3. monitoring & devices used in icu ccu
- 1. MONITORING & DEVICES USED IN ICU 1 Prof. Dr. RS Mehta, BPKIHS
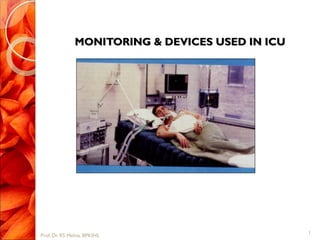
- 2. INTRODUCTION Intensive care unit (ICU) equipment includes patient monitoring, respiratory and cardiac support, pain management, emergency resuscitation devices, and other life support equipment . 2 Prof. Dr. RS Mehta, BPKIHS
- 3. Contd… They are designed to care for patients who are seriously injured, have a critical or life-threatening illness, or have undergone a major surgical procedure thereby requiring 24-hour care and monitoring. 3 Prof. Dr. RS Mehta, BPKIHS
- 4. PURPOSE An ICU may be designed and equipped to provide care to patients with a range of conditions, or it may be designed and equipped to provide specialized care to patients with specific conditions. 4 Prof. Dr. RS Mehta, BPKIHS
- 5. Contd… Neuromedical ICU cares for patients with acute conditions involving the nervous system or patients who have just had neurosurgical procedures and require equipment for monitoring and assessing the brain and spinal cord. 5 Prof. Dr. RS Mehta, BPKIHS
- 6. Contd… A neonatal ICU is designed and equipped to care for infants who are ill, born prematurely, or have a condition requiring constant monitoring. A trauma/burn ICU provides specialized injury and wound care for patients involved in auto accidents and patients who have gunshot injuries or burns. 6 Prof. Dr. RS Mehta, BPKIHS
- 7. 7 Prof. Dr. RS Mehta, BPKIHS
- 8. TYPES OF DEVICES Intensive care unit equipment includes Patient monitoring devices Life support and emergency resuscitation devices, and Diagnostic devices. 8 Prof. Dr. RS Mehta, BPKIHS
- 9. PATIENT MONITORING EQUIPMENT Arterial line Bed side monitor Blood pressure device (sphygmomanometer) Blood pressure monitor Electrocardiograph(ECG or EKG machine) Electroencephalograph(EEG machine) Intracranial pressure monitor Pulse Oximeter Glucometer 9 Prof. Dr. RS Mehta, BPKIHS
- 10. LIFE SUPPORT AND EMERGENCY RESUSCITATION DEVICES MechanicalVentilator Laryngoscope Airway Infusion pump Crash cart(Resuscitation cart) Intra aortic ballon pump Continuous positive air pressure machine (CPAP) Defibrillator 10 Prof. Dr. RS Mehta, BPKIHS
- 11. DIAGNOSTIC EQUIPMENT Mobile x-ray units portable clinical laboratory devices, Bronchoscope Colonoscope Endoscope Gastroscope 11 Prof. Dr. RS Mehta, BPKIHS
- 12. OTHER ICU EQUIPMENT Disposable ICU equipment includes Urinary catheter Urinary drainage collector Suction catheter Nasogastric (NG) tube Intravenous(IV) line or catheter Feeding tube Breathing tube( Endotracheal tube) 12 Prof. Dr. RS Mehta, BPKIHS
- 13. Hemodynamic Monitoring 13 Prof. Dr. RS Mehta, BPKIHS
- 14. Prof. Dr. RS Mehta, BPKIHS
- 15. Overview Blood pressure monitoring ◦ NIBP ◦ IBP Central venous pressure monitoring Pulmonary artery pressure monitoring Mixed venous oxygen monitoring Cardiac output 15 Prof. Dr. RS Mehta, BPKIHS
- 16. Why monitor BP? ◦ Alterations inherent ◦ Provides data for interpretation/therapeutic decisions ◦ Important for determining organ perfusion (MAP most important, except with the heart) 16 Prof. Dr. RS Mehta, BPKIHS
- 17. Noninvasive Hemodynamic Monitoring Noninvasive BP Heart Rate, pulses Mental Status Skin Temperature Capillary Refill Urine Output 17 Prof. Dr. RS Mehta, BPKIHS
- 18. Indications for Arterial Blood Pressure Frequent titration of vasoactive drips Major surgery involving large fluid shifts CVP Aortic surgery Unstable blood pressures Frequent ABGs or labs Unable to obtain Non-invasive BP 18 Prof. Dr. RS Mehta, BPKIHS
- 19. Supplies to Gather Arterial Catheter PressureTubing Pressure Cable Sterile Gown SterileTowels Sterile Gloves Pressure Bag Flush – 500cc NS Suture (silk 2.0) Chlorhexidine Swabs Mask 19 Prof. Dr. RS Mehta, BPKIHS
- 20. Potential Complications Associated With Arterial Lines Hemorrhage Air Emboli Infection Altered Skin Integrity Impaired Circulation 20 Prof. Dr. RS Mehta, BPKIHS
- 21. ARTERIAL LINE DEFINITION: It is the method of direct continuous monitoring of systemic arterial pressure by inserting a catheter into peripheral artery either in arm or in leg. The catheter is connected with a transducer with electrical signals. 21 Prof. Dr. RS Mehta, BPKIHS
- 22. PURPOSE: The arterial line provides a way to constantly measure a patient's blood pressure and may be essential to the stabilization of the patient. Continuous measurement of arterial blood pressure in case of open heart surgery. 22 Prof. Dr. RS Mehta, BPKIHS
- 23. Arterial lines may be useful in patients with very high or low blood pressures. The arterial line also provides access for frequent blood sampling. 23 Prof. Dr. RS Mehta, BPKIHS
- 24. COMPLICATIONS: The major complications associated with the arterial line are bleeding, infection, and rarely, a lack of blood flow to the tissue supplied by the artery. 24 Prof. Dr. RS Mehta, BPKIHS
- 25. NURSES ROLE / NURSING CARE Never give any medication through an arterial line. Always check the pressure of the pressurized bag and maintain a pressure of 300mm of hg. Cover the cannula cap with adhesive tape. Flush properly the arterial line every hour and every time after a blood sample is drawn. Always compress the site after removal of arterial line for 10 min. 25 Prof. Dr. RS Mehta, BPKIHS
- 26. BEDSIDE MONITOR A bedside monitor is a display of major body functions on a device that looks like a television screen or computer monitor. 26 Prof. Dr. RS Mehta, BPKIHS
- 27. It is a comprehensive patient monitoring systems that can be configured to continuously measure and display a number of parameters via electrodes and sensors that are connected to the patient. 27 Prof. Dr. RS Mehta, BPKIHS
- 28. These may include the electrical activity of the heart via an EKG, respiration rate (breathing), blood pressure, body temperature, cardiac output, and amount of oxygen and carbon dioxide in the blood. 28 Prof. Dr. RS Mehta, BPKIHS
- 29. Each patient bed in an ICU has a physiologic monitor that measure these body activities. All monitors are networked to a central nurses' station. 29 Prof. Dr. RS Mehta, BPKIHS
- 30. PURPOSES: The monitor is typically used when the doctor wants to measure functions like the heart rate, respiratory rate, blood pressure and temperature. In addition, special functions such as capnography, oximetry, electroencephalography and pulmonary artery catheter readings are also used in certain situations. 30 Prof. Dr. RS Mehta, BPKIHS
- 31. The bedside monitor has alarms that signal the nurse if a body function needs attention. 31 Prof. Dr. RS Mehta, BPKIHS
- 32. NURSES ROLE: Check properly each connection so as to get a desired reading. Any abnormality in a reading is signalled by an alarm so inform doctor immediately. 32 Prof. Dr. RS Mehta, BPKIHS
- 33. CentralVenous Line or Catheter A central venous catheter is a special IV line that is inserted into a large vein in the body. Several veins are used for central venous catheters including those located in the shoulder (subclavian vein), neck (jugular vein), and groin (femoral vein) 33 Prof. Dr. RS Mehta, BPKIHS
- 34. 34 Prof. Dr. RS Mehta, BPKIHS
- 35. Common sites for central venous catheter insertion 1 Prof. Dr. RS Mehta, BPKIHS
- 36. PROCEDURE The most common used method is seldinger technique. Prof. Dr. RS Mehta, BPKIHS
- 37. In some patients, a central venous catheter may be inserted into the elbow vein (anticubital vein) and advanced into the subclavian vein. 37 Prof. Dr. RS Mehta, BPKIHS
- 38. 38 Prof. Dr. RS Mehta, BPKIHS
- 39. PURPOSE These special IVs are used when the patient either does not have adequate veins in the arms or needs special medications and/or nutrition that cannot be given through the smaller arm veins. Serve as a guide of fluid balance in critically ill patients. Determine the function of the right side of the heart 39 Prof. Dr. RS Mehta, BPKIHS
- 40. complication Bleeding and infection are complications associated with IV catheters. As previously mentioned, collapse of a lung is a rare complication of central venous catheters. If this occurs, a chest tube (thoracostomy tube) may be required to re-expand the lung. 40 Prof. Dr. RS Mehta, BPKIHS
- 41. Arterial puncture, cardiac puncture Pneumothorax, Hemomothorax Air emboli,Thrombosis Cardiac temponade Cardiac arrhythmias Carotid Artery Puncture Perforation of SVC or R.Atrium/Ventricle Pleural Effusion 41 Prof. Dr. RS Mehta, BPKIHS
- 42. NURSES ROLE Monitor for the signs of complications. Assess for patency of the CVP line. Sterile dressing should be done to prevent infection( CVP care per the hospital protocol) The length of the indwelling catheter should be recorded and regularly monitored. 42 Prof. Dr. RS Mehta, BPKIHS
- 43. ICP monitor ICU patients who have sustained head trauma, brain hemorrhage, brain surgery, or conditions in which the brain may swell might require intracranial pressure monitoring. 43 Prof. Dr. RS Mehta, BPKIHS
- 44. PURPOSE The purpose of ICP monitoring is to continuously measure the pressure surrounding the brain. If the pressure surrounding the brain gets too high, it can cause decreased blood flow to the brain and potentially lead to brain damage. 44 Prof. Dr. RS Mehta, BPKIHS
- 45. The ICP monitor is usually inserted by a neurosurgeon while the patient is in the ICU or operating room. After using numbing medicine (local anesthetics), the neurosurgeon makes a skin incision and inserts the ICP monitor into the brain through a very small hole created in the skull. 45 Prof. Dr. RS Mehta, BPKIHS
- 46. The ICP monitor is usually inserted in the left or right top-front part of the brain. Some ICP monitors can drain spinal fluid if necessary. 46 Prof. Dr. RS Mehta, BPKIHS
- 47. complication Potential complications associated with ICP monitoring include infection and brain hemorrhage, which are very infrequent. 47 Prof. Dr. RS Mehta, BPKIHS
- 48. Nurses role Optimizing cerebral tissue perfusion. Preventing infection. Maintaining patient airway. Maintaining negative fluid balance. Prevent infection( dressing) 48 Prof. Dr. RS Mehta, BPKIHS
- 49. PULSE OXIMETER A pulse oximeter is the device that measures and displays the oxygen arterial saturation. The study is called pulse oxymetry. The pulse oximeter is a small device that has to be in contact with the skin to detect the oxygen saturation. 49 Prof. Dr. RS Mehta, BPKIHS
- 50. The device is usually place on the patient's finger, earlobe, toe or nose. The pulse oximeter gives off light that determines the oxygen saturation of the blood. 50 Prof. Dr. RS Mehta, BPKIHS
- 51. Breathing Machine (Mechanical Ventilator A breathing machine helps the patient breathe. It is designed to help patients who cannot breathe adequately on their own. The breathing machine does not fix any problems of the lungs. 51 Prof. Dr. RS Mehta, BPKIHS
- 52. It is a device that simply pushes air and oxygen into the lungs and withdraws carbon dioxide from the lungs. The lungs must function in order for the breathing machine to be effective. 52 Prof. Dr. RS Mehta, BPKIHS
- 53. PURPOSE A breathing machine is used whenever a patient cannot breathe without assistance. Doctors, nurses and respiratory therapists all work to make sure a breathing machine is not used any longer than necessary. 53 Prof. Dr. RS Mehta, BPKIHS
- 54. The goal when a breathing machine is first used is to get the patient to be able to breathe on their own, so that the breathing machine can be removed. 54 Prof. Dr. RS Mehta, BPKIHS
- 55. complications Patients who require breathing machine support are at increased risk to develop pneumonia. Occasionally, patients may develop a collapsed lung. Both of these complications require treatment 55 Prof. Dr. RS Mehta, BPKIHS
- 56. NURSES ROLE Promoting effective airway clearance. preventing trauma and infection. Check Ventilator functioning properly Blockage of air passage Too much sputum, secretions When sedation drugs are used ABG, hypoxia 56 Prof. Dr. RS Mehta, BPKIHS
- 57. b. Suction periodically as per need c. Change the mode setup as adviced. d. Give sedatives as adviced. 57 Prof. Dr. RS Mehta, BPKIHS
- 58. INFUSION PUMP An intravenous (IV) infusion pump is a machine that carefully controls the rate at which IV fluids and/or IV medications are given. 58 Prof. Dr. RS Mehta, BPKIHS
- 59. PURPOSE Under some circumstances, the rate at which IV fluids and/or IV medications are given needs to be closely controlled. 59 Prof. Dr. RS Mehta, BPKIHS
- 60. These pumps are very reliable. Mechanical problems are possible, but very rare. If the IV infusion pump does not work correctly, an alarm will sound. 60 Prof. Dr. RS Mehta, BPKIHS
- 61. NURSES ROLE Using aseptic technique and universal precautions, iv infusion should be set. Set the flow rate as prescribed calculating the amount of fluid. Observe for the signs of infiltration or other complications such as thrombophlebitis. Fluid or electrolyte overload and embolism before administration. 61 Prof. Dr. RS Mehta, BPKIHS
- 62. Resuscitation Cart (Crash Cart) The resuscitation cart contains all of the equipment and medications needed for advanced life support and CPR (cardiopulmonary resuscitation). 62 Prof. Dr. RS Mehta, BPKIHS
- 63. purpose This emergency equipment is used only if the patient's heart or lungs stop working. The cart is brought to the patient's bedside when the patient's heart or lungs are failing or have failed. 63 Prof. Dr. RS Mehta, BPKIHS
- 64. NURSES ROLE Keep the resuscitation cart ready all the time. Check the devices and ensure that the devices are kept in charging. Check for the emergency (life saving) medication for their expiry date. 64 Prof. Dr. RS Mehta, BPKIHS
- 65. DEFIBRILLATOR A defibrillator is a device that is designed to pass electrical current through a patient’s heart. The passing of electrical current through the heart is called defibrillation. A defibrillation is done through pads placed on the patient’s chest. 65 Prof. Dr. RS Mehta, BPKIHS
- 66. purpose A defibrillation is used to restore a patient’s heart rhythm to normal. Abnormal heart rhythms may be treated with medications while other rhythms need to be treated with defibrillation. 66 Prof. Dr. RS Mehta, BPKIHS
- 67. Life threatening heart rhythms need defibrillation immediately while other heart rhythms may be defibrillated in a scheduled fashion. Defibrillation may be done using the manual defibrillator or the automatic external defibrillator (AED). 67 Prof. Dr. RS Mehta, BPKIHS
- 68. Complication The defibrillator pads may cause a skin irritation and leave a temporary redden area where they contacted the chest. Unfortunately defibrillation does not always return the patient’s heart rhythm back to normal. 68 Prof. Dr. RS Mehta, BPKIHS
- 69. NURSES ROLE Keep the patient in comfortable position and obtain 12 lead ECG. Give the patient 100 % oxygen by inhalation. Apply electrode paste on the DC paddle, rub it and apply the paste at the patient’s chest in the second intercostal space at the right side of breast line and at the apex of the heart. 69 Prof. Dr. RS Mehta, BPKIHS
- 70. TURN OFF the oxygen to the patient as a spark from paddle could blow the oxygen on the fire. Be sure to say “ ALL CLEAR”. No one should touch the patient or the bed during cardioversion. Check the rhythm on ECG monitor. Keep the patient in comfortable position and give 100% oxygen by inhalation. 70 Prof. Dr. RS Mehta, BPKIHS
- 71. Report and record the procedure and clean the paddle area with spirit swab. Keep the difibrilator on continue electrical charging. 71 Prof. Dr. RS Mehta, BPKIHS
- 72. MAINTENANCE OF ICU EQUIPMENTS Since ICU equipment is used continuously on critically ill patients, it is essential that equipment be properly maintained, particularly devices that are used for life support and resuscitation. 72 Prof. Dr. RS Mehta, BPKIHS
- 73. Contd… Staff in the ICU should perform daily checks on equipment and inform biomedical engineering staff when equipment needs maintenance, repair, or replacement. For mechanically complex devices, service and preventive maintenance contracts are available from the manufacturer or third- party servicing companies, and should be kept current at all times. 73 Prof. Dr. RS Mehta, BPKIHS
- 74. Health care team roles Equipment in the ICU is used by a team specialized in their use. The team usually comprises a critical care attending physician (also called an intensivist), critical care nurses, an infectious disease team, critical care respiratory therapists, pharmacologists, physical therapists, and dietitians. 74 Prof. Dr. RS Mehta, BPKIHS
- 75. Radiologic technologists perform mobile x ray examinations (bedside radiography). Either nurses or clinical laboratory personnel perform point-of-care blood analysis. Equipment in the ICU is maintained and repaired by hospital biomedical engineering staff and/or the equipment manufacturer. 75 Prof. Dr. RS Mehta, BPKIHS
- 76. Thank you 76 Prof. Dr. RS Mehta, BPKIHS
