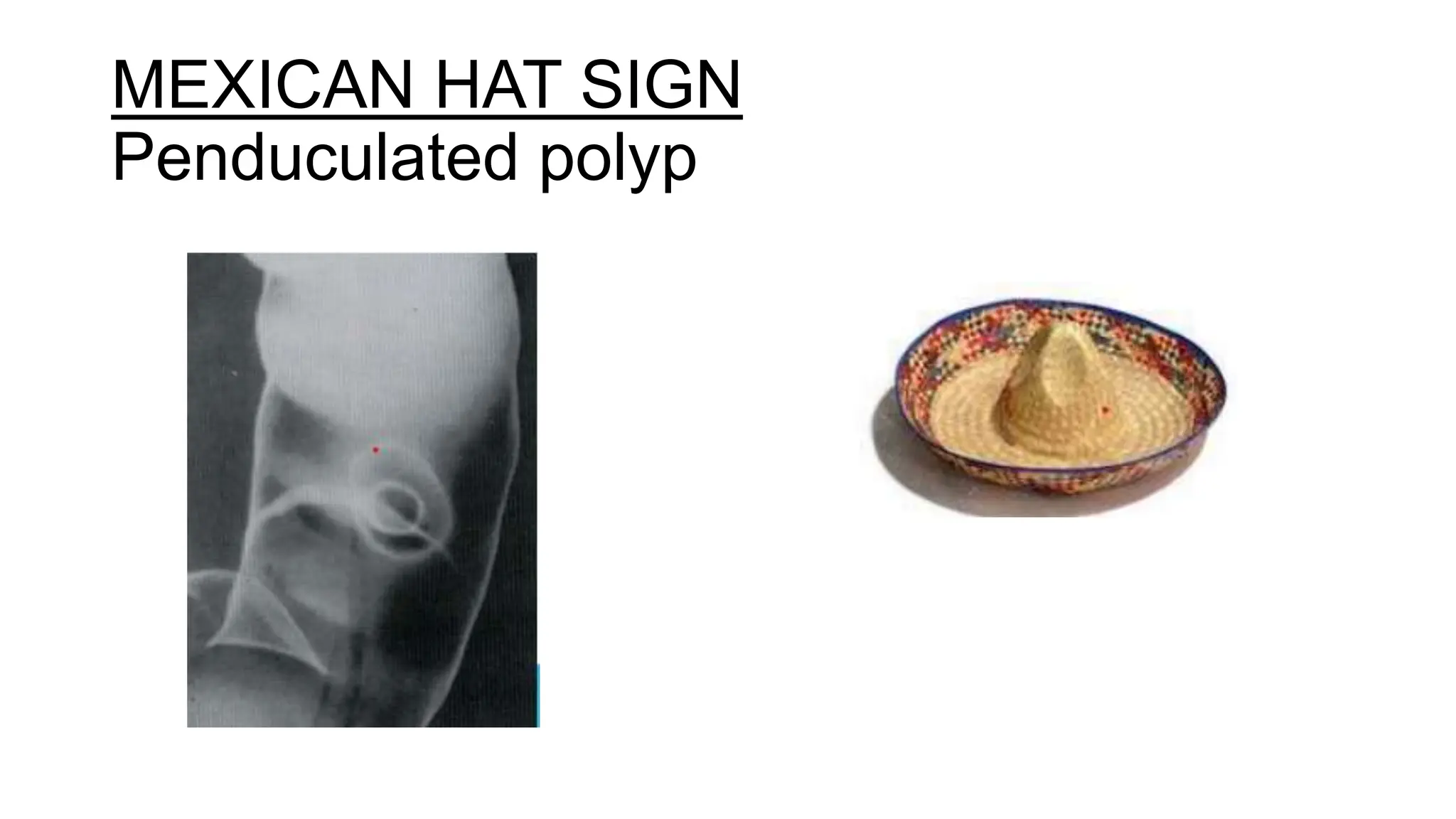
A barium enema involves inserting barium sulfate into the rectum to coat and image the lining of the large intestine. It has advantages over other contrast agents by providing better mucosal detail due to barium's inability to be absorbed. Potential adverse effects include chemical peritonitis and barium embolisms. Proper bowel preparation and catheter placement are important for successful double contrast barium enemas, which allow clearer visualization compared to single contrast exams. Findings may reveal diverticula, polyps, inflammatory conditions, or cancers appearing as characteristic signs.