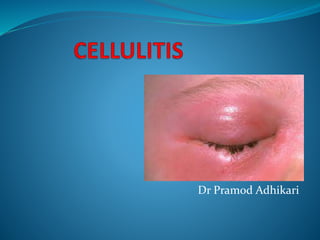
CELLULITIS superficial bacterial infection.pptx
- 3. BACTERIA CAUSES CELLULITIS STAPHYLOCOCCUS AUREUS. STREPTOCOCCUS PYOGENS
- 6. Investigation CBC RBS PUS C/S
- 7. Treatment Analgesic : flexon 1 tab PO TID/SOS or T. ketorol 1 tab TID/SOS or PPI: T. pantop 40 mg/ T. Aciloc 150mg PO BD Antibiotics: Oral: T.Flucloxacillin 500mg PO QID for 7 days / or T. clavum 625mg (Amixycillin and potassium clavulanate) IV: Inj ceftriaxone 1gm iv BD in sever case/ or inj cefazolin 1gm iv BD
- 12. SECONDARY SKIN LESIONS: PUSTULES:It is a bulging patch of skin that’s full of yellowish fluid called pus.eg:acne
- 13. 1)pustules
- 14. CRUSTING
- 15. SCALES
- 16. EXCORIATION
- 20. BACTERIAL INFECTION OF SKIN IMPETIGO FURUNCULOSIS BOILS
- 21. IMPETIGO
- 31. Carbuncle is an infective gangrene of the subcutaneous tissue, which often occurs in the nape of the neck. The subcutaneous tissue become painful and indurated and the overlying skin is red. If not properly treated areas of softening appear, the skin sloughs and discharges pus. Usually there is one central large slough, surrounded by a ‘rosette’ of smaller area of necrosis. Carbuncle
- 33. Site: Nape of the neck Upper part of the back Susceptible group: Diabetic pt Male person Age > 40 yrs Chronic illness Immuno- compromised person Complication: Septicaemia Epidural abscess Meningitis
- 34. Clinical feature: - Uncommon before 40 yrs - M > F - Common in diabetic pt - Skin- red, indurated - Subcutaneous tissue – painful, indurated - Slough out of skin - Multiple discharging sinus Investigations: - CBC - Blood sugar - Urine sugar
- 35. Treatment: - I&D of pus and excision of all dead tissue - Control of DM - Antibiotics to control infection - Regular local wound care- Dressing at regular interval - Improvement of general condition - If required, skin graft after formation of granulation tissue Why nape of the neck is common site - Less vascular area - Lax and extensive tissue planes
- 36. Boil Boil is defined as an acute staphylococcal infection of the hair follicles which usually proceeds to suppuration an central necrosis. It is most common surgical infection. Pathogenesis: Orifices of hair become blocked by keratin or sebum plug contents become infected by staphylococcus leading to inflammation suppuration and subsequent necrosis Boil is formed
- 37. Risk factor Susceptible group: Debilitated pt with chr: illness Anxious & worried people DM The most common places for boils to appear are on the face, neck, armpits, shoulders, and buttocks.
- 38. Sign and symptoms A boil starts as a hard, red, painful lump usually about half an inch in size. Over the next few days, the lump becomes softer, larger, and more painful. These are the signs of a severe infection: The skin around the boil becomes infected. It turns red, painful, warm, and swollen. More boils may appear around the original one. A fever may develop. Lymph nodes may become swollen.
- 39. Complication 1. Cellulitis 2. Secondary boil 3. Abscess 4. Secondary infection of draining L.N 5. Carbuncle.(infective gangrene of the subcutaneous tissue)
- 40. Treatment Improving of the general condition of the pt Proper antibiotics according to C/S Washing of the surrounding skin with antiseptic solution. Keep the skin clean and dry Topical antibiotic: neomycin, mupirocin etc. - IV broad spectrum antibiotics such as Cefuroxime, Ceftriaxone combined with metronidazole
- 41. Preventing Measures Help prevent by following these guidelines: Carefully wash clothes, bedding, and towels of a family member who is infected with boils/ furunculs. Clean and treat minor skin wounds. Practice good personal hygiene. Stay as healthy as possible.
- 42. Contamination of pathogen Due to inappropriate hand washing measure such as not using anti septic hand wash. Improper sterilization of hospital equipments, such as dressing set, towels. Untidy environment surrounding health post. Improper waste management. Improper sanitation disposabale management.
- 43. Health education HYGEINE: -keep the wound clean and dry. -change the clothes daily. -need to take daily shower. NUTRITION: -Eat high protein diet(meat,fish) and fruits. -Avoid alcohal ,smoking, and sugar contained foods. -
- 44. Furunculosis Furunculosis is a deep infection of the hair follicle leading to abscess formation with accumulation of pus and necrotic tissue. Cause It appear on the hair-bearing parts of the skin and the infectious agent is Staphylococcus aureus.
- 45. Have a Good Day
- 46. FUNGAL INFECTION OF SKIN
- 49. Risk factor for fungal infection Sweating heavily. Living in warm or wet environment. Not keeping your skin clean and dry. Sharing items like clothes,shoes,towels or bedding items. Wearing tight clothing or footwear that doesn’t breathe well. Taing part in activities that involve frequesnt skin to skin contact. Coming into contact with animals that may be infected. Having a weakened immune system due to immune suppressant drugs,cancer treatment or condition such as HIV.
- 66. Clinical features Affected site looks typically yellow, brown. Affected nail easily brittle or break. Nail become thick then normal nail
- 72. Prevention of fungal infection Be sure to practice good hygiene. Never share clothes,towels,or any other personal items. Wear clean clothes every day particularly socks and underwear. Choose the clothes that fit properly in your body. Avoid clothes or shoes that are too tight or have restrictive fit. Make sure every clothes dry off properly in the sunlight. Wipe down shared surfaces such as gym equipments or mats. Stay away from animals that have signs of fungal infection such as missing fur or frequent scratching.
- 73. Indication of referal Recurrent symptoms after primary treatments. Fungal infection on immunocompromised patient such as HIV. Secondary skin infection.
- 75. Causes Pityriasis versicoclor is caused by type of yeast called Malassezia. This yeast is found on the skin of more than 90%.
- 77. Investigation Wood lamp (black light) examination. Microscopy using potassium hydroxide (KOH) Skin biopsy.
- 78. Treatment