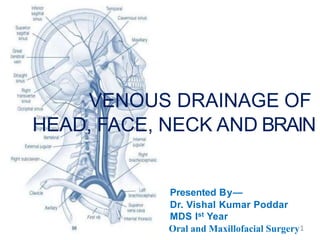
VENOUS DRAINAGE OF HEAD, FACE, NECK AND BRAIN
- 1. VENOUS DRAINAGE OF HEAD, FACE, NECK AND BRAIN Presented By— Dr. Vishal Kumar Poddar MDS Ist Year Oral and Maxillofacial Surgery1
- 2. Index 1.Introduction 2.Venous drainage of Head and Face 3.Venous drainage of Neck 4.Venous drainage of Brain 5.Surgical implications 6.References 2
- 3. Veins (vena) are blood vessels that carry blood towards the heart. Most veins carry deoxygenated blood from the tissues back to the heart. Exceptions are the pulmonary and umbilical veins. 3
- 4. Structure of Vein Veins are thin walled thanarteries. Largelumen. Valves, maintain unidirectional bloodflow. 3 concentric layers (tunicae) 1) Tunica intima - (endothilial cells & internal elastic lamina) 2) Tunica media –(contains muscle tissue, elastic fibers, collagen, external elastic lamina) 3) Tunica adventitia – (elastic and collagen tissue, muscle fibers) 4
- 6. Blood from veins • It is dark red in colour. • Blood flows steadily or gushes. • Bleeding easier to control. • Most veins collapse when cut. • However bleeding from deep veins can be massive and hard to control as arterial bleeding. 6
- 7. 7
- 8. Veins are classified as: • Superficial veins. course is close to the surface of the body, and have no• Are those whose corresponding arteries. • Deep veins. • Are deeper in the body and have corresponding arteries. • Communicating veins. • (Or perforator veins) are veins that directly connect superficial veins to deepveins. • Pulmonary veins. • Are a set of veins that deliver oxygenated blood from the lungs to the heart. • Systemic veins. • Drain the tissues of the body and deliver deoxygenated blood to the heart. 8
- 9. VENOUS SYSTEM ,HOW DOES IT WORK? 9
- 10. -Skin of nose, lips ,ears, nasal & alimentary mucosae, tongue, thyroid gland & sympathetic ganglia. 10
- 11. All the venous drainage from the head and neck terminate ???? 11
- 12. Veins of head, face, neck and brain Exterior of head Neck Brain and face *External Jugular *Diploic veins *Cerebral • Supratrochlear • Supraorbital vein *DuralVenous Sinuses*Internal Jugular *Subclavian *Brachiocephalic • Facial vein • Superficial temporal *Anterior Jugular • Maxillary vein • Pterygoid Venous plexus • Retromandibular • Posterior auricular • Occipital vein 12
- 13. • Venous drainage from the face is entirely superficial. • All the venous drainage from the head and neck terminate in the internal jugular vein which join the subclavian vein to form the brachiocephalic vein behind the medial end of the clavicle. • Two brachiocephalic veins unite to form superior vena cava. 13 VENOUS DRAINAGE OF HEAD AND FACE
- 14. 14
- 17. Supratrochlear and Supraorbital Vein • Drains the scalp. • Supratrochlear and supraorbital vein starts on the forehead from venous network which connects to the frontal tributaries of superficial temporal vein. • Runs downward superficial to the frontalis muscle, and joins at the medial angle of the orbit to form the Facial vein(angular vein). 17
- 18. The Facial Vein primary superficial • Coursing parallel to facial arteries • valveless veins that provide the drainage of the face. • Commences at the side on the root • Formed by the union of the of the nose. supraorbital and supratrochlear veins. 18
- 19. Relationship between the Facial Vein and Facial Artery • Facial vein lies posterior to the facial artery and its course is less tortuous than the artery. • Facial vein is usually located more posterior and superficial to the facial artery. • Of surgical significance, is the fact that the facial artery and vein are close to the mandible in the region of the inferior border. • The only structure that separates the vessels from the bone is the periosteum. 19
- 20. Tributaries Of Facial Vein • Superior ophthalmic vein • Veins of ala of nose • Deep facial vein, from pterygoid plexus • Inferior palpebral • Superior and inferior labial (drains area of upper and lower lip) • Buccinators (drains area of cheek) • Parotid and masseteric veins (drains area from parotid and masseter) • Below mandible it receives submental , tonsillar , external palatine and submandibular vein 20
- 21. Superficial TemporalVein • Drains the scalp. • Begins in a widespread network joined across scalp to contra-lateral vein and with supratrochlear, supraorbital, posterior auricular and occipital veins, all draining same network. • Cross posterior root of zygoma & enters parotid gland to unite with maxillary vein to form retromandibular vein.
- 22. Maxillary Vein
- 23. Maxillary vein the first part of• A short trunk accompanies maxillary artery. • It is confluence of vein from plexus, passes back pterygoid between sphenomandibular ligament and neck of mandible, to enter the parotid gland and here it unites with superficial temporal vein to form retromandibular vein.
- 25. Retromandibular Vein • Runs posterior to ramus of the mandible within the substance of parotid gland • Superficial to external carotid artery and deep to facial nerve • Dividesinto an Anterior branch going forwards to join with facial vein and Posterior branch which joins posterior auricular to form external jugular vein
- 26. Posterior Auricular Vein • Drains the scalp. • Begins upon the side of neck, in a plexus which communicates with tributaries of occipital vein and temporal veins. • Descends behind the auricle and joins the posterior division of retromandibular vein to form external jugular vein. • Receives mastoid emissary veins from sigmoid sinus. Infection here can be dangerous or fatal from retrograde thrombosis of cerebellar and medullary veins.
- 27. Occipital Vein • Begins in posterior network in scalp, pierce the cranial attachment of trapezius, turns into sub occipital triangle and becomes deep. • May follow occipital artery to end in internal jugular vein; or join posterior auricular & hence external jugular vein.
- 28. Lingual Vein Drains Tongue & Sublingual Region 3 branches: • Dorsal lingualvein • Deep lingual vein • Sublingual vein
- 30. a) PTERYGOID Location: Between Lateral and Medial Pterygoid Or between Temporal and Lateral Pterygoid
- 31. Tributaries: 1. Sphenopalatine v 2. Deep temporal v 3. Pterygoid v 4. Masseteric v 5. Buccal v 6. Dental v 7. Greater palatine v 8. Middle meningeal v 9. Inferior opthalmic v
- 32. b) SUBOCCIPITAL- 1. Located in suboccipital triangle 2. Receives blood from 1. Muscular veins 2. Transverse sinus 3. Occipital veins 4. Internal vertebral venous plexus 5. Condylar emmissary veins 3. Drains into vertebral veins
- 33. c) PHARYNGEAL VENOUS PLEXUS: 1. Located on posterolateral region of pharynx. 2. Receives blood from- Pharynx Soft palate Pre vertebral region 3. Drains into internal jugular and facial veins.
- 34. Veins of the neck The word "jugular" refers to the throat or neck. It derives from the Latin ‘jugulum’ meaning throat or collar bone. The jugular veins are relatively superficial and not protected by tissues such as bone or cartilage. This makes them susceptible to damage. Due to the large volumes of blood that flow though the jugular veins, damage to the jugulars can quickly cause significant blood loss, which can lead to hypovolemic shock and then death if not treated. To go for the jugular is to attack a vital part that is particularly vulnerable.
- 35. Veins of the Neck • External Jugular Vein • Anterior Jugular Vein • Internal Jugular Vein • Subclavian Vein • Brachiocephalic Vein
- 36. External Jugular Vein- • External jugular vein largely drains scalp and face, but also some deeper parts. • Formed by union of post division of retromandibular vein & post auricular vein. • Begins near the angle of mandible, just below the parotid gland and drains into subclavian vein. • Covered with platysma and superficial fascia and separated from sternocleidomastoid by deep cervical fascia.
- 38. TRIBUTARIES OF EXTERNAL JUGULAR VEIN • Posterior division of retromandibular vein • Posterior auricular vein • Posterior external jugular vein • Transverse cervical vein • Suprascapular vein • Anterior jugular vein • Occasionally joined by occipital
- 39. Anterior Jugular Vein • Starts near the hyoid bone by confluence of superficial submandibular veins. • Descends between midline and anterior border of Sternocleidomastoid turning laterally, low in neck, posterior to this muscle but superficial to depressor of hyoid bone. Joins external jugular vein or subclavian vein directly.• • There are usually two anterior jugular veins, just above the sternum, communicate by large transverse trunk, the venous jugular arch • Have no valves.
- 40. INTERIOR JUGULAR VEIN • Begins atthe base of the skull in the posterior compartment of jugular foramen collects blood from brain. • Immediately below the jugular foramen, it is widened to form superior bulb of internal jugular v,contained in jugular fossa. • Located post. to internal carotid artery • At its lower end, at the junction with subclavian vein , IJV is again widened to form inferiorbulb • Posterior to sternal end of clavicle, IJV combines with subclavian vein to form bracheocephalic vein. It is a direct continuation of the sigmoid sinus.
- 41. TRIBUTARIES OF INTERNAL JUGULAR VEIN Into Superior Bulb Inferior petrosal sinus Occipital vein Pharyngeal veins Common Facial vein Lingual vein Superior thyroid vein Middle thyroid vein
- 42. Relation With Its Surroundings
- 43. RELATIONS Surrounded By Accompanying Lymph Nodes Relation To Internal Carotid Artery C2: Posteriorly C3: Posterolaterally C4: Laterally Vagus Nerve (CN X) Always Situated Between The ICA And IJV Anteriorly (I.E. Is Crossed By These Structures) Upper Third: Spinal Root Of Accessory Nerve (CN XI) Middle Third: Lower Root Of Ansa Cervicalis Lower Third: Sternocleidomastoid Muscle, Tendon Of Omohyoid Muscle Posteriorly (From Superior To Inferior As The IJV Descends In The Neck) Lateral Mass Of C1 (Atlas) Middle Scalene Muscle Anterior Scalene Muscle Pleura Of Lung Apices
- 44. 36 • Each subclavian vein is a continuation of the axillary vein runs from the outer border of the first rib to the medial border of anterior scalene muscle. • From here it joins with the internal jugular vein to form the brachiocephalic vein (also known as “innominate vein”). The angle of union is termed the Venous Angle. • The thoracic duct drains into the left subclavian vein, near its junction with the left internal jugular vein. SUBCLAVIAN VEIN
- 45. Brachiocephalic vein • Formed behind Sternoclavicular joint
- 46. RIGHT BRACHIOCEPHALIC VEIN • 2.5 cm long • Runs vertically downwards • TRIBUTARIES are namely : 1. Vertebral vein 2. Internal thoracic vein 3. Inferior thyroid vein 4. First posterior intercostal vein
- 47. LEFT BRACHIOCEPHALIC VEIN • 6 cm long • Runs obliquely downwards and to the right behind the half of manubrium sterni • TRIBUTARIES are namely : 1. Vertebral vein 2. Internal thoracic vein 3. Inferior thyroid vein 4. First posterior intercostal 5. Left superior intercostal 6. Thymic and pericardial veins
- 48. SUPERIOR VENA CAVA FORMED by union of right and left Brachiocephalic veins. Formed at lower border of the right first costal cartilage. It pours blood into right atrium of the heart.
- 49. Venous drainage of Brain
- 50. DIPLOIC VEINS These veins occupy channels in diploe of some cranial bones and are devoid of valves. They are large with dilation at regular interval; their thin wall is merely endothelium. Absent at birth, begin to develop at about 2yrs. They communicate with meningeal veins, Dural sinuses & pericranial veins. Frontal diploic vein An anterior temporal diploic vein A posterior temporal diploic vein An occipital diploic vein
- 51. CEREBRAL VEINS They are divided into external & internal groups according to the outer surface or inner parts of hemispheres they drain into. External cerebral veins drain into superior saggital sinus Internal cerebral veins drain into great cerebral veins of Galen
- 52. Dural Venous Sinuses • They are blood-filled spaces situated between the layers of the duramater, • Lined by endothelium, • Walls are thick and composed of fibrous tissue. • They have no muscular tissue. • They have no valves.
- 54. • They receive blood from: 1.The Brain 2.The Meninges 3.Bones of the skull • CSF is also poured in some of them.
- 55. Types of Dural sinuses • There are 23venous sinuses, of which – •8 are PAIRED •7 are UNPAIRED
- 56. Paired 1.Cavernous sinus 2.Superior petrosal sinus 3.Inferior petrosal sinus 4. Transverse sinus 5.Sigmoid sinus 6.Sphenopalatine sinus 7.Petrosquamous sinus 8.Middle Meningeal sinus
- 57. Unpaired 1.Superior sagittal sinus 2.Inferior sagittal sinus 3.Straight sinus 4.Occipital sinus 5.Anterior intercavernous sinus 6.Posterior intercavernous sinus 7.Basilar plexus of veins
- 58. SUPERIOR AND INFERIOR PETROSAL SINUS They are small and situated on the superior and inferior borders of the petrous part of the temporal bone on each side. Each superior sinus drains the cavernous sinus into the transverse sinus. Each inferior sinus drains the cavernous sinus into the internal jugular vein.
- 59. TRANSVERSESINUS They are paired and begin at the internal occipital protuberance. The right sinus is direct continuation of the superior sagittal sinus. The left is continuation of the straight sinus. They drain from the confluence of sinuses to the sigmoid sinuses, which ultimately connect to the Internal jugular vein.
- 60. SIGMOID SINUS They are a direct continuation of the transverse sinuses. Each sinus turns downward and medially and grooves the mastoid part of the temporal bone. Here it lies behind the mastoid antrum. It then turns downward through the posterior part of the jugular foramen to become continuous with the superior bulb of the internal jugular vein.
- 61. SUPERIOR SAGITTAL SINUS It occupies the upper fixed border of the falx cerebri. It begins in the front at the foramen cecum where it receives a vein from the nasal cavity. It runs backward, grooving the vault of the skull and at the internal occipital protuberance it deviates to one side and becomes continuous with the transverse sinus.
- 62. It communicates through small openings with 2 or 3 venous lacunae on each side. Numerous arachnoid villi and granulations project into these lacunae which also receive the diploic; emissary and meningeal veins. It receives the superior cerebral veins . At the internal occipital protuberance it is dilated to form the confluence of the sinuses which is connected to the opposite transverse sinus and receives the occipital sinus.
- 63. INFERIOR SAGITTAL SINUS It occupies the free lower margin of the falx cerebri. It runs backward and joins the great cerebral vein which is formed by the union of the two internal cerebral veins at the free margin of the tentorium cerebelli to form the straight sinus. It receives cerebral veins from the medial surface of the cerebral hemisphere.
- 64. STRAIGHT SINUS It occupies the line of junction of the falx cerebri with the tentorium cerebelli. It is formed by the union of the inferior sagittal sinus with the great cerebral vein. It ends by turning to the left ( sometimes to the right ) to form the transverse sinus.
- 65. OCCIPITAL SINUS It is a small sinus occupying the attached margin of the falx cerebelli. It communicates with the vertebral veins near the foramen magnum. Superiorly it drains into the confluence of sinuses.
- 66. CAVERNOUS SINUS Situated in the middle cranial fossa on each side of the body of the sphenoid bone. Each sinus extends from the superior orbital fissure in front to the apex of the petrous part of the temporal bone behind. The 3rd & 4th cranial nerves and the ophthalmic & maxillary divisions of the trigeminal nerve run forward in the lateral wall of this sinus. The internal carotid artery, its sympathetic nerve plexus and abducent nerve run forward through it.
- 67. TRIBUTARIES It receives blood from the ORBIT, BRAIN and the MENINGES.
- 68. COMMUNICATIONS Transverse sinus through superior petrosal sinus Internal jugular vein trough inferior petrosalsinus Pterygoid plexus through emissary veins Facial vein through superior opthalmicvein Cavernous sinus of opposite side through anterior and posterior intercavernous sinus.
- 69. EMISSARY VEINS • Cranial venous sinuses communicate with veins outside the skull through EMISSARY VEINS • These comminication s help to keep the pressure of blood in the sinuses constant
- 71. Supratrochlear and Supraorbital Vein Surgical Importance- Design of paramedian flap in nasal reconstruction.
- 72. Facial vein • Applied Importance: • Facial veins have no valves and it connects to cavernous sinus by 2 routes. • 1.) via ophthalmic vein or supraorbital vein. • 2)Via deep facial vein to pterygoid plexus and hence to cavernous sinus. • Thus infective thrombosis of facial vein may extend to intracranial venous sinuses. 73
- 73. • Anatomical variations of the facial veins and arteries are of great importance for facial transplantations because they are the main vascular pedicles that will be connected to the patient. A good arterial inflow and venous outflow are essential for the free flap survival.
- 74. RETROMANDIBULAR VEIN(RMV) 74 • Formation of the RMV by union of the superficial temporal vein and maxillary vein mostly occurs at a level higher than the passage of the main trunk and branches of the FN, where they laterally pass to the vein. • In open surgical reduction of mandibular condyle fractures, the FN and its branches can be localized by using the superficial temporal veins and the RMVs as a guide, even in abnormal course of the nerve.
- 75. Lateral view of right facial nerve (FN) giving superior division (SD) and inferior division (ID); each of them pass through a separate ring in the retro-mandibular vein (RMV). 75
- 76. 67 Ronald A. Bergman, PhD Adel K. Afifi, MD, MS Ryosuke Miyauchi, MD
- 77. 77 In 13%, major divisions (temporal and facial) are independent; in 11%, anastomoses occur between rami of the temporal division; in 22%, connections occur between adjacent rami from the major divisions; in 21%, anastomoses representing a composite of those in the11% and 22% categories occur; in 12%, proximal anastomoses occur within the temporal component, as well as distal interconnection between the latter and the cervical component; in 9%, two anastomotic rami connect the buccal divisin of the cervical to the zygomatic part of the temporal; in 5%, a transverse ramus, from the trunk of the nerve, contributes to the buccal ramus formed by anastomosis between the two major divisions; in 7% richly plexiform communications occur, especially within the temporal portion of the nerve.
- 78. Communications of the Pterygoid plexus 1. With Inferior opthalmic vein through the inferior orbital fissure 2. With Cavernous sinus through emissary veins 3. With facial vein through the deep facial vein
- 79. Applied anatomy: PSA block -haematoma -black eye Serves as media for spread of external infection to the cavernous sinus
- 80. A black eye is bruising around the eye commonly due to an injury to the face rather than to the eye. The name is given due to the color of bruising. Although most black eye injuries are not serious, bleeding within the eye, called a hyphema, is serious and can reduce vision and damage the cornea. Hyphema can cause rapid increase eye pressure and vision loss from glaucoma if left untreated. BLACK EYE
- 81. Abnormaly dilated, tortuous veins produced by prolonged, increase intraluminal pressure. Small purplish or blue-black round swellings under the tongue with age and are known as “caviar lesions” No treatment is indicated for lingual varices.. Lingualvaricosity 80
- 82. EXTERNAL JUGULAR VEIN(EJV) • EJV is examined to assess the venous pressure; the right atrial pressure is reflected in it because of absence of valves. • Vein is visible through skin and can be made more prominent by blowing with mouth and nostrils closed. • Normal JVP is 5 to 8 cm. • Vene puncture performed on this vein • Surgical division of sternocleidomastoid muscle requires special care of the vein • Increased venous pressure indicates congestive cardiac failure
- 83. Visualization (LEWIS METHOD) The veins of the neck, viewed from in front. The patient is positioned under 45°, and the filling level of the jugular vein determined. Visualize the internal jugular vein when looking for the pulsation. In healthy people, the filling level of the jugular vein should be less than 3 centimetres vertical height above the sternal angle. JUGULAR VENOUS PULSE 82
- 84. Jugular venous pulse (JVP) • Determine activity of atrium • Seen better then felt • Preferable over EJV • Elevation of JVP indicative of cardiac failure 84
- 85. A man with severe congestive cardiac failure with marked jugular venous distension. External jugular vein marked by arrow. 84
- 86. INTERNAL JUGULAR VEIN(IJV) Infection from middle ear spreads to IJV Surgical removal of deep cervical nodes can puncture IJV Easy accessibility between two heads of sternocleidomastoid muscle for introduction of cannula 86
- 87. Thrombophlebitis can occur by spread of infection in caverous sinus Systolic thrill felt over the vein in mitral stenosis During CCF dilatation of vein occur In congestive cardiac failure, venous pressure is markedly increased, the IJV is dilated and engorged with blood. 87
- 88. • The deep cervical lymph node lie on IJV. These nodes become adherant to veins in malignancy or in T.B. Therefore during such operations the vein is also resected. 88
- 89. Applied anatomy: 1. Special care required to preserve the vein during surgical treatment of WRY NECK ANTERIOR JUGULAR VEIN(AJV) 89
- 90. Jugular phlebectasia in children • Jugular phlebectasia is a congenital dilatation of jugular vein which appears as a soft, compressible mass in the neck only during straining or crying. It should be differentiated from laryngocele, cysts and tumors of neck which may also appear during straining. • Ultrasonography (US) and computerized tomography (CT) are diagnostic methods to distinguish the pathology • More common in internal jugular vein. 89
- 91. DURAL SINUS THROMBOSIS Common causes of dural venous sinus include fractures head and neck infections, head or intracranial hematomas either thrombosis injury,skull by direct compression of the sinus or endothelial damage within the sinus can cause the activation of coagulation system resulting in sinus occlusion. 90
- 92. 91 Brain cells contain an abundance of thromboplastin that is released after injury inducing an hypercoagulable state leading to destruction of platelets & erythrocytes followed by thrombus formation. Most common thrombosed sinuses are tranSverse,cavernous & superior saggital sinus Clinical symptoms headache, papilloedema, impairedconsciousness, vomitting.
- 93. Metastasisof tumour cells to dural sinuses Tha basilar and occipital sinuses communicate through the foramen magnum with the internal venous plexuses. Because these venous channels are valveless, compression of the thorax, abdomen, or pelvis as occurs during heavy coughing and straining may force venous blood from these regions into vertebral venous system and from it into dural venous sinuses. As a a result, pus in the abscesses and tumour cells in these regions may spread to vertebrae and brain. 92
- 95. Thrombosis caused by sepsis in the danger area of face, nasal cavity, paranasal sinuses give rise to : Nervous symptoms: 1)severe pain in the eye and forehead in the area of distribution of opthalmic nerve. 2)Involvement of 3rd, 4th and 6th nerve resulting in paralysis of muscle supplied. 94
- 96. Venous symptoms: 1) Marked edema of eyelid, cornea & exopthalmos due to congestion of orbital vein. Carotid and cavernous communication: because of peculiar relationship of cavernous sinus to internal carotid artery a communication may occur between the two as a result of injury. When this happens the arterial pressure is communicated through the sinus to vein of orbit & as a result the eye become prominent & pulsate with each heart beat( pulsating exopthalmos) 95
- 97. Emissary veins are connection between the extracranial scalp veins and the diploic and intracranial venous systems. These veins are valveless and therefore can transmit infection from the extracranial to the intracranial compartment. The meningeal veins are epidural veins that lie within the dura draining the falx cerebri, the tentorium, and the cranial dura. They run in shallow grooves on the inner table of the skull to communicate with the dural sinuses or traverse extracranially to the pterygoid plexus in the deep face or vertebral plexus around the cervical spine. The diploic veins are small irregular endothelial-lined channels coursing between the inner and outer tables of the skull. These communicate with the extracranial venous system, the meningeal veins, and the dural sinuses. They are rarely seen using angiography unless enlarged, as in the case of an arterial-venous malformation. Communication between extracranial and intracranial veins 96
- 98. 97 Danger triangle of the face consists of the area from the corners of the mouth to the bridge of the nose, including the nose and maxilla. The presence of loose areolar tissue containing the emissary veins allows the spread of retrograde infections from the nasal area to spread to the brain causing cavernous sinus thrombosis, meningitis brain abscess.
- 99. • Sinus pericranii (SP) is a rare disorder characterized by a congenital (or occasionally, acquired) epicranial venous malformation of the scalp. • Sinus pericranii is an abnormal communication between the intracranial and extracranial venous drainage pathways. • Treatment of this condition has mainly been recommended for aesthetic reasons and prevention of hemorrhage. Sinuspericranii 98
- 100. VASCULAR MALFORMATIONS Described as abnormalities of blood and lymphatic vessels, many hemangiomas, vascular malformations, like present at birth but do not undergo proliferation and do not spontaneously involute. • Do not regress with age and may severe be associated with or life threatening haemorrhage. • A large venous malformation appears as bluish, soft, compressible lesion,no bruit or pulsation is present. 99
- 102. • TREATMENT: May be treated with sclerotherapy as well as direct injections of sodium morrhuate, boiling water, alcohol & ethibloc. • Combined application of sodium tetradecyl sulfate sclerothearpy & conservative ablative surgery when larger lesions are involved. 100
- 103. VENOUS MALFORMATIONS Low flow lesion Composed of ectatic venous channels that will continue to grow throughout the patient’s lifetime. The overall incidence of venous malformation is about 1 in 10 000. These lesions commonly occur in the head and neck area with a predilection for the oral cavity, airway, and muscle groups. Several syndromes can be associated with venous malformations Including Blue Rubber Bleb Nevus Syndrome, Glomuvenous Malformation (Associated With Glomulin Mutation), Sturge-weber Syndrome, Klippel– Trenaunay Syndrome etc.
- 104. The lesions vary in colour depending on depth of involvement, from undetectable colour differences to deep purple. The lesions fill with dependency and are compressible, which helps to distinguish them from lymphatic malformations on physical examination. Patients may present with complaints of pain and swelling and this is usually related to clot formation either from trauma or venous stasis. Venous malformations have a propensity to occur in muscle groups but can also involve skin and mucosa. Areas frequently involved in the head and neck are masseter, temporalis, tongue musculature, as well as oral and airway mucosa. MRI remains the diagnostic modality of choice to assess extent and plan treatment for these lesions.
- 105. Telangiectasias or angioectasias are small dilated blood vessels near the surface of the skin or mucous membranes, measuring between 0.5 and 1 millimeter in diameter. They can develop anywhere on the body but are commonly seen on the face around the nose, cheeks, and chin. Some telangiectasia are due to developmental abnormalities that can closely mimic the behaviour of benign vascular neoplasms. They may be composed of abnormal aggregations of arterioles, capillaries, or venules. Telangiectasia 101
- 106. • Telangiectasias on the face are often treated with a laser. • Laser therapy uses a light beam that is pulsed onto the veins in order to seal them off, causing them to dissolve. • These light-based treatments require adequate heating of the veins. • These treatments can result in the destruction of sweat glands, and the risk increases with the number of treatments. 102
- 107. Venipuncture or Phlebotomy Venipuncture is the process of obtaining intravenous access for the purpose of intravenous therapy or for blood sampling of venous blood.
- 108. • Indication: Tointroduce or replace fluids in circulation • Complications: 1.Overloading 2.Thrombophlebitis 3.Haematoma 4.Infection 5.Air embolism 108
- 109. Venesection ( venous cut down) • As an alternative to venipuncture in critically ill patients in need of vascular access, and in whom venipuncture may be difficult • An emergency procedure in which the vein is exposed surgically and then a cannula is inserted into the vein under direct vision. • It is used to get vascular access in trauma and hypovolemic shock patients when peripheral cannulation is difficult or impossible. • Sites for venesection great saphenous vein (most common, usually at the ankle) ,basilic vein, cephalic vein.
- 110. • The skin is cleaned, draped, and anesthetized. • The greater saphenous vein is identified on the surface above the medial malleolus, a full-thickness transverse skin incision is made, and 2 cm of the vein is freed from the surrounding structures. • The vessel is tied closed distally, the proximal portion is transected (venotomy) and gently dilated, and a cannula is introduced through the venotomy and secured in place with a more proximal ligature around the vein and cannula. • An intravenous line is connected to the cannula to complete the procedure.
- 111. Free flap transplantation is an important method for the surgical resurfacing of soft tissue defects in all parts of the body. The arterialized venous flap technique depends on the use of two veins in the skin flap that are used respectively for arterial flow and venous drainage. Survival depends on the size of the flap, arterial inflow, and venous outflow. For good results, an arterialized venous flap should be designed to contain most of the venous network in the centre, the arterial inflow should be anastomosed to one afferent vein, and two or more efferent veins should drain the arterialized venous flap. ARTERIALIZED VENOUS FLAP Ozek et al. studied the changes occurring in the venous system after its arterialization and showed that the thickening and hypertrophy of the vessel walls indicated adaptive changes to withstand the increased stress experienced in their new roles as arterial conduits.
- 112. Central venous line placement A central venous catheter is a special IV line that is inserted into a large vein in the body. Several veins are used for central venous catheters including those located in the shoulder (subclavian vein), neck (jugular vein), and groin (femoral vein). It is used to administer medication or fluids, obtain blood tests (specifically the "mixed venous oxygen saturation"), and directly obtain cardiovascular measurements such as the central venous pressure.
- 113. INDICATIONS AND USES Monitoring of the central venous pressure (CVP) in acutely ill patients to quantify fluid balance Long-term Intravenous antibiotics Long-term Parenteral nutrition especially in chronically ill patients Long-term pain medications Chemotherapy Seldinger Technique 1.desired vessel or cavity is punctured using a trocar (hollow needle). 2.soft curved tip guide wire is then inserted through the trocar and advanced into the lumen. 3.guidewire is held secured in place whilst the introducer trocar is removed. 4.large-bore sheath/cannula/catheter is passed over the guidewire into the lumen/cavity. 5.guidewire is withdrawn leaving the introducer sheath in situ through which catheters and other medical devices can be introduced.
- 114. Air Embolism • External jugular vein pierces the investing layer of deep cervical fascia • The margins of the vein get adherent to the fascia • So, if the vein gets cut, it can not close and air enters into it causing air embolism 114
- 115. 113115
- 116. Vein grafting 116
- 117. Bibliography • B.D. Chaurasia’s Human Anatomy Volume 3 • Gray’s Textbook of Anatomy • Hine, Levy, Shafer’s Textbook of Oral Pathology • Hutchinson’s Textbook of Medicine • Peterson’s Textbook of Oral Surgery • Internet Sources 117
- 118. 118
Editor's Notes
- Chronic Cerebrospinal Venous Insufficiency (CCSVI) is a term used to describe a potential reduction in blood flow in the major veins that drain blood from the brain and spinal cord over a prolonged period. The condition was first described as being a possible contributor to MS by Italian physician, Dr Zamboni in 2009. The proposed treatment for CCSVI, sometimes referred to as “liberation therapy,” is an angioplasty procedure, which involves opening blocked or narrowed veins by inflating a small balloon or inserting a stent to allow for better blood flow and improve drainage of blood from the brain. In May 2012, the U.S. FDA issued a safety communication about procedures to treat CCSVI in people with MS.