Role of adipose tissue inflammation in PAR2-mediated OA progression
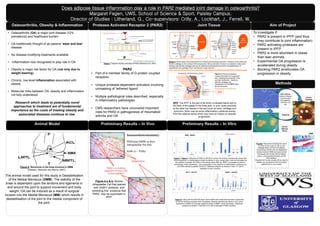
- 1. • Osteoarthritis (OA) is major joint disease (12% prevalence) and healthcare burden • OA traditionally thought of as passive ‘wear and tear’ disease • No disease-modifying treatments available • Inflammation now recognised to play role in OA • Obesity is major risk factor for OA (not only due to weight bearing) • Chronic, low level inflammation associated with obesity • Molecular links between OA, obesity and inflammation not fully understood Research which leads to potentially novel approaches to treatment are of fundamental importance as the costs of treating obesity and associated diseases continue to rise. Preliminary Results – In Vitro Figure 2: a) the tissue and components of a normal joint including synovium, meniscus of the knee and smooth cartilage on the surface of the long bones, (femur and tibia in knee) in comparison to b) a joint showing mild arthritic changes such as an inflamed and thickened synovium, the appearance of osteophytes and cartilage which has become rough and thin. http://www.arthritisresearchuk.org/arthritis-information/conditions/arthritis/what-is-arthritis.aspx Figure 1: Diagram showing activation of PAR2 (McIntosh et al, 2003) Protease Activated Receptor 2 (PAR2) a b Preliminary Results – In Vivo PAR2 +ve staining suggestive of mast cells or macrophages Immunohistochemistry Wild type DMM 14 days Infrapatellar Fat Pad SAM-11 – PAR2 Figure 3: Knee joint showing normal structures of a hinge joint and indicating the proximity of the synovial membrane, meniscus, articular cartilage and Infrapatellar Fat Pat IPFP within the join structure www.interactive-biology.com Osteoarthritis, Obesity & Inflammation To investigate if: • PAR2 is present in IPFP (and thus may contribute to joint inflammation) • PAR2 activating proteases are present in IPFP • PAR2 is more abundant in obese than lean animals • Experimental OA progression is accelerated during obesity • Blocking PAR2 ameliorates OA progression in obesity Aim of ProjectJoint Tissue IPFP Adipocytes Animal Model Figure 6 a & b: Murine Infrapatellar Fat Pad stained with SAM11 antibody and exhibiting first evidence that PAR2 may be expressed in IPFP. a b Does adipose tissue inflammation play a role in PAR2 mediated joint damage in osteoarthritis? Margaret Fegen, UWS, School of Science & Sport, Paisley Campus. Director of Studies : Litherland, G., Co-supervisors: Crilly, A., Lockhart, J., Ferrell, W. IPFP: The IPFP is the pad of fat which is situated below and to the back of the patella in the knee joint. In such close proximity to the other key tissues in the joint such as bone, cartilage and synovium, there may be some inflammatory cytokines arising from the adipose tissue which may have an impact on disease progression. Figure 5: Structures in the knee involved in DMM (Glasson, Blanchet and Morris, 2007) *** *** *** ** Methods n.s. n.s. The animal model used for this study is Destabilisation of the Medial Meniscus (DMM). The stability of the knee is dependent upon the tendons and ligaments in and around the joint to support movement and body weight. OA can be induced as a result of surgical incision into the Medial Meniscus (MM) which results in destabilisation of the joint to the medial component of the joint. Cell Culture: Human Articular Chondrocytes (OA patients), SW1353 cell line Explants Human Cartilage Human Adipose tissue Figure4: Resources including the use of Primary human cells (a), fat (c) and cartilage tissue (b) from OA patients, chondrocyte cell line and an established animal model of DMM (d).Experimental techniques will include cell and tissue culture, Immunohistochemistry, qPCR, RNA isolation. Results from human studies will be used to validate and complement the information gained from in vivo model. DMM Figure 7: Figure 7: Detection of PAR2 by qPCR on human OA primary chondrocytes shows that PAR2 expression is undetectable in basal conditions in vitro, except when cells are stimulated by the cytokine oncostatin M (OSM) or the phorbol ester PMA (a). MMP1 (a protease involved in extracellular matrix breakdown) was upregulated in the presence of inflammatory cytokines but not PAR2 activatory peptide (SLIG) (b). Statistical analysis by student T-Test, n=1 with 6 replicates of each condition. a b c d Figure 8: Using cell line SW1353 which were treated with media that has been conditioned by human fat tissue explants from OA patients showing that there are factors which show expression of PAR2 (a) and also significant levels of MMP1 being expressed. Statistical analysis by student T-Test with n=10 with 6 replicates of each condition. a a b b PAR2 • Part of 4 member family of G-protein coupled receptors • Unique protease-dependent activation involving unmasking of ‘tethered ligand’ • Multiple pathological roles described, especially in inflammatory pathologies • CMS researchers have uncovered important roles for PAR2 in pathogenesis of rheumatoid arthritis and OA * n.s. n.s. n.s. n.s. n.s. n.s. n.s.