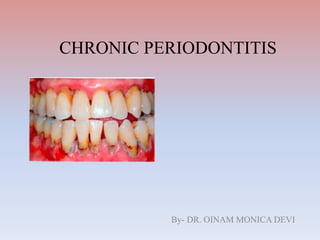
Chronic periodontitis
- 1. CHRONIC PERIODONTITIS By- DR. OINAM MONICA DEVI
- 2. Contents • Definition • Classification • Clinical Features • Clinical Diagnosis • Gingivitis as a risk factor for chronic periodontitis • Disease Distribution • Disease Severity • Symptoms • Disease Progression • Models to describe the rate of disease progression • Prevalence • Immunopathology • References
- 3. • Chronic periodontitis has been defined as "an infectious disease resulting in inflammation within the supporting tissues of the teeth, progressive attachment loss, and bone loss."‘ • This definition outlines the major clinical and etiologic characteristics of the disease: (1) Microbial plaque formation (2) Periodontal inflammation (3) Loss of attachment and alveolar bone Definition
- 4. Classification of periodontitis based on stages defined by severity Papapanou et al., 2018
- 5. Classification of periodontitis based on grades Papapanou et al., 2018
- 6. General Characteristics 1. Supragingival and subgingival plaque and calculus 2. Gingival swelling, redness, and loss of gingival stippling 3. Altered gingival margins (rolled, flattened, cratered papillae, recessions) 4. Pocket formation 5. Bleeding on probing 6. Attachment loss 7. Bone loss (angular/vertical or horizontal) 8. Root furcation involvement 9. Increased tooth mobility 10. Change in tooth position 11. Tooth loss Clinical Features
- 7. Clinical Diagnosis Detection of chronic inflammatory changes in the marginal gingiva Presence of periodontal pockets Loss of clinical attachment It is diagnosed radio graphically by: Localized or generalized loss of alveolar supporting bone, horizontal or vertical Differential diagnosis - Aggressive periodontitis • Based on the age of the patient, rate of disease progression over time, familial nature of aggressive disease, and relative absence of local factors
- 8. Gingivitis as a risk factor for chronic periodontitis • Gingival inflammation is invariably a component of chronic periodontitis. • Gingivitis precedes the onset of periodontitis, manifest after only days or weeks of plaque accumulation. • Destructive chronic periodontitis is a condition that in the majority of cases requires far longer periods of plaque and calculus exposure to develop.
- 9. Disease Distribution • Chronic periodontitis is considered a site-specific disease. • The clinical signs - inflammation, pocket formation, attachment loss, and bone loss are believed to be caused by the direct, site-specific effects of subgingival plaque accumulation. • Localized periodontitis: less than 30% of the sites demonstrate attachment loss and bone loss • Generalized periodontitis: less than 30% or more of the sites demonstrate attachment loss and bone loss
- 10. Localized chronic periodontitis A. Clinical view of anterior teeth showing minimal plaque and inflammation B. Radiographs showing presence of localized, vertical, angular bone loss on the distal side of the maxillary left first molar C. Surgical exposure of the vertical, angular defect associated with the chronic plaque accumulation and Carranza, 11th ed
- 11. Generalized chronic periodontitis A. Clinical view showing minimal plaque and inflammation B. Radiograph showing severe, generalized, horizontal pattern of bone loss Carranza, 11th ed
- 12. The pattern of bone loss Vertical Horizontal • When attachment and bone loss proceeds at a on one tooth surface • Vertical hone loss is usually associated with angular bony defects and intrabonv pocket formation. • When attachment and bone loss proceeds at a uniform rate • Horizontal bone loss is usually associated with suprabony pockets
- 13. Disease Severity • With increasing age, attachment loss and bone loss become more prevalent and more severe. • Slight (mild) periodontitis: No more than 1 to 2 mm of clinical attachment loss • Moderate periodontitis: 3 to 4 mm of clinical attachment loss • Severe periodontitis: 5 mm or more of clinical attachment loss
- 14. American Academy of Periodontology Task Force Report on the Update to the 1999 Classification of Periodontal Diseases and Conditions • This update addresses specific areas of concern with the current classification: 1. Attachment level, 2. Localized versus generalized periodontitis. 1. Use of attachment levels in diagnosis of periodontitis • In clinical practice, measurement of CAL is challenging, and time consuming. • Measuring the location of CEJ when the gingival margin is located coronal to the CEJ is difficult and may involve some guesswork when the CEJ is not readily evident via tactile sensation. • The clinician may chart probing depths alone or probing depths with a single recession measure at the mid-facial or mid-lingual and only when recession is actually present. American Academy of Periodontology Task Force Report on the Update to the 1999 Classification of Periodontal Diseases and Conditions. J Periodontol 2018; 86 (7), 835–38.
- 15. • Another common error occurs when gingival margin measures are charted as ‘‘0 mm’’ when in fact the gingival margin is not right at the level of the CEJ, resulting in attachment levels that are incorrectly charted as being equal to probing depth. • In general, a patient would have periodontitis when one or more sites had bleeding on probing, radiographic bone loss, and increased probing depth or clinical attachment loss. American Academy of Periodontology Task Force Report on the Update to the 1999 Classification of Periodontal Diseases and Conditions. J Periodontol 2018; 86 (7), 835–38.
- 16. Symptoms Slowly progressive disease , does not cause the affected individual to feel pain. Gingival bleeding during oral hygiene procedures or eating Black triangles between the teeth or tooth sensitivity in response to temperature changes (i.e., cold and heat). In patients with advanced attachment and bone loss, tooth mobility, tooth movement, tooth loss may be reported. Areas of localized dull pain that radiate to other areas of the mouth or head Presence of areas of food impaction Gingival tenderness or “itchiness”
- 17. Disease Progression • Patients appear to have the same susceptibility to plaque induced chronic periodontitis throughout their lives. • The rate of disease progression is usually slow but may be modified by systemic or environmental and behavioral factors. • Onset of chronic periodontitis can occur at any time, and the first signs may be detected during adolescence in the presence of chronic plaque and calculus accumulation. • Because of its slow rate of progression, however, chronic periodontitis usually becomes clinically significant in the raid-30s or later.
- 18. • Chronic periodontitis does not progress at an equal rate in all affected sites throughout the mouth. • Some involved areas may remain static for long periods, whereas others may progress more rapidly. • More rapidly progressive lesions occur most frequently in interproximal areas' and may also be associated with areas of greater plaque accumulation and inaccessibility to plaque control measures.
- 19. The continuous model • Disease progression is slow and continuous • Affected sites show a constantly progressive rate of destruction throughout the duration of the disease The ramdom model, or episodic-burst model • Periodontal disease progresses by short bursts of destruction followed by periods of no destruction • Random pattern with respect to the tooth sites affected and the chronology of the disease process. The asynchronus, multiple- burst model of disease • Periodontal destruction occurs around affected teeth during defined periods of life • Bursts of activity are interspersed with periods of inactivity or remission • Chronology of these bursts of disease is asynchronous for individual teeth or groups of teeth. Models to describe the rate of disease progression
- 20. Socransky et al. 1984 Various models of disease progression Socransky, S. S., Haffajee, A. D., Goodson, J. M., & Lindhe, J. (1984). New concepts of destructive periodontal disease. J Clin Periodontol 1984; 11(1); 21–32
- 21. Prevalence • Chronic periodontitis increases in prevalence and severity with age, generally affecting both genders equally. • Periodontitis is an age-associated, not an age-related, disease. • It is not the age of the individual that causes the increase in disease prevalence, but rather the length of time that the periodontal tissues are challenged by chronic plaque accumulation.
- 23. RISK FACTORS FOR DISEASE 1. Prior History of Periodontitis 2. Microbiogolical Aspects 3. Local Factors 4. Systemic Factors 5. Immunologic Factors 6. Environmental & Behavioural Factors 7. Genetic Factors
- 24. Categories of Risk Elements for Periodontal Disease Risk - Defined as is the probability that an individual will get a specific disease in a given period. RISK FACTORS: Tobacco smoking Diabetes Pathogenic bacteria Microbial tooth deposits RISK DETERMINANTS: Genetic factors Age Gender Socioeconomic status Stress RISK INDICATORS: HIV/Aids Osteoporosis Infrequent dental visits RISK MARKERS/PREDICTORS: Previous history of periodontal disease Bleeding on probing
- 25. Prior History of Periodontitis • Disease predictor • Puts patients at greater risk for developing further loss of attachment and bone, given a challenge from bacterial plaque accumulation • A chronic periodontitis patient who has been successfully treated will develop continuing disease it plaque is allowed to accumulate • Emphasizes the need for continuous monitoring and maintenance of periodontitis patients to prevent recurrence of disease
- 26. B. Microbiological Factors • Plaque accumulation primary initiating agent in the etiology of chronic periodontitis. • Attachment and bone loss are associated with an increase in the proportion of gram-negative organisms in the sub-gingival plaque biofilm. • Specific plaque hypothesis- with specific increases in organisms (pathogenic and virulent) Bacteroides gingivalis, Bacteroides forsythus, and Treponema denticola, “Red complex,”. • Impart a local effect on the cells of the inflammatory response and the cells and tissues of the host, resulting in a local, site-specific disease process.
- 27. • Role of immune response-may not depend on the presence of one specific bacterium or bacterial complexes alone. • The occurrence of periodontitis depends on the individual immune response that modifies the onset and progression of the disease. • Poly-microbial disease- It is the result of multi-species infection with a number of different bacteria that influence the pro-inflammatory immune response of the host and produces proteases that directly influence tissue stability and host immune response
- 28. Role of Viruses - Slots in 2010, A high periodontal load of active Epstein–Barr virus or cytomegalovirus is statistically associated with aggressive periodontitis, and latent herpes virus infections are preferentially found in chronic periodontitis and gingivitis sites. • Diagnostic difficulties and natural fluctuation of periodontal herpes virus Role of Archea - Pérez-Chaparro et al. in 2014, “association” studies. The results suggested the association of 17 species or phylotypes have an association with disease. Virus Prevalence Herpes simplex 37-100% Epstein-Barr virus 3-89% Cytomegalovirus 0.3-89%
- 29. C. Local Factors Calculus Sub gingival and/or overhanging margins of restorations Carious lesions that extend subgingivally Furcations Crowded and malaligned teeth Root grooves and concavities Plaque retentive factors are important in the development and progression of chronic periodontitis because they retain plaque microorganisms in close proximity to the periodontal tissues, providing an ecologic niche for plaque growth and maturation.
- 30. D. Systemic Factors Syndromes- Haim-munk syndrome, Ehler-Danlos Syndrome, Kindlers syndrome and Cohen syndrome Human immunodeficiency virus acquired immunodeficiency syndrome Osteoporosis A severely unbalanced diet Stress Dermatologic, hematologic and neoplastic factor interfere with periodontal inflammatory responses. Severe systemic disease such as diabetes mellitus, cardiovascular disease, stroke and lung disease
- 31. E. Immunologic Factors Patient may show alteration in their peripheral monocytes, which are related to the reduced reactivity of lymphocyte or an enhanced B-cell response. B-cells, macrophage, periodontal ligament cells, gingival fibroblast, and epithelial cells synthesize pro-inflammatory mediators (e.g. Interleukin-1 beta, Interleukin-6, Interleukin-8, prostaglandin E-2, tumor necrosis factor – alpha) and modify innate and adaptive immune response at periodontal site. Onset progression and severity of disease depend on the individual hosts immune response
- 32. F. Environmental and Behavioural Factors Smoking Smoking is a major risk factor for development and progression of generalized chronic periodontitis. Periodontitis is affected by smoking in a dose dependent manner. The intake of more than 10 cigarettes per day tremendously increases the risk of disease progression as compared to nonsmoker and former smoker. As compared with non-smoker, the following features are found in smokers- • Increased probing pocket depth of more than 3 mm • Increased attachment loss • More recession • Increased bone loss, • Greater incidence of furcation involvements • Increased tooth loss • Fewer sign of gingivitis (Less bleeding on probing)
- 33. Stress The mechanisms by which stress could affect periodontal disease progression and wound healing have been divided into two main categories: • (i) Health-impairing behaviors such as poor oral hygiene, increased tobacco and alcohol consumption, and poor nutritional intake; • (ii) Pathophysiological factors that lead to higher glucocorticoid and catecholamine levels which indirectly affect hormonal, inflammatory and immunological profiles, leading to an increased susceptibility to periodontal disease. Patients with CP often report the experience of family or work related stress. Positive correlation between cortisol level and periodontal indices, bone loss, and missing teeth has been recorded. Risk indicator
- 34. G. Genetic Factors – Each factor in turn directly related to individual genetic condition. – Genetic variation such as single nucleotide polymorphism (SNPs), and genetic copy number variations may directly influence innate and adaptive immune response as well as the structure of periodontal tissue. – Studies of monozygotic twins suggest a genetic component to chronic periodontitis, but the influences of bacterial transmission among family members and environmental effects make it difficult to interpret a complex interaction.
- 35. Factors Risk of tooth loss IL-1 genotype 2.7 times Heavy smokers 2.9 times Heavy smokers + IL-1 genotype 7.7 times – Interleukin 1-a and interleukin 1-ß polymorphism is associated with an increased susceptibility to a more aggressive form of chronic periodontitis in subjects of Northern European origin. – McGuire & Nunn 1999, followed 42 patients with periodontitis for 14 years and showed that the risk of tooth loss as a result of periodontal disease. – Genome- wide association studies have revealed a significant association between periodontitis and coronary heart disease. – A complex genotype is likely to be identified for many different clinical forms of periodontitis.
- 37. Immunopathology CHARACTERISTICS OF A PROGRESSIVE LESION- • Apical migration of plaque on the root surface, accompanied by sub-gingival calculus formation. • Alveolar bone is destroyed within 2 mm of the plaque front, • Attachment loss and bone resorption cyclical/ intermittent • A predominance of plasma cells • Lesion is further encapsulated by a fibrous band surrounding the infiltrated tissues; however, local fibroblasts in the body of the lesion are reduced in number and altered in appearance. • Relatively few macrophages in the advanced lesion, and it is thought that B cells may be the major source of interleukin-1 and other pro-inflammatory cytokines that produces matrix metalloproteinases, especially by fibroblasts. Results in degradation of the surrounding extracellular matrix. CP is characterized by cycles of progression and stability
- 38. Stable T-cell lesion is mediated by Th1 cells, while the progressive B-cell, plasma cell lesion is associated with Th2 cells. The majority of these T cells are also CD45RO-positive memory cells. Stable, predominantly T-cell lesion and a progressive B-cell lesion. • Recently, Th-17 cells are identified as a separate phenotype • The signature cytokine of these cells is IL-17A, also produce IL-21 and IL- 22 • IL- 17A is important for the recruitment of neutrophils as they up-regulate CXCL8 expression. • Th17 cells may be involved in Th1 modulation and enhanced inflammatory mediators’ production by gingival fibroblasts in periodontal disease • Th17 cells may be primary source of RANKL production in periodontal disease. KV Arun, JISP 2010
- 39. References 1. Newman, Takei, Klokkevold, Carranza. Carranza’s, clinical periodontology, 10th ed; 632-34. 2. Newman, Takei, Klokkevold, Carranza. Carranza’s, clinical periodontology, 13th ed; 1880-1916. 3. Papapanou, P. N., Sanz, M., Buduneli, N., Dietrich, T., Feres, M., Fine, D. H., … Tonetti, M. S. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Periodontol 2018;89: S173-82. 4. American Academy of Periodontology Task Force Report on the Update to the 1999 Classification of Periodontal Diseases and Conditions. J Periodontol 2015; 86 (7), 835–38. 5. Socransky, S. S., Haffajee, A. D., Goodson, J. M., & Lindhe, J. (1984). New concepts of destructive periodontal disease. J Clin Periodontol; 11 (1): 21–32. 6. Pérez-Chaparro, P. J., Gonçalves, C., Figueiredo, L. C., Faveri, M., Lobão, E., Tamashiro, N., … Feres, M. Newly Identified Pathogens Associated with Periodontitis. J Dent Res 2014; 93 (9), 846–58. 7. McGuire, M. K., & Nunn, M. E. (1999). Prognosis Versus Actual Outcome. IV. The Effectiveness of Clinical Parameters and IL-1 Genotype in Accurately Predicting Prognoses and Tooth Survival. J Periodontol;70 (1) : 49–56.
- 40. THANK YOU
Editor's Notes
- (may be the first self-reported sign of disease occurrence.
