Estudio sobre opiáceos vs Biofreeze
- 1. Targeted Topical Analgesics For Acute Pain YVONNE D’ARCY, MS, CRNP, CNS Pain Management and Palliative Care Nurse Practitioner Suburban Hospital-Johns Hopkins Medicine Bethesda, Maryland Ms. D’Arcy is on the fibromyalgia and chronic pain advisory boards for Pfizer, and receives book royalties from Springer Publishing. A s pressure increases to reduce the use of opioids in treating pain, prescribers are looking for ways to treat pain with other types of medications and interventions, either alone or in combination. One option is targeted topical analgesics. Some of the most popular of these medications are nonsteroidal anti-inflammatory drugs (NSAIDs) in liquid, gel, or patch formulations. The relatively easy application and the decreased potential for side effects with topical NSAIDs have made them a more desirable option when patients present with acute pain. PAINMEDICINENEWS.COM56 PRINTER-FRIENDLY VERSION AVAILABLE AT PAINMEDICINENEWS.COM Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
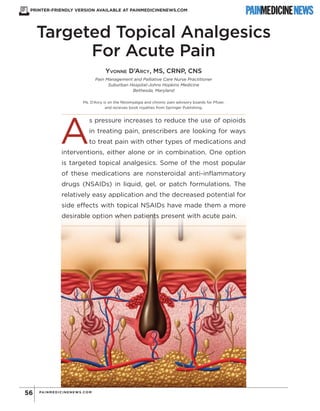
- 2. Increasingly, data are demonstrating that nonsteroidal gels, creams, and patches applied topically can provide pain relief for strains and sprains, and tendinopathies.1 The use of targeted topical analgesics for surgical pain has been limited in the past, as little research has been conducted studying their efficacy. In the United States, about 100 million surgeries are performed annually; 60% are conducted in ambulatory settings and 80% of patients report pain.2,3 Despite a national focus on improving the quality of postoperative pain management5 , patients continue to report unrelieved or undertreated pain. Although the use of topical analgesics is off-label, data demonstrate that they can reduce postoperative pain in patients undergoing prostatectomy and herniorrhaphy, as well as other conditions such as soft tissue injury and acute exacerbations of postherpetic neuralgia (PHN).4 Acute pain is a common complaint of patients presenting to emergency rooms (ERs), primary care clinics, and emergent care centers. Acute pain is defined as stemming from tissue injury, surgery, or trauma and resolves as healing occurs.5 For acute pain that is mild in intensity, patients often turn to their medicine cabinets for an over-the-counter (OTC) medication and self- treat with their favorite home remedy. This may be an analgesic cream, ice pack, or an OTC oral medication such as acetaminophen.6 For pain that is more severe, patients seek help from health care providers. Because the sources of acute pain can be diverse, it is difficult to capture its true prevalence, although it is thought to be quite high. In an ER chart review during a 7-day period, pain was documented in 61% of 1,665 patient charts; pain was identified as the chief complaint in 52% of cases.7 Of the 73 million surgeries performed in 2003, approximately 80% of patients experienced postoperative pain, with 86% reporting pain that was moderate, severe, or extreme.8 Untreated or undertreated acute pain also can result in unanticipated readmissions. Uncontrolled pain is the most common reason patients return to the hospital within the first weeks after surgery.9 In same-day surgery centers, pain accounts for 36% of all unscheduled admissions and readmissions, with orthopedic procedures (33%) the most common surgeries requiring additional pain management.10 Multimodal pain management is recommended in the treatment of acute pain. This includes opioids as well as other classes of medication, ice packs and wraps, and assistive devices such as slings. Among the easiest types of medications to use are topical patches, creams, and gels that contain a local anesthetic or NSAID. Patients can be instructed to apply these medications topically several times per day. Because of their topical application, the mechanism of action of these products is localized and the incidence of side effects is minimized. Additionally, the first-pass effect of oral medications is avoided. This article will address the pathophysiology of pain relief with topical analgesics and offer descriptions of the various compounds that are currently approved by the FDA. It will not address the use of many OTC drugs, privately compounded creams or gels, or medications that are not currently FDA–approved for use in acute pain in the United States. Pathophysiology The discussion of the pathophysiology of pain is ever evolving. As more is learned about how the body processes pain, it becomes clear that there are a number of ways to incorporate medications for pain relief into the pain-processing pathways. Topical medications use the skin as a platform for absorption. Because skin thickness and permeability vary, topical preparations can show great variation in their ability to penetrate and provide pain relief. When a topical analgesic is applied directly to the skin, it must pass through the stratum corneum, the flattened layer of keratinocytes protecting the lower layers of the epidermis. Because of this, the delivery agent in which the medication is suspended should have both hydrophilic and hydrophobic elements to allow for maximum penetration.11,12 Once the topical medication penetrates the stratum corneum, it can enter the skin’s dermal and epidermal layers, thereby gaining access to the cutaneous nociceptors. These nociceptors include unmyelinated C-nerve fibers and other nociceptive fibers, along with associated structural components such as connective tissue and fibroblasts12 (Figure, see page 4). Differences Between Topical and Transdermal Medication Absorption • Topical medications act locally, do not have systemic side effects, and exert their action mainly at the site of application. They penetrate the skin by means of pas- sive diffusion. • Transdermal medications act by systemic absorption and the side-effect profile is comparable to the systemic route. They do not need to be applied at the site of the pain.4,12 PAIN ME DICINE NE WS S P E CIAL E DITI ON 57 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 3. It is important to differentiate between topical and transdermal medication absorption routes (see differences list). A topical agent will act locally and the systemic uptake is limited. Peak plasma levels with topical medication administration range from 0.2% to 8%, with systemic absorption rates of approximately 3% to 5% of the oral route.13 Transdermal medication such as fentanyl patches will be absorbed systemically and dispersed throughout the patient’s body. The side-effect profile is comparable to the systemic route. Although the 2 delivery types can be confused, they are very different and are designed for entirely different drug delivery systems (see differences list). Candidates for Targeted Topical Medications The advantages of using a targeted topical agent for acute pain are numerous, chief among them are that patients like creams and gels. Patients are accustomed to using analgesic balms for self-treating minor aches and pain. These topical medications are not opioids, which often have side effects such as constipation, nausea, or sedation. The side-effect profile of topical agents is generally very benign. Side effects occur in 12% of patients treated with topical NSAIDs, with the most common being skin irritation.13 Patients who are candidates for topical pain medications are numerous, with the caveat that their pain should be localized with an accessible area for application of a patch or cream, gel, or liquid.1 Ideal patient types for using targeted topical agents for acute pain include: • Patients with more than one chronic condition, thus limiting the potential for drug–drug interactions. • Patients with cardiovascular and gastrointestinal risk factors that limit the use of oral NSAIDs. • Patients with renal or hepatic organ dysfunction, where the metabolism or clearance of oral medica- tions is affected. • Older patients, who as a group have greater potential for drug–drug interactions or adverse effects (AEs).1 The use of topical medications to treat pain is increasing. Conditions that are appropriate for topical analgesic use are becoming more numerous, and products such as lidocaine patches are commonly used to treat chronic pain such as that associated with PHN. However, there are some medications that have been designed for acute pain, such as the diclofenac patch (Flector Patch, Pfizer). Currently, topical medications are being used for acute and postoperative pain, as well as acute exacerbations of chronic conditions. Conditions for which targeted topical medications can be used, either alone or in combination with other analgesics, are listed here. Musculoskeletal pain Some of the most common musculoskeletal pain conditions include acute low back pain (LBP), simple ankle sprains, myofascial pain, neck pain, disk degeneration, and osteoarthritis (OA). Although some of these conditions are chronic, there are times when acute exacerbations of pain require additional treatments for pain relief. Adding a topical agent can help reduce pain with minimal intervention, providing a safe and effective option for pain control either alone or in combination with other types of medications. ACUTE LOW BACK PAIN It is estimated that 84% of adults will experience LBP at some time in their lives.14 LBP is the leading patient complaint seen by health care providers in the United States. In a study of 31,044 patients, the authors concluded that about 50% of their patients had LBP in any year and that 15% reported frequent LBP that could last for more than 2 weeks annually.15 With the national LBP treatment guidelines calling for remaining active and using medications such as acetaminophen or NSAIDs,16 targeted topical medications would be an excellent fit either as a primary or an adjunct analgesic. However, more research is needed to support the use of interventions such as lidocaine patches, although they are currently used off-label and are well tolerated. In an open-label study of 131 patients with acute/ subacute LBP, short-term chronic LBP, or chronic LBP, all 3 groups reported that use of a 5% lidocaine patch resulted in significant reductions in pain intensity.17 Similar findings were reported in a study of 71 patients, with participants reporting significant improvement at weeks 2 and 6 as measured by score changes on the Neuropathic Pain Scale.18 These findings seem to suggest that the lidocaine patch can reduce LBP in the acute phase. There is some evidence to support the use of capsaicin cream, an OTC preparation derived from cayenne peppers, to treat LBP. The main mechanism of action of capsaicin cream is as a counterirritant thought to decrease the production of substance P and desensitize nociceptive sensory neurons.12,19 The action is biphasic with TRPV1 agonist action that increases the release of substance P from the cutaneous nociceptors causing neurogenic inflammation, with subsequent reversal of defunctionalization of nerve endings causing an inhibition of pain transmission.11 Capsaicin cream is available in 2 strengths (0.025% and 0.075%) for topical application and must be applied several times a day for at least 2 weeks to achieve maximum benefit.6 A 2006 Cochrane review indicated improved visual analog scale pain scores for patients with acute back pain using capsaicin cream on days 3 and 4.19 A pooled analysis of 368 patients with PAINMEDICINENEWS.COM58 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 4. musculoskeletal pain using 0.025% capsaicin cream showed a 38% reduction in pain compared with a 25% decrease in the placebo arm (number needed to treat [NNT], 8.1).12 Because of the localized irritation, patients who are using capsaicin cream to treat acute LBP should be advised to wear gloves when applying the cream and to not touch other areas of their body, such as the eyes.6 The major AE seen with capsaicin cream is an intense burning and pain at the application site experienced by approximately 80% of patients.20 Some patients find this AE sufficiently distressing to discontinue the medication. NECK PAIN Strong evidence for the use of topical analgesics for acute neck pain is lacking. Capsaicin cream is recommended, but again the resultant burning and Figure. Cross-section of the layers of the skin. (Meissner’s) Haircorpuscle Capillaries shaft Dermal Sweat of touch papillae pore Arteriole Venule Papilla Lamellated (Panician) of the hair corpuscle Stratum corneum Stratum lucidum Stratum granulosum Stratum spinosum Stratum basale Papillary muscle Sebaceous (oil) gland Sweat gland duct Sudoriferous (sweat) gland Adipose tissue Epidermis Dermis Subcutaneous layer (Hypodermis) PAIN ME DICINE NE WS S P E CIAL E DITI ON 59 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 5. pain at the application site limits its use.20 If the patient can tolerate the applications, this AE should lessen within 1 to 2 weeks.1 SOFT TISSUE INJURIES, SPRAINS, AND STRAINS Among the many types of soft tissue injuries, sprains and strains are responsible for more than 30% of reported injuries in the United States. These injuries are commonly seen and treated by primary care practitioners or in ERs. Between 2004 and 2005, soft tissue injuries of various types were responsible for 18% of all initial visits to US ERs.21 Other common injuries such as ankle sprains cause approximately 2 million patients to seek help annually.21 The diclofenac 1.3% patch is indicated for use in soft tissue injuries such as strains and sprains. In a study of 101 patients with minor sports injuries, treatment with the diclofenac patch provided a 61% reduction in pain.22 Jousellin23 studied 134 patients with ankle pain, and found that pain at rest, pain with movement, and pain with pressure were significantly improved by day 3 when the patch was used. Overall, data from multiple studies demonstrated that the diclofenac patch is superior to placebo. The patch also has proven to reduce pain and to be well tolerated by the majority of patients. Postherpetic Neuralgia Once a patient has had chickenpox, the varicella virus is present and lies dormant in the nerve endings, waiting for a time when the patient is immunocompromised either through an illness such as cancer or has decreased immune function through normal aging. Many patients who develop herpes zoster (HZ, or shingles) experience pain accompanied by rash, with pain resolving once the rash heals. The reactivation of the varicella virus into a painful eruption of blisters that itch and burn is usually accompanied by a prodromal time period when the patient feels ill and experiences pain in the dermatome that will be the site of the eruption.6 About 10% to 18% of patients with HZ, most often those who experience severe pain during the acute phase, are likely to develop PHN.24 Once the rash heals, the affected area can become highly sensitized to the point where the wearing of clothes or mild touch are extremely painful. Patients describe this pain as comparable to the burn of a hot iron touching the skin or a horribly painful itching. The intense pain of PHN is thought to be the result of neuronal changes not only in the periphery as evidenced by neuronal loss but also atrophy of the spinal cord dorsal horn.25,26 This pain can last for weeks, months, or even years and is extremely difficult to treat. Placing a lidocaine patch over the affected area once the rash has healed can be effective in reducing pain. Qutenza (8% capsaicin patch, Acorda), can be placed over the affected area for 1 hour after a local anesthetic has been applied to reduce burning. Once the patch is removed, pain relief can last for up to 12 weeks. Despite the potential severity of pain in the eruption phase, these patches are only to be applied over areas of intact skin. Postoperative Pain Postoperative pain continues to be problematic in the United States. Despite efforts and public calls for change, patients continue to report unrelieved or undertreated pain after surgery. In a study of 300 surgical patients, 80% reported concern over control of their postoperative pain.27 Of the inpatient participants, 75% reported moderate, severe, or extreme postoperative pain, whereas 72% of the outpatients reported pain at moderate to extreme levels.27 Patients who experienced high levels of pain before surgery reported pain levels in the postoperative period to be greater. When questioned about medication choices, 57% of patients in the study preferred non-narcotic pain medications, although only 30% expressed concerns about addiction. Although opioids are considered the mainstay of acute postoperative pain management, using a multimodal approach with a variety of medications is currently recommended, making topical analgesics an option with great potential merit. Using topical analgesics for postoperative pain is attractive for several reasons. Opioids cause sedation, especially in opioid-naive surgical patients, as well as side effects that delay recovery such as nausea and vomiting. The use of topical analgesics avoids adding a medication that potentially results in these side effects. There is, however, concern over systemic absorption if the area of pain is open, a wound, or over surgical incisions, as topical analgesics are limited to areas of intact skin. The use of lidocaine patches is considered off- label in postoperative patients; however, results from 2 studies have supported their use. In a prospective, double-blind, placebo-controlled study with 71 retropubic prostatectomy patients, normal postoperative analgesic methods such as patient- controlled analgesia were supplemented with the use of a 5% lidocaine patch cut in half and placed on both sides of the surgical incision. Patients in the placebo group had a sterile gauze placed in the same location in the same fashion. The study patch and the placebo gauze were removed after 24 hours. Findings from this study indicate that the addition of the lidocaine patch along the surgical incision for 24 hours resulted in reduced pain. There was also some evidence that the reduction in pain positively affected mood and ability to walk and breathe deeply.27 In a second study with 30 patients who underwent PAINMEDICINENEWS.COM60 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 6. laparoscopic ventral hernia repair, 50% had a 5% lidocaine patch placed over the area of the underlying mesh, whereas the other half did not. Results indicated that the patients in the patch group had a statistically significant reduction in pain scores at discharge.28 The reduced pain scores continued out to a 2-week period. Although the research base is not large, it has been indicated that the use of a lidocaine patch can reduce pain in postoperative patients. In future studies, other patient types can be identified and other techniques explored. Medications A variety of medications have been adapted for use as targeted topical analgesics. Studies have shown that using the medications in this way can provide excellent pain relief. In a meta-analysis of 86 randomized studies with 10,160 patients with analysis at 1 week for acute pain, the relative benefit for pain relief was calculated at 1.7 with an NNT of 3.9.29 Patients in these studies also reported reduced pain levels compared with placebo, and none reported a better analgesic benefit with oral medications compared with topical preparations.30 In a review of 19 double-blind studies with more than 3,000 patients, the use of topical diclofenac medications reduced pain and inflammation in the area of the injury.31 Clearly, topical preparations result in satisfactory analgesic effects. GELS AND LIQUIDS The 2 medications that are most commonly used in the gel and liquid category are diclofenac sodium 1% gel (Voltaren Gel, Endo, Novartis) and diclofenac sodium topical solution 1.5% w/w dimethyl sulfoxide (Pennsaid, Mallinckrodt) liquid. Both products are FDA–approved for use in treating localized pain from OA. In a comparison study with 24 patients, 40 drops of Pennsaid and 4 grams of Voltaren gel were applied to the knee. Ninety percent of patients preferred the preparation containing dimethyl sulfoxide.31 Patients perceived a difference in the odor, feel, and stickiness of the 2 products. Both medications use the same NSAID, diclofenac, but in different formulations with different carriers. There is scant evidence for use in acute pain but there is good indication for use in OA.32 Pennsaid Pennsaid consists of diclofenac sodium 1.5% w/w dimethyl sulfoxide, which is used to enhance penetration into the skin. To apply the liquid, the patient dispenses 10 drops at a time, 4 times, into their hand and places them around the knee front to back, 4 times per day.32 Voltaren Gel Voltaren gel consists of 1% diclofenac sodium coupled with isopropyl alcohol, propylene glycol, and water, which allows for better penetration of the skin layer.32 A dosing card is supplied with the product indicating 2 g for each elbow, and 4 g for each knee, ankle, or foot, with a maximum daily dose of 32 g. Studies have found that the use of either topical diclofenac product can reduce pain and increase functionality. Baraf et al33 found that patients with knee OA who used diclofenac 1% gel 4 times daily reported improved pain relief and better function at 12 weeks compared with patients in the control group. Herndon34 found that diclofenac solution reduced pain and enhanced physical functioning at a similar level as oral diclofenac. Unfortunately, there is a lack of research on the use of these 2 products for treatment of acute pain. PATCHES The 2 analgesic patches that are most commonly used are lidocaine 5% topical anesthetic patch and diclofenac epolamine topical patch 1.3% (Flector Patch). Both patches have a flannel-type backing over a medication-infused gel and are covered by a plastic film. To use the patch, the plastic film is removed and the patch is then applied over the painful area, medication side down. 5% Lidocaine Patch Topical anesthetics such as the 5% lidocaine patch are thought to relieve pain by leaving skin sensation intact but blocking ectopic discharges from abnormal sodium channels in dermal nociceptors.12 The patches are best used in localized areas of pain. The 5% lidocaine patch consists of a woven flannel backing with 5% lidocaine in an adhesive material over the inner surface. The flannel backing helps control the release of the medication over the 12-hour application period, although patients have worn the patch for 24 hours with no ill effects.5 The maximum number of patches that can be applied at any time is 3. The patch is simple and easy to use and patients report satisfactory pain reduction. In a review of lidocaine patches,35 the use of the patch versus pregabalin in the settings of PHN and painful diabetic neuropathy demonstrated similar levels of pain relief but a greater safety profile with the patch. Single studies examining the use of lidocaine patches off-label in a variety of painful neuropathic conditions such as polyneuropathy indicated that pain control was effective; however, larger sample sizes and more studies would help confirm the positive effect of patch use. Flector Patch Flector Patch uses an NSAID, diclofenac epolamine 1.3%, encased in a ready-to-use patch that can be applied over the site of a sprain, strain, or contusion. The patch has an outer layer of polyester felt and the inner adhesive layer contains 1.3% of diclofenac epolamine in PAIN ME DICINE NE WS S P E CIAL E DITI ON 61 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 7. a polymeric hydrogel.21 The felt backing helps prevent drying of the hydrogel layer and hydrates the area of skin covered by the patch. The hydrogel enhances the absorption of the medication to allow for release over 12 hours. Multiple studies have shown the effectiveness of the Flector patch for analgesia and anti-inflammatory effect. In a multicenter, placebo-controlled study of ankle sprain treatment with 140 patients, pain scores at initiation and at 3 and 7 days were significantly improved when the Flector patch was used compared with placebo.36 In a study of 222 patients with benign sports injuries, placebo patches and Flector patches were placed over the area of the injury. The Flector patch patients reported significantly better pain relief even at 14 days.37 The most common AE with the Flector patch was topical irritation at the application site. In a comparison study with 22,949 patch applications for the Flector patch group, pruritus was the most commonly reported AE (1.6%), followed by erythema (0.6%), application site reaction (0.3%), and rash (0.3%).30 The risk–benefit analysis of using the Flector patch points to it being an effective method of pain relief and inflammation with a low incidence of AEs. Concerns for the Older Patient Topical medications are ideal for older patients who cannot tolerate opioids or oral NSAIDs. Applying a gel or liquid over a painful area can help reduce pain to a level that is tolerable and improve function. The improved pain relief with reduced AEs is a big selling point for patients with limited choices for pain medications, such as the geriatric population. There are some special concerns that bolster the arguments for using topical analgesics in the geriatric patient population. These include the following: • Reduced fat-to-muscle ratios in this age group result in a variability of drug levels, making the use of medications such as opioids less than optimal. • Reduced renal and hepatic metabolism also can affect drug clearance in older patients using oral medications. • Older patients often are taking a number of med- ications for various comorbidities, making med- ications with mild AE profiles like topicals more appealing. • Topical analgesics can help reduce the likelihood of medication interactions as well as provide localized pain relief. • The American College of Rheumatology 2012 strongly recommends the use of topical NSAIDs rather than oral NSAIDs for the management of OA of the hand, hip, and knee. • The American Geriatrics Society recommends using topical analgesics for neuropathic considerations and using topical lidocaine for localized non-neuro- pathic pain; patients with localized non-neuropathic persistent pain also may be candidates for topical NSAIDs.1 Summary The future of topical medications is wide open. There are any number of medications that can be formulated into a topical product, which would increase the number of available treatments. As demand grows for these easy-to-use medications, more investment in the development of additional products will be necessary. There is also an opportunity to develop more potential dispensing systems to better move the medications into the dermal layers. Any method to increase the active period of the medications would improve the usability of the products. Overall, topical medications in any form seem to be well accepted by the patients who use them. Side effects are low and pain relief is excellent. Increasing the use of topical analgesics in the acute pain patient population will only enhance pain relief for those patients who are now reporting unrelieved pain from surgery and acute injuries. References 1. McCarberg B, D’Arcy Y. Options in topical therapies in the management of patients with acute pain. Postgrad Med. 2013;125 (4 suppl):19-24. 2. Cullen K, Hall M, Golosinsky A. Ambulatory surgery in the United States. Nat Health Stat Rep. 2009;11:1-25. 3. National Center for Health Statistics. Number of all-listed proce- dures from discharges from short-stay hospitals by procedure category and age: United States 2009. Atlanta, GA: Centers for Disease Control and Prevention. 4. Casale R, Mattia C. Building a diagnostic algorithm on local- ized neuropathic pain (LNP) and targeted topical treatment: focus on 5% lidocaine medicated plaster. Ther Clin Risk Manag. 2014;10:259-268. 5. American Pain Society. Principles of Analgesic Use in the Treat- ment of Acute Pain and Cancer Pain. Sixth Edition. Glenview, IL: APS; 2008. 6. D’Arcy Y. A Compact Clinical Guide to Acute Pain Management. New York, NY: Springer Publishing; 2011. PAINMEDICINENEWS.COM62 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
- 8. 7. Cordell W, Keene K, Giles B, et al. The high prevalence of pain in emergency care. Am J Emerg Med. 2002;20(3):165-169. 8. Apfelbaum J, Chen C, Mehta S, et al. Postoperative pain experience: results from a national survey suggest postop- erative pain continues to be undermanaged. Anesth Analg. 2003;97(2):534-540. 9. Palomano R, Dunwoody C, Krenzischeck D, et al. Perspective on pain management in the 21st century. Pain Manag Nurs. 2008;9(1):S3-S10. 10. Coley K, Williams B, DaPos S, et al. Retrospective evaluation of unanticipated admissions and readmissions after same day surgery and associated costs. J Clin Anesth. 2002;14(5):349-353. 11. Zempsky W. Topical analgesics in treating neuropathic and muscu- loskeletal pain. Pain Medicine News. 2013;11(10):7-10. 12. Stanos S. Topical agents for the management of musculoskeletal pain. J Pain Symptom Manage. 2007;33(3):342-355. 13. Heyneman C, Lawless-Liday C, Wall G. Oral versus topical NSAIDs in rheumatic diseases: a comparison. Drugs. 2000;60(3):555-574. 14. Walker B. The prevalence of low back pain: systematic review of the literature from 1966 to 1998. J Spinal Disord. 2000;13(3):205-217. 15. Deyo R, Mirza S, Martin B. Back pain prevalence and visit rates: estimates for U.S. national surveys. Spine. 2002;31(23):2724-2727. 16. Chou R, Huffman L. Medications for acute and chronic low back pain: a review of the evidence for an American Pain Society/Amer- ican College of Physicians clinical practice guideline. Ann Intern Med. 2007;147(7):505-514. 17. Gimbel J, Linn R, Hale M, et al. Lidocaine patch treatment in patients with low back pain: results of an open label non-random- ized pilot study. Am J Ther. 2005;12(4):311-319. 18. Galer B, Gammaitoni A, Oleka N, et al. Use of the lidocaine patch 5% in reducing intensity of various pain qualities reported by patients with low back pain. Curr Med Res Opin. 2004;20(suppl 2):S5-S12. 19. Becker J, Stumbo J. Back pain in adults. Prim Care. 2013;40:271-288. 20. Pangarkar S, Lee P. Conservative treatment for neck pain: medica- tions, physical therapy, and exercise. Phys Med Rehabil Clin N Am. 2011;22:503-520. 21. McCarberg B, Argoff C. Topical diclofenac epolamine patch 1.3% for treatment of acute pain caused by soft tissue injury. Int J Clin Pract. 2010;64(11):1546-1533. 22. Jenoure P, Segessar B, Luhti U, et al. A trial with diclofenac HEP plaster as topical treatment in minor sports injuries. Drugs Exp Clin Res. 1993;19:125-131. 23. Jousellin E. Flector Tissugel in the treatment of painful ankle sprain. Traumatol Sport. 2003;20:1S5-1S9. 24. Hampton T. When shingles wanes but the pain does not: researchers target chronic postherpetic neuralgia. JAMA. 2005;293(20):2459-2460. 25. Oaklander A, Bowsher D, Galer B, et al. Herpes zoster itch: Preliminary epidemiologic data. J Pain. 2003;4(6):338-343. 26. Oaklander A. Mechanisms of pain and itch caused by herpes zoster (shingles). J Pain. 2008;9(1 suppl 1):S10-S18. 27. Habib A, Polascik T, Weizer A, et al. Lidocaine patch for postop- erative analgesia after radical retropubic prostatectomy. Anesth Analg. 2009;108(6):1950-1958. 28. Saber A, Mohammed H, Elgamal A, et al. Early experience with lidocaine patch for postoperative pain control after laparoscopic ventral hernia repair. Int J Surg. 2009;7:36-38. 29. Moore R, Tramer M, Carol D, et al. Quantitative systematic review of topically applied non-steroidal anti-inflammatory drugs. BMJ. 1998;316(7128):333-338. 30. Kuehl K. Review of the efficacy and tolerability of the diclofenac epolamine topical patch 1.3% in patients with acute pain due to soft tissue injuries. Clin Ther. 2010;32:1001-1014. 31. Galer B. A comparative subjective assessment study of Pennsaid and Voltaren Gel, two topical formulations of diclofenac sodium. Pain Pract. 2011;11(3):252-260. 32. McPherson M. Cimino N. Topical NSAID formulations. Pain Med. 2013;14:S35-S39. 33. Baraf H, Gold M, Clark M, et al. Safety and efficacy of topical diclof- enac sodium 1% gel in knee osteoarthritis: a randomized controlled trial. Phys Sportsmed. 2010;38(2):19-28. 34. Herndon C. Topical delivery of nonsteroidal anti-inflammatory drugs for osteoarthritis. J Pain Palliat Care. 2012;26:18-23. 35. Mick G, Correa-Illanes G. Topical pain management with 5% lidocaine medicated plaster-a review. Curr Med Res Opin. 2012;28(6):937-951. 36. Salliant G. Study comparing the efficacy and tolerability of Flector tissugel to that of placebo in the treatment of benign ankle sprain. Sports Med. 1998;72:1-5. 37. Galer B. Rowbotham M, Perander J, et al. Topical diclofenac patch relieves minor sports injury pain: Results from a multicenter con- trolled clinical trial. J Pain Symptom Manage. 2000;19:287-294. Suggested Reading Chang Chien G. Mathur S, Harvey R, Harden N. Topical diclofe- nac treatment for post-incisional neuropathic pain. Pain Med. 2013;14:950-951. McCleane G. Topical application of analgesics: a clinical option in day case anesthesia. Curr Opin Anesthesiol. 2010;23:704-707. PAIN ME DICINE NE WS S P E CIAL E DITI ON 63 Copyright© 2014 M cM ahon Publishing G roup unless otherw ise noted. A llrights reserved.Reproduction in w hole orin partw ithoutperm ission is prohibited.
