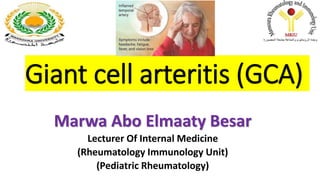
Giant cell arteritis (GCA): causes, symptoms and treatment
- 1. Giant cell arteritis (GCA) Marwa Abo Elmaaty Besar Lecturer Of Internal Medicine (Rheumatology Immunology Unit) (Pediatric Rheumatology)
- 2. Giant cell arteritis (GCA) • Is vasculitis characterized by a granulomatous infiltrate. • GCA involve medium and large arteries, in a “cephalic” phenotype, characterized by steno-occlusion of the extra-cranial branches of the external carotid arteries. • Well developed wall layers and advential vasa vasorum. • The new proposed Chapel Hill classification 2013, • GCA is one of the two main subtypes of large vessel vasculitis (LVV), together with Takayasu arteritis • “Temporal arteritis”???:- • Not all patients have temporal artery involvement. • Other vasculitis can affect the temporal arteries. Jennette JC,etal 2013
- 3. The vascular beds, • The external carotid branches; (temporal and occipital arteries). • The ophthalmic, vertebral, distal subclavian, and axillary arteries, the aorta (especially thoracic segment). • Rarely: • lower limb arteries • Intracranial arteries. • Even though LVV affect large arteries much more, large artery injury is not the cause of the most significant morbidity and many smaller branches affected (especially medium arteries).
- 4. Cardiovascular disease and Giant-cell arteritis: • Aorta involvement occurs in 15 % of patients with GCA. • GCA have an increased risk of developing aortic aneurysm (TAA) and dissection and cerebrovascular accidents, but without excess mortality. • The association was higher 1 month after the diagnosis than during follow up. • But, discovered only some years after GCA diagnosis, in the event of (often fatal) dissection or rupture. America Guidelines recommend CT or MRI of the thoracic aorta in the initial evaluation of GCA. Tomasson G,etal 2014 Current UK guidelines for management of GCA suggest a chest radiograph every 2 years to screen for TAA, but the chest radiography is not a very sensitive test.
- 5. Epidemiology:- • The prevalence; 1.47 to 20 / 100,000 people over 50 years. the highest in northern European countries and in North America. lower in Mediterranean countries. the lowest in Arabian and Asian countries (Japan). • The incidence increased over the past 20-40 years. • Age: increase progressively after 50 years of age. a mean age of onset around 72 years. • Sex: Women : men = 2-3 :1. • 45% of GCA patients have polymyalgic symptoms and 5–15 % of PMR patients will be diagnosed of GCA S.L. Bosello et al. 2016 Weyand CM, etal.2014
- 6. Pathogenesis:- • GCA remains unknown. • Both the innate and adaptive immune systems contribute to GCA pathogenesis. • Exposure to bacterial or viral antigens following infection or vaccination, in genetically predisposed patients. • Vascular lesions in inflamed temporal arteries contain an array of cytokines and inflammatory mediators. • Autoantibodies were not consistently found in GCA. • The exception was in few studies the antiphospholipid antibodies, which were found in 30–80 % of GCA cases. González-Gay MA, etal.2015
- 8. Histopathological Findings:- • The large-sized and medium-sized muscular arteries, especially the proximal aorta and its branches, (the temporal artery, occipital or cervical arteries). • Biopsy from the temporal artery as soon as possible; • Granulomatous inflammation and multinucleated giant cells at the junction of media and intima. • A mononuclear transmural infiltrate without giant cells. • Vasculitis involving small vessels close to a non-inflamed temporal artery. • False channel, inflammatory infiltrate, media modifications, and abnormalities in smooth muscle cells, associated with phagocytic activity. Carmona FD, etal 2014
- 10. Clinical Manifestations:- • Severe headache; 2/3 patients, most common onset symptoms. • Scalp tenderness; 1/5 patients. Limited to the temporal arteries, but it may also involve larger areas. Pain is usually continuous throughout the day. worsened by brushing or combing the hair.. Often interferes with sleep. Responds incompletely to analgesic drugs. • The temporal arteries appear thickened, nodulous, painful and erythematous with impaired or absent pulse. • “ jaw claudication ” is a high predictor of GCA, but is not pathognomonic. • Tongue pain, dysphagia and impaired swallowing;
- 11. • Permanent visual loss, partial or total,20% is often the first manifestation of the disease. Once established, permanent visual deficiencies. Amaurosis fugax precedes permanent loss in 44 % of the patients. Transient diplopia is present in around 6 %. • Polymyalgia is the most frequent musculoskeletal manifestation in GCA. Is 3 to 10 times more frequent in patients with GCA. can occur before, during or after the vasculitis diagnosis. some patients with PMR have subclinical vasculitis. Follow up is needed. Distal symptoms (peripheral arthritis and distal swelling, pitting oedema and Raynaud’s phenomenon) in 25 % of the patients. González-Gay MA etal 2015
- 12. Ocular Manifestations:- • Sudden, severe, and sequential vision loss is the hallmark of GCA. • The vision loss; upon awakening in the morning. Visual acuity is usually < 20/200 in more than 60 % of patients. The fellow eye usually within days to weeks of the initial eye. Can cause a sudden permanent vision loss. GCA can present weeks earlier with amaurosis fugax or a temporary vision loss. GCA may initially also present with diplopia or eye pain. • Anterior ischemic optic neuropathy (AION), A swollen optic disk accompanied by haemorrhages and sometimes exudates. This pallid swelling is due to the extreme ischemia of GCA. Due to an inflammatory thrombosis of the short posterior ciliary arteries, Jaw claudication , diplopia and temporal abnormalities are predictor. Chatterjee S eal 2014
- 13. • Posterior ischemic optic neuropathy (PION) :- Ischemia to the optic nerve posteriorly, therefore no disk swelling. • Central retinal artery occlusion (CRAO) :- About 5 % of patients over age 50. A classic cherry red spot in the macula, but no cholesterol or calcific embolus. • Ocular ischemic syndrome, Rarely cause a cilio-retinal artery occlusion. Eye pain, iritis , and hypotonia. • Cotton wool spots indicate concurrent retinal ischemia. Fluorescein angiography (FA) may helpful.
- 14. Any elderly patient presenting with visual symptoms or eye pain should be considered to be a GCA until proven otherwise in order to minimize permanent vision loss in GCA patients.
- 15. • Systemic manifestations: fever, malaise, anorexia, and weight loss. • Fever; low grade, but it reach 39–40 °C in 15 % of patients. might be the presenting manifestation. or the only feature of giant-cell arteritis. • Neurological manifestations; 30% Peripheral mononeuropathies and polyneuropathies of the upper and lower extremities. Cranial nerve palsies or ischemic myopathy rarely occur. • Respiratory tract symptoms: Cough, sore throat and hoarseness 10% Ear pain, and dizziness, vestibular or cochlear dysfunction.
- 16. • Large vessel vasculitis 25 % of patients • Aortic arch syndrome 10–15 % of patients; Claudication of the arms. Bruits over the carotid, subclavian, axillar and brachial arteries. Absent or decreased pulses in the neck or arms. • Thoracic aortic aneurysm and dissection of the aorta; late • Unfortunately, no clinical predictors to identify risk. • Disease recurrences and an incomplete response to standard steroid would raise possibility. Guida A etal 2014
- 18. Diagnosis • The diagnosis of GCA is particularly challenging. • The superficial temporal artery biopsy; the gold standard. 10–15 % of the biopsies are falsely negative. Soon when cranial GCA is suspected. Ideally prior to starting glucocorticoids. Even up to 4 weeks after initiation of therapy. On the most symptomatic side. A contralateral biopsy ??? No absolute contraindication, complications are uncommon. Segmental involvement, The facial or occipital arteries. EULAR recommendations for the management LVV recommended, (2009) that “ A temporal biopsy should be performed whenever a diagnosis of GCA is suspected, but this should not delay the treatment. A contralateral biopsy is not routinely indicated”
- 19. • Laboratory • non-specific but indicate the inflammatory nature. Increased ESR and C–reactive protein (CRP) 97%. Thrombocytosis indicate inflammation. A moderate anaemia of chronic disease. liver enzymes—particularly alkaline phosphatase. Serum interleukin-6 concentrations correlate with disease activity, a better predictor of relapse than ESR. • Imaging: • The ultrasound of the temporal artery, the ultrasound color-doppler:- A “halo” effect, a specific aspect in patients with clinically active arteritis. Sensitivity is low (40 %). US of the temporal artery, Halo sign.
- 20. • Computed tomography (CT), magnetic resonance imaging (MR), contrast angiography and positron emission tomography (PET): useful for corroborating the clinical diagnosis. to rule out asymptomatic large vessel involvement. to rule out asymptomatic progression. to evaluate cause of worsening. Cost and accessibility, radiation and contrast toxicity. • MR and CT of the aortic arch and its major branches:- Assess the extent of arterial involvement (stenosis, dissection, aneurysms) To monitor vascular lesions for any signs of progression. • 18 F-Fluorodeoxyglucose ( 18 F-FDG) PET: Provide metabolic assessment of GCA. For the diagnosis, grading, and follow-up of patients.
- 21. A 93.5 % sensitivity and to a 91.2 % specificity The American college of Rheumatology 1990 criteria for the classification of giant cell arteritis. (GCA)
- 22. Therapeutic Management:- • Corticosteroids are the cornerstone of the therapy in GCA. • The length of treatment; for 2 years to reduce the chances of relapses; or as long as 5 years. • The symptoms of GCA should respond rapidly to high-dose steroid treatment, followed by resolution of the inflammatory response. • Failure improvement, should search for an alternative diagnosis. • The incidence of new visual damage appears to decrease with disease duration. • Repeat a temporal artery biopsy, if relapse after 18–24 months and before restarting corticosteroids. • Monitoring of therapy by clinical and inflammatory markers.
- 23. Glucocorticoid Therapy:- EULAR recommends, 2009:- High-dose pulsed intravenous corticosteroids in patients with visual impairment Prednisolone 1 mg/kg/day for 1 month (in uncomplicated GCA without jaw claudication and visual disturbance) Established vision loss: 60 mg prednisolone daily to protect the contralateral eye. Tapering gradually corticosteroids: 10 mg every 2 weeks to 20 mg/die, then 2.5 mg every 2–4 weeks to 10 mg/die, then 1 mg every month Not alternate day therapy (more likely relapse) Therapy should last 1–2 years Low dose aspirin (75–150 mg per day), in the absence of contraindications.
- 24. Combination Therapy:- • Hydroxychloroquine , Methotrexate , Cyclophosphamide ,Leflunomide, Azathioprine; used as steroid sparing. • EULAR recommendations (2009) and British guidelines (2010) recommend : an immunosuppressive agent as adjunctive therapy, especially in recurrent relapses. • (Yates M etal.2014), meta-analysis; no clear benefit from using adjunct therapy with corticosteroids for the treatment.
- 25. Biologic Therapy:- • The use of anti-TNF agents is limited. Infliximab; increased risk of infection. Adalimumab; also increase infection. • IL-6 receptor antagonist tocilizumab At a dose of 8 mg /kg/ month. Rapid suppression of systemic inflammation. Increase risk of infection. • New drugs blocking IL17; achieve interesting results in GCA. Loricera J, Blanco R etal 2015
- 29. Don’t miss
- 30. Reference: 1. Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, Flores-Suarez LF, Gross WL, Guillevin L, Hagen EC, Hoffman GS, Jayne DR, Kallenberg CG, Lamprecht P, Langford CA, Luqmani RA, Mahr AD, Matteson EL, Merkel PA, Ozen S, Pusey CD, Rasmussen N, Rees AJ, Scott DG, Specks U, Stone JH, Takahashi K, Watts RA (2013) 2012 revised international Chapel Hill consensus conference nomenclature of Vasculitides. Arthritis Rheum 65(1):1– 11,January 2013. 2. González-Gay MA, Pina T (2015) Giant cell arteritis and polymyalgia rheumatica: an update. Curr Rheumatol Rep 17(2):6, February 2015. 3. Carmona FD, González-Gay MA, Martín J (2014) Genetic component of giant cell arteritis. Rheumatology (Oxford) 53(1):6–18, January 2014. 4. Chatterjee S, Flamm SD, Tan CD, Rodriguez ER (2014) Clinical diagnosis and management of large vessel vasculitis: giant cell arteritis. Curr Cardiol Rep 16(7):498, July 2014. 5. Guida A, Tufano A, Perna P, Moscato P, De Donato MT, Finelli R, Caputo D, Di Minno MN (2014) The thromboembolic risk in giant cell arteritis: a critical review of the literature. Int J Rheumatol 2014, 806402. 6. Tomasson G, Peloquin C, Mohammad A, Love TJ, Zhang Y, Choi HK, Merkel PA (2014) Risk for cardiovascular disease early and late after a diagnosis of giant-cell arteritis: a cohort study. Ann Intern Med 160(2):73–80, 21 January 2014. 7. Yates M, Loke YK, Watts RA, MacGregor AJ (2014) Prednisolone combined with adjunctive immunosuppression is not superior to prednisolone alone in terms of effi cacy and safety in giant cell arteritis: meta-analysis. Clin Rheumatol 33(2):227–236, February 2014 8. Loricera J, Blanco R, Hernández JL, Castañeda S, Mera A, Pérez-Pampín E, Peiró E, Humbría A, Calvo-Alén J, Aurrecoechea E, Narváez J, Sánchez-Andrade A, Vela P, Díez E, Mata C, Lluch P, Moll C, Hernández Í, Calvo-Río V, Ortiz-Sanjuán F, González-Vela C, Pina T, González-Gay MÁ (2015) Tocilizumab in giant cell arteritis: multicenter open-label study of 22 patients. Semin Arthritis Rheum 44(6):717–723, June 2015