thyroid hormone.pdf
- 1. Thyroid hormone By Dr Marwa Mahfouz
- 2. Actions • The thyroid gland facilitates normal growth and maturation by maintaining a level of metabolism in the tissues that is optimal for normal function • as They are catabolic hormones and increase the breakdown of fats (to FFA), carbohydrates (cause hyperglycemia) and proteins (cause weight loss). They are also calorigenic and increase basal metabolic rate (BMR).
- 3. Actions • The two major thyroid hormones are triiodothyronine (T3; the most active form) and thyroxine (T4). Inadequate secretion of thyroid hormone (hypothyroidism) leads to myxedema in adults and bradycardia, cold intolerance, and mental and physical slowing. In children leads to cretinism, this can cause mental retardation and dwarfism.
- 4. Actions • By contrast, excess secretion of thyroid hormones (hyperthyroidism) can cause tachycardia and cardiac arrhythmias (atrial fibrillation can occur), body wasting, nervousness, tremor, and heat intolerance.
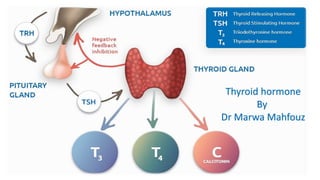
- 5. Thyroid hormone synthesis and secretion • Thyroid gland contains follicular cells and parafollicular (C) cells. Former secretes thyroid hormones (T3 and T4) whereas the latter is responsible for the secretion of calcitonin.
- 6. Thyroid hormone synthesis and secretion • The thyroid gland is made up of multiple follicles that consist of a single layer of epithelial cells surrounding a lumen filled with thyroglobulin (the storage form of thyroid hormone). Thyroid function is controlled by TSH (thyrotropin), which is synthesized by the anterior pituitary.
- 7. Thyroid hormone synthesis and secretion • Note: • The hypothalamic thyrotropin releasing hormone (TRH) governs the generation of TSH.
- 8. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • Iodine is first taken up in the follicular cell with the help of Na+: I– symporter (NIS).
- 9. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • Iodine is first taken up in the follicular cell with the help of Na+: I– symporter (NIS).
- 10. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • After entry in the follicular cells, iodine is oxidized to form iodinium (I- ) ions. These ions combine with tyrosine residues of thyroglobulin to form mono-iodo tyrosine (MIT) and di-iodo- tyrosine (DIT). This process is known as organification of iodine.
- 11. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • DIT combines with DIT to form tetra- iodo-thyronine (T4) and with MIT to form tri-iodo-thyronine (T3). This process is known as coupling
- 12. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • Oxidation, organification and coupling reactions are catalyzed by thyroid peroxidase enzyme.
- 13. Thyroid hormone synthesis and secretion • Thyroid hormones are synthesized and stored in thyroid follicles in the following manner: • After formation, T3 and T4 are transported to the follicles where these remain stored as colloid. On stimulation via TSH, these hormones are released in the circulation. In the liver and kidney, T4 is converted to T3 (peripheral conversion) and taken up by target tissues.
- 16. Treatment of hypothyroidism • Main indication of thyroid hormones is hypothyroidism (cretinism, myxedema and myxedema coma). • Hypothyroidism usually results from autoimmune destruction of the gland and is diagnosed by elevated TSH. • Levothyroxine (T4) is preferred over T3 (liothyronine) or T3/T4 combination products (liotrix) for the treatment of hypothyroidism.
- 17. Treatment of hypothyroidism • Levothyroxine is better tolerated than T3 preparations and has a longer half-life. It is dosed once daily, and steady state is achieved in 6 to 8 weeks. Toxicity is directly related to T4 levels and manifests as nervousness, palpitations and tachycardia, heat intolerance, and unexplained weight loss.
- 18. Treatment of hypothyroidism • Myxedema coma is an emergency situation, in which liothyronine (only indication) can also be used (It should be used cautiously in patients with heart diseases like AF).
- 19. Treatment of hyperthyroidism (thyrotoxicosis) • Grave’s disease, an autoimmune disease that affects the thyroid, is the most common cause of hyperthyroidism. In these situations, TSH levels are low due to negative feedback. [Note: Feedback inhibition of TRH occurs with high levels of circulating thyroid hormone, which, in turn, decreases secretion of TSH.]
- 20. Treatment of hyperthyroidism (thyrotoxicosis) • The goal of therapy is to decrease synthesis and/or release of additional hormone. This can be accomplished by removing part or all of the thyroid gland, by inhibiting synthesis of the hormones, or by blocking release of hormones from the follicle.
- 22. Treatment of hyperthyroidism (thyrotoxicosis) • 1. Removal of the thyroid • This can be accomplished surgically or by destruction of the gland with radioactive iodine (131I), which is selectively taken up by the thyroid follicular cells. • Most patients become hypothyroid after radioactive iodine and require treatment with levothyroxine.
- 23. Treatment of hyperthyroidism (thyrotoxicosis) • 2. Inhibition of thyroid hormone synthesis (Thyroid Peroxidase Inhibitors) • Thyroid peroxidase enzyme catalyzes three reactions (oxidation, organification and coupling) in the process of thyroid hormone synthesis. • Carbimazole, methimazole and propylthiouracil act by inhibiting this enzyme. PTU also blocks the peripheral conversion of T4 to T3.
- 24. Treatment of hyperthyroidism (thyrotoxicosis) • Note: • These drugs inhibit the formation of new thyroid hormones but their action manifests only when already stored pool of T3 and T4 is utilized as they have no effect on thyroglobulin already stored in the gland.
- 25. Treatment of hyperthyroidism (thyrotoxicosis) • Note: • Thus, a lag period of 1-3 weeks is present and clinical effects may be delayed until thyroglobulin stores are depleted. These drugs can rarely cause reversible agranulocytosis (most serious adverse effect)
- 26. Treatment of hyperthyroidism (thyrotoxicosis) • Methimazole is preferred over PTU because it has a longer half-life, allowing for once-daily dosing, and a lower incidence of adverse effects. • However, PTU is recommended during the first trimester of pregnancy due to a greater risk of teratogenic effects with methimazole. PTU has been associated with hepatotoxicity and, rarely, agranulocytosis.
- 27. Treatment of hyperthyroidism (thyrotoxicosis) • Note: Propylthiouracil has been found to be hepatotoxic and FDA has declared methimazole as preferred drug over propylthiouracil for all patients except in first trimester of pregnancy and lactation.
- 28. Treatment of hyperthyroidism (thyrotoxicosis) • Thyroid peroxidase inhibitors are used for: • the control of thyrotoxicosis in patients with Graves’ disease and toxic nodular goiter. • These are also used in young patients before performing thyroidectomy. • Another use of antithyroid drugs is to make the patient euthyroid before application of radioactive iodine.
- 29. Treatment of hyperthyroidism (thyrotoxicosis) • 3. Inhibitors of Thyroid Hormone Release • A pharmacologic dose of iodide inhibits the iodination of tyrosines (“Wolff Chaikoff effect”), but this effect lasts only a few days. https://www.youtube.com/watch?v=ZWnWvWoUW6M
- 30. Treatment of hyperthyroidism (thyrotoxicosis) • 3. Inhibitors of Thyroid Hormone Release • Sodium iodide, potassium iodide and Lugol’s solution act as ‘thyroid constipating agents’ by inhibiting the release of T3 and T4 from thyroglobulin. • These drugs are the fastest acting anti- thyroid drugs but is not useful for long-term therapy; the thyroid ceases to respond to the drug after a few weeks.
- 31. Treatment of hyperthyroidism (thyrotoxicosis) • 3. Inhibitors of Thyroid Hormone Release • In sensitive individuals, acute reaction consisting of swelling of lips, angioedema, fever, joint pain and petechial hemorrhages can occur. Chronic overdose of iodides is called iodism.
- 32. Treatment of hyperthyroidism (thyrotoxicosis) • 3. Inhibitors of Thyroid Hormone Release Major symptoms are inflamed mucus membranes, increase in secretions (salivation, lacrimation and rhinorrhoea), headache, rashes and gastrointestinal distress. These drugs may also cause flaring up of acne in adolescents.
- 33. Treatment of hyperthyroidism (thyrotoxicosis) • 4. Drugs Causing the Destruction of Thyroid Gland • I131 is the most commonly used radioactive iodine with a half-life of 8 DAYS (stable isotope of iodine is I127). • When administered (as sodium salts, orally), these are actively taken up by the thyroid gland and stored in the colloid. Concentration of radioactive iodine by the thyroid gland is responsible for its selective thyroid destroying effect.
- 34. Treatment of hyperthyroidism (thyrotoxicosis) • 4. Drugs Causing the Destruction of Thyroid Gland • I131 can be used for the treatment of hyperthyroidism but response is slow (maximum response may take 3 months). Thyroid peroxidase inhibitors are administered to make the patient euthyroid. • After a gap of 5 days (after stopping anti-thyroid drugs), radioactive iodine is given and thyroid peroxidase inhibitor treatment is resumed till the effect of I131 starts.
- 35. Treatment of hyperthyroidism (thyrotoxicosis) • 4. Drugs Causing the Destruction of Thyroid Gland • Radioactive iodine therapy is primarily indicated for patients older than 35 years, those with heart disease and in the presence of other contra- indications of surgery. These drugs are not suitable for young children and in the pregnancy. Another disadvantage of radioactive iodine is that if hypothyroidism develops, it is permanent (requiring life long T4 therapy).
- 36. Thyroid storm • Thyroid storm presents with extreme symptoms of hyperthyroidism. The treatment of thyroid storm is the same as for hyperthyroidism, except that the drugs are given in higher doses and more frequently. β-Blockers, such as metoprolol or propranolol antagonize the sympathetic effects of thyrotoxicosis like tremors, tachycardia, palpitations and anxiety. Note: Propranolol inhibits the peripheral conversion of T4 to T3
