larva, Adult worm › 4. Modes of Infection- › Sources of Infection: › i. Contaminated food & water › ii. Contaminated soil polluted with human faeces › iii. Different animals › iv. Insect vectors
- 9. › Portal of entry › i. By ingestion (faeco oral route) › ii. By Ingesting the parasite in raw under cooked meat › iii. By penetration of skin with the larva › iv. Through insect bite (vectors) › 5.Life Cycle – Cycle of development of a parasite. The parasite may pass its life cycle in one and the same host or it may change its host. › 6. Lab Diagnosis – Following material should be collected. › 1.Blood- For those parasites which infect blood stream. › 2.Stool- for diagnosing intestinal parasites. › 3.Urine- Parasites in the urinary tract. › 4.sputum- In respiratory tract.
- 10. › 5.Biopsy Material › 6.Indirect evidence- › i.Change in the blood, Eosinophilia, Leucopenia, Anaemia › ii. serological tests. › Iii. Skin tests (Intradermal reaction) › Emerging parasites- (Newly arising pathogen) › 1.Cryptosporidium- Intestinal parasite › 2.Isospora- Intestinal parasite › Commensals but now a days these are important organism because of their association with HIV inf & Aids in which they cause severe infection.
- 11. AMOEBA- Protozoa: unicellular, all functions like reproduction, digestion,respiration,excretion Microscopic .Basic structure- protoplasm enclosed in cell membrane. Protoplasm differentiated into cytoplasm& Nucleus. Exhibit movements by cilia, flagella, pseudopodia. Classification: Intestinal species:1.Entamoeba histolytica 2.E.hartmanni 3.E.coli 4.E.polecki. Endolimax nana. 6.Iodamoeba butschlii. Extra intestinal-1.Entamoeba gingivalis. 2. Acanthamoeba sp. 3.Naegleria fowleri.
- 12. Entamoeba histolytica › Entos = inside + amoibs = changing; histos = tissue + luein = to dissolve › Was first described by Losch in 1875 after being isolated in Russia from a patient with dysenteric tool. › Only amoeba to have definite pathogenic potential is Entamoeba histolytica, a major cause of bloody diarrhea (dysentery) and extra-intestinal invasive disease in humans. › 2nd most common parasitic cause of mortality (after malaria), accounting for an estimated 55,000 deaths each year. › Risk factors – Young age, pregnancy, corticosterioid use, alcoholism, malignancy, malnutrition etc.
- 13. Morphology › E. histolytica – Trophozoite – Pre-cyst – Cyst – Metcyst › Trophozoite (Trophe = Food + Zoon = animal) › It is amoeboid in shape › 20-30µm in size (though it could range from 10- 60µm) › Actively motile in fresh stool with short hyaline pesudopodia
- 14. Morphology › Cytoplasm visible with a clear, thin ectoplasm on the outside and a granular “ground glass” endoplasm inside. › Iron hematoxylin stain clear visualization of nucleus single, spherical with a compact karyosome at its centre. › Inner layer of nuclear membrane lined with evenly distributed fine chromatin granules. › Food vacuoles with ingested RBCs and bacteria can often be seen.
- 15. Cyst (Kystis=bladder) › Trophozoite condense to form Pre- cysts mature cysts (10x20µm) › An early cyst has one nucleus divides into two or four nuclei (metacyst) on maturation.
- 16. Life cycle: (simple) man is the only host Quadrinucleated cyst Human (by ingestion) Cyst (pass upto ileo-ceacal region) Excystation occur (due to surrounding alkalinity and damage by trypsin to cyst wall) Quadrinucleate cyst
- 17. Life cycle: (simple) man is the only host Divide 8 small ameobae (amoebulae or metacystic trophozoites) Develops into trophozoites Large intestine – live in the lumen without invading intestinal mucosa (90% infected persons) They encyst when conditions becomes unfavorable -Cyst in feces (carriers)- maintainence & spread of infection in community In remaining 10 % infected persons – amoebae invade the host tissue ( bowel mucosa- causes dysentry)
- 19. Pathogenesis Human infected with cystic forms of E. histolytica After excystation, some amoeba colonises large intestine manifests from carrier state to diarrhoea or invasive disease. Several virulence factors causes extensive tissue destruction by lysing host cells. Mechanism of pathogenesis of infection:- Adherence by galactose and N-acetyl D-galactosamine lectin (Gal/GalNAc) to epithelial cells and other target cells. Mucin facilitates binding of parasite and protects the intestinal epithelium from direct lysis.
- 20. Pathogenesis Cytolysis:- extensive cytolysis brought by Gal/GalNAc lectin and other amoebaphores Cell death results from swelling, chromatin condensation, membrane blebbing, DNA fragmentation and non-classsical apoptosis. Phagocytosis:- amoeba ingests cell debris and RBCs. Cysteine proteases:- responsible for the degradation and digestion of mucin glycoproteins, Hb, villin and extracellular matrix (fibronectin, laminin, elastin and collagen)
- 21. Intestinal Amoebiasis › Causes disruption of the epithelium and the depletion of the mucus followed by formation of ulcers. › Lesions commonly develop – Caecum – Rectum – Ascending colon – Sigmoid colon – Rarely transverse and descending colon. › Further invasion of submucosa and underlying blood vessels facilitates migration of trophozoites to liver, lungs and other organs from secondary lesions.
- 22. Extra-intestinal Amoebiasis › Commonest secondary lesion liver abscess postero-superior surface of the right lobe of the liver. › The pus of is made up of – Liquified necrotic liver tissue and blood (thick chocolate brown) – Contains few leukocytes – Bacteriologically sterile › Trophozoite carried via the blood stream cause metastatic abscesses anywhere in the body.
- 23. Clinical Features › I.P. 1-4 weeks. Asymptomatic disease › 90% of the infections remain asymptomatic or mildly symptomatic. Symptomatic disease › Diarrhea – Gradual onset of lower abdominal pain and mild diarrhea – Malaise, weight loss and diffuse lower abdominal pain – Occasionally progressing to dysentery.
- 24. Clinical Features › Amoebic dysentery – Onset is gradual – Colicky abdominal pain – Fever – Prostation – Bloody diarrhea with mucus and pus cells. – Resembles bacillary dysentery, a few clinical and laboratory features help to differentiate between two entites.
- 25. Differential features of amoebic and bacillary dysentery S.No. Clinical Features Amoebic dysentery Bacillary Dysentery 1 Onset Gradual Acute 2 Fever Present in <40% Almost always present 3 Abdominal tenderness Localised to the right upper quadrant of the abdomen or referred to the shoulder Generalised 4 Tenesmus Absent Present Stool Sample 5 Odour Offensive Not offensive 6 Colour Dark red Bright red 7 Nature Scanty feces mixed with blood and mucus; hme-positive Blood and mucus with little or no feces 8 Consistency Not adherent to container Adherent to container 9 Reaction Acidic Alkaline
- 26. › Amoebic appendicitis – Acute right lower abdominal pain that mimics appendicitis. › Amoeboma – May present as a palpable abdominal mass confused with carcinoma. › Fulminant colitis or toxic megacolon – Intense colicky pain – Fever – Profuse bloody diarrhea – Mortalitiy rate is very high (40%) in patients with corticosteroid therapy – Note:- so important to exclude amoebiasis in patients with inflammatory bowel disease. › Chronic non-dysenteric colitis – Resembles inflammatory bowel disease with potentially severe consequences if corticosteroids are administered.
- 27. Extra-intestinal Amoebiasis › Hepatic involvement most common extra-intestinal complications of amoebiasis reported in 2-10% of the individuals infected with E. histolytica. S. No. Clinical Features Amoebic liver abscess (ALA) Pyogenic abscess 1 Age 20-40 >50 2 Male:female ratio 10:1 1:1 3 Number of abscesses Solitary abscess in 80% of chronic ALA cases and about 50% of acute ALA Multiple abscesses in approx 50% of all cases 4 Diabetes mellitus Less common, approximately 2% of patients More common, approx one fourth of the patients 5 Jaundice Uncommon Common 6 Pruritus Uncommon Common Elevated bilirubin Uncommon Common Elevated liver enzymes Uncommon Common
- 28. › ALA present with – fever – Abdominal pain localised to the right upper quadrant – Weight loss – Pain may radiate to the right shoulder and my be accompanied by a non-productive cough. – On, examination tenderness of the liver, hepatomegaly, jaundince less common. – ALA tend to rupture into the adjacent tissues and may affect other body organs.
- 29. Pulmonary amoebiasis › Lung – involved by extension of liver abscess through diaphragm or – by direct hematogenous spread from the intestine. – Hepato-bronchial fistula results with expectoration of chocolate brown sputum amoeba can be demonstrated. › Cutaneous amoebiasis › Other organ involvement – Abscesses may develop in (through hematogenous route) › Brain (fatal) › Spleen › Kidney › Genitourinary organ › adrenals
- 30. Diagnosis of Intestinal Amoebiasis › Microscopy – Trophozoites and cysts – Direct microscopy of stool using wet mount and iodine mount
- 31. Diagnosis of Intestinal Amoebiasis › Culture – NIH (National institurte of health) media, Boeck and Drbohlav egg serum medium containing Locke’s solution, Balamuth’s medium and diamond’s medium – Zymodeme/isoenzyme analysis › Coproantigen detection: ELISA and immunochromatographic tests › DNA detection: PCR and real-time PCR.
- 32. Diagnosis of Amoebic Liver Abscess (ALA) › Microscopy – Trophozoites and cysts – Direct microscopy of aspirated pus and sputum (Pulmonary rupture) › Culture – NIH (National institurteu of health) media, Boeck and Drbohlav egg serum medium containing Locke’s solution, Balamuth’s medium and diamond’s medium – Zymodeme/isoenzyme analysis › Ag detection:- ELISA and immunochromatographic tests › DNA detection: PCR and real-time PCR. › Other diagnostic parameters: – Leukocytosis, – Alkaline phosphatase – Radiology ultrasonography
