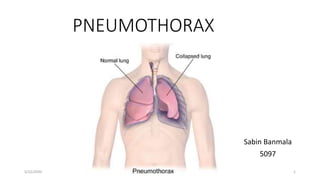
Pneumothorax
- 3. 35/22/2020
- 4. • What is PNEUMOTHORAX? • What is its pathophysiology? • ETIOLOGY? • C/F? • Investigation? • Treatment? 45/22/2020
- 5. • Pneumothorax is defined as presence of air in the pleural space 55/22/2020
- 6. 65/22/2020
- 7. Primary spontaneous pneumothorax • Occurs in young individuals without any underlying lung disease • Risk factors Smoking Tall thin male Presence of apical sub pleural blebs 75/22/2020
- 8. Secondary Spontaneous Pneumothorax • COPD • TB • Asthma • Lung abscess • Pulmonary infarcts • Lung cancer • Fibrotic and cystic diseases 85/22/2020
- 9. Pathophysiology and Mechanism • In normal people, the pressure in pleural space is negative during the entire respiratory cycle. • Two opposite forces result in negative pressure in pleural space(outward pull of the chest wall and elastic recoil of the lung) • The negative pressure will be disappeared if any communication develops . 95/22/2020
- 10. 5/22/2020 10
- 11. Pathophysiology and Mechanism • When a communication develops between an alveolus or other intrapulmonary air space and pleural space, air will flow into the pleural space until there is no longer a pressure difference or the communication is sealed • When a communication develops through chest wall between atmosphere and pleural space, air will flow into the pleural space until there is no longer a pressure difference or the communication is sealed 5/22/2020 11
- 12. Pathophysiology and Mechanism in PSP • Probable cause is rupture of apical bleb or bulla • Because the compliance of blebs or bulla in apices is lower compared with that of similar lesions situated in the lower parts of lungs • Smoking increases 9x risk in female and 22x in male smokers 5/22/2020 12
- 14. Pathophysiology Negative pressure eliminated The lung recoil-& lung-volume decrease V/Q low –anatomic shunt Hypoxia Positive pressure(Tension PNX) Compress blood vessels and heart Decreased cardiac output Impaired venous return Hypotension Result A decrease in vital capacity A decrease in PaO2 145/22/2020
- 15. 155/22/2020
- 16. Closed Pneumothorax Open Pneumothorax Tension Pneumothorax Pleural tear is sealed Pleural tear is open Pleural tear acts as one way valve(ball and valve mechanism) Pleural pressure < atmospheric pressure Pleural pressure = atmospheric pressure Pleural pressure > atmospheric pressure 165/22/2020
- 17. C/F Symptoms • Breathlessness • Unilateral pleuritic chest pain of sudden onset Signs Vitals • Closed and Open- Normal • Tension Pnx-Marked tachycardia, hypotension, rapid pulses, raised jvp cyanosis • Fever + if secondary infection occur 175/22/2020
- 18. Systemic examinatiom Inspection • Dysnea with accessary muscle use • Tracheal shift(trials sign) • Diminished chest movement in affected side Palpation • Trachea and mediastinum shifted to opposite side • Tactile fremitus absent • Diminished chest expansion of diminished side 185/22/2020
- 19. Percussion • Hyper resonant note on affected side • Liver dullness shifted inferiorly- right sided PNX • Cardiac dullness shifted to opposite side- Left sided PNX Auscultation • Breath sound absent or reduced 195/22/2020
- 21. 215/22/2020
- 22. 225/22/2020
- 23. 235/22/2020
- 24. 245/22/2020
- 25. 255/22/2020
- 26. 265/22/2020
- 27. 275/22/2020
- 28. 285/22/2020
- 29. 295/22/2020
- 30. 305/22/2020
- 31. CT Scan • It is recommended in difficult cases such as patients in whom the lungs are obscured by overlying surgical emphysema • To differentiate a pneumothorax from suspected bullous disease 315/22/2020
- 32. 325/22/2020
- 33. 335/22/2020
- 34. 345/22/2020
- 35. 355/22/2020
- 36. Treatment Goal • To promote lung expansion • To eliminate the pathogenesis/cause • To decrease pneumothorax recurrence 365/22/2020
- 37. Treatment Options 1. Supplemental Oxygen 2. Simple needle aspiration 3. Catheter aspiration 4. Intercostal tube drainage with under water seal 5. Surgery 375/22/2020
- 38. Treatment options depends on • Classification of pneumothorax • Pathogenesis • The extension of lung collapse(small or large Pnx) • Severity of disease • Complication and concomitant underlying diseases 385/22/2020
- 39. Supplemental Oxygen • Inhalation of high concentration oxygen at the rate of 10L/min • Increases the rate of reabsorption of air from pleural space • Because it reduces the total pressure of gases in pleural capillaries by reducing partial pressure of Nitrogen 395/22/2020
- 40. Simple needle aspiration Indication • PSP with significant breathlessness and/or size > 2cm • SSP with pt age<50 and even with small pnx(size<2cm) 405/22/2020
- 41. Catheter aspiration • PSP when 1st aspiration is unsuccessful • Or volume of <2.5L aspirated in 1st aspiration 415/22/2020
- 43. Intercostal tube drainage • inserted in the fourth, fifth or sixth intercostal space in the mid- axillary line, connected to an underwater seal or one-way Heimlich valve secured firmly to the chest wall. • Clamping of an intercostal drain is potentially dangerous and rarely indicated • drain removed the morning after the lung has fully re-inflated and bubbling has stopped. • Continued bubbling after 5–7 days is an indication or surgery. • If bubbling in the drainage bottle stops before full re-inflation, the tube is either blocked or kinked or displaced 435/22/2020
- 44. Surgical pleurodesis Indication • 2nd ipsilateral PNX (Recurrent PNX) • Continued bubbling after 5-7 days of ICTD • B/L PNX • Professions at risk (divers, pilot) even after 1st PNX Techniques • Open thoracotomy: partial pleurectomy/ pleural abrasion • VATS(Video assisted thoracic surgery): partial pleurectomy/ pleural abrasion 445/22/2020
- 45. 455/22/2020
- 46. 5/22/2020 46
- 47. Tension PNX • Life threatening condition • Pressure in the pleural space > atmospheric pressure throughout the respiration • PP-Traumatic, Positive airway pressure C/F- Symptoms: • rapidly progressive SOB, chest pain 475/22/2020
- 48. Signs • Tachypnea • tachycardia, • Hypotension • Cyanosis • Raised jvp 485/22/2020
- 49. CXR • Mediastinal shift • Flattening of the hemidiaphragm • Lung collapse. 495/22/2020
- 50. Management • Give high flow 0xygen • Percutaneous needle aspiration-hissing air confirms diagnosis • Insert intercostal tube drainage 505/22/2020
- 51. • What is PNEUMOTHORAX? • What is its pathophysiology? • ETIOLOGY? • C/F? • Investigation? • Treatment? 515/22/2020
Editor's Notes
- Positive pressure ventilation: Alveolar rupture interstitial emphysema pneumothorax.(B/L PNX) I nterventional procedures: Biopsy, thoraco-centesis, CVP line,trachestomy
- Amphoric breath sound-BP fistula Hamman sign-left sided PNX