This document summarizes a public engagement event on integrating care in Eastern Cheshire. It includes:
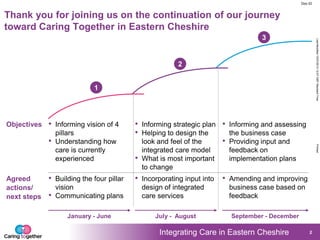
1. An agenda for the event that focused on international case examples of integrated care, developing a vision for integrated care locally, and what integrated care could look like in practice.
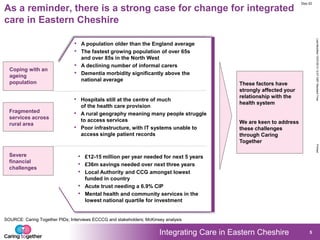
2. Feedback from previous engagement events emphasizing a need for improved coordination, communication, and community-based care.
3. A vision for integrated care centered around four pillars: empowering individuals, community-provided care, local specialist care, and regional specialized care.
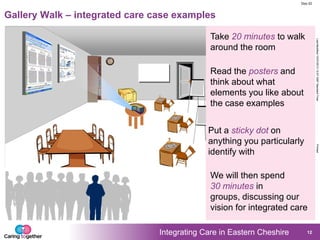
4. Activities where attendees provided input on what improved integration would look like in practice and reviewed international case studies. They discussed and provided feedback on a vision