MeningoccalDisease-ADAM.pptx
•Download as PPTX, PDF•
0 likes•9 views
kmlm rg ;[rl.,golp,r \[l,rglk,ewr \p;klrm,g[we; ]f;[]wel[ [wee kwe,g[\lwe\gl w;[]\lw [lw[] ;] [[wel;[] wel.[] '\wel;.[] ]wewel [w.e \]l.,p;le. '\.];lekgmlew ]'polweookmgflewk, pl;kmeklgmelw; ]\;'lkew,meglgew,m '\]L
Report
Share
Report
Share
Recommended
Recommended
More Related Content
Similar to MeningoccalDisease-ADAM.pptx
Similar to MeningoccalDisease-ADAM.pptx (20)
imagingofintracranialinfectionsincludingcovid19pk2-200605190339 (1).pptx

imagingofintracranialinfectionsincludingcovid19pk2-200605190339 (1).pptx
More from mernahazazah
More from mernahazazah (11)
General Approaches to Prevent and Control NCDs.pdf

General Approaches to Prevent and Control NCDs.pdf
Recently uploaded
God is a creative God Gen 1:1. All that He created was “good”, could also be translated “beautiful”. God created man in His own image Gen 1:27. Maths helps us discover the beauty that God has created in His world and, in turn, create beautiful designs to serve and enrich the lives of others.
Explore beautiful and ugly buildings. Mathematics helps us create beautiful d...

Explore beautiful and ugly buildings. Mathematics helps us create beautiful d...christianmathematics
Mehran University Newsletter is a Quarterly Publication from Public Relations OfficeMehran University Newsletter Vol-X, Issue-I, 2024

Mehran University Newsletter Vol-X, Issue-I, 2024Mehran University of Engineering & Technology, Jamshoro
Recently uploaded (20)
Explore beautiful and ugly buildings. Mathematics helps us create beautiful d...

Explore beautiful and ugly buildings. Mathematics helps us create beautiful d...
Mixin Classes in Odoo 17 How to Extend Models Using Mixin Classes

Mixin Classes in Odoo 17 How to Extend Models Using Mixin Classes
Presentation by Andreas Schleicher Tackling the School Absenteeism Crisis 30 ...

Presentation by Andreas Schleicher Tackling the School Absenteeism Crisis 30 ...
Beyond the EU: DORA and NIS 2 Directive's Global Impact

Beyond the EU: DORA and NIS 2 Directive's Global Impact
Unit-IV; Professional Sales Representative (PSR).pptx

Unit-IV; Professional Sales Representative (PSR).pptx
Micro-Scholarship, What it is, How can it help me.pdf

Micro-Scholarship, What it is, How can it help me.pdf
Asian American Pacific Islander Month DDSD 2024.pptx

Asian American Pacific Islander Month DDSD 2024.pptx
Python Notes for mca i year students osmania university.docx

Python Notes for mca i year students osmania university.docx
Ecological Succession. ( ECOSYSTEM, B. Pharmacy, 1st Year, Sem-II, Environmen...

Ecological Succession. ( ECOSYSTEM, B. Pharmacy, 1st Year, Sem-II, Environmen...
General Principles of Intellectual Property: Concepts of Intellectual Proper...

General Principles of Intellectual Property: Concepts of Intellectual Proper...
Web & Social Media Analytics Previous Year Question Paper.pdf

Web & Social Media Analytics Previous Year Question Paper.pdf
Russian Escort Service in Delhi 11k Hotel Foreigner Russian Call Girls in Delhi

Russian Escort Service in Delhi 11k Hotel Foreigner Russian Call Girls in Delhi
Measures of Central Tendency: Mean, Median and Mode

Measures of Central Tendency: Mean, Median and Mode
Seal of Good Local Governance (SGLG) 2024Final.pptx

Seal of Good Local Governance (SGLG) 2024Final.pptx
MeningoccalDisease-ADAM.pptx
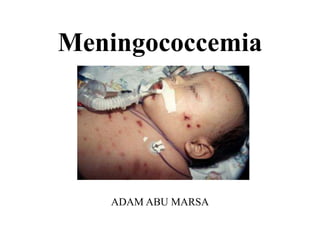
- 2. • Meningococcemia is defined as dissemination of meningococci (Neisseria meningitides) into the bloodstream • Patients with acute meningococcemia may present with • (1) meningitis ( 30%-50%) • (2) meningitis with meningococcemia (40%) • (3) meningococcemia without clinically apparent meningitis (7%-10%)
- 3. Background • Neisseria meningitidis is an encapsulated gram-negative diplococcus • There are at least 13 serogroups of the bacterium • Transmission: The human nasopharynx is the only known reservoir for N meningitides, transmitted via aerosols and nasopharyngeal secretions
- 4. Pathophysiology • fundamental pathologic change: diffuse vascular injury characterized by: 1- endothelial necrosis 2- intraluminal thrombosis 3- perivascular hemorrhage
- 5. Pathophysiology • Endotoxin, cytokines, and free radicals damage the vascular endothelium, producing platelet deposition and vasculitis • Multiple organ failure, shock, and death may results due to Disseminated intravascular coagulation (DIC)
- 6. Pathophysiology – Patients with fulminant meningococcemia develop thrombosis and hemorrhage in: • skin • mucous membranes • serosal surfaces • adrenal sinusoids • renal glomeruli
- 7. clinical presentation • include any of the following: • A nonspecific prodrome of cough, headache, and sore throat • Fever and chills • malaise, weakness, myalgias, headache, nausea, vomiting, and arthralgias • characteristic petechial skin rash is usually located on the trunk and legs and may rapidly evolve into purpura
- 8. clinical presentation • Meningitis S&S: Headache, Fever, Vomiting, Photophobia, Lethargy, Neck stiffness • In fulminant meningococcemia, a hemorrhagic eruption, hypotension, and cardiac depression, as well as rapid enlargement of petechiae and purpuric lesions
- 9. Physical findings may include the following: • Dermatologic manifestations: Petechiae, rash, ecchymoses, purpura • Meningococcal meningitis: Pain and resistance to neck flexion, other signs of meningeal irritation, petechiae, fever (of variable intensity) • Meningococcal septicemia: Fever, rash, tachycardia, hypotension, cool extremities, initially normal level of consciousness • Fulminant meningococcemia: Purpuric eruption, hemorrhages on buccal mucosa and conjunctivae, no signs of meningitis, cyanosis, hypotension, profound shock, high fever, pulmonary insufficiency
- 15. Diagnosis • Definitive diagnosis of meningococcal disease is established by isolation of N. meningitidis from a normally sterile body fluid such as blood, CSF, or synovial fluid • CBC, electrolytes, coagulation studies, Blood urea nitrogen and creatinine, Lumbar puncture and CSF analysis, blood culture
- 16. PROGNOSIS • Most deaths occur within 48 hr of hospitalization in children with meningococcemia • Poor prognostic factor: hypothermia or extreme hyperpyrexia, hypotension or shock, purpura fulminans, seizures, leukopenia, thrombocytopenia (including DIC), acidosis, and high circulating levels of endotoxin and TNF-α • poorer prognosis: The presence of petechiae for <12 hr before admission, absence of meningitis, and low or normal ESR
- 17. Management • Third-generation cephalosporins such as ceftriaxone (2 g IV /24h) or cefotaxime (2 g IV q4-6h) are the preferred antibiotics • Alternative agents include • (1) ampicillin 12 g/d either by continuous infusion or by divided dosing q4h • (2) moxifloxacin 6-8 g/d IV • The course of therapy is 7-10 days