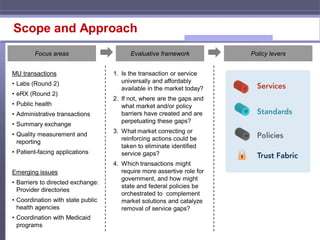
The document outlines an agenda and proposed next steps for the Information Exchange Workgroup. Key points include:
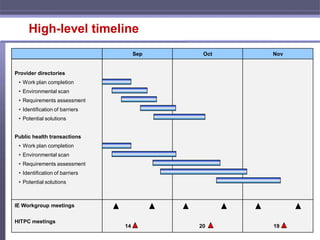
- Establishing two task forces focused on provider directories and public health transactions.
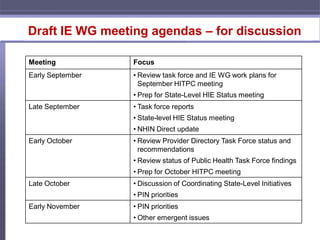
- Developing work plans and timelines for each task force to assess current issues, identify barriers, and make recommendations.
- Prioritizing initial areas like laboratory results, electronic prescribing, and patient summary exchange in relation to Meaningful Use.
- Coordinating activities with the HIT Policy Committee and ensuring alignment with other national health IT initiatives.
The workgroup aims to address specific challenges to information exchange and make policy recommendations to facilitate interoperability goals.