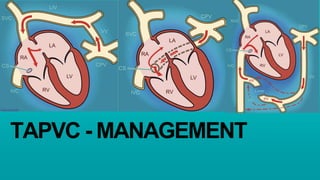
Management of tapvc
- 2. TYPES
- 6. DIAGNOSIS
- 7. DIAGNOSIS • Clinical Presentation • ECG • Imaging ✦ CXR ✦ Echocardiography ✦ Contrast CT ✦ Catheter Angiography
- 8. ECG • Obstructed TAPVC ✦ Right ventricular hypertrophy ★ qR complex or only R wavein right chest leads ✦ Right atrial enlargement is infrequent. ★ Only seen in cardiac TAPVC with obstruction at ASD level • Non-obstructed TAPVC ✦ Resembles that of an OS-ASD ✦ Right axis deviation ✦ Right atrial and ventricular enlargement ✦ Incomplete right bundle branch block pattern.
- 9. CXR • Non Obstructed ✦ Cardiomegaly ✦ RV Apex ✦ RA and RV Enlargement ✦ Enlarged PA Segment ✦ Pulmonary Plethora
- 10. CXR • Obstruction ✦ Vertical Vein - Normal Cardiac Size ✦ ASD - Cardiomegaly ✦ White out / Ground Glass Opacity lung field ★ DDX • Meconium Aspiration Syndrome • Hyaline Membrane Disease ✦ Enlarged PA Segment
- 12. OBSTRUCTED TAPVC • CXR ✦ Plethoric Lung Fields / Ground Glass appearance ✦ Absence of cardiomegaly ✦ Indistinct cardiac silhouette • DDX ✦ Meconium Aspiration ✦ Hyaline Membrane Disease
- 13. ECHOCARDIOGRAPHY • Diagnostic and Investigation of Choice • Important Observation ✦ PV not draining into LA ✦ Type of TAPVC ★ Cardiac - Dilated CS ★ Supracardiac - Dilated innominate vein and SVC ★ Infracardiac - Dilated IVC ✦ Insertion of Vertical Vein ✦ Narrowing of Vertical Vein ✦ Adequacy of ASD
- 14. ✦ RA and RV Dilatation ✦ TR ✦ PAH ✦ RV Function ✦ Small LA ✦ LV size and Function ✦ PV Narrowing ✦ Size ✦ Doppler - Velocity > 2m/s ✦ Coexisting Congenital Defect ✦ VSD ✦ PDA
- 17. CARDIAC CATHERISATION • Always Diagnostic • Indication ✦ Measure PVRI / Reversibility in older children ✦ Diagnosis not clear on Echocardiography ✦ Intervention - BAS, PV dilatation, Vertical Vein Dilatation • PA/PV Angiogram ✦ PA injection with venous follow through preferred over direct PV injection ✦ Anatomy of TAPVC ✦ Type ✦ Drainage ✦ Site of Obstruction
- 18. CARDIAC CATHERISATION • Oximetry ✦ Similar saturation in all chamber • Drawbacks ✦ Delays management ✦ Aggravate pulmonary edema ✦ Contrast related
- 22. CROSS SECTIONAL IMAGING • CT and MRI • Indication ✦ Complex pulmonary venous drainage pattern, not clearly defined on Echo ✦ Heterotaxy syndromes with TAPVC ✦ Post operative Pulmonary vein Stenosis • Drawbacks ✦ Contrast related ✦ Requires sedation
- 23. SC- TAPVC CTA
- 24. CARDIAC TAPVC • CTA ✦ Common chamber opening into CS ✦ Small LA ✦ Dilated RA ✦ ASD
- 25. IC-TAPVC CTA
- 26. DECISION MAKING
- 27. FACTORS TO CONSIDER • Age of Patient • Weight of the patient • Type of TAPVC • Obstructed or Non Obstructed • Clinical Status of Patient ✦ Ventilator ✦ Inotropes ✦ Acidosis • LV and RV function • PAH • Presence of PVOD
- 28. INDICATION FOR SURGERY • Diagnosis of TAPVC
- 29. TIMING OF SURGERY • Immediate Emergency Surgery ✦ Sick Neonate ✦ Obstructed TAPVC • Urgent ✦ Presentation before 6 months • As soon as feasible ✦ Presentation between 6 months to 1 year • >1 year age ✦ PVRI < 8 U.m2 ✦ PVRI >8 U.m2, but reversible
- 32. MEDICAL THERAPY • Only supportive in managing TAPVC • Intended to stabilise the patient before surgery • Goals ✦ Correct acidosis and hypotension ✦ Fluid management ✦ Mechanical ventilation • Prostaglandin ✦ Helpful in keeping ductus venosus open in infra-diaphragmatic TAPVC ✦ Other forms - Increases right to left shunting and systemic desaturation
- 34. BAS • Short term palliation • Indication ✦ Sick neonate with TAPVC ✦ Obstruction at ASD level • Goal ✦ Improve mixing ✦ Improve cardiac output ✦ Relief systemic and pulmonary congestion • Technically challenging ✦ Small left atrium ✦ Echocardiographic guidance is often helpful • Success of a BAS ✦ Drop in pulmonary artery pressure ✦ Increase in systemic pressure ✦ Drop in systemic saturation
- 35. BALLON DILATION/ STENTING VV • Occasionally performed to relieve obstruction • Indication ✦ Sick neonates presenting with obstructed TAPVC • Technically challenging
- 39. PRINCIPLES • Principle ✦ On CPB or Circulatory arrest ✦ Identify 4 PV, common chamber and dissect and loop vertical vein ✦ Achieve wide tension free non obstructing anastomosis between common chamber and LA ✦ Avoiding purse stringing of suture line ✦ Divert all pulmonary venous blood to LA ✦ Close intra-atrial communication ★ Patch Material • Pericardium • Dacron ( Polyethylene terephthalate ) ✦ Ligate vertical vein close to insertion into systemic vein
- 40. CLOSED APPROACH William H Muller
- 42. SC - TAPVC - POSTERIOR APPROACHPaul Ebert
- 46. SC-TAPVC RIGHT BIATRIAL APPROACH Shumacker and King
- 48. RIGHT SIDED APPROACH - LA Kirklin
- 51. TRANS RA TRANS LA Cooley
- 56. CS-TAPVC -CS CUT BACK Malm
- 60. IC- TAPVC - ORIENTATION OF COMMON CHAMBER
- 66. CONTROVERSIES
- 67. PRIMARY SUTURELESS VS CONVENTIONAL REPAIR
- 69. OVERALL AND EARLY MORTALITYOverallMortalityEarlyMortality
- 70. VERTICAL VEIN LIGATION • Proponents of Ligation ✦ Large left to right shunt with RV volume overload ✦ Requires additional procedure for closure ✦ No survival benefit ✦ Ligating the vertical vein close to its insertion into the systemic vein, the vertical vein adds to the reservoir of the LA • Proponents of Leaving the vertical vein open ✦ Serves as a pop off for the non compliant left heart ✦ Spontaneously closes over time ✦ Less turbulent immediate postoperative course, especially in obstructed TAPVC
- 74. Surviours - 12 Not ligated vertical vein - 10 Median Follow up - 4.7 years Spontaneous closure - 5 Required Ligation - 4
- 76. LA ENLARGMENT • Proponents ✦ Increase in reservoir capacity ✦ Better LV Filling and Cardiac Output ✦ Decreased incidence of Pulmonary venous hypertension and reactive PAH • Oponents ✦ Incorporation of common venous sinus enlarges LA adequately ✦ Patch material is non contractile • Literature ✦ No significant difference in survival with LA enlargement ★ Katz NM, Kirklin JW, Pacifico AD. Concepts and practices in surgery for total anomalous pulmonary venous connection. Ann Thorac Sure 1977
- 77. PFO • Benefits ✦ Popoff for RV in patients with severe PAH ✦ Maintain cardio output at the cost of desaturation • Drawbacks ✦ Risk of paradoxical embolism ✦ Significant right to left requiring additional procedure for closure
- 79. PHYSIOLOGY • Preoperative ✦ Small LA ✦ Underfilled LV ✦ RA/RV Volume Overload ✦ Increased Qp • Postoperative ✦ Offloading of Right Heart ✦ Volume loading in not compliant LV
- 80. ANTICIPATED PROBLEMS • Non Compliant LV ✦ > Acute Dilatation > Septal Dysfunction > LV Dysfunction > Increase in LA Pressure • Non Compliant LA > Surges in LA pressure > ✦ PVH > PAH Crisis ✦ Pulmonary Hemorrhage > Stiff Lungs • Post Op PAH > RV Dysfunction > LCOS • LV Dysfunction > LCOS
- 81. COMPLICATIONS OF SURGERY • Bleeding • LV diastolic dysfunction (Low Compliance) • RV dysfunction • Pulmonary hypertension and PAH crisis • Gradient across anastomosis • Pulmonary vein stenosis
- 82. STRATEGIES • Avoid surges is LA pressure ✦ Fluid Restriction ✦ Avoid Fluid Bolus • Inodilators ✦ Dobutamine/Milrinone • Afterload Reduction - Vasodilators ✦ NTG/SNP • Avoid Triggers of PAH • Refractory PAH ✦ Echo - R/o Anastamotic stenosis/ Pulmonary vein stenosis ✦ NO Ventilator ✦ Mechanical Support
- 83. ISSUES • LV dysfunction ✦ Inodilators ✦ Monitor LA pressure ✦ Positive pressure ventilation ✦ Prevent fluid overloading ( Low Threshold for PD) ✦ ECMO
- 84. ISSUES • PAH ✦ Adequate sedation in the first 24-48 hours ✦ Avoid ★ Hypercardbia ★ Hypoxia ★ Acidosis ✦ Adequate lung recruitment ✦ Pulmonary dilatation ★ SNP, Milrinone ✦ Avoid triggers of PAH ★ Suctioning ✦ Refractory Cases - NO Ventilation
- 85. PEARLS • Avoid Fluid Bolus • Accept low BP if no Lactic Acidosis • Avoiding Weaning when LA pressure high • Low threshold for Peritoneal dialysis • Avoid triggers of PAH • Elective CPAP after extubation helps with LV dysfunction
- 86. RESULTS
- 87. MORTALITY • Early Mortality ✦ STS - 10-30% ✦ Individual Centers - 2-20% • Late Mortality ✦ Very few late mortality ✦ Survival depends on early survival
- 88. MODES OF DEATH • Cardiac Failure • PAH Crisis • Sepsis • Pathophyiological correlates to mortality ✦ Preoperative cardiopulmonary instability ★ Acidosis ★ Ventilator Requirement ✦ Post op PAH Crisis ★ Preop Lung Injury ★ CPB related ★ Postop Acidosis ✦ Progression of Pulmonary Vein Stenosis
- 89. • Cause of Death • Low Cardiac Output ( 70%) • Sepsis (30%)
- 90. RISK FACTORS FOR EARLY DEATH • Low birth weight • Infracardiac TAPVC • Mixed TAPVC • Obstructed TAPVC • Poor preoperative physiological state • Postop Pulmonary Venous Obstruction • Increased PVRI • Single ventricle physiology
- 92. Over all mortality <2 Kg Mixed vs Others Postop PVO Reoperation PVO Reoperation Mixed TAPVC
- 94. HEMODYNAMIC OUTCOME • RV - Size decreases to normal • PA - Pressure normalises • LA ✦ Size increases to normal ✦ Compliance below normal • LV ✦ Volume increases to normal ✦ Systolic function improves to normal • Rhythm ✦ Ectopic pacemaker activity due to damage of internodal preferential pathway
- 95. FUNCTIONAL STATUS • Most surviving patients are NYHA 1 ary and musculoskeletal exercise performance after repair for total anomalous pulmonary venous connection during infancy. J Thorac Cardiovasc Surg 2007;133:1533-9.
- 99. AIIMS RESULT • Patients - 248 (168 boys, 80 girls) • Age - 1 day to 24 years (median 8 months) ; 145 infants • Weight - 2 to 52 kg (median 5 kg). 70% were less than the 50th percentile of predicted weight for age and sex. • Type ✦ Supracardiac - 134 (54%) ✦ Cardiac - 80 (32.2%) ✦ Infracardiac - 9 (3.6%) ✦ Mixed - 25 (10.1%) • Obstructed TAPVC - 50 (20.2%) • Mod-Sev PAH - 76 patients (30.2%) Choudhary SK, Bhan A, Sharma R, et al. Total anomalous pulmonary venous connection: surgical experience in Indians. Indian Heart J. 20
- 100. • Emergency surgery - 45 patients (18.1%) • Circulatory Arrest - 114 • Early Mortality - 45 (19.1%) ✦ Pulmonary arterial hypertensive crisis - 19 ✦ Low cardiac output syndrome - 17 • Risk Factors ✦ Age < 1 year (OR 2.16; 95% CI: 1.22-3.82, p=0.008) ✦ Severe pulmonary arterial hypertension (AR 5.86; 95% CI: 2-17, p=0.001), ✦ Emergency surgery (OR 3.65; 95% CI: 1.59-8.38, p=0.002) • Late Mortality - 4 • Follow-up ranged from 1 to 180 months (median 48 months). • Actuarial survival at 12 years - 92.6% +/- 2.8%. Choudhary SK, Bhan A, Sharma R, et al. Total anomalous pulmonary venous connection: surgical experience in Indians. Indian Heart J. 20
- 101. REOPERATION
- 102. ANASTAMOTIC STENOSIS • Incidence - 10% • Occurs early postoperative period ✦ Later anastomosis grows and child grows • Factors which decrease risk ✦ Open anastomosis ✦ Wide anastomosis ✦ Absorbable monofilament sutures ✦ No difference between continuous and interrupted suture technique • Reoperation ✦ Risk of restenosis ✦ Poor outcome
- 103. PULMONARY VEIN STENOSIS • Incidence - 5- 15% • Usually occurs within the first 6 months • Pathophysiology ✦ Diffuse fibrotic thickening of PV ✦ Localised narrowing at PV-LA junction ✦ May or may not be associate with anastomotic stenosis • Presentation ✦ Progressive Dyspnea • Investigation ✦ Echocardiography ★ PV Flow velocity > 2m/s ✦ Cross Sectional Imaging
- 108. CTA • Narrowing in PV just proximal to insertion into common chamber/LA
- 109. PULMONARY VEIN STENOSIS • Treatment ✦ Steroids or Chemotherapy to minimise fibrosis ✦ Balloon dilatation/stenting ✦ Ostial endarterectomy of intimal hyperplasia IRevising the common pulmonary vein to left atrium anastomosis with or without patch enlargement ✦ Sutureless repair
- 115. • Developed PVO - 71/406 (17.5%) ✦ Cardiac - 9/67 (13%) ✦ Supracardiac -25/205 (12%) ✦ Infracardiac - 25/110 (23%) ✦ Mixed - 11/37 (30%) • Median time to diagnosis from surgery - 49days ( 0 - 5.9 yrs) ✦ Diagnosed within 6 months of surgery - 59/71 (83%) ✦ Echo - 30% , Angiography - 54% and CT/MRI - 16% • Intervention ✦ 60 patients required intervention ✦ 56 received intervention ★ 50% required more than 1 intervention
- 118. THANK YOU
Editor's Notes
- Vertical vein was looped and snared in all patients. Loosened in all patients with obstructed TAPVC
- Group 1 - No VV ligation Group 2 - VV ligation
