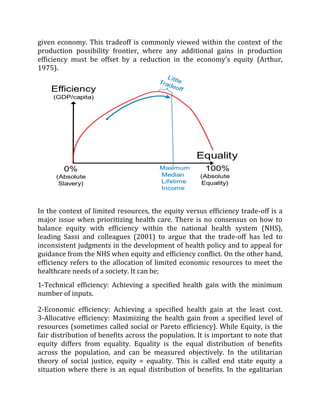
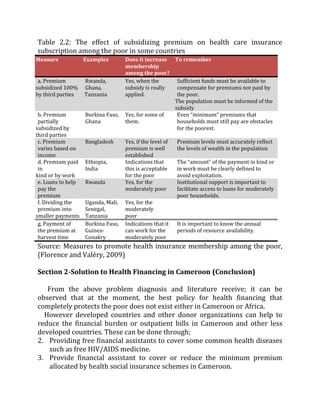
This document discusses financing primary health care in Cameroon. It notes that currently, household health financing is mostly done through out-of-pocket payments, which can lead to catastrophic health expenditures and push households into poverty. While Cameroon has social health insurance and community-based insurance programs, coverage remains low, with 62% of Cameroonians lacking access to quality healthcare. The document proposes studying alternative sustainable financing methods to improve access and reduce financial barriers to healthcare.









![Sassi F, Le Grand J, Archard L (2001). “Equity versus efficiency: a
dilemma for the NHS”. BMJ, 323: 762-763
OECD (2011), “Burden of out-of-pocket health expenditure”, in Health at a
Glance 2011: OECD Indicators, OECD
Publishing.http://dx.doi.org/10.1787/health_glance-2011-54-en
Oluyele A. Chitalu M. Naomi T. (2013), Health financing and catastrophic
payments for health care: evidence from household-level survey data in
Botswana and Lesotho, Department of Economics, University of Pretoria,
Pretoria 0002, South Africa p.g 1
PHAST (2011), Balancing Equity and Efficiency Available at
<http://www.healthknowledge.org.uk/public-health-textbook/medical-
sociology-policy-economics/4c-equality-equity-policy/balancing-equity-
efficiency>
Rama J. (2008), Can Insurance Reduce Catastrophic Out-of-Pocket Health
Expenditure? Indira Gandhi Institute of Development Research, Mumbai [pdf]
Available at <
http://www.eaber.org/sites/default/files/documents/IGIDR_Joglekar_2008.p
df> accessed in 2/07/2014 p.1
Swadhin M. Barun K. David H. P. Henry L. (2011), Catastrophic out-of-
pocket payment for health care and its impact on households: Experience
from West Bengal, India [pdf] Available at
http://www.chronicpoverty.org/uploads/publication_files/mondal_et_al_heal
th.pdf> Accessed on 1/07/2014 p.1
World Health Organization (2008), Health financing policy [pdf] Available
at <
http://www.euro.who.int/__data/assets/pdf_file/0004/78871/E91422.pdf>
p. 46
WHO (2014), Out-of-pocket health expenditure (% of private expenditure on
health) World Health Organization National Health Account database,
Available at <http://data.worldbank.org/indicator/SH.XPD.OOPC.ZS?page=4>
WHO, 2010, Monitoring the building blocks of health systems: a handbook of
indicators and their measurement strategies, Geneva: WHO.
http://www.who.int/healthinfo/systems/WHO_MBHSS_2010_full_web.pdf
World Health Organization (2010), the world health report Health systems
financing: the path to universal coverage Geneva: World Health Organization](https://image.slidesharecdn.com/finalassignment-151208170807-lva1-app6891/85/Finance-for-Development-13-320.jpg)
