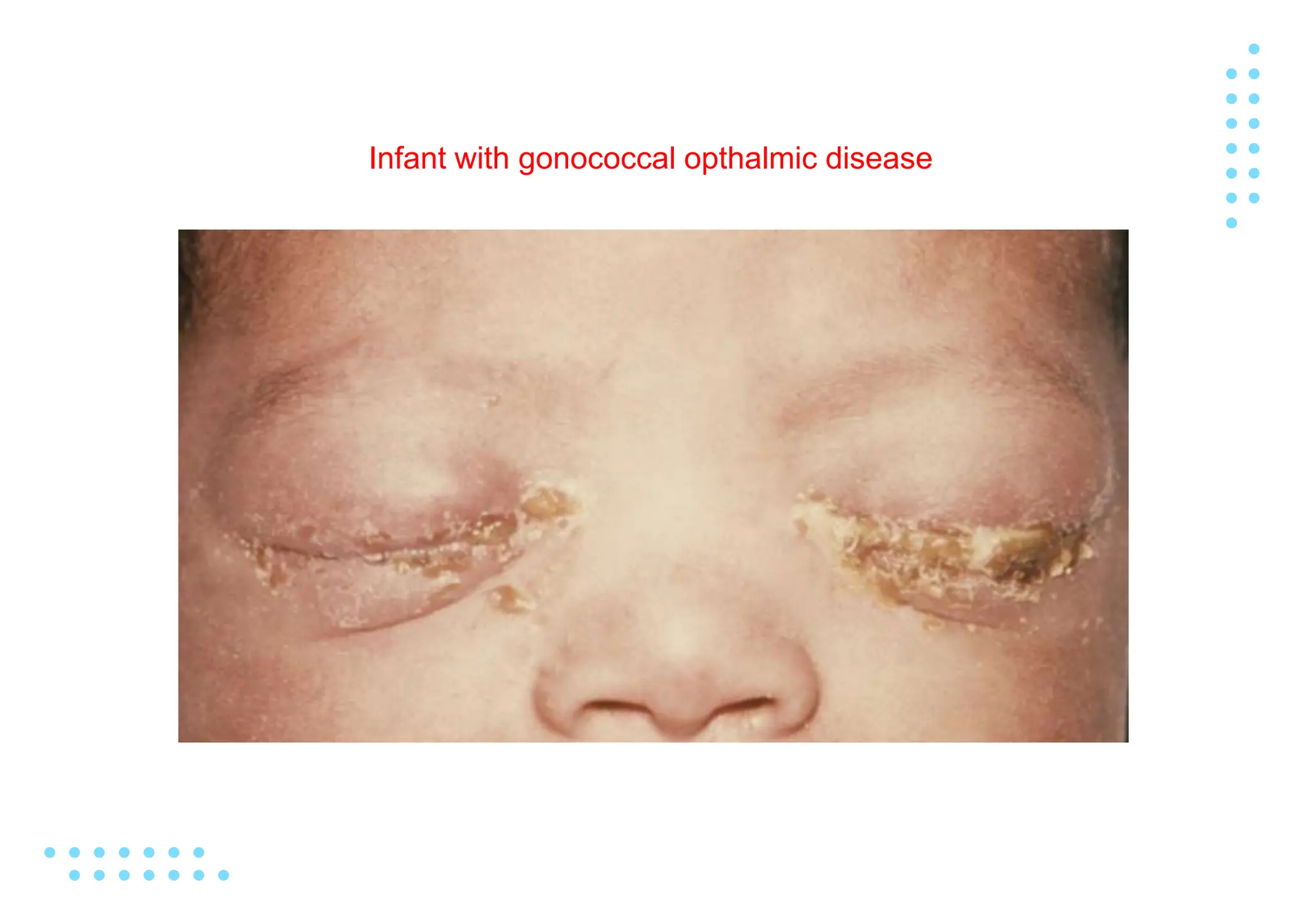
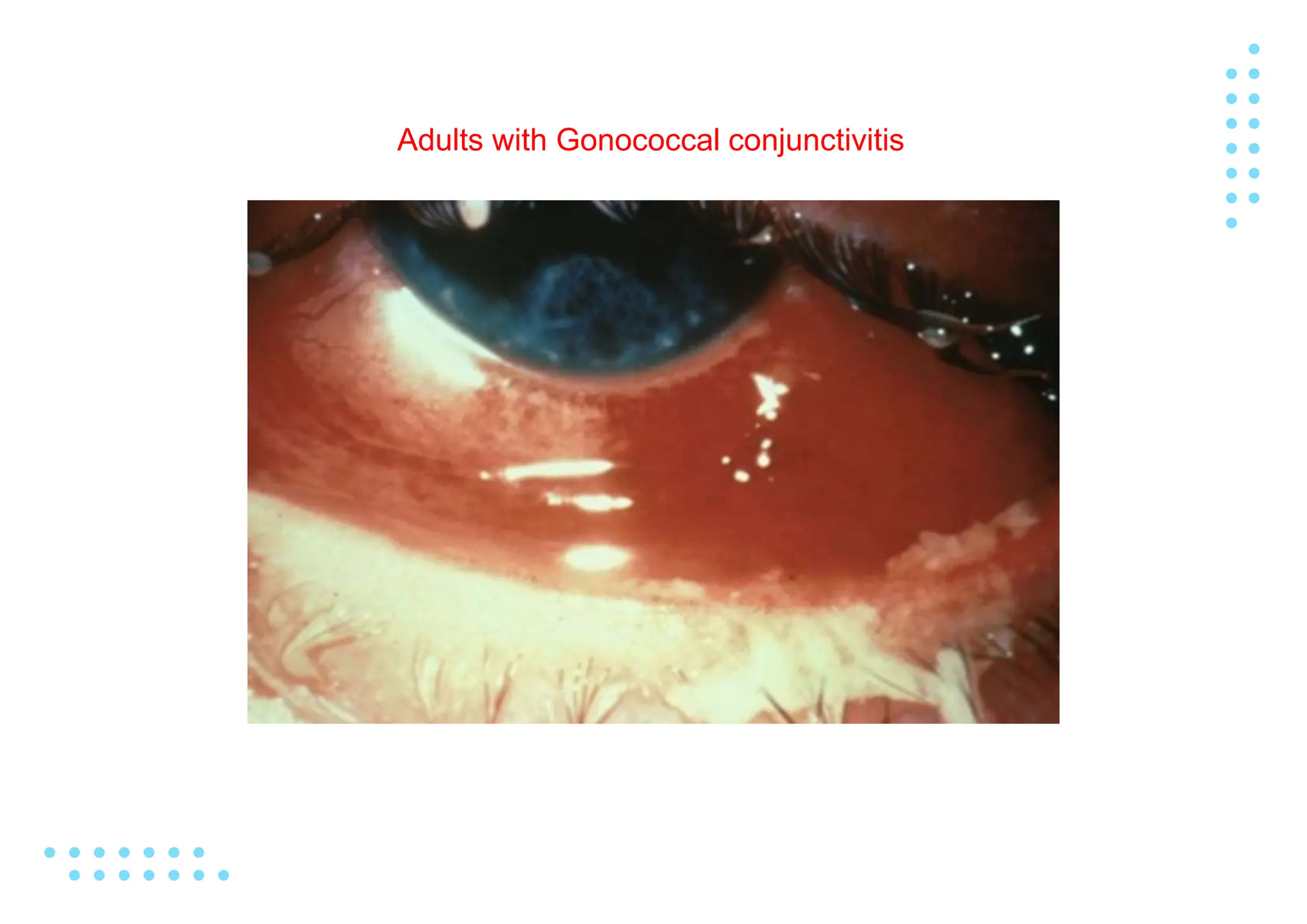
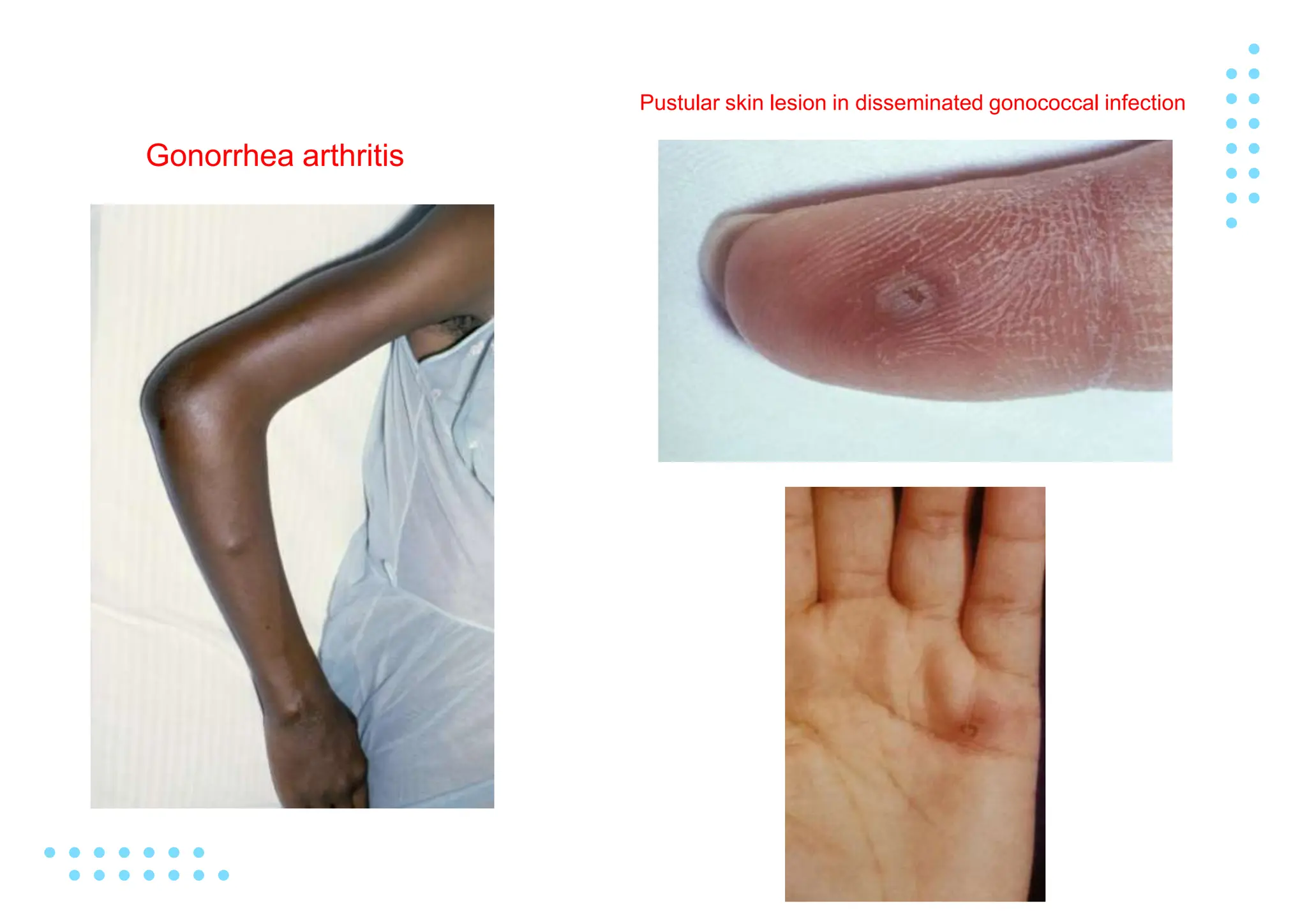
Gonorrhea is a sexually transmitted infection caused by the bacterium Neisseria gonorrhoeae. It commonly causes urethritis in men and cervicitis in women. Left untreated, it can spread and cause more serious complications like pelvic inflammatory disease, infertility, ectopic pregnancy, and disseminated infection. Diagnosis involves culture, nucleic acid amplification tests of genital secretions, and gram stain. Treatment consists of antibiotic therapy. Public health efforts aim to control the global prevalence of this highly transmissible infection.