Population Health - HEDIS - Health Plan
•
2 likes•601 views
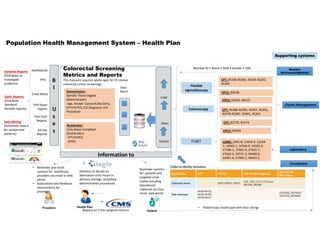
This document describes a population health management system for a health plan. It includes supporting systems like claims management, laboratories, and member services. The system focuses on colorectal cancer screening metrics and uses data from various sources to calculate screening rates. It extracts, cleans, and loads this data into data marts and warehouses. Dashboards, reports, alerts and ad hoc queries are then used to monitor screening rates and identify opportunities for outreach and provider interventions to improve preventive care services.
Report
Share
Report
Share
Download to read offline
Recommended
PROactive evaluation of function to Avoid CardioToxicity

This study is intended to evaluate a new more in-depth and higher resolution cardiac MRI, MyoStrain®, to
transform the early detection of cardiac damage that can occur frequently as a result of cancer
chemotherapy. By detecting cardiac damage early, cardiologists can provide optimal cardio-protection
and allow continued use of life-saving cancer treatment for patients.
Understanding and Predicting Breast Cancer Events After Treatment

our primary outcomes will help define the relationships between cancer therapy,
CV injury, exercise intolerance and fatigue, while also accounting for the relative contributions of age,
menopause status, race/ethnicity, radiation therapy, and psychosocial and behavioral risk factors. In
addition, we will assess pre-existing cardiac risk factors (hypertension, smoking, diabetes, coronary artery
disease, dynamic changes in body mass
index, blood pressure, serum lipids and
fasting glucose, physical activity, and
chemo- and immunotherapy).
CardiovaScUlar toxicity in cancer and improvement In recovery

Patient charts should be reviewed for suspected cardiac events at each follow up time point.
Site PI’s will likely need to go through the form with the coordinators for the first 10 patients to ensure accuracy of data entered.
In Arm 1: Visit Data, there is a suspected cardiac event form to be completed at each follow up time point.
This form is basically just asking if you reviewed the patient’s chart for suspected cardiac events.
If the patient does have a suspected cardiac event, you would then complete Arm 3: Suspected Cardiac Events for that patient.
When entering information into Arm 3: Suspected Cardiac Events, the first part of the form is assessing the event from a cardiology perspective. The second part of the form is assessing the event based on CTCAE v5.0 criteria.
Medicare Advantage Ad - Testing Patients with Indications

This was created to support the use of PADnet in the Medicare Advantage space by testing patients with primary indications for peripheral artery disease
Recommended
PROactive evaluation of function to Avoid CardioToxicity

This study is intended to evaluate a new more in-depth and higher resolution cardiac MRI, MyoStrain®, to
transform the early detection of cardiac damage that can occur frequently as a result of cancer
chemotherapy. By detecting cardiac damage early, cardiologists can provide optimal cardio-protection
and allow continued use of life-saving cancer treatment for patients.
Understanding and Predicting Breast Cancer Events After Treatment

our primary outcomes will help define the relationships between cancer therapy,
CV injury, exercise intolerance and fatigue, while also accounting for the relative contributions of age,
menopause status, race/ethnicity, radiation therapy, and psychosocial and behavioral risk factors. In
addition, we will assess pre-existing cardiac risk factors (hypertension, smoking, diabetes, coronary artery
disease, dynamic changes in body mass
index, blood pressure, serum lipids and
fasting glucose, physical activity, and
chemo- and immunotherapy).
CardiovaScUlar toxicity in cancer and improvement In recovery

Patient charts should be reviewed for suspected cardiac events at each follow up time point.
Site PI’s will likely need to go through the form with the coordinators for the first 10 patients to ensure accuracy of data entered.
In Arm 1: Visit Data, there is a suspected cardiac event form to be completed at each follow up time point.
This form is basically just asking if you reviewed the patient’s chart for suspected cardiac events.
If the patient does have a suspected cardiac event, you would then complete Arm 3: Suspected Cardiac Events for that patient.
When entering information into Arm 3: Suspected Cardiac Events, the first part of the form is assessing the event from a cardiology perspective. The second part of the form is assessing the event based on CTCAE v5.0 criteria.
Medicare Advantage Ad - Testing Patients with Indications

This was created to support the use of PADnet in the Medicare Advantage space by testing patients with primary indications for peripheral artery disease
Designed this online educational booklet for Association of Community Cancer ...

VSGD design for ACCC
Critérios de escolha do tratamento - Denizar Vianna 

Palestra apresentada por Denizar Vianna no dia 19/05/2016, no VI Fórum Nacional de Políticas de Saúde em Oncologia
Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...

Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...Health Sciences North | Horizon Santé Nord
Dr. Amanda Hey's presentation from the 2013 Regional Oncology ConferenceThe Waikato Virtual Lesion Clinic - better, sooner and more convenient

The Waikato Virtual Lesion Clinic - better, sooner and more convenientHealth Informatics New Zealand
Dr. David Lim
Waikato District Health Board
(4/11/10, Illott, 10.30)Meaningful Use: Programs, Penalities, and Payments

Meaningful Use is not dead!
MIPS may be just around the corner, but MU is still very much in the picture. There is enough time, however, for your practice to optimize 2016 reporting and increase 2018 payments and avoid penalties.
This presentation takes you through the steps needed to successfully attest for 2016 and be prepared for upcoming changes.
Northeast Case for Action: Colorectal Cancer, Mr. Mark Hartman

Northeast Case for Action: Colorectal Cancer, Mr. Mark HartmanHealth Sciences North | Horizon Santé Nord
Mark Hartman's opening presentation for the 2013 Regional Oncology Conference.WON Molecular Tumor Board Presentation

By Dr. Mark Burkard of the University of Wisconsin Carbone Cancer Center.
WONIX - Wisconsin Oncology Network of Imagine Excellence

Learn about WONIX - the Wisconsin Oncology Network of Imagine Excellence, based at the University of Wisconsin Carbone Cancer Center in Madison.
Risk Adjustment: Determining Risk Determines Reward

Are you:
Keeping up to date with your risk scoring?
Missing out on reimbursement premiums?
Ensuring accurate health profiles for your patients?
Proper risk adjustment is important, not only to ensure your patients' quality of care, but also to improve your bottom line. This CareOptimize presentation will take you from the basic tenets of risk adjustment to specific ways you can increase your risk scores and get the highest premium payments.
Radiation Oncology Department Awarded Prestigious Accreditation

The prestigious ACR accreditation is awarded only to facilities that prove during a rigorous peer-review evaluation that they meet specific Practice Guidelines and Technical Standards developed by the ACR.
American College of Surgeons Commission on Cancer Recognizes South Nassau Can...

American College of Surgeons Commission on Cancer Recognizes South Nassau Can...South Nassau Communities Hospital
This is the third consecutive time that South Nassau has earned the national mark of excellence, which is awarded to eligible ACS accredited cancer programs every three years.Risk adjustment documentation and coding overview

A collection of information from publicly available sources to help you:
• Know what Risk Adjustment (RA) is and why it is important to Medicare Advantage providers
• Understand Hierarchical Condition Categories (HCCs)
• Become familiar with Risk Adjustment Documentation and Coding Requirements
CanIMPACT Clinical Map - Jones

Peter Jones, Smriti Shakdher, Prateeksha Singh
Clinical Synthesis Map: Cancer Care Pathways in Canadian Healthcare
Jones PH, Shakdher S and Singh P. Systemic visual knowledge translation for breast and colorectal cancer research. Current Oncology 2017 (in press).
The Clinical Map visually represents breast and colorectal cancer processes across Canadian provincial and territorial systems. A roadmap metaphor illustrates a system-wide view of patient flow across the stages of cancer care. Green “road signs” identify clinical cancer stages across the roadmap: Pre-Diagnosis, Peri-Diagnosis, Diagnostic Interval, Diagnosis, Treatment, Rehabilitation, After Care, and Survivorship (with Palliative Care expressed as an end point). The visual metaphor of seasonal trees visually connects these stages to the patient’s cancer journey from pre-diagnosis (summer) through treatment (winter), followed by new growth (spring) in survivorship.
The levels of primary, secondary and tertiary care guide the vertical dimension. Information and communications technology reaches across levels and stages, but is shown disconnected from primary care. The road-like pathways are colour-coded where experts differentiated care pathways between breast cancer (pink) and colorectal (blue). Where not distinguished (white), the pathways indicate current practices shared across the cancer journeys.
Yellow navigation signs indicate cancer events across primary care pathways. Starting with Prevention and ending with Long-term Care, these events show points for primary care continuity during cancer treatment. A parallel path below the stages indicates where some patients may also employ complementary or alternative therapies.
Significant areas of complexity generalized across cancer care are revealed in peri-diagnosis and the diagnostic interval pathways. A patient can be screen-detected (and then present to a family physician, shown in the breast cancer pathway) or may be initially diagnosed in primary care (white pathway). The circular pathways in the diagnostic cycle suggest multiple possible tests within primary care. With a primary care diagnosis, patients are referred and flow to secondary/tertiary cancer care. The stages of intake, biopsy, pathology, and confirmed diagnosis are shown, and the complex pathways of cancer treatment, shown on the map in a typical (not definitive) order of surgery, radiation/chemotherapy, and continuing treatment through assessment of outcome.
Coding For RCM Managers

What to measure and track in a coding operation. How to improve quality and reimbursement. The benefits of using computer-assisted coding software.
More Related Content
What's hot
Designed this online educational booklet for Association of Community Cancer ...

VSGD design for ACCC
Critérios de escolha do tratamento - Denizar Vianna 

Palestra apresentada por Denizar Vianna no dia 19/05/2016, no VI Fórum Nacional de Políticas de Saúde em Oncologia
Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...

Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...Health Sciences North | Horizon Santé Nord
Dr. Amanda Hey's presentation from the 2013 Regional Oncology ConferenceThe Waikato Virtual Lesion Clinic - better, sooner and more convenient

The Waikato Virtual Lesion Clinic - better, sooner and more convenientHealth Informatics New Zealand
Dr. David Lim
Waikato District Health Board
(4/11/10, Illott, 10.30)Meaningful Use: Programs, Penalities, and Payments

Meaningful Use is not dead!
MIPS may be just around the corner, but MU is still very much in the picture. There is enough time, however, for your practice to optimize 2016 reporting and increase 2018 payments and avoid penalties.
This presentation takes you through the steps needed to successfully attest for 2016 and be prepared for upcoming changes.
Northeast Case for Action: Colorectal Cancer, Mr. Mark Hartman

Northeast Case for Action: Colorectal Cancer, Mr. Mark HartmanHealth Sciences North | Horizon Santé Nord
Mark Hartman's opening presentation for the 2013 Regional Oncology Conference.WON Molecular Tumor Board Presentation

By Dr. Mark Burkard of the University of Wisconsin Carbone Cancer Center.
WONIX - Wisconsin Oncology Network of Imagine Excellence

Learn about WONIX - the Wisconsin Oncology Network of Imagine Excellence, based at the University of Wisconsin Carbone Cancer Center in Madison.
Risk Adjustment: Determining Risk Determines Reward

Are you:
Keeping up to date with your risk scoring?
Missing out on reimbursement premiums?
Ensuring accurate health profiles for your patients?
Proper risk adjustment is important, not only to ensure your patients' quality of care, but also to improve your bottom line. This CareOptimize presentation will take you from the basic tenets of risk adjustment to specific ways you can increase your risk scores and get the highest premium payments.
Radiation Oncology Department Awarded Prestigious Accreditation

The prestigious ACR accreditation is awarded only to facilities that prove during a rigorous peer-review evaluation that they meet specific Practice Guidelines and Technical Standards developed by the ACR.
American College of Surgeons Commission on Cancer Recognizes South Nassau Can...

American College of Surgeons Commission on Cancer Recognizes South Nassau Can...South Nassau Communities Hospital
This is the third consecutive time that South Nassau has earned the national mark of excellence, which is awarded to eligible ACS accredited cancer programs every three years.Risk adjustment documentation and coding overview

A collection of information from publicly available sources to help you:
• Know what Risk Adjustment (RA) is and why it is important to Medicare Advantage providers
• Understand Hierarchical Condition Categories (HCCs)
• Become familiar with Risk Adjustment Documentation and Coding Requirements
CanIMPACT Clinical Map - Jones

Peter Jones, Smriti Shakdher, Prateeksha Singh
Clinical Synthesis Map: Cancer Care Pathways in Canadian Healthcare
Jones PH, Shakdher S and Singh P. Systemic visual knowledge translation for breast and colorectal cancer research. Current Oncology 2017 (in press).
The Clinical Map visually represents breast and colorectal cancer processes across Canadian provincial and territorial systems. A roadmap metaphor illustrates a system-wide view of patient flow across the stages of cancer care. Green “road signs” identify clinical cancer stages across the roadmap: Pre-Diagnosis, Peri-Diagnosis, Diagnostic Interval, Diagnosis, Treatment, Rehabilitation, After Care, and Survivorship (with Palliative Care expressed as an end point). The visual metaphor of seasonal trees visually connects these stages to the patient’s cancer journey from pre-diagnosis (summer) through treatment (winter), followed by new growth (spring) in survivorship.
The levels of primary, secondary and tertiary care guide the vertical dimension. Information and communications technology reaches across levels and stages, but is shown disconnected from primary care. The road-like pathways are colour-coded where experts differentiated care pathways between breast cancer (pink) and colorectal (blue). Where not distinguished (white), the pathways indicate current practices shared across the cancer journeys.
Yellow navigation signs indicate cancer events across primary care pathways. Starting with Prevention and ending with Long-term Care, these events show points for primary care continuity during cancer treatment. A parallel path below the stages indicates where some patients may also employ complementary or alternative therapies.
Significant areas of complexity generalized across cancer care are revealed in peri-diagnosis and the diagnostic interval pathways. A patient can be screen-detected (and then present to a family physician, shown in the breast cancer pathway) or may be initially diagnosed in primary care (white pathway). The circular pathways in the diagnostic cycle suggest multiple possible tests within primary care. With a primary care diagnosis, patients are referred and flow to secondary/tertiary cancer care. The stages of intake, biopsy, pathology, and confirmed diagnosis are shown, and the complex pathways of cancer treatment, shown on the map in a typical (not definitive) order of surgery, radiation/chemotherapy, and continuing treatment through assessment of outcome.
What's hot (20)
Designed this online educational booklet for Association of Community Cancer ...

Designed this online educational booklet for Association of Community Cancer ...
Critérios de escolha do tratamento - Denizar Vianna 

Critérios de escolha do tratamento - Denizar Vianna
Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...

Colorectal Cancer Disease Pathway Management, Northeast Ontario Context, Dr. ...
The Waikato Virtual Lesion Clinic - better, sooner and more convenient

The Waikato Virtual Lesion Clinic - better, sooner and more convenient
Meaningful Use: Programs, Penalities, and Payments

Meaningful Use: Programs, Penalities, and Payments
Northeast Case for Action: Colorectal Cancer, Mr. Mark Hartman

Northeast Case for Action: Colorectal Cancer, Mr. Mark Hartman
WONIX - Wisconsin Oncology Network of Imagine Excellence

WONIX - Wisconsin Oncology Network of Imagine Excellence
Risk Adjustment: Determining Risk Determines Reward

Risk Adjustment: Determining Risk Determines Reward
Radiation Oncology Department Awarded Prestigious Accreditation

Radiation Oncology Department Awarded Prestigious Accreditation
American College of Surgeons Commission on Cancer Recognizes South Nassau Can...

American College of Surgeons Commission on Cancer Recognizes South Nassau Can...
Similar to Population Health - HEDIS - Health Plan
Coding For RCM Managers

What to measure and track in a coding operation. How to improve quality and reimbursement. The benefits of using computer-assisted coding software.
Kaiser Permanente HealthConnect - EHR and SNOMED

Andrew M. Wiesenthal, MD, SM
Associate Executive Director, The Permanente Federation
The Future of Personalized Medicine

Edgewater Technology Healthcare Executive Event
Houston, TX October 2, 2008
Ed Martinez
Moffit Cancer Center
PQRS - Avoiding the Penalties?

A discussion with Jackie Coult, CHBC regarding the Physician Quality Reporting System (PQRS) and avoiding potential reimbursement penalties in 2015.
2011 ncra educational conference

Presentation for Pacific Oncology Data Management Association. Information from the 2011 NCRA educational conference.
mHealth Israel_US Reimbursement_David Farber_King & Spalding

Presentation for mHealth Israel by David Farber, Partner, King & Spalding, about US Reimbursement. The path from approval to market and navigating the world of reimbursement. The lecture introduces the basics of Medicare reimbursement, explores strategies to maximize reimbursement in certain key areas, distinguishes the differences between CMS’s mission and FDA’s mission, and emphasizes steps in an early reimbursement strategy for successful product development.
Content analytics for healthcare

Lecture at World Health Organization - Family of International Classifications Network Annual Meeting 2014
POCkeT: Reducing Cervical Cancer in Peru through GVC analysis 

POCkeT: Reducing Cervical Cancer in Peru through GVC analysis Duke University Global Value Chains Center (GVCC)
Duke student Shruti Rao presentation covers the Colposcope Value Chain.Himss Overview, Madrid Cio Meeting

Presentación utilizada por Stephen Lieber, HIMSS Global CEO en la reunión con CIO's organizada en Madrid (Febrero 2010). Introducción de HIMSS Global
Similar to Population Health - HEDIS - Health Plan (20)
The Standards Rule and the NPRM for Meaningful Use

The Standards Rule and the NPRM for Meaningful Use
mHealth Israel_US Reimbursement_David Farber_King & Spalding

mHealth Israel_US Reimbursement_David Farber_King & Spalding
POCkeT: Reducing Cervical Cancer in Peru through GVC analysis 

POCkeT: Reducing Cervical Cancer in Peru through GVC analysis
DIABETES MELLITUS WITH Applied Research in Healthcare Administration.docx

DIABETES MELLITUS WITH Applied Research in Healthcare Administration.docx
More from CARMEN ALCIVAR
More from CARMEN ALCIVAR (6)
Auditing a Wireless Network and Planning for a Secure WLAN Implementation

Auditing a Wireless Network and Planning for a Secure WLAN Implementation
Population Health - HEDIS - Health Plan
- 1. Population Health Management System – Health Plan Supporting systems Member Services(eligibility) Member Services(eligibility) Claims ManagementClaims Management LaboratoryLaboratory Colorectal Screening Metrics and Reports This measure requires adults ages 50-75 receive colorectal cancer screenings. Extract Clean Dashboards LoadStatic Reports (Distribute Standard Periodic reports) Dynamic Reports (Drill down to investigate problems) Data Mining (Automatic search for unexpected patterns) Numerator: Only those Compliant (Numerator) CPT/HCPCS LOINC Numerator: Only those Compliant (Numerator) CPT/HCPCS LOINC Data Marts B I U s e s KPIs Email Alerts Information to Drill Down reports One Click Reports Ad Hoc Reports Denominator: Identify Those Eligible (Denominator) Age, Except: Cancer/Colectomy, CPT/HCPCS, ICD Diagnosis, ICD Procedure Denominator: Identify Those Eligible (Denominator) Age, Except: Cancer/Colectomy, CPT/HCPCS, ICD Diagnosis, ICD Procedure CPT: 44388-44394, 44397, 45355, 45378-45387, 45391, 45392 CPT: 44388-44394, 44397, 45355, 45378-45387, 45391, 45392 LOINC: 2335-8, 12503-9, 12504- 7, 14563-1, 14564-9, 14565-6, 27396-1, 27401-9, 27925-7, 27926-5, 29771-3, 56490-6, 56491-4, 57905-2, 58453-2 LOINC: 2335-8, 12503-9, 12504- 7, 14563-1, 14564-9, 14565-6, 27396-1, 27401-9, 27925-7, 27926-5, 29771-3, 56490-6, 56491-4, 57905-2, 58453-2 HPCS: G0328HPCS: G0328 FOBT Flexible sigmoidoscopy Colonoscopy HPCS: G0105, G0121HPCS: G0105, G0121 HPCS: G0104HPCS: G0104 CPT: 45330-45335, 45337-45342, 45345 CPT: 45330-45335, 45337-45342, 45345 CPT: 82270, 82274CPT: 82270, 82274 Member ID • Name • DOB • Gender • SSN Providers Health Plan Patient • Reminder and recall systems for healthcare providers via email or web portal • Assessment and feedback interventions for providers. Reminder systems for patients and targeted small media including educational materials via mail, email, web portal Reports on 5 star program metrics EnrollmentEnrollment • Patient buys health plan with best ratings Statistics to decide on alternative clinic hours or delivery settings, simplified administrative procedures
- 2. References Sources: • https://www.google.com/imgres?imgurl=http://practicalanalytics.files.wordpress.com/2013/07/healthvaluechain.png&imgrefurl= http://practicalanalytics.co/2013/07/15/informatics-or-analytics-understanding-healthcare-provider-use- cases/&h=612&w=1023&tbnid=C83W5EDinr4CdM:&docid=bceW7m0m7yh4JM&ei=-drpVomhE4bW- QGc3KmADw&tbm=isch&ved=0ahUKEwjJgZvMncbLAhUGaz4KHRxuCvAQMwgnKAowCg&biw=1366&bih=667 • https://www.google.com/imgres?imgurl=https://www.healthcatalyst.com/wp-content/uploads/2013/07/enterpruse-data-model- grphic.png&imgrefurl=https://www.healthcatalyst.com/best-healthcare-data-warehouse- model&h=732&w=975&tbnid=d5RUhcbuBmfimM:&docid=KXbM8E7SBuassM&ei=-drpVomhE4bW- QGc3KmADw&tbm=isch&ved=0ahUKEwjJgZvMncbLAhUGaz4KHRxuCvAQMwhDKBowGg#h=732&imgdii=d5RUhcbuBmfimM%3A% 3Bd5RUhcbuBmfimM%3A%3Bj30fAU63iplVUM%3A&w=975 • https://www.bcbsnc.com/assets/providers/public/pdfs/u9209m_hedis_provider_tool_for_colorectal_cancer_screening.pdfhttps:/ /www.google.com/imgres?imgurl=http://image.slidesharecdn.com/healthcarepayermedicalinformaticsandanalytics- 140714155347-phpapp01/95/healthcare-payer-medical-informatics-and-analytics-30- 638.jpg%253Fcb%253D1405353445&imgrefurl=http://www.slideshare.net/frankfangwang/healthcare-payer-medical-informatics- and-analytics&h=479&w=638&tbnid=iYCwbNES47gKRM:&docid=HoRKPe2IhWI9UM&ei=-drpVomhE4bW- QGc3KmADw&tbm=isch&ved=0ahUKEwjJgZvMncbLAhUGaz4KHRxuCvAQMwgfKAIwAg#h=479&w=638 • https://www.google.com/search?espv=2&biw=1366&bih=667&tbm=isch&sa=1&q=dashboards+health+care&oq=dashboards+hea lth+care&gs_l=img.3...36026.39556.0.39658.0.0.0.0.0.0.0.0..0.0....0...1c.1.64.img..0.0.0.2gqWhPkjmYI • http://www.cdc.gov/pcd/issues/2013/13_0180.htm • http://www.hrsa.gov/quality/toolbox/measures/colorectalcancer/part4.html • Presentation class 12 Data Management
