This document summarizes strategies for improving outcomes in ICU patients receiving sedation, including:
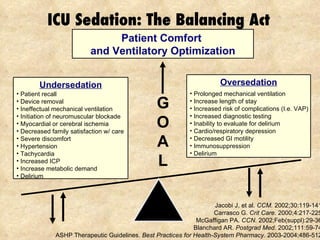
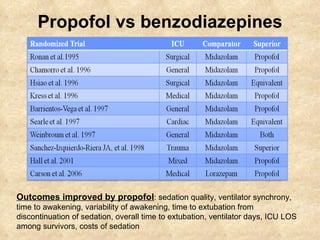
1) Using analgesia-first sedation and targeting light sedation to minimize risks of oversedation like longer duration of mechanical ventilation.
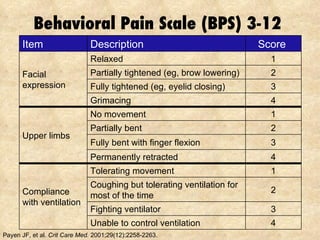
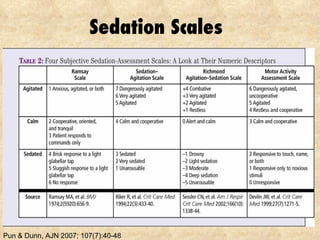
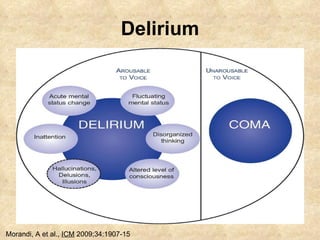
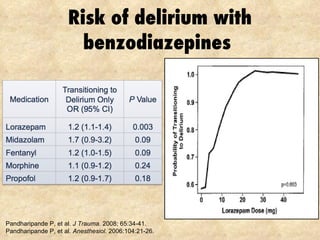
2) Regularly assessing sedation levels and pain to guide treatment. Non-benzodiazepine sedatives like dexmedetomidine may reduce risks of delirium.
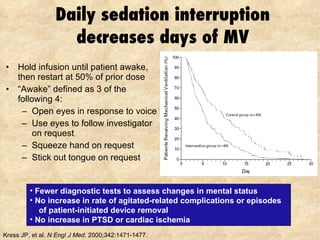
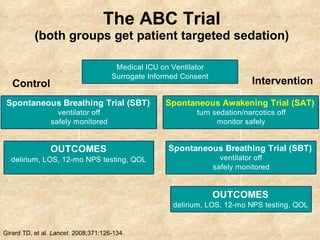
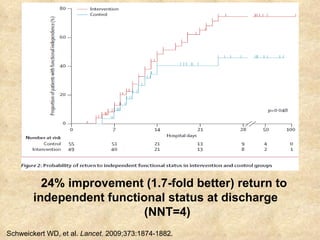
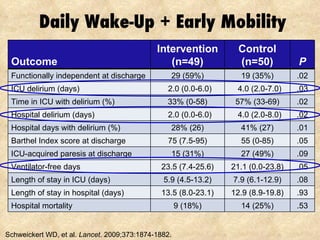
3) Daily sedation interruption or awakening trials combined with early mobility can decrease duration of mechanical ventilation and length of stay.








































![Educational Delirium Website www.ICUdelirium.org [email_address] [email_address]](https://image.slidesharecdn.com/bogotasedation052110-100724183319-phpapp01/85/Bogota-sedation052110-53-320.jpg)