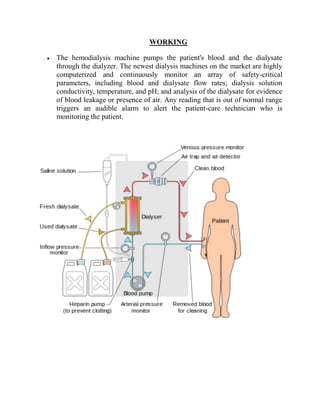
This document provides information about hemodialysis machines. It discusses how hemodialysis machines work by pumping blood and dialysate through a dialyzer to remove waste and fluid from the bloodstream. The main components of hemodialysis machines are the water system, which purifies water used in dialysate, and the dialyzer, which contains hollow fibers that allow diffusion and osmosis across a semipermeable membrane. Hemodialysis machines must meet various technical specifications to safely and effectively perform hemodialysis treatments.