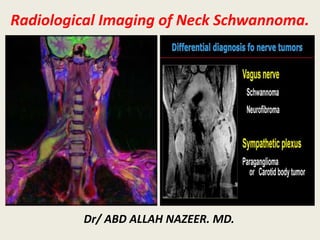
Radiological Imaging of Neck Schwannoma
- 1. Radiological Imaging of Neck Schwannoma. Dr/ ABD ALLAH NAZEER. MD.
- 2. Schwannomas are benign neoplasms of the peripheral nerves originating in the Schwann cells. They are rare and usually solitary, with clearly delimited capsules. They occur in the head and neck region in only 25 % of the cases, and may be associated with Von Recklinghausen’s disease. Schwannomas are always a diagnostic dilemma as they are asymptomatic for long time and histopathology is the gold standard for diagnosis. The nerves affected included the brachial plexus, vagus nerve, sympathetic chain and lingual nerve. The nerve of origin was identified based on intra-operative findings and post-operative neurological deficits. Schwannomas are generally benign, and rarely recur.
- 3. Schwannoma is a benign, slow growing encapsulated perineural tumour of neuro ectodermal derivation, originating from Schwann cells of the neural sheath of motor and sensitive peripheral nerves. As a slowly growing benign tumour, it has been reported that 25–45 % of schwannomas were located in the extracranial head and neck region. It involves the cranial nerves such as V, VII, X, XI, and XII or sympathetic and peripheral nerves. Extracranial head and neck schwannoma is a challenging condition to the head and neck surgeons. For tumours arising from the major cranial nerves, excision of tumour with the division of the nerve of origin (NOO) renders lifelong morbidity to the patients. On the other hand, other nerve-preserving excision method, e.g. intracapsular enucleation, does not guarantee intact nerve function after surgery. Because of the substantial chance of nerve palsy after operation, obtaining an accurate preoperative diagnosis, and preferably, with the identification of the NOO is crucial in the management of the disease.
- 4. Neurilemmoma also known as schwannoma is a benign tumor of nerve sheath origin, arising from any nerve covered with a schwann cell sheath, which includes the cranial nerves (except for optic and olfactory), the spinal nerves, and autonomic nervous system. Schwannomas occurring in the head and neck region are frequent, with 25–45% of all reported schwannomas being found in this region. These tumors are generally encapsulated except from the sinonasal tract and nasopharynx. Most often these tumors are solitary but can occur in multiple areas also. Multiple occurrences are usually associated not only with neurofibromatosis II but also schwannomatosis. Head and neck are the most commonly affected regions (25–45%) with the lateral neck being the frequently involved site. Cytogenetic abnormality of chromosome 22 is seen in 50% cases, and those are associated with neurofibromatosis II. Sinonasal schwannoma contributes about 4% of head and neck schwannomas. It remains asymptomatic for a quite long period because of slow growth. Nasal obstruction is the main symptom of this tumor. Pain, bony dehiscence including skull base and neural symptoms develop later as the tumor enlarges. It can also simulate rhinosinusitis as clinical features are similar. Brachial plexus tumors are rare comprising of only 5% of all tumors of upper limb. The most frequent site is in the head and neck, which comprises 25% of all schwannomas and only about 5% of schwannomas present as brachial plexus tumors. The two most common brachial plexus region tumors are the schwannomas and neurofibromas, both of which are benign and arise from the nerve sheath.
- 5. Most often, early in the course, minimal neurological deficit will be present, or there will be none at all. Manipulation of the mass can produce paraesthesias or “shocks” in the distribution of the affected nerve, and this can be an important aid to diagnosis. Side-to- side mobility greater than longitudinal mobility of the mass from the nerve is more common in cases of benign lesions, whereas malignancy is associated with firmness and immobility. In cases of brachial plexus lesions, MR imaging is the study of choice to delineate the margins of the tumor from surrounding tissues with greatest contrast. Importantly, however, MR imaging is currently unable to differentiate between schwannoma and neurofibroma. Computerized tomography scanning is optimal at revealing osseous erosion around the spine or changes in neural foramina. A newer modality, MR neurography (MR-magnetic resonance), has the potential to demonstrate the entire course of visualized peripheral nerves. Schwannomas of the vagus nerve grow between the common carotid artery and the internal jugular vein. This growth pattern often leads to a divergence of both structures, which is visible in CT scan or MRI. Cervical vagal schwannomas constitute about 2–5% of neurogenic tumors. These tumors usually present as asymptomatic masses as in our case, if symptomatic patients will present with hoarseness as the main symptom. The sign usually seen in these cases is unilateral vocal cord paralysis. The reported incidence of preoperative vocal cord paralysis is about 12%. Clinical sign elicited in case of vagal schwannoma is a paradoxical cough on palpating the mass due to vagal stimulation. The presence of this sign together with palpation of mass medial to the sternocleidomastoid should arouse the suspicion of a neurogenic tumor
- 6. A 32-year-old female with left facial nerve schwannoma. Sagittal T2 weighted image (A) showing hyperintense bilobed mass in the left parotid region (thin arrow) and the left mastoid region (dashed arrow). Interconnecting stalk seen along the vertical (mastoid) segment of facial nerve (squiggly arrow). Diffusion- weighted image at b = 0 (B), b = 1000 (C) s/mm2, and ADC map (D) show restricted diffusion in the lesion (thick arrows).
- 8. Intraparotid schwannoma. (A) Axial T2-weighted MR image shows a hyperintense well- defined mass (arrow) in the left parotid gland. (B) Axial fs gadolinium-enhanced T1- weighted MR image of the same tumour (arrow) shows intense peripheral enhancement.
- 9. Intraparotid Facial Nerve Schwannoma: A, Axial T1-weighted image (spin-echo: TR/TE, 650/10.7) shows a low-signal- intensity well-defined mass in the right parotid gland. B, Axial T2-weighted image (fast spin-echo: TR/TE, 3150/108) shows peripheral high signal intensity surrounding a central region of lower signal intensity.
- 10. Intraparotid fascial nerve Schwannoma. A, Axial T1-weighted image (spin-echo: TR/TE, 650/9.3) shows a lobulated mass in the right parotid gland, with a low-signal- intensity well-defined mass in the right parotid gland. B, Axial T2-weighted image (fast spin-echo: TR/TE, 3150/108) shows a heterogeneous hyperintense mass. C, Axial gadolinium-enhanced T1-weighted image (spin echo; TR/TE, 650/9.3) shows a mass in the right parotid gland with heterogeneous enhancement. D, Coronal STIR image (TR/TE/TI, 3216/36/165) shows a hyperintense mass in the right parotid gland. The tumor is situated directly caudal to the stylomastoid foramen and protrudes into it (arrow).
- 11. Schwannoma of the parapharyngeal space. A rounded, regular, well defined, encapsulated soft tissue mass is seen at the left parapharyngeal space. it compresses the pharyngeal air column and displaces the carotid vessels/jugular vein laterally. It exhibits low T1, bright T2/STIR signal with patchy moderate enhancement after contrast administration.
- 15. The schwannoma shows intense heterogeneous enhancement on the postgadolinium fat- saturated T1WI (A) and appears heterogeneously bright on the fat-saturated T2WI (B). The nonenhancing areas in the center of the mass correspond to the areas of fluid signal intensity seen in the T2WI. The entire carotid sheath (arrows) is displaced in an anterolateral direction.
- 16. Coronal MRI T1-weighted image reveals mass in left parapharyngeal space Schwannoma.
- 17. A 35-year-old female with left parapharyngeal space schwannoma. Axial T2 weighted fat-saturated image (A) showing well-defined heterogeneously hyperintense mass in the left parapharyngeal space. Central area of the lesion (double ended arrow) is more hyperintense than the peripheral (dashed arrow). Diffusion-weighted image at b = 1000 (B) s/mm2 and ADC map (C) show restriction at the peripheral rim of the tissue (thin arrows) with free diffusion in the centre (thick arrows).
- 18. A 37-year-old man with right parapharyngeal space schwannoma. Coronal T2 weighted image (A) shows fusiform shaped mass in the right parapharyngeal space with heterogeneous hyperintense signal intensity. No central necrosis seen. Diffusion weighted images at b = 0 (B), b = 1000 (C) s/mm2, and ADC map (D) show free diffusion throughout the mass (thick arrows).
- 19. Sympathetic chain schwannomas in a 33-year-old woman (case number 4). (a) Axial T2-weighted image at the C3 level shows the ICA and IJV both displaced anterolaterally by the SC schwannoma, with no separation between them. On coronal(b) and sagittal (c) MIP of the DW-MRN, both of the SC and the VN seem to connect to the tumor. (d) an intraoperative photograph revealed the VN coursing downward between the CA and the IJV.
- 20. Sympathetic chain schwannoma. Axial T1- weighted MR image shows a mass slightly hypointense to muscle in the left post-styloid parapharyngeal space causing anterior lateral displacement of carotid sheath structures. This mass increases in signal intensity on the T2 sequence and enhances heterogeneously after contrast administration. The normal anatomic relationship of the sympathetic chain (arrow) and the carotid sheath are shown in the illustration.
- 21. Schwannoma of cervical sympathetic chain at the left para- pharyngeal space.
- 22. Contrast enhanced computed tomography scan shows isodense mass in right carotid space with non homogenous enhancement. Pre-operative photograph of the patient with arrow pointing at cervical sympathetic chain schwannoma.
- 23. Pre-operative photography, CECT and MRI T1WI of neck showing the parapharyngeal mass occupying the poststyloid compartment in the vagal schwannoma patient.
- 24. Neck CT image of a vagal schwannoma patient. Tumor (asterisk) is separating the common carotid artery (white arrow) anteriorly and internal jugular vein (arrow head) posteriorly.
- 25. Schwannoma of left cervical vagus nerve. Contrast-enhanced CT scan shows left-sided, well- circumscribed, heterogeneously hypodense mass with few areas of patchy enhancement. Anterior displacement of internal carotid artery (ICA), external carotid artery (ECA), and parapharyngeal fat and medial displacement of visceral space (white arrow) are shown here. The internal jugular vein is compressed by tumor and hence is not visualized in this image.
- 26. Schwannoma of left cervical vagus nerve.
- 27. CT and MRI for schwannoma of right cervical vagus nerve.
- 28. Neck CT image of a sympathetic schwannoma patient. Tumor (asterisk) is anteriorly displacing the common carotid artery (white arrow) and internal jugular vein (arrow head) together without separating them.
- 30. Schwannoma of the carotid sheath: axial T2-weighted image and angiogram.
- 31. Schwannoma of the carotid sheath, (a) MRI angiography showing splaying of the carotids by the tumor. (b) T2-weighted coronal cut. (c) T2-weighted axial cut. (d) Postcontrast T1 sagittal cut.
- 33. left trigeminal nerve schwannoma. Axial T1 weighted image (A) showing well-defined left parapharyngeal space mass, isointense to muscle, with few internal hypointense areas (white arrow). Axial T2 weighted image (B) showing heterogeneous mass with markedly hyperintense centre and relatively isointense periphery. Blood fluid level noted in central hyperintense area (double ended arrow). Coronal T2 weighted image (C) showing intracranial extension via left foramen ovale (dashed arrows). Diffusion-weighted images at b = 0 (D), b = 1000 (E) s/mm2, and ADC map (F) reveal marked restriction at the peripheral rim of the tissue (thin arrows) with free diffusion in the centre (thick arrows)
- 34. Sagittal view of the tumor on MRI. The arrow indicates a 7x4 cm mass lesion originating from the vagus nerve.
- 35. A parapharyngeal space schwannoma arising from the vagus nerve.
- 37. (A and B): Paraspinal schwannoma: Axial T1 and T2W images show an oblongated lesion (arrows), which is isointense on T1 and heterogeneously hyperintense on T2 in the cervical spine, causing widening of the neural canal (dotted arrows) and extending into the soft tissues of the neck
- 39. Schwannoma, well defined oval shaped enhancing mass is noted at right upper cervical region. Small focus of calcification is present within the mass. The mass is located between the sternoclidomastoid muscle and main cervical vessels at the right side. Internal jugular vein and common carotid artery and its main branches are displaced medially by the mass and there are no frank evidence of local invasion. Several prominent lymph nodes are identified at right anterior cervical spaces.
- 41. Schwannoma.
- 43. Sinonasal schwannoma is generally a well-defined soft-tissue mass most frequently occurring in the nasal cavity and ethmoid sinus and frequently associated with pressure remodeling of the adjacent bone. These tumors are isoattenuating on CT and predominantly isointense on both T1- and T2-weighted MR images, compared with the brain stem. Mild contrast enhancement on CT and strong enhancement on MR images were also demonstrated in most of the tumors. Although sinonasal schwannomas are rare and their imaging findings are rather nonspecific, CT and MR imaging studies are helpful for preoperative diagnosis and surgical planning in patients with schwannoma of the sinonasal cavity.
- 44. Schwannoma of the nasal cavity in a 79-year-old man. A, Pre-contrast axial CT scan with a bone algorithm shows a polypoid mass in the left anterior nasal cavity, originating from the nasal septum. B, Contrast-enhanced axial CT scan with a soft-tissue algorithm shows mild and patchy enhancement of the mass. C, Fat-suppressed axial T2- weighted MR image shows that the mass is isointense to the brain stem. D, Contrast-enhanced fat-suppressed sagittal T1-weighted MR image shows marked contrast enhancement within the mass.
- 45. Schwannoma of the nasal cavity in a 22-year-old man. A, Contrast-enhanced coronal CT image shows a tubular expansile soft-tissue mass in the left nasal cavity, demonstrating mild enhancement. B, Axial T1-weighted MR image shows the tumor extending in the anteroposterior dimension and remodeling the lateral nasal wall. C, Fat-suppressed axial T2-weighted MR image shows that the tumor is hyperintense to the brain stem. D, Contrast-enhanced fat-suppressed axial T1-weighted MR images show marked homogeneous enhancement within the tumor.
- 46. Schwannoma of the nasal cavity and ethmoid sinus in a 42-year-old woman. A, Precontrast axial CT scan shows a large lobulated expansile mass isoattenuating to the brain stem and centered in the right posterior ethmoid sinus. B, Postcontrast axial CT scan shows marked enhancement of the mass, greater than that of the muscles in the masticator space. The mass extends to the ipsilateral orbit and maxillary and sphenoid sinuses with scalloping and remodeling of the bony walls of the nasal septum, maxilla, and sphenoid bone. C, Coronal T2-weighted MR image shows heterogeneous signal intensity of the mass and signal voids within the lesion, suggestive of prominent vascularity. D, Contrast-enhanced fat-suppressed coronal T1- weighted MR image shows marked and heterogeneous enhancement of the mass.
- 47. Schwannoma of the maxillary sinus in a 24-year-old woman. A and B, Precontrast axial and coronal CT scan with a bone algorithm shows a lobulated expansile mass arising from the left infraorbital canal, which replaces the left maxillary sinus. Note cortical thinning and remodeling of the orbital floor and the medial and posterior maxillary sinus walls by the mass. C, Fat-suppressed axial T2-weighted MR image shows multiple fluid-fluid levels within the lesion, which are suggestive of intratumoral hemorrhage. D, Contrast-enhanced fat-suppressed coronal T1-weighted MR image shows cystic change at the lower part of the mass and marked enhancement in the upper solid part of the mass.
- 48. Schwannoma, (a) Preoperative CT showing the tumor () present in the posterior part of the left maxillary sinus and the left nostril. (b) Postoperative CT.
- 49. Conclusion: Schwannomas are derived from Schwann cells. They are usually solitary lesions, except in Von Recklinghausen’s disease. Pain and neurological symptoms are uncommon, and become evident only at advanced stages. They are generally benign, and rarely recur. An accurate preoperative workup with the identification of NOO is very important not only for a correct diagnosis, but also for surgical planning and informing the patient about the possible complications. This allows the patient to make an informed decision on whether to undergo operation or observation.
- 50. Thank You.
