EPIDEMIOLOGY OF DIPTHERIA
- 1. p
- 2. EPIDEMIOLOGY OF DIPHTHERIA DR. MAHESWARI JAIKUMAR. maheswarijaikumar2103@gmail.com
- 3. DIPHTHERIA • Is an acute infectious disease caused by toxigenic strains of Cornybacterium diphtheriae.
- 4. • The bacilli multiply locally, usually in the throat, and elaborate a powerful exotoxin which is responsible for the following pathology.
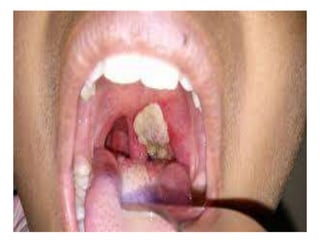
- 5. • The formation of grayish or yellowish membrane (false membrane) commonly over the tonsils, pharynx, with well defined edges and the membrane cannot be wiped away.
- 6. • Marked congestion, edema or local tissue destruction. • Enlargement of the regional lymph nodes. • Signs and symptoms of toxemia.
- 8. AGENT
- 11. • The causative agent, C diphtheriae is a gram-positive, non motile organism. • It has no invasive power, but produces a powerful exotoxin which can affect the heart leading to myocarditis.
- 12. • Four types of Diphtheria bacilli are differentiated. • gravis, mitis, belfanti and intermedius, all pathogenic to man.
- 13. SOURCE OF INFECTION • The source of infection may be a case or a carrier.
- 14. CASE • Cases range from subclinical infection to frank clinical cases. • Mild or silent infections may exhibit no more than a mere running nose or sore throat. These cases pose more threat in the spread than the active cases.
- 15. CARRIER • Carriers are common sources of infection. • Carriers may be temporary or chronic nasal or throat carriers.
- 16. INFECTIVE MATERIAL • Nasopharyngeal secretions, discharges from skin lesions, contaminated fomites and possibly infected dust.
- 17. INFECTIVITY • The period of infectivity may vary from 14 to 28 days from the onset of the disease. • But carriers may remain infective for much longer periods.
- 18. • A case or a carrier may be considered non communicable, when at least 2 cultures properly obtained from nose and throat, 24 hours apart are negative for diphtheria bacilli.
- 19. HOST FACTORS • AGE : Diphtheria particularly affects children (1-5 yrs). • GENDER : Both genders are affected.
- 20. IMMUNITY • Infants born of immune mothers are relatively immune during the first few months of life. • Children in developing countries seem to acquire active immunity through active infection.
- 22. • Case of diphtheria occur in all seasons, although winter months favour its spread.
- 23. MODE OF TRANSMISSION • The disease is spread mainly by droplet infection. • It can also be transmitted directly to susceptible persons from infected cutaneous lesions.
- 24. • Transmission by objects (cups, thermometers, toys, pencils) contaminated by the nasopharyngeal secretions of the patients is possible, but only for short periods.
- 25. PORTAL OF ENTRY • RESPIRATORY ROUTE : Commonly the portal of entry is the respiratory tract. • NON RESPIRATORY ROUTE : The portal of entry sometimes may be the skin where cuts, wounds and ulcers not properly attended to, may get infected with diphtheria bacilli.(umbilical cord)
- 26. INCUBATION PERIOD • 2 To 6 days. • Occasionally longer.
- 27. CLINICAL FEATURE • Respiratory tract forms of diphtheria consists of pharygotonsillar, larygotonsillar, nasal and combinations thereof.
- 28. • Patients with pharyngotonsillar diphtheria usually have a sore throat, difficulty in swallowing and low grade fever at presentation.
- 29. • Examination of the throat may show only mild erythema, localized exudate or a pseudomembrane.
- 30. PSEUDOMEMBRANE
- 31. • The membrane may be a localized patch of the posterior pharynx or tonsil, may cover the entire tonsil, or less frequently, may spread to cover the soft palates and the posterior portion of the pharynx.
- 34. • In the early stage the pseudo- membrane may be whitish and may wipe off easily. • The membrane may extend to become thick, blue-white to grey-black and adherent.
- 35. • Attempts to remove the membrane may result in bleeding. • A minimal area of mucosal erythema surrounds the membrane.
- 36. • Patients with severe disease may have marked edema of the sub mandibular area and the antererior portion of the neck, along with lymphadenopathy, giving a characteristic “bull- necked” appearance.
- 38. • Laryngeotracheal diphtheria is most often preceded by pharygotonsillar disease, usually is associated with fever, hoarseness and croupy cough at presentation.
- 39. • If the infection extends into the bronchial tree, it is the most severe of disease. • Initially it may be clinically indistinguishable from viral croup or epiglottitis.
- 40. • Prostration and dyspnoea soon follow because of the obstruction caused by the membrane. • This obstruction may even cause suffocation if not promptly relieved by intubation or tracheostomy.
- 41. • The diphtheria bacilli within the membrane continue to produce toxin actively.
- 42. • This is absorbed and results in distant toxic damage, particularly paranchymatous degeneration, fatty infiltration and necrosis in heart muscle, liver, kidneys and adrenals and some time accompanied by gross hemorrhage.
- 43. • Irregularities of the cardiac rhythm indicate damage to the heart. • Later there may be difficulties with vision, speech, swallowing, or movement of the arms or legs.
- 44. • The toxin also produces nerve damage, resulting in paralysis of the soft palate, eye muscles or extremities. • Patients who survive complications recover completely.
- 45. • Nasal diphtheria, the mildest form of respiratory diphtheria, usually is localized to the septum or turbinates of one side of the nose. • Occasionally a membrane mat extend into pharynx.
- 46. • Non respiratory mucosal surface i.e., the conjunctivae and genitals may also be sites of infection. • Cutaneous form of diphtheria is common in tropical areas.
- 47. • Cutaneous diphtheria appears as a secondary infection of a previous skin abrasion or infection. • The presenting lesion, often an ulcer, may be surrounded by erythema and covered with a membrane.
- 48. • Patients generally seek treatment because of the chronicity of the skin lesion.
- 49. CONTROL OF DIPHTHERIA (Cases & Controls)
- 50. EARLY DETECTION • An active search for cases and carriers should start immediately amongst family and school contacts. • Carriers can be detected only by culture method.
- 51. • Swabs should be taken from both the nose and throat and examined by culture methods for diphtheria bacilli. • Test should be made for the virulence of the organism.
- 52. ISOLATION • All cases, suspected cases and carriers should be promptly isolated, preferably in a hospital, for at least 14 days or until proved free of infection.
- 53. • At least 2 consecutive nose and throat swabs , taken 24 hrs apart, should be negative before terminating isolation.
- 54. TREATMENT (CASES) • When diphtheria is suspected, diphtheria antitoxin should be given without delay, IM or IV , in doses ranging from 20,000 to 100,000 units or more, depending on the severity of the case following a test dose of 0.2ml subcutaneously to detect sensitization to horse serum.
- 55. • For mild early pharyngeal of laryngeal disease the dose is 20,000-40,000 units. • For moderate nasopharyngeal disease, 40,000-60,000 units is administered.
- 56. • For severe, extensive or late (3 days or more) disease, 80,000- 100,000 units. • In addition to anti toxin every case should be treated with penicillin or erythromycin for 5 to 6 days to clear the throat of C. diphtheriae (this decreases toxin production)
- 57. CARRIERS • The carriers should be treated with 10 day course of oral erythromycin, which is the most effective drug for the treatment of carriers. • The immunity status should be upgraded as follows.
- 58. CONTACTS • Contacts merits special attention. They should be throat swabbed and their immunity status determined.
- 59. • Non immunized close contact should receive prophylactic penicillin or erythromycin. (1000-2000 units of diphtheria antitoxin and actively immunized against diphtheria).
- 60. • Contacts should be under medical surveillance and examined daily for evidence of diphtheria for at least a week after exposure.
- 61. COMMUNITY • Effective control measure is by active immunization with diphtheria toxoid of all infants as early in life as possible (national immunization schedule).
- 62. • Subsequent booster doses every 10 years there after. • Immunization does not prevent the carrier state.
- 64. DPT VACCINE • It is a combined vaccine. • The preparation of choice is DPT, because it can be immunized simultaneously against three diseases, viz., Diphtheria, pertussis, and tetanus.
- 66. • There are two types of vaccine : plain and adsorbed. • Adsorption is usually out on a mineral carrier like aluminum phosphate or hydroxide.
- 67. • Adsorption increases immunological effectiveness of the vaccine. • WHO recommends the use of adsorbed vaccines.
- 68. DPT STORAGE • DPT/DT vaccine should not be frozen. • They should be stored in a refrigerator between 2 to 8 degree Celsius.
- 69. • The vaccine should be used before the date of expiry indicated on the vial. • The vaccine will lose it’s potency if it is kept in room temperature over a long period of time.
- 70. OPTIMUM AGE • Young infants respond well to immunization with potent vaccines and toxoids, even in the presence of low to moderate levels of maternal antibodies.
- 71. • The Expanded programme of Immunization has recommended that DPT vaccine can be safely and effectively administered as early as 6 weeks after birth.
- 72. NUMBER OF DOSES • Three doses of DPT each of which is usually 0.5ml, should be considered optimal for primary immunization.
- 73. INTERVAL BETWEEN DOSES • The current recommendation is to allow an interval of 4 weeks between 3 doses, with a booster injection at one and a half years or two years, followed by another booster (DT only)at the age of 5 to 6 years.
- 74. MODE OF ADMINISTRATION • All vaccines containing mineral carriers or adjuvants should be injected deep intramuscular. • This applies to DPT also.
- 75. • DPT is given in the upper and outer quadrant of the gluteal region. • For children under one year of age, DPT should be administered in (lateral aspect) of the thigh. (1984 Global Advisory Group).
- 76. • The most severe complications that could follow DPT immunization are encephalitis, encephalopathy, prolonged convulsions, infantile spasms and Reye’s syndrome.
- 77. CONTRAINDICATIONS • Minor conditions such as cough, cold, mild fever are not contraindications. • Seriously ill children are not vaccinated.
- 78. • DPT should not be repeated if a severe reaction occurred after a previous dose.
- 79. • Such reactions include collapse, shock like state, persistent screaming episodes, temperature above 40 degree Celsius, convulsions and other neurological symptoms.
- 80. • DT only is recommended in such case. (2 doses with 4 weeks apart with a booster dose 6 months to one year). • Children who have received DPT earlier, should receive only DT as booster at 5-6 years or at school entry.
- 82. ANTISERA Diphtheria antitoxin prepared in horse serum is still the mainstay of passive prophylaxis and also for treatment of diphtheria.
- 84. THANK YOU
