Viral encephalitis
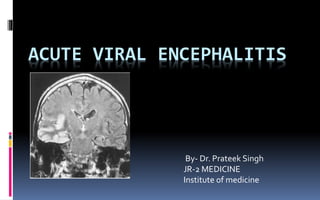
- 1. ACUTE VIRAL ENCEPHALITIS By- Dr. Prateek Singh JR-2 MEDICINE Institute of medicine
- 2. Introduction Encephalitis is defined as an inflammation of the brain caused either by infection, usually with a virus, or from a primary autoimmune process . Many patients with encephalitis also have evidence of associated meningitis (meningoencephalitis) and, in some cases, involvement of the spinal cord or nerve roots (encephalomyelitis, encephalomyeloradiculitis)
- 3. Definitions Meningoencephalitis - is an acute inflammatory process involving the meninges and to a variable degree, brain tissue. Is a common term that recognizes the overlap Encephalopathy - describes a clinical syndrome of altered mental status, manifesting as reduced consciousness or altered behaviour.
- 5. Causes of encephalopathy Systemic infection, Metabolic derangement (e.g. DKA) Toxins Drugs & Poisoning Hypoxia Trauma Vasculitis CNS infection.
- 6. Causes of encephalitis Infectious causes: – Viral Herpesvirus.- Hsv 1,2,6 , varicella-zoster, epstein bar , Alpha virus -eastern equine encephalitis Flaviviruses -west nile virus, st. louis virus, japanese encephalitis , Mumps. RSV, Rubeola, Rubella or Rabies (Occasionally) Bunyaviruses -California encephalitis virus serogroup, La Crosse virus) DengueVirus Measles virus
- 7. Bacterial (TBM) Ricketssial, Fungal Parasites - pl falciparum , Naegleria,Acanthamoeba,
- 8. Non infectious causes • Acute Disseminated Encephalomyelitis (ADEM) • Antibody-associated encephalitis, • Allergy: PostVaccine. • Heat Hyperpyrexia
- 9. Viral encephalitis WHO Clinical case definition of acute encephalitis syndrome • Person of any age, at any time of year, with • Acute onset of fever AND • Change in mental status (including symptoms such as confusion, disorientation, coma, or inability to talk)AND/OR • New onset of seizures (excluding simple febrile seizures) • Other early clinical findings can include an increase in irritability, somnolence or abnormal behaviour greater than that seen with usual febrile illness
- 10. herpes simplex virus type 1 (HSV1) is reportedly the commonest cause of adult sporadic encephalitis while varicella zoster virus (VZV) account for most of paediatric encephalitis Recent studies have identified many emerging encephalitic viruses such as Chandipura and Nipah viruses particularly in South Asia
- 13. Scenario in Nepal Although Japanese encephalitis virus (JEV) was thought to be a major cause for acute encephalitis syndrome, more non-Japanese encephalitis virus cases are reported. N 52 – Encephalitis 9 JE -33% HSV 1- 22.2% cause not known – 44.8%(4)
- 14. n-85 Meningitis – 65(70.58%) meningoencephalitis - 17 (20.0%) encephalitis - 8 (9.41%) JE-4
- 17. Pathogenesis Entry Respiratory/olfactory,GI, GU, skin, conjunctiva, blood Entry into the CNS Hematogenous dissemination Intraneural spread Neurovirulence Direct cytopathic effect Immune-mediated injury
- 18. Histopathologic Changes • Perivascular infiltration of mononuclear inflammatory cells • Reactive astrocytosis • Formation of glial nodules “owls eye” • Neuronophagia
- 19. Specific sites of viral predilection Temporal and inferior frontal lobes (HSV) Periventricular areas (CMV) Limbic system (RV) Cerebellum (VZV) Basal ganglia (JEV)
- 20. Clinical manifestations Fever Headache Lethargy Vomiting Impairment of consciousness (confusion, behavioral abnormalities, lethargy to coma ) Focal neurological signs aphasia, ataxia, upper or lower motor neuron patterns of weakness, involuntary movements (e.g., myoclonic jerks, tremor), and cranial nerve deficits (e.g., ocular palsies, facial weakness). Seizures.
- 21. may have hallucinations, agitation, personality change, behavioral disorders, and, at times, a frankly psychotic state. Involvement of the hypothalamic-pituitary axis may result in temperature dysregulation, diabetes insipidus, or the development of SIADH
- 22. occasionally accompanied by photophobia and a stiff neck. Physical examination characteristically reveals signs of nuchal rigidity, but its absence does not rule out the diagnosis.
- 23. Clinical clues Encephalitis associated with GIT symptoms -Enteroviruses, -Rotavirus, - Parechovirus. Encephalitis associated with respiratory illness -Influenza viruses: Myositis may also be associated. -Paramyxoviruses, - Bacteria.
- 24. Skin rash: – Meningococcemia, – Dengue, – Measles, –Varicella, – Rickettsial diseases, – Arboviral diseases, – Enteroviral encephalitis.
- 25. Parotitis (mumps) Pharyngitis & lymphadenopathy (EBV) Dermatomal rash (VZV) Herpangina (Coxsackie virus) Pneumonitis (LCMV)
- 27. CSF examination CSF pleocytosis ( >5 cells/μL) - 95% patients rare cases, a pleocytosis may be absent on the initia lumbar puncture (LP) but present on subsequent LPs. Mildly elevated protein Normal glucose concentration CSF pressure normal or slightly raised
- 28. Arboviruses (e.g., EEE virus or California encephalitis virus), mumps, and lymphocytic choriomeningitis virus (LCMV) may occasionally cell counts >1000/μL Atypical lymphocytes -EBV , CMV, HSV plasmacytoid or Mollaret-like large mononuclear cells –WNV About 20% of patients with encephalitis will have a significant number of red blood cells (>500/μL) in the CSF in a nontraumatic tap. hemorrhagic encephalitis of the type seen with HSV
- 29. CSF PCR primary diagnostic test for CNS infections caused by CMV, EBV, HHV-6, and enteroviruses. sensitivity (~96%) and specificity (~99%) of HSV CSF PCR negative HSV CSF PCR tests that were obtained early (≤72 h) following symptom onset and that became positive when repeated 1–3 days later. PCR results are generally not affected by ≤1 week of antiviral therapy
- 30. CSF culture is generally of limited utility in the diagnosis of acute viral encephalitis. Serum antibody determination is less useful for viruses with high seroprevalence rates in the general population such as HSV,VZV, CMV, and EBV antibodies to HSV-1 glycoproteins and HSV glycoprotein antigens have been detected in the CSF. Optimal detection of both HSV antibodies and antigen typically occurs after the first week of illness, limiting the utility of these tests in acute diagnosis. Useful in detecting illness is >1 week in duration and who are CSF PCR–negative for HSV .
- 31. EEG EEG is strongly recommended in any suspected case of acute encephalitis since it may help in distinguishing focal encephalitis from generalised encephalopathy. non-specific (slowing) with more characteristic changes (2–3 Hz periodic lateralised epileptiform discharges originating from the temporal lobes) limited to about half the cases in the later stages
- 32. Imaging CT subtle low density within the anterior and medial parts of the temporal lobe and the island of Reil (insular cortex) MRI
- 33. Temporal lobe involvement is strongly suggestive of herpes simplex virus (HSV) encephalitis, although other herpes viruses (eg,VZV, Epstein-Barr virus, human herpesvirus 6) areas of increased signal intensity in the frontotemporal, cingulate, or insular regions of the brain on T2 ,(FLAIR), or dwi MRI common in HSV encephalitis. thalamus or basal ganglia may be observed in the setting of encephalitis due to respiratory viral infection, Creutzfeld-Jacob disease, arbovirus, and tuberculosis
- 35. HSV
- 37. Varicella zoster
- 38. Management Emergent issues -ABC of resuscitation -Consider admission to ICU -Fluid restriction -Avoidance of hypotonic intravenous solutions -Suppression of fever -Management of raised ICP
- 39. Acyclovir is of benefit in the treatment of HSV and should be started empirically in patients with suspected viral encephalitis . deoxypyrimidine (thymidine) kinase acyclovir acyclovir-5′-monophosphate inhibiting viral DNA polymerase and by causing premature termination of nascent viral DNA chains
- 40. IV Acyclovir 10mg/kg every 8 hrly ( 30mg/kg total daily dose) * 21 days acyclovir should be diluted to a concentration ≤7 mg/mL , Each dose should be infused slowly over 1 h minimize the risk of renal dysfunction . Oral antiviral drugs with efficacy against HSV,VZV, and EBV, including acyclovir, famciclovir, and valacyclovir, have not been evaluated
- 41. IV Dexamethasone (10 mg every 6 h intravenously for 4 days) is efficacious . Ganciclovir and foscarnet, either alone or in combination, are often used in the treatment of CMV-related CNS infection. -Induction Ganciclovir 5 mg/kg every 12 h given IV over 1 h. - maintenance therapy of 5 mg/kg every day for an indefinite period -induction Foscarnet 60 mg/kg every 8 h administered by constant infusion over 1 h. For 14-21 days maintenance therapy (60–120 mg/kg per day) cont.
- 42. Intravenous ribavirin (15–25 mg/kg per day in divided doses given every 8 h) California encephalitis (LaCrosse) virus. No specific antiviral therapy of proven efficacy is currently available for treatment of WNV encephalitis Patients have been treated with interferon-α, ribavirin, an Israeli IVIg preparation that contains high-titer anti-WNV antibody (Omr-IgG-am)
- 43. Seizures should be treated with standard anticonvulsant regimens, and prophylactic therapy should be considered in view of the high frequency of seizures in severe cases of encephalitis
- 44. Features of raised ICP Asymmetric pupil, Tonic posturing, Papilloedema Managemant - Proper positioning: Head elevated 15-300. -Fluid Restriction: 2/3rd of maintenance. • 20% Mannitol 5 ml/kg over 10 – 15 min followed by 3 ml/kg every 6 hourly for 48 hrs then SOS, or -Acetazolamide: 50 – 75 mg/kg/day, or -Glycerin: 1 ml/kg/day through NGTube
- 47. Japanese encephalitis JEV is the most important cause of viral encephalitis in Asia. Primarily affects children under age 15 . Most JEV infections are mild (fever and headache) or without apparent symptoms transmitted to humans through bites from infected mosquitoes of the Culex species WHO recommends testing for JEV-specific IgM antibody in a single sample of cerebrospinal fluid (CSF) There is no antiviral treatment for patients with JE
- 48. Nipah virus encephalitis first recognised among pig farmers in Malaysia between 1998 and 1999 paramyxovirus (named Nipah virus) human illness was characterised by a history of direct contact with pigs in the livestock farm. short incubation period (two weeks), rapidly declining level of consciousness, prominent brain stem dysfunction, and high fatality rates. segmental myoclonus, areflexia, hypotonia, and dysautonomia Supportive care is the mainstay of treatment
- 49. Sequele Behavioural and psychiatric disturbances Epilepsy Post-encephalitic parkinsonism Memory difficulties Speech disturbances Permanent home care
- 50. Prognosis Factors of bad prognosis • Severe neurologic impairment • Older age • High viral load in CSF • Delay in initiation of therapy
- 51. Rehabilitation Periodic neuropsychiatric evaluation Speech therapy Physiotherapy Occupational rehabilitation
- 52. Take home message -Acute viral encephalitis is frequently devastating- -All patients with a febrile illness and altered behaviour or consciousness should be investigated promptly for viral encephalitis -Patients suspected need a lumbar puncture as soon as possible -Early institution of therapy improves prognosis
- 53. Thank you
