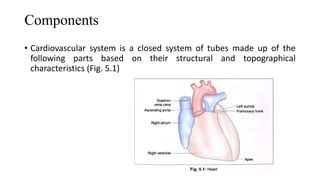
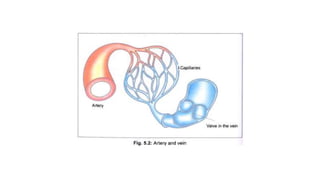
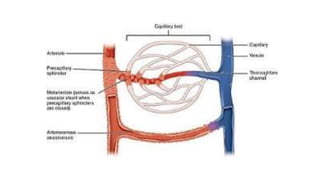
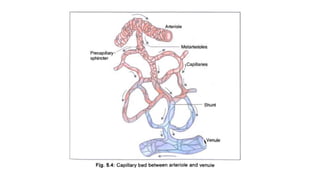
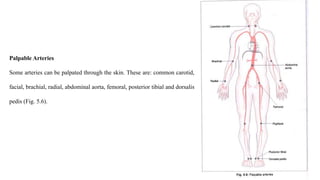
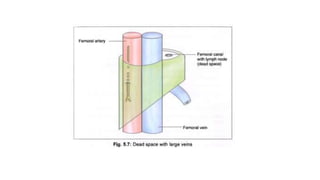
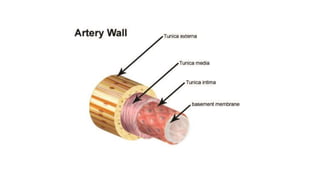
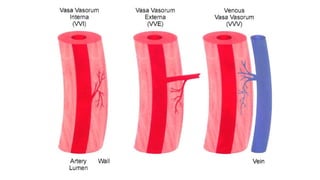
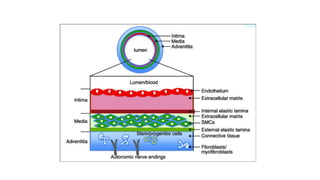
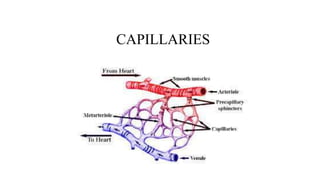
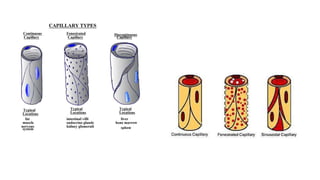
The cardiovascular system consists of the heart, arteries, veins, and capillaries. The heart pumps blood through arteries, which branch into smaller vessels and eventually capillaries where nutrients and waste are exchanged. Capillaries then drain into veins which collect blood and return it to the heart. The cardiovascular system transports blood throughout the body in two circuits - systemic circulation from the heart to the body and pulmonary circulation from the heart to the lungs.