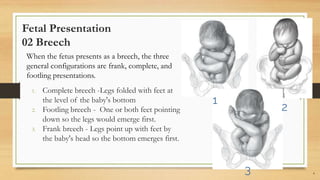
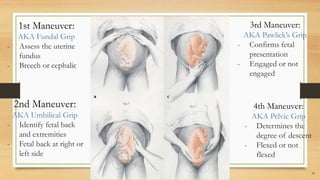
The document provides a comprehensive overview of normal labor and delivery processes, including mechanisms of labor, fetal presentations, and the stages of labor. It details management strategies during the first and second stages, along with diagnostic techniques like Leopold's maneuver, and emphasizes the importance of proper monitoring and assistance during childbirth. Additionally, it discusses the third stage of labor, highlighting placental delivery and postpartum care.