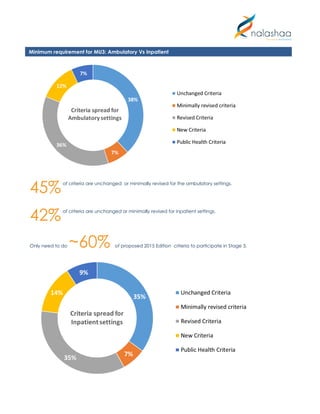
Meaningful Use Stage 3 represents the next evolution of healthcare standards, with providers now able to utilize APIs to meet reporting criteria. Starting in 2018, all health organizations will be mandated to report according to new criteria, which include a reduction in objectives and an increased focus on interoperability. Key changes include fewer total objectives for eligible professionals and hospitals, as well as a shift towards more flexible public health reporting measures.