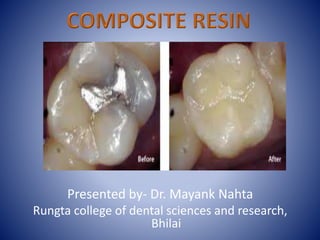
Dental Composite Materials: Classification, Composition and Polymerization
- 1. Presented by- Dr. Mayank Nahta Rungta college of dental sciences and research, Bhilai
- 2. CONTENT • INTRODUCTION • HISTORY • USES • CLASSIFICATION • COMPOSITION
- 3. INTRODUCTION • They are highly crosslinked polymeric materials reinforced by a dispersion of glass,crystalline or resin filler particles or short fibres bound to the matrix by silane coupling agents. • It may be defined as a system composed of a mixture of two or more macromolecule which are essentially insoluble in each other and differ in form .
- 4. History • In 1962 Dr. Ray Bowen developed a new type of material known as composite resin. The main innovation was a resin matrix of Bisphenol-A-Glycidyl Methacrylate (Bis-GMA) and a fillers agents. (silica,quartz,glass). Dr. Ray Bowen
- 5. Composite restorative materials Uses- Restoration of anterior and posterior teeth Used as a veneers material. To bulid up cores Cementation of orthodontic brackets,maryland bridges,ceramic crowns,inlays ,onlays,laminates Pit and fissure sealants Repair of chipped porcelain restorations
- 6. Classification 1.Based on polymerization method • Self cured. • light cured,UV light cured ,Visible light cured • Dual light cured. • 2. According to Anusavice (Phillips) Based on size of filler particles- • Conventional 8-12 um • Small particle 1-5 um • Microfilled 0.04-0.4 um • Hybrid 0.6-1.0 um
- 7. 3.Acco. To Marzoak 6 generations of composites:- •First generation of composite •Second generation of composite •Third generation of composite •Fourth generation of composite •Fifth generation of composite •Sixth generation of composite 4. Based on matrix composition Bis-GMA UDMA Bis-EMA TEGDMA Other resin
- 8. 5) Based on Radiopacity •Radiopaque Glasses with barium, strontium, or lithium Ytterbium fluoride (YF3) •Not radiopaque •2 paste system -base & reactor. Chemically activated •Single paste & liquid -chemically cured. •Single paste system -supplied in syringes. Light activated. •Disposable capsules -compomers 6 ) Based on mode of supply :
- 9. 7)According to Graham J. Mount; W.R. Hume : T ype 1 - Macrofilled composite resin T ype 2 - Microfilled composites resin Type 3 – hybrid composite resin 8)Based on viscosity Flowable composites. Medium viscosity composites. Packable composites 9).Classification based on area used Anterior composite Posterior composite
- 10. 10). Classification according to Bayne and Heyman: •Megafill-1-2µm •Macrofill-10-100µm •Midifill-1-10µm •Minifill-.01-.1µm. •Microfill -0.04-0.4µm •Nanofill-.005-.01µm
- 11. Midi -filler - 2 um (beachball) Mini -filler - 0.1 um (canteloupe) Nanofiller - .02 um (pea) Microfiller - .04 um (marble) Relative Particle Sizes (not to scale)
- 12. Composition RESIN MATRIX FILLER PARTICLES COUPLING AGENT THEY ALSO CONTAIN: HYDROQUINONE U.V ABSORBER OPACIFIER COLOUR PIGMENT
- 13. Resin matrix • BIS-GMA resin is the base for composite. Diluents are added to increase flow and handling characteristics or provide cross linking for improved strength. Common examples are: • RESIN:- BIS-GMA bisphenol glycidylmethacrylate • DILUENTS:- MMA methylmethacrylate BIS-DMA bisphenol dimethacrylate UDMA urethane dimethacrylate • CROSS LINK DILUENTS TEGDMA triethylene glycol dimethacrylate EGDMA ethylene glycol dimethacrylate
- 14. FILLERS •Silica particles •Quartz •Glass ( Ba, Sr, Zr) If the composite is made up of the resin matrix AND fillers, it is called Filled Resin
- 15. (1) reinforcement of the matrix resin, resulting in increased hardness, strength, and decreased wear (2) reduction in polymerization shrinkage (3) reduction in thermal expansion and contraction (4) improved workability by increasing viscosity (5) reduction in water sorption, softening, and staining (6) increased radiopacity Benefits of fillers-
- 16. • Ground quartz- Makes restoration difficult to polish and cause abrasion of opposing teeth and restorations • Colloidal silica— Used in microfilled composites Thicken the resin • Glasses of ceramic containing heavy metals Radiopacity eg.Barium Types of fillers used-
- 17. Coupling Agent • Chemical bond – filler particle - resin matrix • transfers stresses • Organosilane (bifunctional molecule) – siloxane end bonds to hydroxyl groups on filler – methacrylate end polymerizes with resin CH3-C-C-O-CH2-CH2-CH2-Si-OH CH2 O OH OH Bonds with filler Silane Bis-GMA Bonds with resin Phillip’s Science of Dental Materials 2003
- 18. Inhibitors • Prevents spontaneous polymer formation – heat – light • Extends shelf life • Butylated Hydroxytoluene Phillip’s Science of Dental Materials 2003
- 19. Pigments and UV Absorbers • Pigments – metal oxides • provide shading and opacity • titanium and aluminum oxides • UV absorbers – prevent discoloration – acts like a “sunscreen” • Benzophenone Phillip’s Science of Dental Materials 2003
- 20. Visible-Light Activation • Camphorquinone – most common photoinitiator • absorbs blue light – 400 - 500 nm range • Initiator reacts with amine activator • Forms free radicals • Initiates addition polymerization OCH2CHCH2O-C-C=CH2CH2=C-C-O-CH2CH-CH2O -C- CH3 CH3 CH3 CH3OH OH O O Bis-GMA
- 21. Polymerization mechanism 1. Chemically activated 2. Light-activated
- 22. Two paste system Base paste – benzoyl peroxide initiator Catalyst paste– tertiary amine activator (N,N-dimethyl-p-toludine) 1.Chemically activated composite system
- 23. • Earliest system---UV light activated system • Limitations – Limited penetration of light into resin Lack of penetration through tooth structure 2.Light activated composite resins—
- 24. Visible light activated system--- • Single paste system • Photoinitiator – Camphoroquinone • Amine accelerator – diethyl-amino-ethyl-methacrylate
- 25. Types of lamps used for curing LED lamps. Using a solid-state, electronic process, these light sources emit radiation only in the blue part of the visible spectrum between 440 and 480 nm QTH lamps. QTH lamps have a quartz bulb with a tungsten filament that irradiates both LTV and white light that must be filtered to remove heat and all wavelengths except those in the violet-blue range (400 to 500 nm).
- 26. PAC lamps. PAC lamps use a xenon gas that is ionized to produce a plasma. The high-intensity white light is filtered to remove heat and to allow blue light (400 to 500 nm) to be emitted. Argon laser lamps- have the highest intensity and emit at a single wave length.lamps currently avaialble emit 490 nm
- 27. •Consists of 2 light curable pastes Benzoperioxide and aromatic tertiary amine •Light curing – promoted by amine/CQ combination •Chemical- amine/BPO interaction APPLICATION: •Cementation of bulky ceramic inlays Dual Cure
- 28. High intensity curing • High intensity lamps could provide savings in chair time. • However high intensity, short exposure times cause accelerated rates of curing, which leads to substantial residual stress build up.
- 29. Depth of cure and exposure time • Light absorption and scattering in resin composites reduces the power density and degree of conversion (DC) with depth of penetration • Intensity can be reduced by a factor of 10 to 100 in a 2-mm thick layer of composite which reduces monomer conversion to an accceptable level. • The practical consequence is that curing depth is limited to 2- 3mm • Light attenuation vary from one type of composite to other depending on opacity,filler size,filler concentration and pigment shade
- 30. • Darker shades require long curing time • When polymerising resin through tooth structure exposure time should be increased by a factor of 2 – 3 to compensate for reduction in light intensity • For halogen lamps light intensity can decrease depending on quality and age of light source,orientation of light tip,distance between light tip and restoration and presence of contamination,such as composite residue on light tip • Despite the many advantages of light cured resins,there is still need for chemically cured composites for eg chemicaly cured materials can be used with reliable results as luting agent under metallic restorations.
- 31. Polymerization • Initiation – production of reactive free radicals • typically with light for restorative materials • Propagation – hundreds of monomer units – polymer network – 50 – 60% degree of conversion • Termination Craig Restorative Dental Materials 2002
- 32. C= C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C=C C= C C= C C= CC= C C= C C= C C= C C=C C=C C=C C=C C= C C= C polymeriza tion Ferraca ne
- 33. Degree of conversion • DC is a measure of percentage of carbon-carbon double bonds that have been converted to single bonds to form polymeric resin • The higher the DC the better the strength,wear,resistance • Conversion values of 50%-70% are achieved at room temperature for both types of curing system
- 34. Polymerization Shrinkage Composites exhibit shrinkage while hardening. More common when the restoration has extended onto root surface results in gap formation. Most imp regarding the effects of polymerization shrinkage is C-factor.
- 35. C--FACTOR The C-factor is the ratio of bonded (flow-inactive) to unbonded or free (flow- active) surfaces. The ratio of the restorations bonded to unbonded ( free) surfaces. C=BONDED WALLS/UNBONDED WALLS
- 36. Higher the C-factor , greater is the potential for bond disruption from polymerization effects. Class IV with C-factor 0.2 is at low risk compared to class I with C-factor 5 is at high risk.
- 37. Incremental buildup and cavity configuration • One technique is the attempt to reduce the so called C- factor(configuration factor) which is related to the cavity preparation geometry • A layering technique in which restoration is built up in increments , reduces polymerization stress by minimising the Cfactor. • Incremental technique overcomes both limited depth of cure and residual stress concentration.
- 39. Conventional / traditional /macrofilled composite • Composition- Ground quartz most commonly used filler Average size : 8- 12 µm Filler loading - 70-80 weight % or 50 – 60 vol %
- 40. Properties • Compressive strength- Four to five times greater than that of unfilled resins ( 250-300 Mpa) • Tensile strength- Double than of unfilled acrylic resins (50 – 65 Mpa) • Elastic modulus- Four to six times greater (8-15 Gpa) • Hardness – Considerably greater (55 KHN) than that of unfilled resins • Coefficient of thermal expansion- High filler –resin ratio reduces the CTE significantly.
- 41. • Esthetics – Polishing result in rough surface Selective wear of softer resin matrix Tendency to stain • Radiopacity – Composites using quartz as filler are radioluscent Radiopacity less than dentin
- 42. • Clinical considerations- Polishing was difficult Poor resistance to occlusal wear Tendency to discolor Rough surface tends to stain Inferior for posterior restorations
- 43. Microfilled composites Developed to overcome surface roughness of conventional composites Composition- Smoother surface is due to the incorporation of microfillers. Colloidal silica is used as the microfiller 200—300 times smaller than the average particle in traditional composites Filler particles consists of pulverized composite filler particles
- 44. Properties • Inferior physical and mechanical properties to those of traditional composites • 40 – 80 % of the restorative material is made up of resin • Increased surface smoothness • Areas of proximal contact- Tooth drifting .
- 45. Compressive strength- 250- 350 Mpa. Tensile strength- 30- 50 Mpa. Lowest among composites Hardness – 25- 30 KHN. Thermal Expansion Coefficient- highest among composite resins
- 46. Clinical considerations • Choice of restoration for anterior teeth. • Greater potential for fracture in class 4 and class 2 restorations. • Chipping occurs at margins.
- 47. Small particle composite • Introduced in an attempt to have good surface smoothness and to improve physical and mechanical properties of conventional composites. Composition – Smaller size fillers used- Colloidal silica - present in small amounts ( 5 wt % ) to adjust paste viscosity Heavy metal glasses . Ground quartz also used Filler content 65 – 70 vol % or 80 – 90 %
- 48. Properties • Due to higher filler content the best physical and mechanical properties are observed • Compressive strength- Highest compressive strength (350 – 400 Mpa ) • Tensile strength- Double that of microfilled and 1.5 times greater than that of traditional composites ( 75- 90 Mpa )
- 49. • Hardness – Similar to conventional composites ( 50 – 60 KHN) • Thermal expansion coefficient- Twice that of tooth structure • Esthetics – Better surface smoothness than conventional because of small and highly packed fillers • Radiopacity – Composites containing heavy metal glasses as fillers are radio-opaque which is an important property in restoration of posterior teeth
- 50. Clinical considerations • In stress bearing areas such as class 4 and class 2 restorations • Resin of choice for aesthetic restoration of anterior teeth • For restoring sub gingival areas
- 51. Hybrid composite • Developed in an effort to obtain even better surface smoothness than that provided by the small particle composite. • Composition – 2 kinds of fillers- Colloidal silica –present in higher concentrations 10 – 20 wt % Heavy metal glasses – Constituting 75 % Average particle size 0.4 – 1.0 µm
- 52. Properties • Range between conventional and small particle • Superior to microfilled composites • Compressive strength- Slightly less than that of small particle composite(300 – 350 Mpa ) • Tensile strength- Comparable to small particle (70 – 90 Mpa ) • Hardness – Similar to small particle ( 50 – 60 KHN )
- 53. • Esthetics – Competitive with microfilled composite for anterior restoration • Radiopacity – Presence of heavy metal glasses makes the hybrid more radio-opaque than enamel
- 54. Clinical considerations • Used for anterior restorations including class 4 because of its smooth surface and good strength • Widely employed for stress bearing restorations
- 55. Flowable composites • Modification of SPF and Hybrid composites. • Reduced filler level • Clinical considerations- Class 1 restorations in gingival areas. Class 2 posterior restorations where acess is difficult. Fissure sealants.
- 56. Composites for posterior restorations • Amalgam choice of restoration for posterior teeth • Mercury toxicity and increased esthetic demand. • All types of composites except flowable composites • Conservative cavity preparation • Meticulous manipulation technique.