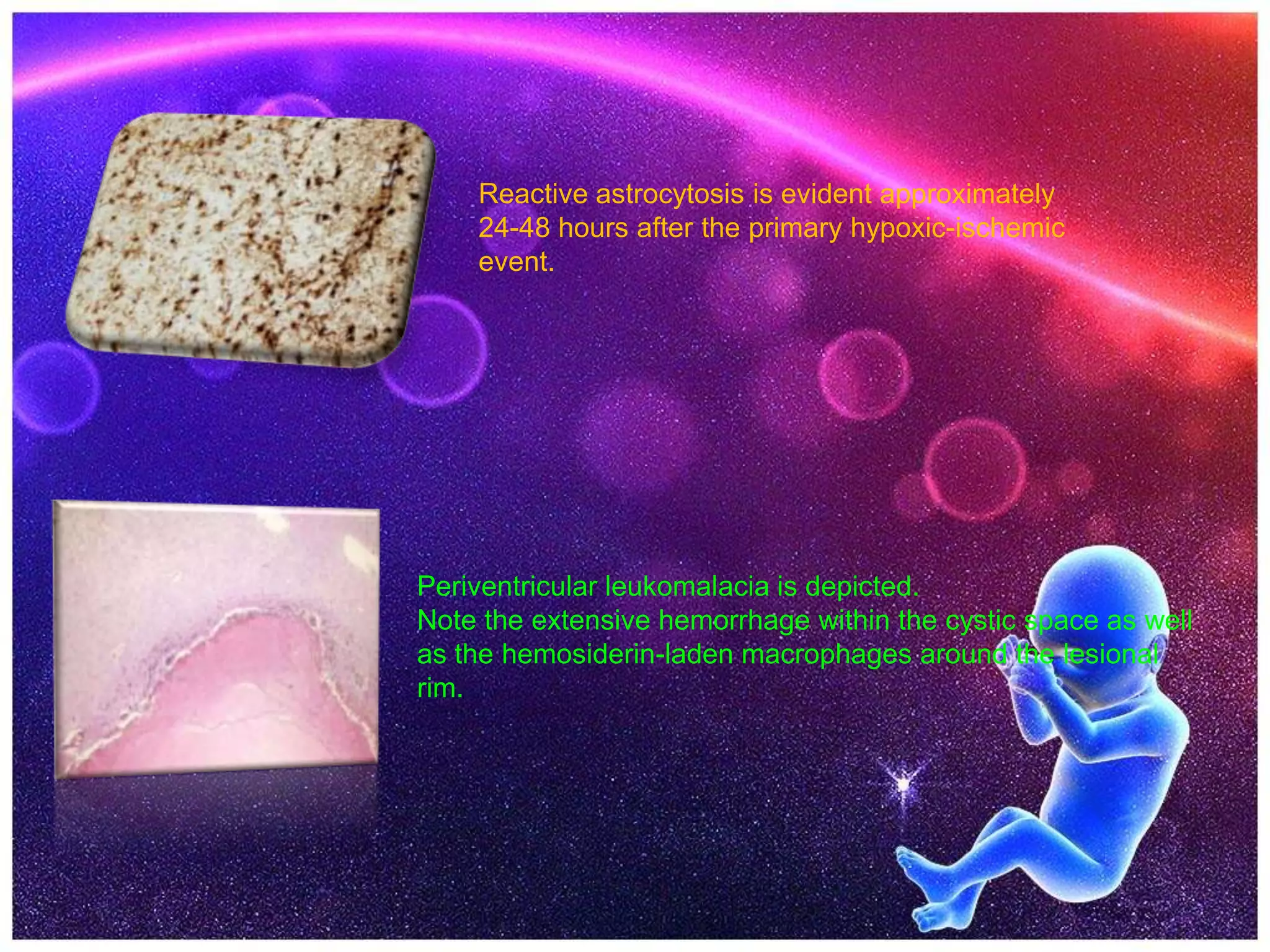
Hypoxic-ischemic encephalopathy (HIE) is brain injury caused by lack of oxygen and blood flow around the time of birth. It can cause death or long-term disabilities like cerebral palsy. Diagnosis is based on clinical presentation and lab/imaging findings. Cranial ultrasound and MRI are useful imaging modalities. HIE is characterized by Sarnat stages ranging from hyperalert to stuporous. Prognosis depends on severity - mild cases often have no complications while severe cases have high mortality or serious disabilities.





















![Treatment
Medical care
a) Initial Resuscitation and Stabilization-
• Delivery room management follows standard Neonatal Resuscitation
Program (NRP) guidelines. Close attention should be paid to appropriate
oxygen delivery, perfusion status, and avoidance of hypoglycemia and
hyperthermia.
• A lot of attention is currently focused on resuscitation with room air
versus 100% oxygen in the delivery room. Several clinical trials indicate
that room air resuscitation for infants with perinatal asphyxia is as
effective as resuscitation with 100% oxygen.
• International Liaison Committee on Resuscitation (ILCOR)
recommendations include initiating neonatal resuscitation with
concentrations of oxygen between 21-100%
Guideline] Ten VS, Matsiukevich D. Room air or 100% oxygen for
resuscitation of infants with perinatal depression. Curr Opin Pediatr. Apr
2009;21(2):188-93](https://image.slidesharecdn.com/hypoxicischaemicencephalopathy-120430100906-phpapp02-230821070951-cb9e21d3/75/hypoxicischaemicencephalopathy-120430100906-phpapp02-pdf-24-2048.jpg)
![b) Supportive Care in Patients with Hypoxic-ischemic
Encephalopathy
• Most infants with severe hypoxic-ischemic encephalopathy need
ventilatory support during first days of life.
• The role of mechanical ventilation is to maintain the blood gases and
acid-base status in the physiological ranges and prevent
hypoxia, hyperoxia, hypercapnia, and hypocapnia.
• Infants with hypoxic-ischemic encephalopathy are also at risk for
pulmonary hypertension and should be monitored. Nitric oxide (NO) may
be used according to published guidelines.
[Guideline] American Academy of Pediatrics. Committee on Fetus and Newborn. Use of
inhaled nitric oxide. Pediatrics. Aug 2000;106(2 Pt 1):344-5.](https://image.slidesharecdn.com/hypoxicischaemicencephalopathy-120430100906-phpapp02-230821070951-cb9e21d3/75/hypoxicischaemicencephalopathy-120430100906-phpapp02-pdf-25-2048.jpg)




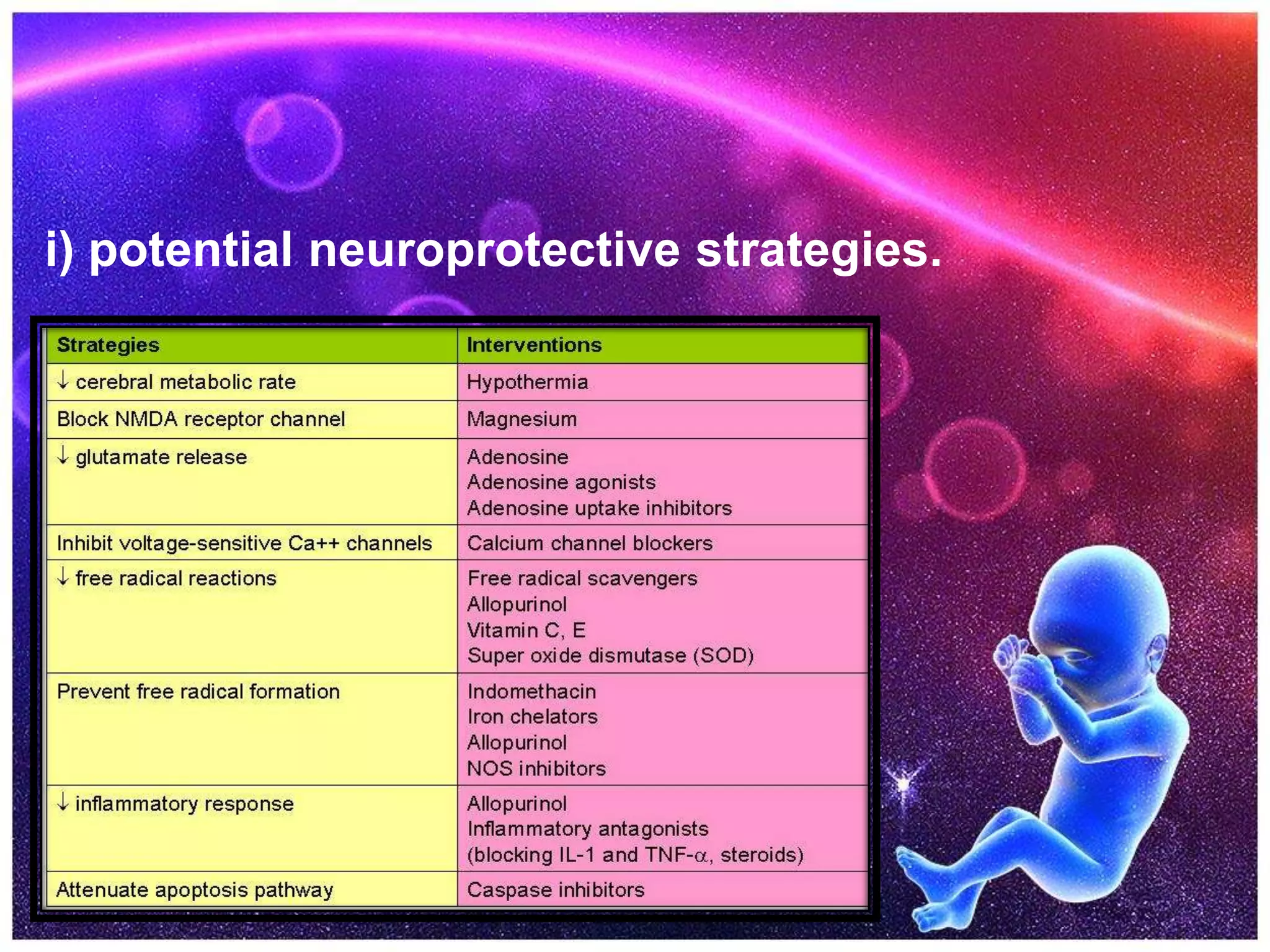
![f) Hypothermia Therapy
• Mild hypothermia (3-4°C below baseline temperature) applied within a few hours
(no later than 6 h) of injury is neuroprotective. Possible mechanisms include
(1) reduced metabolic rate and energy depletion;
(2) decreased excitatory transmitter release;
(3) reduced alterations in ion flux;
(4) reduced apoptosis due to hypoxic-ischemic encephalopathy; and
(5) reduced vascular permeability, edema, and disruptions of blood-brain barrier
functions.
• Therapeutic hypothermia when applied within 6 hours of birth and maintained for
48-72 hours is a promising therapy for mild-to-moderate cases of hypoxic-ischemic
encephalopathy.
Best Evidence] Azzopardi DV, Strohm B, Edwards AD, et al. Moderate hypothermia to treat
perinatal asphyxial encephalopathy. N Engl J Med. Oct 1 2009;361(14):1349-58.](https://image.slidesharecdn.com/hypoxicischaemicencephalopathy-120430100906-phpapp02-230821070951-cb9e21d3/75/hypoxicischaemicencephalopathy-120430100906-phpapp02-pdf-30-2048.jpg)