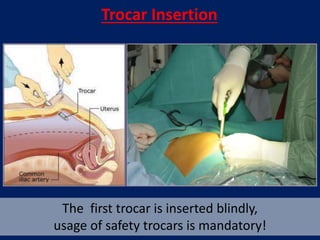
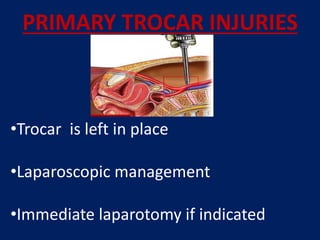
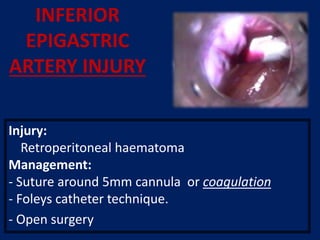
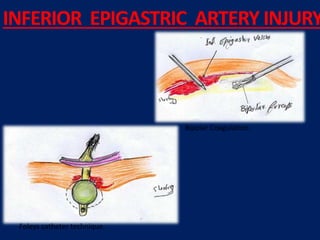
- Inserts a Foley catheter through the 5mm port
- Inflates the balloon in the retroperitoneum
- Compresses the bleeding vessel
- Allows controlled deflation after haemostasis
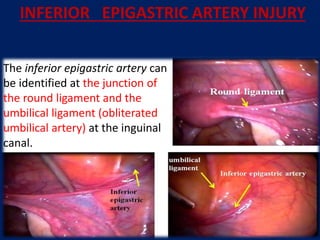
INFERIOR EPIGASTRIC ARTERY INJURY
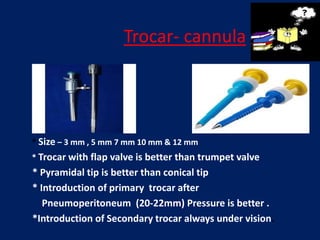
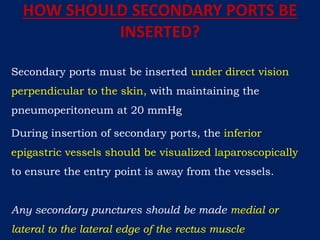
�SECONDARY TROCAR INJURIES
- Bowel injury
- Vascular injury
- Bladder injury
- Ureteric injury
Risk factors:
- Poor technique
- Adhesions
- Obesity
- Previous surgery
Management:
- Laparoscopic repair
- Conversion to laparotomy
SECONDARY TROCAR INJURIES
�HAND INSTRUMENT