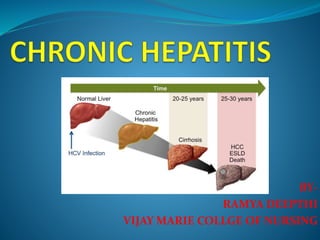
Chronic hepatitis
- 1. BY- RAMYA DEEPTHI VIJAY MARIE COLLGE OF NURSING
- 2. Definition Chronic hepatitis is defined as continuing or relapsing hepatic disease for more than 6 months, with presence of symptoms and other diagnostic parameters- serology, biochemical and histopathology.
- 3. Etiology Usually due to hepatitis B, C, or a combined hepatitis B, D Non viral causes- 1. Wilson disease 2. Antitrypsin deficiency 3. Chronic alcoholism 4. Impaired immunity 5. Extremes of age Chronic hepatitis is a carrier state where the individual harbors and replicates virus, hence can transmit the organism.
- 4. Clinical features Common features are- Fatigue Loss of appetite Mild jaundice Raised serum transaminases Lab findings reveal liver cell injury
- 5. Morphology MICROSCOPY: histological features of chronic hepatitis ranges from mild to severe. 1. PIECEMEAL NECROSIS: piece by piece necrosis around the portal tract, infiltration of lymphocytes, plasma cells and macrophages.
- 6. 2. INTRALOBULAR LESION: Focal area of necrosis and inflammation are seen in adjacent areas of liver parenchyma called interface hepatitis. These have scattered acidophilic body and kupffer cell hyperplasia.
- 7. 3. BRIDGING FIBROSIS: Initially portal tract and later periportal areas exhibit fibrosis followed by linking fibrous septa between lobules causing disarray of the architecture.
- 8. Activity score Evolved to assess the activity of chronic hepatitis based on the histomorphology as follows. a. Necrosis: periportal bridging- score ranges from 0-10 0- no necrosis 10- multilobular necrosis b. Inflammation: depth/ extent. Score ranges from 0-4 0- no inflammation 4-marked portal inflammation c. fibrosis: density/ extent. Score ranges form 0-4 0- no fibrosis 4- resembles cirrhosis
- 9. Based on activity score chronic hepatitis is further classified into - Chronic persistent hepatitis- mild activity Chronic lobular hepatitis- mild to moderate fibrosis Chronic active hepatitis- moderate to severe fibrosis.
- 10. IV. CARRIER STATE Individual with out symptoms but harboring infection with hepatotrophic virus and is capable of transmitting infection to others is called carrier state. Hepatitis A and E do no produce carrier state. Hepatitis B is mostly responsible for all carrier cases in the world. It is detected by HBsAg in the serum. Morphology: Carrier on biopsy do not show any changes on liver. They show granular ground glass eosinophilic cytoplasm as evidenced by HBsAg.
- 11. V. FULMINANT HEPATITIS It is most severe form of acute hepatitis seen within 2-3 weeks of onset of symptoms and progress to fulminate hepatic failure. 2 patters are seen- 1. Sub fulminate- has a less rapid course, and 3extends up to 3months 2. Fulminate type: it has 2 etiological agents- a. Viral- usually HBV, HAV, HCV and rarely HBV HDV.
