Endocrine system pharm D.pdf
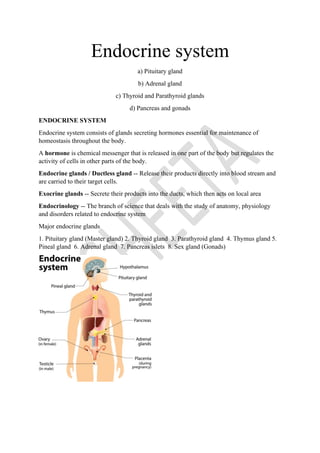
- 1. Endocrine system a) Pituitary gland b) Adrenal gland c) Thyroid and Parathyroid glands d) Pancreas and gonads ENDOCRINE SYSTEM Endocrine system consists of glands secreting hormones essential for maintenance of homeostasis throughout the body. A hormone is chemical messenger that is released in one part of the body but regulates the activity of cells in other parts of the body. Endocrine glands / Ductless gland -- Release their products directly into blood stream and are carried to their target cells. Exocrine glands -- Secrete their products into the ducts, which then acts on local area Endocrinology -- The branch of science that deals with the study of anatomy, physiology and disorders related to endocrine system Major endocrine glands 1. Pituitary gland (Master gland) 2. Thyroid gland 3. Parathyroid gland 4. Thymus gland 5. Pineal gland 6. Adrenal gland 7. Pancreas islets 8. Sex gland (Gonads)
- 2. PITUITARY GLAND • Pituitary gland or hypophysis was called the “master” endocrine gland because it secretes several hormones that control other endocrine glands • 1-1.5 cm Anatomy • Pea shaped structure that measures 1–1.5 cm in diameter • Located in the hypophyseal fossa of the sphenoid bone.
- 3. • It attaches to the hypothalamus by a stalk called infundibulum and has two anatomically and functionally separate portions: the anterior pituitary and the posterior pituitary. • Both hypothalamus and pituitary gland function as a unit to regulate all endocrine glands • Grow upto 40 years and then size get reduced The anterior pituitary (anterior lobe): • Also called the adenohypophysis, and is composed of epithelial tissue. • Forms total 75% of pituitary gland • All the hormones released are regulated by hormones from hypothalamus • Anterior pituitary consists of three parts: The pars distalis, Pars intermedia and pars tuberalis. • Pars distalis is the larger portion, and pars tuberalis forms a sheath around infundibulum. • Pars intermedia- third region that lies between pars distalis and pars tuberalis, degenerate during human fetal development. Characters of ant. Pit hormones
- 4. • 1. proteinaceous in nature • 2. Being water soluble effect exert via second messengers • 3. released in response to hormonal stimuli and their regulation is done by negative feedback mechanism • 4. all the hormones from ant pituitary regulate the hormone release of other glands • 5. all the ant pit hormone release is regulated by releasing or inhibiting hormone by hypothalamus HORMONES OF ANTERIOR PITUITARY • Anterior pituitary releases seven hormones. • The release of all these hormones is regulated by releasing hormones and by inhibiting hormones released by the hypothalamus. • Anterior pituitary hormones are: Growth hormone, Thyroid- stimulating hormone, Follicle stimulating hormone, Luteinizing hormone, Prolactin, Adrenocorticotropic hormone, melanocyte stimulating hormone. Types of Anterior Pituitary Cells: Five types of anterior pituitary cells—somatotrophs, thyrotrophs, gonadotrophs, lactotrophs, and corticotrophs— all together secrete seven hormones. 1) Somatotrophs secrete human growth hormone (hGH) or somatotropin. 2) Thyrotrophs secrete TSH or thyrotropin. 3) Gonadotrophs secrete two gonadotropins: FSH and LH 4) Lactotrophs secrete prolactin 5) Corticotrophs secrete ACTH or corticotropin Corticotrophs of pars intermedia, also secrete melanocyte-stimulating hormone (MSH) The posterior pituitary (posterior lobe): • Also called the neurohypophysis • composed of neural tissue. • Consists of two parts: the pars nervosa (larger bulbar portion) and the infundibulum. • Posterior pituitary also consists of axons and axon terminals with more than 10,000 neurons. • Axon terminals in the posterior pituitary are associated with specialized neuroglia called pituicytes, which stores 2 hypothalamic hormones, oxytocin and vasopressin.
- 5. 1. HUMAN GROWTH HORMONE • Somatotrophs produce human growth hormones which stimulate skeletal muscles, cartilage, bones and other tissues to produce insulin like growth factors/ somatomedins. Functions of IGFs • 1. Helps in the growth and proliferation of cells and thymus gland • 2. Maintain the mass of muscle and bones. • 3. Promote wound healing • 4. Enhance lipolysis in adipose tissue and release fatty acid (used for energy) • 5. Regulation of glucose level • 6. Enhance protein and carbohydrate metabolism • 7. Increase growth of long bones and increase blood level of Na, K, PO4, Cl, Mg etc… Hormonal imbalance • Both over production and under production of GH may lead to structural abnormalities. a.Pituitary dwarfism: Deficiency of hGH in children during growing years causes stunted growth. • Results in Premature closure of epiphyseal plate Symptoms: Arms and legs become shorter, protruding forehead, flat nasal bridge, large head, constrained elbow movement, delayed puberty Treatment- hGH in childhood before closure of epiphyseal plate b. Gigantism: Abnormal increase in the secretion of growth hormones in children during growing year • characterized by abnormal increase in the length of bones. • caused by an adenoma, a tumor of the pituitary gland. Treatment – administration of inhibiting hormone before closure of epiphyseal plate c. Acromegaly: Abnormal increase in the secretion of growth hormones in adults after closure of epiphyseal plate Symptoms: • Enlarged hands and feet, enlarged facial features, including the facial bones, eyelids, lips, nose and tongue, increased blood glucose level, size of metabolic organs, sweating • No further increase in height
- 6. Regulation • Secretion is regulated by 2 hypothalamic hormones • 1. Growth hormone releasing hormone (GHRH) • 2. Growth hormone inhibiting hormone (GHIH) 2. THYROID STIMULATING HORMONE • A glycoprotein hormone, secreted by thyrotrophs of anterior pituitary gland. • regulate the growth and functioning of the thyroid gland. • TSH stimulates the synthesis and secretion of the two thyroid hormones, thyroxin (T4) and triiodothyronine (T3) by the thyroid gland. • Thryotropin releasing hormone (TRH) from hypothalamus control TSH secretion. • Release of TRH in turn depends on the blood levels of T3 and T4 • high levels of T3 and T4 inhibit secretion of TRH via negative feedback. Functions: 1. It stimulates growth and activity of the thyroid gland which secretes the hormones T4 &T3 that regulates the metabolic activities and brain development. 2. Regulates the body temperature 3. Detection of imbalances and abnormal functioning of the thyroid gland 3. GONADOTROPINS a. FOLLICLE-STIMULATING HORMONE (FSH) • It is a gonadotropic hormone ie, its target site are the gonads. • It is produced by gonadotrophs in the anterior pituitary Functions: • 1. In male, stimulates spermatogenesis, a process of sperm production in the testes • 2. In females, induces maturation of graafian follicles therefore facilitate ovulation • 3. It also stimulates the follicular cells to secrete the female sex hormones. b. LUTEINIZING HORMONE (LH) • A glycoprotein made up of one α-subunit and one β-subunit. • also a gonadotropin and is secreted by gonadotrophs of the anterior pituitary. Functions: 1. In males: Initially stimulates the growth and development of interstitial (Leydig) cells of testes and then stimulates them to release testosterone.
- 7. 2. In females: responsible for complete development of ovarian follicles and thus ovulation. 3. Like FSH, it also stimulates the ovarian cells to secrete estrogens. 4. It initially stimulates the formation of corpus luteum and subsequently induces it to release progesterone. Gonadotropin releasing hormone produced by the hypothalamus induce release of LH and FSH from the anterior pituitary No inhibiting hormones are there and so sex hormones through negative feedback mechanism inhibit the release of FSH and LH Hormonal imbalance 1) Hyposecretion of FSH and LH: • As these gonadotropins are essential for fertility, their hyposecretion results in reduced fertility in both the genders. 2) Hypersecretion of FSH and LH • This condition has not been associated with any disorders. • But when women with reduced fertility are administered certain drugs that increase the release of these hormones, they usually results in multiple births. This is due to multiple ovulation which occurs at the same time 4. PROLACTIN • A single chain polypeptide hormone. • also known as luteotrophic hormone/ mammotrophin hormones. • Produced by lactortrophs in anterior pituitary, immune cells, brain and pregnant uterus. Functions 1. Stimulates the development of mammary gland and ducts and so milk production after delivery. 2. Also cause Amenorrhoea and galactorrhoea 3. No role in males, but in some hypersecretion results in erectile dysfunction Regulation -Prolactin-releasing hormone (PRH), from hypothalamus induce release of prolactin. In non-pregnant women lactation is inhibited by prolactin inhibiting hormone (PIH) or dopamine 5. ADRENOCORTICOTROPHIC HORMONE (ACTH)/ CORTICOTROPIN • A polypeptide hormone released from the corticotrophs of the anterior pituitary.
- 8. • controls the production and secretion of cortisol and other glucocorticoids by the cortex of the adrenal glands Functions • 1. Responsible for promoting the growth of cortex • 2. Stimulates the secretion of cortisol from the adrenal cortex. • 3. Facilitates the uptake of lipoproteins into the cortical cells. Regulation: Corticotropin-releasing hormone (CRH) from the hypothalamus stimulates secretion of ACTH by corticotrophs. • Stress-related stimuli, such as low blood glucose or physical trauma etc. also stimulate release of ACTH. • Inhibition is done by adrenal hormone by negative feedback mechanism 6. MELANOCYTE-STIMULATING HORMONE (MSH) • A peptide hormone, secreted by pars intermedia of pituitary gland • MSH increases skin pigmentation by stimulating melanocytes. • Excessive levels of corticotropin-releasing hormone (CRH) can stimulate MSH release; • dopamine inhibits MSH release. • Group of melanocytes on the skin are called moles. Functions: • 1. Stimulates the release and distribution of melanin • 2. Presence of MSH receptors in the brain influence brain activity. • 3. Melanocytes present on the skin and eye produce melanin pigments HORMONES OF POSTERIOR PITUITARY • Also called neurohypophysis, does not produce hormones but acts as their storage site. • The two hormones, oxytocin and ADH are actually synthesized by the neurosecretory cells of the hypothalamus. 1. OXYTOCIN: • The 2 main target organs of oxytocin are the uterus of the pregnant women and mammary glands of the lactating mothers. • During child birth, oxytocin facilitates the expulsion of the child by inducing the contractions of the uterus and increased stretching of the uterine cervix.
- 9. • After delivery, the suckling induces the release of oxytocin which inhibits the release of prolactin inhibiting hormone (PIH) thereby prolonging prolactin secretion and lactation. Functions: 1. Stimulates the contraction of smooth muscles in uterus during child birth. 2. Stimulates milk ejection from mammary glands. 3. In non-pregnant uterus-facilitate the transport of sperms through female genital tract up to the fallopian tube 4. Have some antidiuretic action Regulation • By two positive feedback mechanism • 1. cervical distension during delivery- stimulate hypothalamus • 2. suckling by baby- stimulate hypothalamus 2. ANTIDIURETIC HORMONES • Peptide hormone, which decrease urine output. • ADH is packed in secretory vesicles. Functions: 1. Decrease urine output 2. Absorption of water by kidney 3. Maintain fluid electrolyte balance. 4. It stimulates the smooth muscles of the urinary bladder and ureters. Hormonal imbalance • Diabetes incipidus (DI): It occurs due to inappropriate secretion of ADH which leads to increased urinary output. It is of 2 types • i. Neurogeneic DI: occurs due to decreased secretion of ADH due to brain tumour or head trauma that damages posterior pituitary. • ii. Nephrogenic DI: Kidneys don’t respond to ADH due to its damage or due to non functioning of the ADH receptors. Symptoms: increased urinary output, dehydration, intense thirst, bed wetting which is common in children. Treatment- Neurogenic DI- with analogues of ADH as s.c injection or nasal spray Nephrogenic DI- reduce consumption of salt in diet along with some antidiuretic drugs
- 10. Regulation • Regulated by osmoreceptors in hypothalamus • The variation in osmotic pressure of blood is sensed by osmoreceptors in hypothalamus • Decrease or increase ADH synthesis by hypothalamus THYROID GLAND • Highly vascularized • About 20-25g located at the base of throat just inferior to the larynx. • It is brownish red in colour, butterfly shaped • Anatomically divided into two lobes- right and left lateral lobes • Right lobe is little larger than left • They are connected by a middle lobe called isthmus which is anterior to the trachea. • An additional third lobe called the pyramidal lobe which extends from the isthmus to neck • Thyroid artery and thyroid veins are responsible for blood flow • This rich blood flow provide adequate supply of Iodine • Up on microscopic examination, thyroid gland is composed of follicles or vesicles. • It consist of follicular cells • These follicles are filled with sticky, proteinaceous material called colloid. • Colloid contains thyroglobulin • T3 and T4 are synthesized by follicular cells and stored as thyroglobulin • Thyroid gland also contains parafollicular cells or C cells • C cells synthesis calcitonin • The special feature of thyroid gland is that it store large quantity of preformed thyroid hormones
- 11. • • Thyroid hormones • Ratio of T4 and T3 in blood is 20:1 • Both are responsible for the proper growth and functioning of the body cells • T4 is the major hormone • Formation, Storage, and Release of Thyroid Hormones • 1. Iodide trapping: Thyroid follicular cells trap iodide ions (I) from the blood • 2. Synthesis of thyroglobulin: Follicular cells are also synthesize a protein called thyroglobulin (TGB) and stored in secretory vesicles. • The vesicles then undergo exocytosis, which releases TGB into the lumen of the follicle. • 3. Oxidation of iodide: Negatively charged iodide ions cannot bind to tyrosine, they undergo oxidation in presence of peroxidase and they pass through the membrane into the lumen of the follicle. • 4. Iodination of tyrosine: Combination of iodine with tyrosine is known as iodination.
- 12. • It is catalysed by iodinase. • Iodination of tyrosine occurs in several stages. • Tyrosine is iodinated into monoiodotyrosine (MIT), then to di-iodotyrosine (DIT). • 5. Coupling: Iodotyrosine residues get coupled with one another. • One molecule of DIT and one molecule of MIT combine to form tri-iodothyronine (TID or T3). • Two molecules of DIT combine to form tetraiodothyronine (TIT or T4). • 6. Pinocytosis and digestion of colloid and release of hormones: Digestive enzymes in the lysosomes break down colloid and therefore TGB and release T3 and T4 into blood as per need. • T4 normally is secreted in more quantity than T3 • But T3 is several times more potent.
- 13. Regulation • Two major hormones that regulate thyroid hormones are • 1. Thyrotropin releasing hormone (TRH from hypothalamus) • 2. Thyrotropin stimulating hormone or thyrotropin (TSH from anterior pituitary) • Positive feedback mechanism • Low blood level of thyroid hormone or low metabolic rate stimulate hypothalamus to release TRH • TRH then stimulate anterior pituitary to release TSH • TSH stimulate thyroid gland to release more amount of T4 and T3 • Negative feedback mechanism • High level of thyroid hormone or high metabolic rate inhibit hypothalamus and anterior pituitary • It reduce the hormone release by thyroid gland Function • Calorigenic effect : Increase cellular oxygen uptake, ATP production and basal metabolic rate (BMR) • Increase body temperature
- 14. • Increase protein metabolism • Increase lipolysis • Osteoporosis as they stimulate removal of calcium and phosphorous from bones • Responsible for general growth and development of nervous and skeletal system • Carbohydrate metabolism • Increase glucose absorption • Convert glycogen to glucose • Gluconeogenesis • Increase action of adrenaline and nor adrenaline- so increase heart rate and BP • Increase milk ejection and protein content in milk • Renal effects • Increase renal excretion of nitrogen and creatinine • Diuretic effect – excrete water and electrolytes Calcitonin: • It is a hormone produced by the parafollicular cells or C-cells of the thyroid gland • CT (Calcitonin) can decrease the level of calcium in the blood by inhibiting the action of osteoclasts. • It is regulated by the levels of calcium ions (Ca2+) in the blood. • High blood Ca2+ levels increase the production of calcitonin whereas decreases Ca2+ levels in blood decrease the production of calcitonin. Functions • 1. calcium homeostasis along with parathyroid hormone • 2. maintain phosphate level in blood • 3. improve bone strength