Respiratory System unit-I cop.pptx
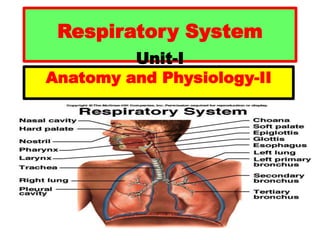
- 1. Respiratory System Unit-I Anatomy and Physiology-II
- 2. Objectives Define respiratory system. Define respiration. Describe the structure and the function of: • upper respiratory tract (Nose, Pharynx, Larynx) • lower respiratory tract (Trachea, Bronchial tree, lungs) Discuss the physiology of respiration by explaining the mechanism of: • Pulmonary Ventilation • External Respiration • Internal Respiration Discuss nervous control of respiration Briefly discuss the lung volumes & capacities
- 3. Respiratory System • Definition: A system consisting of lungs and air passages specialized for the intake of oxygen and exchange of gases with the blood. • Respiration: The exchange of oxygen and carbon dioxide between the atmosphere and the cells of the body. Respiration includes three things: 1) Ventilation of lungs (inspiration and expiration), 2) External respiration (the exchange of gases between lungs and blood) and Internal respiration (between blood and tissues), and 3) The use of oxygen in cellular metabolism.
- 4. Functions Respiratory and Non-Respiratory Functions Respiratory Functions are: 1. Pulmonary ventilation 2. Diffusion of O2 and CO2 b/w alveoli and blood 3. Transport of O2 and CO2 to and from tissues 4. Regulation of O2 and CO2 in blood and tissues
- 5. Functions cont.... Non Respiratory Functions are: • Air filtration • Protective/Cleansing Reflexes (SSC reflexes) • Olfaction • Vocalization • Defence mechanism..... Includes leukocytes, NK cells, macrophages, dendrite cells, mast cells, defensins and cathelicidins. • Maintenance of water • Regulation of body temperature • Regulation of PH • Secretion of ACE
- 6. Angiotensin-converting enzyme (EC 3.4. 15.1), or ACE, is a central component of the renin– angiotensin system (RAS), which controls blood pressure by regulating the volume of fluids in the body. ... Therefore, ACE indirectly increases blood pressure by causing blood vessels to constrict.
- 7. Respiratory Division Respiratory tract is divided into two: • Upper Respiratory Tract (URT): consists of nose, pharynx, and larynx. • Lower Respiratory Tract (LRT): consists of Trachea, Bronchi, bronchioles and lungs.
- 8. 8
- 9. Upper Respiratory Tract Nose: Apart from olfaction the nose has several functions: it warms, cleanses, and humidifies the inhaled air. It serves as a resonating chamber that amplifies the voice. • nasal cavity • nasal septum • mucous membrane – mucus – hair – olfactory receptors
- 10. Pharynx: Is a muscular tube extending about 13 cm (5 inch). It is divided into three regions: Nasopharynx -- Lies dorsal to the soft palate. -- Receives the eustachian (auditory) tubes. -- Houses pharyngeal tonsils.
- 11. Oropharynx -- The space between the soft palate and root of the tongue which extends inferiorly to the hyoid bone. Means it extends from the Uvula to the level of the hyoid bone. -- It contains palatine and lingual tonsils. Laryngopharynx It extends from the hyoid bone to the cricoid cartilage. Oropharynx and Laryngopharynx serve as a common passageway for both food and air.
- 13. Larynx • The larynx or voice box is a cartilaginous chamber about 4 cm long. • Its primary function is to keep food and drink out of the airway, but it also produces sound. • The superior opening of the larynx, the glottis (at the base of the tongue) is guarded by a flap of tissue called the epiglottis. • During swallowing, extrinsic muscles of the larynx pull the larynx upward toward the epiglottis, the tongue pushes the epiglottis downward, and the epiglottis directs food and drink into the esophagus dorsal to the airway. • The vestibular folds of the larynx also keeps food and drink out of the airway even if epiglottis is removed.
- 15. Larynx • There are nine cartilages, three unpaired and three paired. The unpaired cartilages of the larynx are thyroid, cricoid and epiglottis. • The paired cartilages of the larynx are the arytenoids, corniculates, and the cuneiforms. • Thyroid Cartilage: This forms the Adam's apple. It is usually larger in males than in females. The thyrohyoid membrane is a ligament associated with the thyroid cartilage that connects the thyroid cartilage with the hyoid bone.
- 16. Cricoid cartilage: A ring of hyaline cartilage that forms the inferior wall of the larynx. It is attached to the top of trachea. Epiglottis: A large, spoon-shaped piece of elastic cartilage. During swallowing, the pharynx and larynx rise. Elevation of the pharynx widens it to receive food and drink; elevation of the larynx causes the epiglottis to move down and form a lid over the glottis, closing it off.
- 17. Larynx cont…. • Paired Arytenoid Cartilage: They are smaller, the arytenoid cartilages are the most important because they influence the position and tension of the vocal folds. These are triangular pieces of hyaline cartilage located at the posterosuperior border of the cricoid cartilage. • Paired Corniculate Cartilage: Horn- shaped pieces of elastic cartilage located at the apex of each arytenoid cartilage. • Paired Cuneiform Cartilage: Club-shaped pieces of elastic cartilage located anteriorly to the corniculate cartilages.
- 18. • The first three are relatively large and unpaired. The superior one, the epiglottic cartilage, is a spoon shaped supportive plate in the epiglottis. The largest, the thyroid cartilage. It has an anterior peak, the laryngeal prominence, commonly called Adam’s apple, which is larger in males due to testosterone. Inferior to the thyroid cartilage is ring like cricoid cartilage which connects larynx to the trachea. • The remaining cartilages are smaller and occur in three pairs. Posterior to the thyroid cartilage are paired arytenoid, paired corniculate, and paired cuneiform cartilages.
- 20. Lower Respiratory Tract Trachea The trachea or windpipe is a rigid tube 12 cm long and 2.5 cm wide lying anterior to the esophagus. It is supported by about 20 C-shaped rings of hyaline cartilage, some of which we can palpate between larynx and sternum. The open part of the C faces posteriorly which allows room for the esophagus to expand when the swallowed food passes by. The cartilages are spanned by trachealis muscles.
- 21. Bronchi and Bronchial Tree At the level of fifth thoracic vertebra, the trachea divides into a right primary bronchus and left primary bronchus. The right primary bronchus is more vertical, shorter, and wider than the left. As a result, an aspirated object is more likely to enter and lodge in the right primary bronchus than the left. Like the trachea, the primary bronchi contain incomplete rings of cartilage and are lined by ciliated pseudostratified columnar epithelium.
- 22. • The point where the trachea divides into right and left primary bronchi is called carina. The mucous membrane of the carina is one of the most sensitive areas of the larynx and trachea for triggering a cough reflex. • On entering the lungs, the primary bronchi divide to form smaller bronchi called secondary bronchi. Each lobe in the lungs receive one secondary (lobar) bronchus. • The secondary bronchi continue to branch, forming still smaller bronchi, called tertiary (segmental) bronchi.
- 23. Cont… • These bronchi further divide into bronchioles (1 mm or less in diameter). • The portion of the lung ventilated by one bronchiole is called a pulmonary lobule. • The bronchioles further divide to form terminal bronchioles. This extensive branching from the trachea resembles an inverted tree and is commonly referred to as the bronchial tree.
- 24. Branches of Bronchial Tree Trachea ↓ Primary bronchi ↓ Secondary bronchi ↓ Tertiary bronchi ↓ Bronchioles ↓ Terminal bronchioles ↓ Respiratory bronchiole
- 26. • The larynx, trachea, and bronchial tree are lined mostly by ciliated pseudostratified columnar epithelium, which functions as a mucociliary escalator. That is, the mucous traps the inhaled particles and then the ciliary beating drives the mucus up to the pharynx where it is either swallowed or spit out. Respiratory unit includes: • 1. Respiratory bronchioles • 2. Alveolar ducts • 3. Alveolar sacs • 4. Antrum • 5. Alveoli
- 27. Lungs • Each lung is a somewhat conical shaped organ with a broad concave base resting on the diaphragm and a blunt peak called apex faces upward to clavicles. The broad costal surface is pressed against the rib cage, and the smaller concave mediastinal surface faces medially. The lung receives the bronchus, blood vessels, and nerves through its hilum, a slit in a mediastinal surface. The left lung is a little smaller than the right because of the heart tilting to the left giving indentation to the lung called cardiac impression or Cardiac notch.
- 28. The left lung has two lobes as superior and inferior lobe with a deep fissure between them called oblique fissure. The right lung has three lobes as superior, middle, and inferior lobe. Superior lobe is separated from the middle lobe by horizontal fissure and the inferior lobe from the middle one by oblique fissure.
- 29. Alveoli • An alveolus (plural alveoli) is pouch about 0.2 to 0.5 mm in diameter. • It is lined by simple squamous epithelium. • An alveolar sac consists of two or more alveoli that share a common opening. • The surface area of the alveoli is about 70 m2.The walls of alveoli consist of two types of alveolar epithelial cells. • Type I alveolar cells which are numerous and form a continuous layer. They are simple squamous epithelial cells. Gaseous exchange occurs here. • Type II alveolar cells also called septal cells, rounded or cuboidal, which are fewer in number and found between type I cells.
- 30. Alveoli cont…. • They secrete alveolar fluid to keep the surface moist. • Included the alveolar fluid is surfactant, a mixture of phospholipids and lipoproteins. • Surfactant lowers the surface tension of the alveolar fluid, which reduces the tendency of the alveoli to collapse. • Associated with the alveolar wall are alveolar macrophages (dust cells). They are phagocytes which remove fine dust particles and other debris and pathogens from the alveolar surface. • Alveoli are surrounded by a network of blood capillaries for gaseous exchange.
- 31. 31
- 32. Capillary Red Blood Cell Oxygen is picked up Carbon Dioxide is dropped off Wall of the air sac
- 33. Plural Membrane • The lungs are enclosed and protected by two layers of serous membrane which are collectively called plural membrane or pleura. The outer layer, called parietal membrane, lines the wall of the thoracic cavity. The inner layer, called the visceral membrane, covers the lungs themselves. Between the visceral and parietal membranes (pleurae) is a small space called pleural cavity. The plural cavity contains a small amount of lubricating fluid secreted by the serous membrane. This pleural fluid reduces the friction between the membranes when sliding over one another during breathing.
- 35. Respiratory Muscles Muscles of Inhalation: • Diaphragm • External intercostals • Sternocleidomastoid • Scalenes Muscles of Exhalation: • Internal intercostals • External oblique • Internal oblique • Transverse abdominis • Rectus abdominis
- 36. The scalene muscles are three paired muscles (anterior, middle and posterior), located in the lateral aspect of the neck. Collectively, they form part of the floor of the posterior triangle of the neck. The scalenes act as accessory muscles of respiration, and perform flexion at the neck.
- 37. Diaphragm • Is a skeletal muscle separating chest and abdomen • Inspiration: diaphragm contracts and increases thoracic space – air flows in • Expiration: diaphragm relaxes and decreases thoracic space – air flows out • Innervated by phrenic nerve fibers (C3, C4, C5)
- 38. 38 Mechanisms of Breathing: How do we change the volume of the rib cage ? Inhalation is ACTIVE process • Diaphragm Rib Cage Contract Diaphragm Volume •External Intercostal Muscles Intercostals Contract to Lift Rib Spine Ribs Volume Both actions occur simultaneously – otherwise not effective
- 39. Functions of Diaphragm • Diaphragm is the muscle of: • Inspiration • Abdominal straining • Weight-lifting • Thoracoabdominal pump
- 40. Nervous Control of Respiration Respiration is controlled by the respiratory center in the central nervous system. The respiratory muscles contract as a result of nerve impulses transmitted to them from centers in the brain and relax in the absence of nerve impulses. These nerve impulses are sent from clusters of neurons located bilaterally in the medulla oblongata and pones of the brain stem. This group of neurons, collectively called respiratory center, which is divided into three areas as:
- 41. 1.Medullary Rhythmicity Area: 2. It is located in the medulla oblongata. It controls the basic rhythm of respiration. There are inspiratory and expiratory areas. During quiet breathing, inhalation lasts for about 2 seconds and exhalation lasts for about 3 seconds. Inspiratory area establishes the basic rhythm of breathing by generating nerve impulses.
- 42. Inspiratory area sends impulses to the external intercostal muscles through intercostal nerves (T1 to T11) and to the diaphragm via the phrenic nerves (C3 to C5). When the nerve impulses reach the diaphragm and external intercostal muscles, the muscles contract and inhalation occurs. At the end of 2 seconds, the inspiratory area becomes inactive and nerve impulses cease. With no impulses arriving, the diaphragm and intercostal muscles relax for about 3 seconds, allowing lungs and thoracic wall to recoil. Then, the cycle repeats.
- 43. Nervous Control of Respiration cont… • The neurons of the expiratory area remain inactive during quiet breathing. • However, during forceful breathing nerve impulses from the inspiratory area activate the expiratory area Impulses causing contraction of the internal intercostal and abdominal muscles and thus forceful expiration occurs.
- 44. 2. Pneumotaxic Area: (pneumo= air; taxic= arrangement) In the upper pons, it transmits inhibitory impulses to the inspiratory area to turn off the inspiratory phase before the lungs become too full of air. Breathing rate is more rapid when the pneumotaxic area is more active. It means that it shortens the duration of inhalation. 3. Apneustic Area: In the lower pons of the brain stem, the apneustic area sends stimulatory impulses to the inspiratory area that activate it and prolong inhalation. It causes a long and deep inhalation. Thus pneumotaxic and apneustic area coordinate the transition between inhalation and exhalation.
- 45. Respiratory Volumes • Tidal Volume (TV): The amount of air normally inhaled or exhaled with one breath. (500 ml) • Inspiratory Reserve Volume (IRV): The amount of (additional) air forcefully inhaled after a normal tidal volume inhalation. (3000 ml) • Expiratory Reserve Volume (ERV): The amount of air forcefully exhaled after a normal tidal volume exhalation. (1200 ml) • Residual Volume (RV): The amount of air remaining in the lungs after maximum expiration. (1300 ml)
- 46. Respiratory Capacities • Vital Capacity (VC): Maximum amount of air expired after a maximum inspiratory effort. (4700 ml) VC= TV+IRV+ERV • Inspiratory Capacity (IC): Maximum amount of air inspired after a normal tidal expiration. (3500 ml) IC= TV+IRV • Functional Residual Capacity (FRC): Volume of air remaining in the lungs after a normal tidal volume expiration. (2500 ml) FRC= ERV+RV • Total Lung Capacity (TLC): The amount of air in lungs after a maximum inspiratory effort. (6000 ml) TLC= TV+IRV+ERV+ RV
- 47. Clinical Conditions • Inflammation of the pleural membrane is called pleurisy or pleuritis and as a result the accumulation of excess fluid in the pleural cavity is called pleural effusion. • The introduction of air into the plural cavity (either by surgical opening or stab or gunshot) is called pneumothorax while blood or pus in it is called hemothorax. The collapse of lungs is known as atelectasis (ateles = incomplete; ectasis = expansion).
- 48. Clinical terminology of ventilation • Apnea: Temporary cessation of breathing. • Dyspnea: Difficulty in breathing. Eg. SOB • Eupnea: Normal breathing. 12 to 15 b/m • Hyperpnea: Increased rate and depth of breathing. • Hyperventilation: Increased pulmonary ventilation leading to low blood level of CO2
- 49. Hypoventilation: Decreased pulmonary ventilation leading to increased blood level of CO2 Orthopnea: Dyspnea that occurs when a person is lying down. Tachypnea: Abnormal quick shallow breathing Bradypnea: Abnormal slow breathing. Hypoxia: Low oxygen level
- 50. Thank you