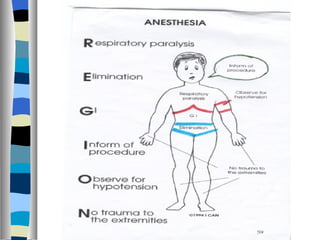
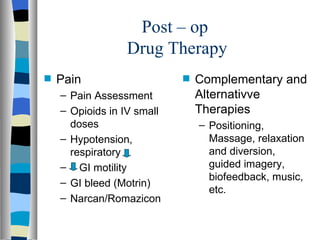
This document discusses perioperative care and defines the three phases as preoperative, intraoperative, and postoperative. It outlines nursing responsibilities and goals in each phase, including assessment, monitoring for complications, education, and promoting patient well-being and recovery.