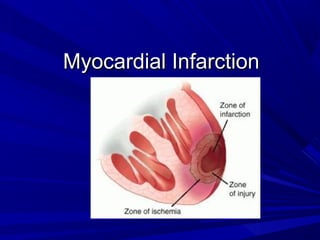
Acute Myocardial Infarction
- 3. Definitions • Acute coronary syndrome is defined as myocardial ischemia due to myocardial infarction (NSTEMI or STEMI) or unstable angina • Unstable angina is defined as angina at rest, new onset exertional angina (<2 months), recent acceleration of angina (<2 months), or post revascularization angina
- 4. Sponsored Medical Lecture Notes – All Subjects USMLE Exam (America) – Practice
- 6. ACS-STEMIACS-STEMI ACUTE CORONARY SYNDROMES No ST elevation ST elevation Unstable angina NSTEMI STEMIStable angina
- 8. BackgroundBackground Myocardial Infarction if the rapidMyocardial Infarction if the rapid development of myocardial necrosis by adevelopment of myocardial necrosis by a critical imbalance between oxygen supplycritical imbalance between oxygen supply and demand to the myocardiumand demand to the myocardium
- 9. ClassificationClassification Anatomic or morphologicAnatomic or morphologic Transmural= Full thicknessTransmural= Full thickness Non-transmural= Partial thicknessNon-transmural= Partial thickness ECGECG Q wave MIQ wave MI Non Q wave MINon Q wave MI Does not distinguish transmural from a non-Does not distinguish transmural from a non- transmural MI as determined by pathologytransmural MI as determined by pathology
- 10. Diagnosis • Dx of acute coronary syndrome is based on history, physical exam, ECG, cardiac enzymes • Patients can then be divided into several groups – Non-cardiac chest pain (i.e., Gastrointestinal, musculoskeletal, pulmonary embolus) – Stable angina – Unstable angina – Myocardial infarction (STEMI or NSTEMI) – Other cardiac causes of chest pain (i.e., aortic dissection, pericarditis)
- 11. HistoryHistory Chest Pain- anterior precordium tightnessChest Pain- anterior precordium tightness Pain may radiate to jaw, neck andPain may radiate to jaw, neck and epigastriumepigastrium Dyspnea- angina equivalent, poor LVDyspnea- angina equivalent, poor LV functionfunction Nausea/abdominal pain with posterior MINausea/abdominal pain with posterior MI AnxietyAnxiety
- 13. Differential Diagnosis of Chest Pain Cardiac Ischemic Angina Unstable angina AMI Non-ischemic Pericarditis Aortic dissection Valvular Myositis
- 14. Differential Diagnosis of Chest Pain Non-cardiac Gastroesophageal Causes GERD Esophageal spasm PUD Boerhaave’s Syndrome Cholecystitis
- 15. Differential Diagnosis of Chest Pain Non-cardiac Non-gastroesophageal Pneumothorax Pulmonary embolism Musculoskeletal Somatoform disorders
- 16. Chest Pain-Diagnosis History and Physical ECG Cardiac serum markers
- 17. HistoryHistory Nausea with and without vomitingNausea with and without vomiting Diaphoresis or sweatingDiaphoresis or sweating Syncope or near syncopeSyncope or near syncope Elderly present with MS changes, fatigue,Elderly present with MS changes, fatigue, syncope or weaknesssyncope or weakness As many as half of MI are clinically silentAs many as half of MI are clinically silent
- 18. PhysicalPhysical The physical exam can often beThe physical exam can often be unremarkableunremarkable HypertensionHypertension HypotensionHypotension Acute valvular dysfunction may be presentAcute valvular dysfunction may be present RalesRales Neck vein distentionNeck vein distention
- 19. PhysicalPhysical Third heart sound may be presentThird heart sound may be present A fourth heart sound poor LV complianceA fourth heart sound poor LV compliance DysrhythmiasDysrhythmias Low grade feverLow grade fever
- 20. CausesCauses Most frequent cause is rupture of anMost frequent cause is rupture of an atherosclerotic lesion within coronary wallatherosclerotic lesion within coronary wall with subsequent spasm and thrombuswith subsequent spasm and thrombus formationformation Coronary artery vasospasmCoronary artery vasospasm Ventricular hypertrophyVentricular hypertrophy HypoxiaHypoxia Coronary artery emboliCoronary artery emboli
- 21. CausesCauses CocaineCocaine ArteriesArteries Coronary anomaliesCoronary anomalies Aortic dissectionAortic dissection Pediatrics Kawasaki disease, TakayasuPediatrics Kawasaki disease, Takayasu arteritisarteritis Increased afterload which increasesIncreased afterload which increases myocardial demandmyocardial demand
- 22. Risk factors for atherosclerosisRisk factors for atherosclerosis AgeAge Male genderMale gender SmokingSmoking Hypercholesterolemia and triglyceridemiaHypercholesterolemia and triglyceridemia Diabetes MellitusDiabetes Mellitus Poorly controlled hypertensionPoorly controlled hypertension
- 23. Risk factors for atherosclerosisRisk factors for atherosclerosis Family HistoryFamily History Sedentary lifestyleSedentary lifestyle
- 24. Mechanisms of Myocardial damageMechanisms of Myocardial damage The severity of an MI is dependent of threeThe severity of an MI is dependent of three factorsfactors The level of the occlusion in the coronaryThe level of the occlusion in the coronary The length of time of the occlusionThe length of time of the occlusion The presence or absence of collateralThe presence or absence of collateral circulationcirculation
- 25. Cardiac BiomarkersCardiac Biomarkers Cardiac biomarkers are protein moleculesCardiac biomarkers are protein molecules released into the blood stream fromreleased into the blood stream from damaged heart muscledamaged heart muscle Since ECG can be inconclusive ,Since ECG can be inconclusive , biomarkers are frequently used tobiomarkers are frequently used to evaluate for myocardial injuryevaluate for myocardial injury These biomarkers have a characteristicThese biomarkers have a characteristic rise and fall patternrise and fall pattern
- 26. Troponin T and ITroponin T and I These isoforms are very specific forThese isoforms are very specific for cardiac injurycardiac injury Preferred markers for detectingPreferred markers for detecting myocardial cell injurymyocardial cell injury Rise 2-6 hours after injuryRise 2-6 hours after injury Peak in 12-16 hoursPeak in 12-16 hours Stay elevated for 5-14 daysStay elevated for 5-14 days
- 27. Creatinine Kinase ( CK-MB)Creatinine Kinase ( CK-MB) Creatinine Kinase is found in heart muscleCreatinine Kinase is found in heart muscle (MB), skeletal muscle (MM), and brain(MB), skeletal muscle (MM), and brain (BB)(BB) Increased in over 90% of myocardialIncreased in over 90% of myocardial infractioninfraction However, it can be increased in muscleHowever, it can be increased in muscle trauma, physical exertion, post-op,trauma, physical exertion, post-op, convulsions, and other conditionsconvulsions, and other conditions
- 28. Creatine Kinase (MB)Creatine Kinase (MB) Time sequence after myocardial infarctionTime sequence after myocardial infarction Begins to rise 4-6 hoursBegins to rise 4-6 hours Peaks 24 hoursPeaks 24 hours returns to normal in 2 daysreturns to normal in 2 days MB2 released from heart muscle andMB2 released from heart muscle and converted to MB1.converted to MB1. A level of MB2 > or = 1 and a ratio ofA level of MB2 > or = 1 and a ratio of MB2/MB1 > 1.5 indicates myocardialMB2/MB1 > 1.5 indicates myocardial injuryinjury
- 29. MyoglobinMyoglobin Damage to skeletal or cardiac muscleDamage to skeletal or cardiac muscle release myoglobin into circulationrelease myoglobin into circulation Time sequence after infarctionTime sequence after infarction Rises fast 2hoursRises fast 2hours Peaks at 6-8 hoursPeaks at 6-8 hours Returns to normal in 20-36 hoursReturns to normal in 20-36 hours Have false positives with skeletal muscleHave false positives with skeletal muscle injury and renal failureinjury and renal failure
- 30. Renal Failure and RenalRenal Failure and Renal TransplantationTransplantation Diagnostic accuracy of serum markers ofDiagnostic accuracy of serum markers of cardiac injury are altered in patients withcardiac injury are altered in patients with renal failurerenal failure Cardiac troponins decreased diagnosticCardiac troponins decreased diagnostic sensitivity and specificity in patientssensitivity and specificity in patients receiving renal replacement therapyreceiving renal replacement therapy Current data show levels of troponin I areCurrent data show levels of troponin I are unaltered while levels of troponin T mayunaltered while levels of troponin T may be elevatedbe elevated
- 31. CBCCBC Leukocytosis may be observed withinLeukocytosis may be observed within several hours after myocardial injury andseveral hours after myocardial injury and returns returns to levels within thereturns returns to levels within the reference range within one weekreference range within one week
- 32. Chemistry ProfileChemistry Profile Potassium and magnesium levels shouldPotassium and magnesium levels should be monitored and correctedbe monitored and corrected Creatinine levels must be consideredCreatinine levels must be considered before using contrast dye for coronarybefore using contrast dye for coronary angiography and percutanousangiography and percutanous revascularizationrevascularization
- 33. C-reactive Protein (CRP)C-reactive Protein (CRP) C- reactive protein is a marker of acuteC- reactive protein is a marker of acute inflammationinflammation Patients without evidence of myocardialPatients without evidence of myocardial necrosis but with elevated CRP are atnecrosis but with elevated CRP are at increased risk of an eventincreased risk of an event
- 34. Chest X-RayChest X-Ray Chest radiography may provide clues toChest radiography may provide clues to an alternative diagnosis ( aortic dissectionan alternative diagnosis ( aortic dissection or pneumothorax)or pneumothorax) Chest radiography also revealsChest radiography also reveals complications of myocardial infarctioncomplications of myocardial infarction such as heart failuresuch as heart failure
- 36. EchocardiographyEchocardiography Use 2-dimentional and M modeUse 2-dimentional and M mode echocardiography when evaluating overallechocardiography when evaluating overall ventricular function and wall motionventricular function and wall motion abnormalitiesabnormalities Echocardiography can also identifyEchocardiography can also identify complications of MI ( eg. Valvular orcomplications of MI ( eg. Valvular or pericardial effusion, VSD)pericardial effusion, VSD)
- 37. ElectrocardiogramElectrocardiogram A normal ECG does not exclude ACSA normal ECG does not exclude ACS High probability include ST segmentHigh probability include ST segment elevation in two contiguous leads orelevation in two contiguous leads or presence of q wavespresence of q waves Intermediate probability ST depressionIntermediate probability ST depression T wave inversions are less specificT wave inversions are less specific
- 40. Progression of wave changesProgression of wave changes Hyperacute T wave changes - increased T waveHyperacute T wave changes - increased T wave amplitude and width; may also see ST elevation.amplitude and width; may also see ST elevation. Marked ST elevation with hyperacute T waveMarked ST elevation with hyperacute T wave changes (transmural injury)changes (transmural injury) Pathologic Q waves, less ST elevation, terminal TPathologic Q waves, less ST elevation, terminal T wave inversion (necrosis) (Pathologic Q waveswave inversion (necrosis) (Pathologic Q waves are usually defined as durationare usually defined as duration >>0.04 s or >25%0.04 s or >25% of R-wave amplitude)of R-wave amplitude) Pathologic Q waves, T wave inversion (necrosisPathologic Q waves, T wave inversion (necrosis and fibrosis)and fibrosis) Pathologic Q waves, upright T waves (fibrosisPathologic Q waves, upright T waves (fibrosis))
- 41. Current of Injury Patterns
- 43. Electrocardiographic evolution of myocardial infarction. After the first few minutes the T waves become tall, pointed and upright and ST segment elevation develops After the first few hours the T waves invert, the R wave voltage is decreased and Q waves develop. After a few days the ST segment returns to normal. After weeks or months the T wave may return to upright but the Q wave remains.
- 45. This picture shows a normal sinus complex. The ST segment is on the iso-electric line. At the onset of pain the ECG would be normal but the ST segment would soon start to change. In this picture, the T wave has grown taller. Within an hour the ST segment would be noticeably elevated, indicating the onset on myocardial necrosis. (tissue death). This is the point at which we would be aiming to administer the thrombolytic (clot-busting) drug. If thrombolysis is administered, we would be looking for specific changes on the ECG. A 50% reduction in ST segment elevation is a good indicator of success. In this picture, the ST elevation has reduced by more than 50% from picture 2. We would expect to see these changes within 90 minutes of administering thrombolysis. You can also see the T wave invertion is much deeper. This is a good sign of reperfusion. (blood flow returning to the damaged area.) 24 hours later, the ST segment may have returned to the iso-electric line. In this picture you can see the ST segment is back on the iso-electric line but the T wave remains inverted. It may stay inverted for days, weeks or months. 6. In some cases, after a few months the ECG looks relatively normal. Compare picture 6 with picture 1. They look much the same but for the deep Q wave in picture 6. A deep Q wave is an indicator of myocardial tissue death and will remain on the ECG. A "pathological" Q wave is not "time-specific". It may be there from a previous heart attack and therefore is not part of the criteria for evaluating an Acute Myocardial Infarction.
- 46. MIs can be locatedMIs can be located in thein the anterior,anterior, septal,septal, lateral,lateral, posterior,posterior, or inferior wallsor inferior walls of the left ventricle.of the left ventricle. LOCATION OF THE INFARCTIONLOCATION OF THE INFARCTION
- 47. Diagram of the coronary arteries arising from the aorta and encirclingDiagram of the coronary arteries arising from the aorta and encircling the heart. Some of the coronary veins also are shown.the heart. Some of the coronary veins also are shown.
- 49. Inferior MIInferior MI Pathologic Q waves and evolving ST-Pathologic Q waves and evolving ST- T changes in leads II, III, aVF.T changes in leads II, III, aVF. Q waves usually largest in lead III,Q waves usually largest in lead III, next largest in lead aVF, and smallestnext largest in lead aVF, and smallest in lead IIin lead II
- 51. Inferoposterior MIInferoposterior MI ECG changes are seen in anterior precordial leadsECG changes are seen in anterior precordial leads V1-3, but are theV1-3, but are the mirror imagemirror image of an anteroseptalof an anteroseptal MI,MI, Increased R wave amplitude and duration (i.e., aIncreased R wave amplitude and duration (i.e., a "pathologic R wave" is a mirror image of a"pathologic R wave" is a mirror image of a pathologic Q).pathologic Q). R/S ratio in V1 or V2 >1 (i.e., prominent anteriorR/S ratio in V1 or V2 >1 (i.e., prominent anterior forces).forces). Hyperacute ST-T wave changes: i.e., STHyperacute ST-T wave changes: i.e., ST depression and large, inverted T waves in V1-3.depression and large, inverted T waves in V1-3. Late normalization of ST-T with symmetricalLate normalization of ST-T with symmetrical upright T waves in V1-3.upright T waves in V1-3. Often seen with inferior MI (i.e., "inferoposteriorOften seen with inferior MI (i.e., "inferoposterior MI")MI")
- 54. Right Ventricular MIRight Ventricular MI Right Ventricular MI (only seen withRight Ventricular MI (only seen with proximal right coronary occlusion;proximal right coronary occlusion; i.e., with inferior family MI's)i.e., with inferior family MI's) ECG findings usually requireECG findings usually require additional leads on right chest (V1Radditional leads on right chest (V1R to V6R, analogous to the left chestto V6R, analogous to the left chest leads)leads) ST elevation,ST elevation, >>1mm, in right chest1mm, in right chest leads, especially V4R.leads, especially V4R.
- 56. Right Ventricular MIRight Ventricular MI
- 58. High Lateral MIHigh Lateral MI
- 59. What is the diagnosis?What is the diagnosis?
- 60. MI plus LBBBMI plus LBBB Q waves of any size inQ waves of any size in twotwo or more of leads I, aVL, V5, oror more of leads I, aVL, V5, or V6 (See below: one of the most reliable signs and probablyV6 (See below: one of the most reliable signs and probably indicatesindicates septalseptal infarction, because the septum is activatedinfarction, because the septum is activated early from the right ventricular side in LBBB).early from the right ventricular side in LBBB). Reversal of the usual R wave progression in precordialReversal of the usual R wave progression in precordial leads.leads. Notching of the downstroke of the S wave in precordialNotching of the downstroke of the S wave in precordial leads to the right of the transition zone (i.e., before QRSleads to the right of the transition zone (i.e., before QRS changes from a predominate S wave complex to achanges from a predominate S wave complex to a predominate R wave complex); this may be a Q-wavepredominate R wave complex); this may be a Q-wave equivalent.equivalent.
- 61. MI plus LBBBMI plus LBBB Notching of the upstroke of the S wave in precordial leadsNotching of the upstroke of the S wave in precordial leads to the right of the transition zone (another Q-waveto the right of the transition zone (another Q-wave equivalent).equivalent). rSR' complex in leads I, V5 or V6 (the S is a Q-waverSR' complex in leads I, V5 or V6 (the S is a Q-wave equivalent occurring in the middle of the QRS complex)equivalent occurring in the middle of the QRS complex) RS complex in V5-6 rather than the usual monophasic RRS complex in V5-6 rather than the usual monophasic R waves seen in uncomplicated LBBB; (the S is a Q-wavewaves seen in uncomplicated LBBB; (the S is a Q-wave equivalent).equivalent). "Primary" ST-T wave changes (i.e., ST-T changes in the"Primary" ST-T wave changes (i.e., ST-T changes in the same direction as the QRS complex rather than the usualsame direction as the QRS complex rather than the usual "secondary" ST-T changes seen in uncomplicated LBBB);"secondary" ST-T changes seen in uncomplicated LBBB); these changes may reflect an acute, evolving MI.these changes may reflect an acute, evolving MI.
- 62. Old MI plus LBBOld MI plus LBB
- 63. Non-Q wave MINon-Q wave MI Recognized by evolving ST-T changes over time without theRecognized by evolving ST-T changes over time without the formation of pathologic Q waves (in a patient with typical chestformation of pathologic Q waves (in a patient with typical chest pain symptoms and/or elevation in myocardial-specific enzymes)pain symptoms and/or elevation in myocardial-specific enzymes) Although it is tempting to localize the non-Q MI by the particularAlthough it is tempting to localize the non-Q MI by the particular leads showing ST-T changes, this is probably only valid for the STleads showing ST-T changes, this is probably only valid for the ST segment elevation pattern.segment elevation pattern. Evolving ST-T changes may include any of the following patterns:Evolving ST-T changes may include any of the following patterns: Convex downward ST segment depression only (common)Convex downward ST segment depression only (common) Convex upwards or straight ST segment elevation only.Convex upwards or straight ST segment elevation only. Symmetrical T wave inversion only (common)Symmetrical T wave inversion only (common)
- 64. Non-Q wave MINon-Q wave MI
- 65. Differential MI patternDifferential MI pattern WPW preexcitation (WPW preexcitation (negativenegative delta wavedelta wave may mimic pathologic Q waves)may mimic pathologic Q waves) IHSS (septal hypertrophy may makeIHSS (septal hypertrophy may make normal septal Q waves "fatter" therebynormal septal Q waves "fatter" thereby mimicking pathologic Q waves)mimicking pathologic Q waves) LVH (may have QS pattern or poor R waveLVH (may have QS pattern or poor R wave progression in leads V1-3)progression in leads V1-3) RVH (tall R waves in V1 or V2 may mimicRVH (tall R waves in V1 or V2 may mimic true posterior MI)true posterior MI) Complete or incomplete LBBB (QS wavesComplete or incomplete LBBB (QS waves or poor R wave progression in leads V1-3)or poor R wave progression in leads V1-3)
- 66. Differential MI patternDifferential MI pattern Pneumothorax (loss of right precordial R waves)Pneumothorax (loss of right precordial R waves) Pulmonary emphysema and cor pulmonale (lossPulmonary emphysema and cor pulmonale (loss of R waves V1-3 and/or inferior Q waves withof R waves V1-3 and/or inferior Q waves with right axis deviation)right axis deviation) Left anterior fascicular block (may see small q-Left anterior fascicular block (may see small q- waves in anterior chest leads)waves in anterior chest leads) Acute pericarditis (the ST segment elevation mayAcute pericarditis (the ST segment elevation may mimic acute transmural injury)mimic acute transmural injury) Central nervous system disease (may mimic non-Central nervous system disease (may mimic non- Q wave MI by causing diffuse ST-T wave changesQ wave MI by causing diffuse ST-T wave changes
- 67. Localizing Infarcts on the 12 Lead ECG anterior Lateral - Cx posterior anterior Inferior - RCA Inferior - RCA Ant – sep - LAD Ant – sep - LAD septal Anterior - LAD anterior
- 68. ECG #1- 68 year old with chest pain for 3 daysECG #1- 68 year old with chest pain for 3 days
- 69. ECG #2- 66 year old man with 1 hour historyECG #2- 66 year old man with 1 hour history of chest pressureof chest pressure
- 70. ECG #4 - 62 year old with profuse diaphoresisECG #4 - 62 year old with profuse diaphoresis and vomitingand vomiting
- 71. ECG #6- 45 year old female with onset of chestECG #6- 45 year old female with onset of chest discomfort 2 hours ago – PMH ?Cancerdiscomfort 2 hours ago – PMH ?Cancer
- 72. ECG #7 – 50 year old man with crushing substernal chest pain for 30 minutes
- 73. ECG #8- 72 year old female with history ofECG #8- 72 year old female with history of HTN found unconsciousHTN found unconscious
- 74. ECG #9- 67 year old man with PMH of MI inECG #9- 67 year old man with PMH of MI in respiratory failure due to acute CHFrespiratory failure due to acute CHF
- 75. ECG #10- Chest pain radiating to the jaw inECG #10- Chest pain radiating to the jaw in a 41 year old womana 41 year old woman
- 76. ECG #1- 32 year old with chest pain at a party
- 77. Anterolateral MI
- 78. Anterolateral MI - II
- 79. Anterolateral MI - III
- 80. 65 year old with acute chest pain
- 81. Anterior MI
- 86. 53 year old with severe light headedness, nausea, diaphoresis, and upper abdominal pain. Bloods pressure 85/palp. Acute Inferoposterior MI
- 87. R R R R R
- 88. Acute Lateral MI
- 89. ECG #4 - 62 year old with profuse diaphoresis and vomiting
- 90. ECG #7 – Acute Posterior MI - Old inferior MI
- 91. Inferior MI
- 92. (MR# 866159) -77 year old male with chest pain and palpitation
- 93. Anterior MI
- 94. LVH with ST-T Wave Changes
- 99. TherapyTherapy The goals of therapy in AMIThe goals of therapy in AMI are the expedient restorationare the expedient restoration of normal coronary flow andof normal coronary flow and the maximum salvage ofthe maximum salvage of functional myocardiumfunctional myocardium
- 100. REPERFUSION STRATEGY
- 101. • Patients receiving fibrinolysis should be risk-stratified to identify need for further revascularization with percutaneous coronary intervention (PCI) or coronary artery bypass graft surgery (CABG). • All patients should receive late hospital care and secondary prevention of STEMI. Fibrinolysis Primary PCI Noninvasive Risk Stratification Late Hospital Care and Secondary Prevention PCI or CABG Not PCI Capable PCI Capable Rescue Ischemia driven Options for Transport of Patients With STEMI andOptions for Transport of Patients With STEMI and Initial Reperfusion TreatmentInitial Reperfusion Treatment
- 102. Treatments Oxygen Aspirin Nitroglycerin Morphine Beta - blocker Heparin/ Lovenox Clopidogrel Fibrinolytics Percutaneous Coronary Intervention (PCI)
- 103. Percutaneous transluminal coronary angioplasty (PTCA procedure) is another important method of thrombolysis and reperfusion.
- 105. Bypass surgery, is indicated in the following situations associated with myocardial infarction: PTCA procedure failure (with persistent pain or hemodynamic instability), PTCA risk procedure due to the coronary anatomy (left common trunk stenosis), coronary occlusion occurred after catheterization, cardiogenic shock.
- 106. Antiplatelet AgentsAntiplatelet Agents Aspirin at lease 160mg immediatelyAspirin at lease 160mg immediately Interferes with function of cyclooxygenaseInterferes with function of cyclooxygenase and inhibits the formation of thromboxaneand inhibits the formation of thromboxane ASA alone has one of the greatest impactASA alone has one of the greatest impact on the reduction of MI mortality.on the reduction of MI mortality. Clopidogrel, ticlopidine, have not beenClopidogrel, ticlopidine, have not been shown in any large scal trail to be superiorshown in any large scal trail to be superior to Aspirin in acute MIto Aspirin in acute MI
- 107. Supplemental OxygenSupplemental Oxygen Because MI impairs the circulatoryBecause MI impairs the circulatory function of the heart, oxygen extraction byfunction of the heart, oxygen extraction by the heart and other tissues may bethe heart and other tissues may be diminisheddiminished Supplemental oxygen should beSupplemental oxygen should be administered to patient with symptomsadministered to patient with symptoms and or signs of pulmonary edema or pulseand or signs of pulmonary edema or pulse oximetry readings less than 90%.oximetry readings less than 90%.
- 108. NitratesNitrates IV nitrates to all patients with MI andIV nitrates to all patients with MI and congestive heart failure, persistentcongestive heart failure, persistent ischemia, hypertension, or large anteriorischemia, hypertension, or large anterior wall MIwall MI Primary benefit vasodilator effectPrimary benefit vasodilator effect Metabolized to nitric oxide in the vascularMetabolized to nitric oxide in the vascular endothelium, relaxes endotheliumendothelium, relaxes endothelium Vasodilatation reduces myocardial oxygenVasodilatation reduces myocardial oxygen demand and preload and afterloaddemand and preload and afterload
- 109. Beta-blockersBeta-blockers Recommended within 12 hours of MIRecommended within 12 hours of MI symptoms and continued indefinitelysymptoms and continued indefinitely Reduces Myocardial mortality byReduces Myocardial mortality by decreasing arrythmogenic deathdecreasing arrythmogenic death Decrease the rate and force of myocardialDecrease the rate and force of myocardial contraction and decreases overall oxygencontraction and decreases overall oxygen demanddemand
- 110. Unfractionated heparinUnfractionated heparin Forms a chemical complex withForms a chemical complex with antithrombin III inactivates both freeantithrombin III inactivates both free thrombin and factor Xathrombin and factor Xa Recommended in patients with MI whoRecommended in patients with MI who undergo PTCA or fibrinolytic therapy withundergo PTCA or fibrinolytic therapy with alteplasealteplase
- 111. Low-molecular weight heparinLow-molecular weight heparin Direct activity against factors Xa and IIaDirect activity against factors Xa and IIa Proven to be effective in treating ACS thatProven to be effective in treating ACS that are characterized by unstable angina orare characterized by unstable angina or non ST- elevation MInon ST- elevation MI Their fixed doses are easy to administerTheir fixed doses are easy to administer and laboratory testing to measure theirand laboratory testing to measure their therapeutic effect is not necessary makestherapeutic effect is not necessary makes them attractive alternative of un-them attractive alternative of un- fractionated heparinfractionated heparin
- 113. ThrombolyticsThrombolytics Indicated with MI and ST segmentIndicated with MI and ST segment elevation greater than 0.1mV in 2elevation greater than 0.1mV in 2 contiguous ECG leads, or new onsetcontiguous ECG leads, or new onset LBBB, who present less than 12 hours butLBBB, who present less than 12 hours but not more than 24 hours after symptomnot more than 24 hours after symptom onsetonset The most critical variable in achievingThe most critical variable in achieving successful fibrinolysis is time formsuccessful fibrinolysis is time form symptom onset to drug administrationsymptom onset to drug administration
- 116. ThrombolyticsThrombolytics As a class the plasminogen activators haveAs a class the plasminogen activators have been shown to restore coronary blood flow in 50-been shown to restore coronary blood flow in 50- 80% of patients80% of patients Contraindication active intracranial bleeding,Contraindication active intracranial bleeding, CVA 2months, CNS neoplasm, HTN,CVA 2months, CNS neoplasm, HTN, coagulopathycoagulopathy Retaplase slightly higher angiographic patencyRetaplase slightly higher angiographic patency but did not translate into survival benefitbut did not translate into survival benefit Intracranial bleed risk major drawbackIntracranial bleed risk major drawback
- 117. Glycoprotein IIb/IIIa AntagonistsGlycoprotein IIb/IIIa Antagonists Potent inhibitors of platelet aggregationPotent inhibitors of platelet aggregation Use during PCI and in patients with highUse during PCI and in patients with high risk features ACS have been shown torisk features ACS have been shown to reduce the composite end points of death,reduce the composite end points of death, reinfraction and the need for target lesionreinfraction and the need for target lesion
- 118. Percutanous Coronary InterventionPercutanous Coronary Intervention Alternative if performed by skilled operatorAlternative if performed by skilled operator in an experienced centerin an experienced center Standard is a “ door to balloon” time of 90Standard is a “ door to balloon” time of 90 minutesminutes PCI can successfully restore coronaryPCI can successfully restore coronary blood flow in 90 to 95% of MI patientsblood flow in 90 to 95% of MI patients PCI definitive survival advantage overPCI definitive survival advantage over fibrinolytics for MI patients who are infibrinolytics for MI patients who are in cardiogenic shockcardiogenic shock
- 119. Surgical RevascularizationSurgical Revascularization Emergent or surgical revascularization inEmergent or surgical revascularization in setting of failed PTCA in patients withsetting of failed PTCA in patients with hemodynamic instability and coronaryhemodynamic instability and coronary anatomy amendable to surgical graftinganatomy amendable to surgical grafting Also indicated of mechanicalAlso indicated of mechanical complications of MI including VSD, freecomplications of MI including VSD, free wall rupture, or acute MRwall rupture, or acute MR Carries a higher risk of perioperativeCarries a higher risk of perioperative mortality than elective CABGmortality than elective CABG
- 120. Lipid ManagementLipid Management All post MI patients should be on AMAAll post MI patients should be on AMA step II diet ( < 7% of calories fromstep II diet ( < 7% of calories from saturated fats)saturated fats) Post MI patients with LDL > 100 mg/dl arePost MI patients with LDL > 100 mg/dl are recommended to be on drug therapy to tryrecommended to be on drug therapy to try to lower levels to <100 mg/dlto lower levels to <100 mg/dl Recent data indicate that all MI patientsRecent data indicate that all MI patients should be on statin therapy, regardless ofshould be on statin therapy, regardless of lipid levels or dietlipid levels or diet
- 121. Long term MedicationsLong term Medications Most oral medications instituted in theMost oral medications instituted in the hospital at the time of MI are continuedhospital at the time of MI are continued long termlong term Aspirin, beta blockers and statin areAspirin, beta blockers and statin are continued indefinitelycontinued indefinitely ACEI indefinitely in patients with CHF,ACEI indefinitely in patients with CHF, ejection fraction <.40, hypertension, orejection fraction <.40, hypertension, or diabetesdiabetes
- 122. 1st1st 24 h24 h DuringDuring HospHosp Hosp DC +Hosp DC + Long TermLong Term Aspirin 162-325 mg chewed 75-162 mg/d p.o. 75-162 mg/d p.o. Fibrinolytic tPA,TNK, rPA, SK UFH 60U/kg (4000) 12 U/kg/h (1000) aPTT 1.5 - 2 x C aPTT 1.5 - 2 x C Beta-blocker Oral daily Oral daily Oral daily Summary of Pharmacologic Rx:Summary of Pharmacologic Rx: IschemiaIschemia JACC 2004;44: 671 Circulation 2004;110: 588
- 123. 1st1st 24 h24 h During HospDuring Hosp Hosp DC +Hosp DC + Long TermLong Term ACEI Anterior MI, Pulm Cong., EF < 40 Oral Daily Oral Daily IndefinitelyARB ACEI intol., HF, EF < 40 Aldo Blocker No renal dysf, K+ < 5.0 mEq/L On ACEI, HF or DM Same as during Hosp. Statin Start w/o lipid profile Indefinitely, LDL << 100 Summary of Pharmacologic Rx:Summary of Pharmacologic Rx: LVD, Sec. Prev.,LVD, Sec. Prev., JACC 2004;44:671JACC 2004;44:671 Circ 2004;110:588Circ 2004;110:588
- 124. Vascular Complications Recurrent ischemia Recurrent infarction Mechanical Complications Left ventricular free wall rupture Ventricular septal rupture Papillary muscle rupture with acute mitral regurgitation Myocardial Complications Diastolic dysfunction Systolic dysfunction Congestive heart failure Hypotension/cardiogenic shock Right ventricular infarction Ventricular cavity dilation Aneurysm formation (true, false)
- 125. Pericardial Complications Pericarditis Dressler’s syndrome Pericardial effusion Thromboembolic Complications Mural thrombosis Systemic thromboembolism Deep venous thrombosis Pulmonary embolism Electrical Complications Ventricular tachycardia Ventricular fibrillation Supraventricular tachydysrhythmias Bradydysrhythmias Atrioventricular block (first, second, or third degree)
- 126. Thank You!Thank You!
- 127. Summary: pump failure and shock. Diagnosis: chest X-ray, echocardiography, right heart catheterization. Treatment of mild and moderately severe heart failure: O2 furosemide: 20–40mg intravenously repeated at 1–4 hourly intervals if necessary nitrates: if no hypotension ACE inhibitors in the absence of hypotension, hypovolaemia or renal failure. Treatment of severe heart failure: O2 furosemide: cfr. supra nitrates if no hypotension inotropic agents: dopamine and/or dobutamine haemodynamic assessment with balloon floating catheter ventilatory support if inadequate oxygen tension consider early revascularization. Treatment of shock: O2 haemodynamic assessment with balloon floating catheter inotropic agents: dopamine and dobutamine ventilatory support if inadequate oxygen tension intraaortic balloon pump consider left ventricular assist devices and early revascularization.
Editor's Notes
- When faced with a patient with acute chest pain, we must distinguish myocardial infarction from all other causes of chest pain. If MI is suspected, current therapeutic practice includes: deciding whether to administer thrombolytics or PTCA and whether to admit patient to CCU. The former decision is based on ECG changes, including ST elevation or LBBB. Despite advances in investigative modalities, a focused history of the event ,physical examination and the 12-lead electrocardiogram (ECG) remain the key tools for the diagnosis of AMI. Cardiac serum markers help with risk stratification of unstable angina and diagnosis of AMI, but are not useful in the acute setting in the ED for thrombolytic inclusion
- Initial broad R in V1 and V2
